ABSTRACT
BACKGROUND: Prominent ear is the most common congenital defect of the ear, with an incidence of 5% in Caucasians. Surgical treatment should correct the auriculocephalic and conchoscaphal angles as well as protrusion of the lobe when present. This paper aims to report the experience of our service in the treatment of prominent ears with a combination of several available techniques.
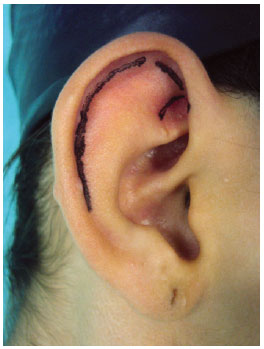
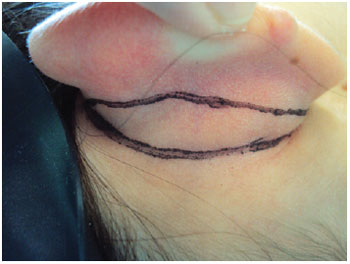
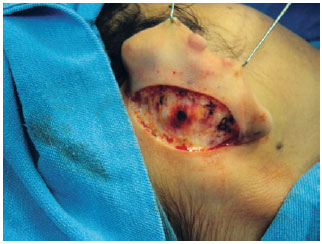
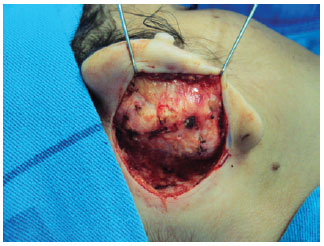
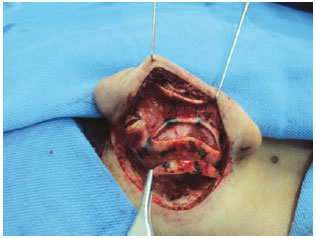
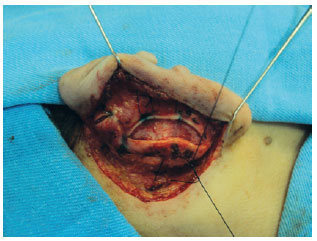
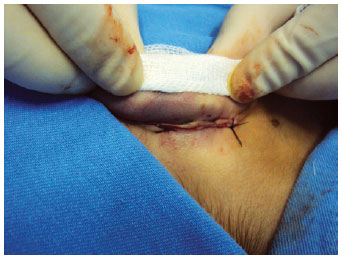
METHODS: Forty-seven patients operated with a combination of previously described techniques were evaluated, and cartilaginous incision, Mustardé sutures for antihelix definition, and concha-mastoid fixation were performed. Patients less than 15 years of age were operated under general and local anesthesia, while the remaining patients underwent only local anesthesia. All patients were reassessed on the first postoperative day.
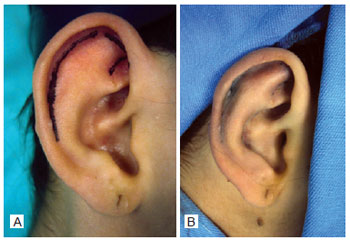
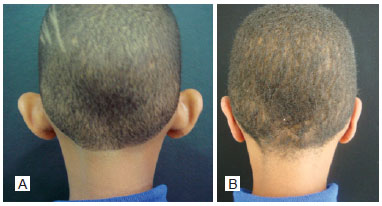
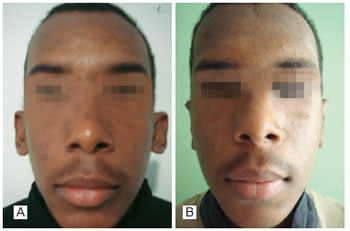
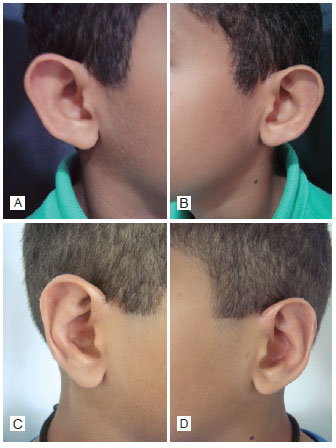
RESULTS: The postoperative results were considered satisfactory by both patients and surgical staff, with no stigma development in the operated ear.
CONCLUSIONS: The best treatment of prominent ears is achieved by a combination of techniques. The approach used on the studied patients has produced natural-looking results with low complication rates, satisfying the surgical staff and, most importantly, the patients.
Keywords: External ear/surgery. Plastic surgery/methods. Ear diseases/surgery.