ABSTRACT
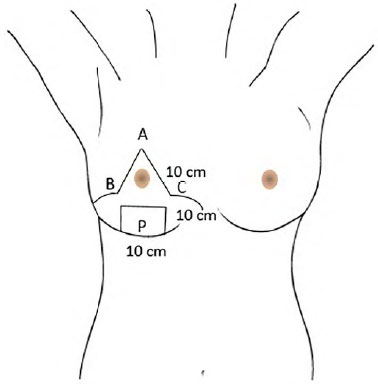
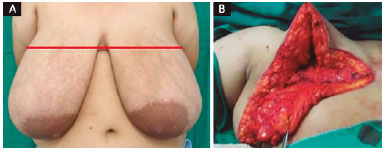
INTRODUCTION: Patients with gigantomastia have multiple physical and psychosocial symptoms. Various techniques have been proposed for their treatment. Described by Torek in 1922, mammary amputation was presented as a great alternative, but resulted in reduced mammillary functionality and loss of breast format. In 1975, Liacyr Ribeiro described the use of dermaglandular inferior pedicle as safety tissue to allow for mammary resection, to facilitate breast assembly and to improve projection. The author proposed to unite these two consolidated techniques with the intention of improving breast amputation outcomes.
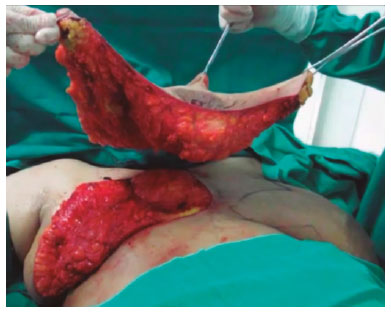
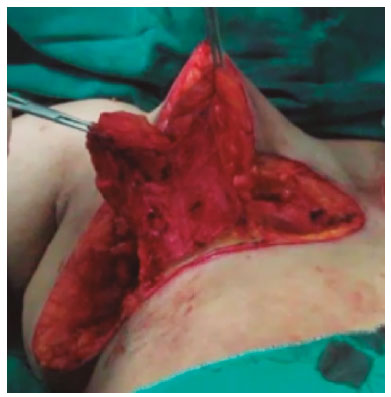
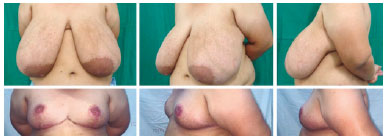
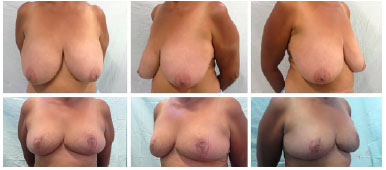
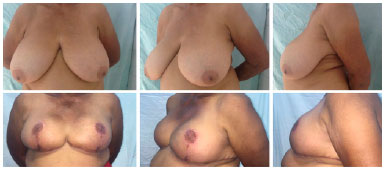
METHODS: Eleven gigantomastia patients were operated on by means of the amputation technique using dermaglandular inferior pedicle.
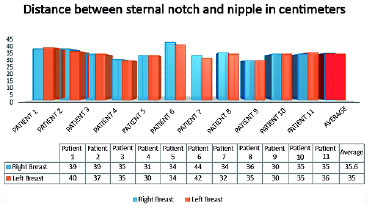
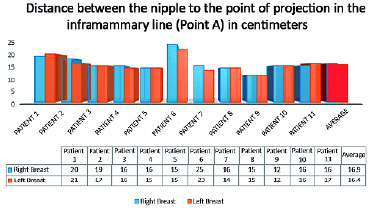
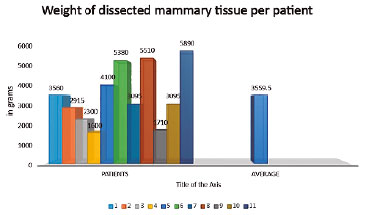
RESULTS: The mean distance between the sternal notch and the nipple was 35.6 cm for the right breast and 35 cm for the left breast, with all measures ranging between 30 cm and 44 cm. Rise of the nipple-areola complex was in average 16.9 cm for the right breast and 16.4 cm for the left breast, varying from 12 to 25 cm. The amount of breast tissue resection per patient was, in average, 3559.5 grams, ranging from 1600 grams to 5890 grams. Hypopigmentation of the nipple-areola complex was present in three patients (27%). Dehiscence of the T was observed in two patients (18%). Partial non-integration of the graft occurred in three patients (27%), with loses estimated at 10%, 30% and 80% of the graft.
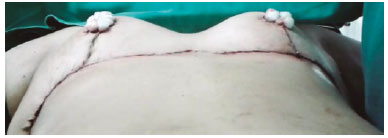
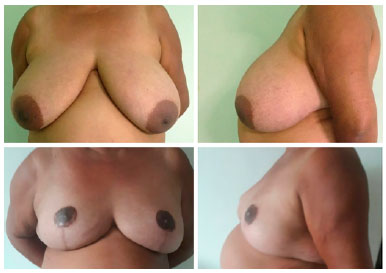
CONCLUSION: Associating mammary amputation with an inferior dermaglandular pedicle provides good remodeling and safe assembling of the breast, in addition to providing proper projection.
Keywords:
Breast/abnormalities; Mammaplasty; Hyperthophy; Amputation.
RESUMO
INTRODUÇÃO: Pacientes com gigantomastia apresentam múltiplos sintomas físicos e psicossociais. Várias técnicas foram propostas para o seu tratamento. A amputação mamária, descrita por Torek em 1922, apresenta com excelente alternativa, porém com prejuízo na funcionalidade mamilar e no formato da mama. Liacyr Ribeiro, em 1975, descreveu o retalho inferior dermoglandular não areolado a fim de proporcionar tecido de segurança para ressecção mamária, facilitar a montagem da mama e melhorar sua projeção. Este trabalho propôs unir estas duas consagradas técnicas, visando aprimorar os resultados das amputações mamárias.
MÉTODOS: Foram operadas 11 pacientes com gigantomastia com prole definida, pela técnica de amputação mamária associada ao pedículo inferior não areolado.
RESULTADOS: Distância média da fúrcula esternal ao mamilo foi de 35,6 centímetros na mama direita e 35 centímetros na mama esquerda, variando de 30 a 44 centímetros. A ascensão do complexo areolomamilar foi em média de 16,9 centímetros na mama direita e 16,4 centímetros na mama esquerda, variando de 12 a 25 centímetros. A quantidade de ressecção média de tecido mamário por paciente foi de 3559,5 gramas, variando de 1600 a 5890 gramas. A hipopigmentação do complexo areolamamilar esteve presente em três (27%) pacientes. A deiscência do T foi observada em dois (18%) pacientes. A não integração parcial do enxerto ocorreu em três (27%) das pacientes, com perdas estimadas de 10%, 30% e 80% do enxerto.
CONCLUSÃO: A associação da amputação mamária com o pedículo dermoglandular inferior não areolado nos oferece um melhor remodelamento da mama, segurança na montagem desta, além de proporcionar uma adequada projeção da mesma.
Palavras-chave:
Mama/anormalidades; Mamoplastia; Hipertrofia; Amputação.