ABSTRACT
INTRODUCTION: An approach based on multiple anatomical structures and the use of different surgical strategies seems to achieve more lasting results in cervical rejuvenation surgery. Thus, extended cervicoplasty is an option with favorable results and low complication rates. However, little has been published regarding the durability of the results. This study aimed to objectively evaluate the long-term results obtained with extended cervicoplasty in difficult cases.
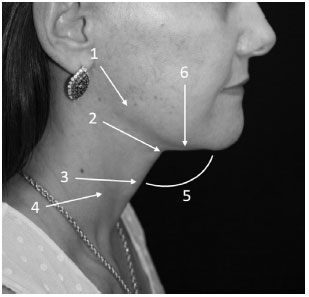
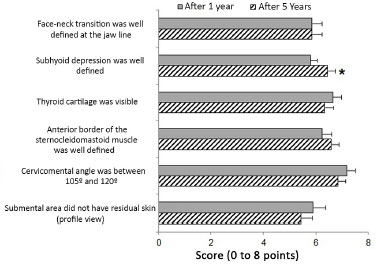
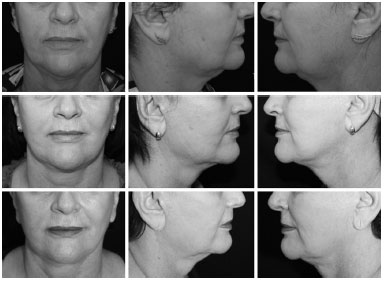
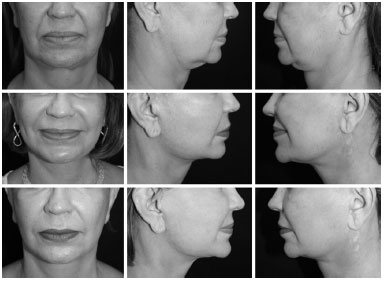
METHODS: Twenty patients, classified as having a "difficult neck," underwent extended cervicoplasty and were followed for 5 years. The results at 1- and 5-year post-operative follow-up were evaluated by eight plastic surgeons, using six objective criteria based on a theoretically ideal neck. The comparison of the results obtained at these time points was performed using a paired Student's t-test, with a level of significance of 5%.
RESULTS: There was no significant difference in five of the six items evaluated (p-value ranging from 0.137 to 1.000), in the comparison between the first and fifth postoperative years. Subhyoid depression displayed a significantly better mean score in the fifth evaluation year than that observed in the first year after surgery (p = 0.039): from 5.80 ± 0.25 points (mean ± standard error of the mean) in the first year, to 6.45 ± 0.30 points in the fifth postoperative year.
CONCLUSION: Extended cervicoplasty is an important alternative in the treatment of the neck region, and even provides lasting results in difficult cases.
Keywords: Rhytidoplasty; Cervicoplasty; Neck muscles; Rejuvenation; Neck.