ABSTRACT
INTRODUCTION: Evaluation of a 5-year epidemiological analysis and updated surgical treatment of high-voltage electrical burns.
METHODS: A descriptive, retrospective cross-sectional study was conducted in the Center of Burn Treatment Dr. Oscar Plaisant, Federal Hospital of Andaraí, Rio de Janeiro, Brazil, from January 2009 to December 2014. A form was applied to the medical records of 38 patients included in the study in order to assess the defined variables.
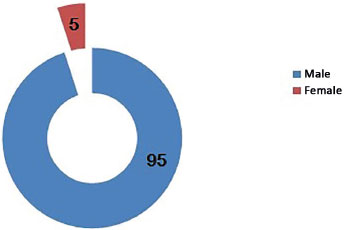
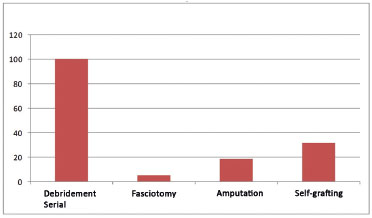
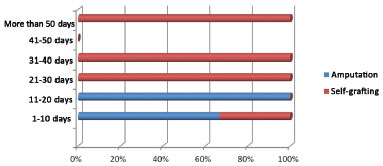
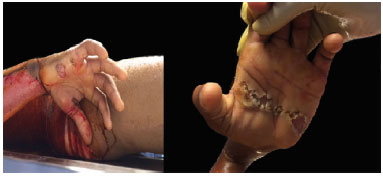
RESULTS: In total, 38 patients with high-voltage burns were evaluated, 95% of whom were men aged between 21 and 42 years. The most frequent place of occurrence was the workplace in 55.3% of cases. The percentage of burned total body surface area ranged from 1% to 60%. The most affected part of the body was the left hand in 55.26% cases. Presurgical preparation for self-grafting was necessary in 34.21% subjects, and the mean time elapsed was 37.5 days. The type of surgical treatment was serial debridement under general anesthesia in 100% of the patients, self-grafting in 31.6%, amputation in 18.4%, and fasciotomy in 5.3%. The mortality rate was 0%.
CONCLUSIONS: The study indicated that electrical burns occur most often in young adults in the workplace; therefore, policies should be developed to raise safety awareness in the workplace. Despite the severity of the injury, patients with adequate clinical support and early surgical evaluation are more likely to survive, even with high rates of amputation, confirming the need for more research on electroporation.
Keywords:
Burns; Electrical burns; Work accidents; Epidemiology.
RESUMO
INTRODUÇÃO: Avaliar cinco anos de análise epidemiológica e tratamento cirúrgico atualizado das queimaduras elétricas por alta voltagem.
MÉTODOS: Foi realizado um estudo descritivo, retrospectivo de corte transversal, no Centro de Terapia de Queimados Dr. Oscar Plaisant, do Hospital Federal do Andaraí, Rio de Janeiro, Brasil, no período de janeiro de 2009 a dezembro de 2014. Foi aplicado um formulário nos prontuários dos 38 pacientes incluídos no estudo, a fim de avaliar as variáveis definidas.
RESULTADOS: Foram analisados 38 pacientes por queimadura elétrica de alta voltagem, sendo 95% dos casos do sexo masculino, com faixa etária entre 21-42 anos. O local de ocorrência mais frequente foi o trabalho, em 55,3%. A porcentagem de SCQ variou de 1-60%. A parte do corpo mais acometida foi a mão esquerda, em 55,26%. O preparo pré-cirúgico para autoenxertia foi necessário em 34,21%, sendo a média de tempo transcorrido 37,5 dias, o tipo de tratamento cirúrgico foi desbridamento seriado sob anestesia geral em 100%, autoenxertia em 31,6%, amputação em 18,4% e fasciotomia em 5,3% dos pacientes. A taxa de óbito foi de 0%.
CONCLUSÕES: O estudo observou que as queimaduras elétricas ocorrem mais frequentemente em adultos jovens no local de trabalho, portanto, é necessário desenvolver políticas de sensibilização para a segurança no local de trabalho. Apesar da gravidade da lesão, pacientes com suporte clínico adequado e avaliação cirúrgica precoce têm mais probabilidade de sobreviver, mesmo com altas taxas de amputação, confirmando a necessidade de mais pesquisas sobre a eletroporação.
Palavras-chave:
Queimaduras; Queimaduras elétricas; Acidentes de trabalho; Epidemiologia.