

Original Article - Year 2012 - Volume 27 -
Evaluation of depressive symptoms in patients with venous ulcers
Avaliação de sintomas depressivos em pessoas com úlcera venosa
ABSTRACT
BACKGROUND: Venous ulcers play an important role in patients' lives, as the incidence of deformities caused by this type of wound might produce adverse consequences, including psychosocial disorders. The objective of this study is to evaluate the occurrence of depressive symptoms presented by patients with venous ulcers.
METHODS: An exploratory, descriptive, analytical, and cross-sectional study was conducted at the Outpatient Wound Clinic of the Hospital Set within the State of São Paulo. The data were collected by interviews between December 2008 and April 2009 after approval of the research project by the Research Ethics Committee of the Federal University of São Paulo (CEP-1611/08). The Beck Depression Inventory was the instrument of the study.
RESULTS: Sixty patients participated in the survey. The majority (91.66%) showed some level of depression. There was a higher frequency of symptoms ranging from mild to moderate (n = 39; 65%). All levels of depression showed statistical differences. The five symptoms most commonly found were sadness, distorted body image, self-depreciation, decreased libido, and social withdrawal. Symptoms less represented were suicidal ideation and loss of appetite, each mentioned by only one patient. Forty-three patients were over 61 years old. Of these, 38 (88.4%) had depressive symptoms ranging from mild to severe.
CONCLUSIONS: The data obtained and evaluated by the Beck Depression Inventory allow the conclusion that patients with venous ulcers present different levels of depressive symptoms.
Keywords: Depression. Self concept. Quality of life. Varicose ulcer.
RESUMO
INTRODUÇÃO: A úlcera venosa assume grande importância na vida dos pacientes, pois a ocorrência de deformidades causadas por esse tipo de ferida pode gerar consequências adversas, as quais incluem distúrbios psicossociais. O objetivo deste estudo é avaliar o nível de ocorrência de sintomas depressivos apresentados pelos pacientes com úlcera venosa.
MÉTODO: Estudo exploratório, descritivo, analítico e transversal, realizado no Ambulatório de Feridas de um Conjunto Hospitalar, localizado no interior do estado de São Paulo. Os dados foram coletados por meio de entrevistas, no período compreendido entre dezembro de 2008 e abril de 2009, após aprovação do projeto de investigação pelo Comitê de Ética em Pesquisa da Universidade Federal de São Paulo (CEP-1611/08). Foi utilizado o Inventário de Avaliação de Depressão de Beck.
RESULTADOS: Participaram da pesquisa 60 pacientes. A maioria (91,66%) apresentou algum nível de depressão. Houve maior frequência de sintomas no nível leve a moderado (n = 39; 65%). Todos os níveis apresentaram diferença estatística. Os cinco sintomas mais encontrados foram: tristeza, distorção da imagem corporal, autodepreciação, diminuição da libido e retração social. Os sintomas menos representados foram ideia suicida e perda do apetite, sendo referidos por um paciente em cada aspecto. Quanto à idade, 43 pacientes tinham mais de 61 anos, dos quais 38 (88,4%) apresentavam sintomas depressivos no nível leve a grave.
CONCLUSÕES: Os resultados obtidos por meio do Inventário de Avaliação de Depressão de Beck permitiram concluir que pacientes com úlcera venosa apresentam níveis diferentes de sintomas depressivos.
Palavras-chave: Depressão. Auto-imagem. Qualidade de vida. Úlcera varicosa.
The presence of chronic ulcers in the lower limbs affects up to 5% of the adult population in the western countries, causing a significant socioeconomic impact. Its etiology is associated with several factors, such as chronic venous disease, peripheral arterial disease, neuropathies, arterial hypertension, physical trauma, sickle cell anemia, skin infections, inflammatory diseases, neoplasias, and nutritional changes1.
Studies show a prevalence of venous ulcers around 0.3%1,2. Their incidence increases with age, exceeding 4% in people over 65 years old and 1% of the adult population with a history of active or scarred ulcers; therefore, they are considered a serious problem for public health1,2.
Venous ulcers are a chronic disease that is characterized by periods of exacerbation and remission. Their long healing process generates physical and psychological discomfort. Restrictions resulting from the resulting treatment alter the individual's way of life and interfere with the daily activities of the individual3-5.
The population most affected by venous ulcers is the elderly, who have, in addition to the wound, a decline in their activities because of their chronic degenerative diseases. Emotional support and mechanisms to face this situation are therefore required, since these people often have shaken emotions and feelings.
Having a wound, with its associated exudate, odor, pain, and difficulty healing, limited the individual's possibilities to transform his/her existence. Family, social, and leisure relationships are important for the recovery of these injured people, and the lack of these activities might lead to a reduction in their quality of life, lowered self-esteem, anxiety, and depression5.
A study on the prevalence of anxiety and depression in 190 patients with chronic venous ulcers performed using the Hospital Anxiety and Depression Scale (HADS) revealed that 52 (27%) patients with depression and 50 (26%) were classified as anxious. The two symptoms associated with anxiety and depression were pain and odor3.
Pain and quality of life ratings among 233 females and 148 males were evaluated in a study of patients with chronic ulcers using the SF-12 survey and the visual analogue scale (VAS). Women reported more pain and worse quality of life than men. A direct correlation between pain and quality of life was detected. The authors concluded that vascular ulcers are very painful and result in poor quality of life, with a decline in self-esteem and depression6.
Depression is considered one of the ten leading causes of disability worldwide, limiting performance in physical, social, and personal activities. However, only a small number of affected people receive an appropriate treatment.
The way the population identifies symptoms of depression (and their beliefs about the etiology of depression) might influence the processes of seeking help and treatment consent and the community's attitude and behavior toward people with this disorder7.
However, depression has been underdiagnosed, undertreated, and undetected by the doctor in around 50-60% of the cases. In addition, depressed patients very often receive an inadequate and non-specific treatment. The morbidity associated with depression might be largely (around 70%) prevented with the correct treatment8.
Venous leg ulcers play an important role in the patient's life, as the incidence of deformities caused by this type of wound might induce adverse consequences, including psychosocial disorders.
Investigation and treatment of depression, especially in the practice of health professionals treating people with skin wounds, is not always emphasized as a benefit to increase the patient's quality of life, self-esteem, or self-image. In keeping with this notion, the present study is aimed to evaluate the incidence of depressive symptoms reported by patients with venous ulcers.
METHODS
An exploratory, descriptive, analytical, cross-sectional study was conducted at the Outpatient Wound Clinic of the Hospital Set in the State of São Paulo.
The criteria for inclusion in the study were as follows: diagnosis of venous ulcers by a vascular surgeon, age over 18 years old, and treatment at the outpatient wound clinic.
We excluded patients who, according to the evaluation of the investigator, presented physical or mental conditions that prevented them from answering the questions of the survey.
The data were collected by interviews between December 2008 and April 2009 after approval of the research project by the Research Ethics Committee of the Federal University of São Paulo (CEP-1611/08).
The data were collected by researchers after obtaining, in writing, the free informed consent of each patient in a previously prepared room, guaranteeing comfort and tranquility to the interviewee.
The study used the Beck Depression Inventory8,9 as an instrument to measure and self-evaluate depression. It is employed in the clinic, in research, and is considered to be a complement to patient evaluation10.
The inventory presents 21 categories of symptoms and attitudes typical of depression and each one is rated in terms of four different degrees of intensity of manifestation (0-3 points), totaling 63 points.
For this study, the following scores were considered: less than 9 (no or minimal depression), 10-18 (mild to moderate depression), 19-29 (moderate to severe depression), and 30-63 (severe depression)9.
The validation and reliability verification of the Beck Depression Inventory were carried out in three samples: first, the profile of scores obtained in a sample of Brazilian undergraduate students was assessed with the Beck Depression Inventory and compared to profiles obtained with different versions in terms of languages and cultures. The internal consistency of the Beck Depression Inventory was high (0.81), and the general pattern of results confirmed the validity of the Portuguese version of the survey. In the second study, the Portuguese version of the Beck Depression Inventory was assessed by obtaining its profile in three samples: undergraduate students, patients with panic, and patients with depression. In the third study, other psychometric properties, such as gender differences in depressive symptoms, were investigated by factorial and discriminant analysis in a large non-clinical sample of undergraduate students. Regarding reliability, the internal consistency of the scale was 0.81 for the full sample, 0.76 for the subsample of males, and 0.83 for females. In the validation study, the internal consistency of the sample for depressed patients was 0.88.
Data analysis was performed employing the SPSS software package version 15.0; chi-squared tests of independence and Kruskal-Wallis tests were used.
For all statistical tests, the level of significance was set at 5% (P < 0.05).
RESULTS
Sixty patients participated in the survey and the majority (91.66%) presented some level of depression (Table 1). There was a higher incidence of symptoms in the range from mild to moderate (n = 39, 65%). All levels showed statistical differences.

As shown in Table 2, the five most common symptoms were sadness, body image distortion, self-depreciation, decreased libido, and social withdrawal. The less-represented symptoms were suicidal ideation and loss of appetite, each one described by a patient.

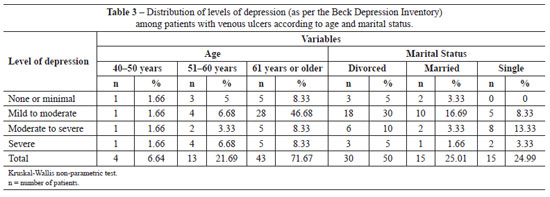
In terms of age, 43 patients were over 61 years old, among whom 38 (88.4%) presented depressive symptoms ranging from mild to severe. Of 51 (85.01%) white patients, 22 (36.69%) presented depression ranging from mild to moderate. Regarding marital status, there was a predominance of divorced patients. However, depressive symptoms also appeared in single, married, and separated people. There were statistically significant differences in rates of depression in terms of age group and marital status (P = 0.001) (Table 3).
In the sample studied, the majority of the patients were female individuals, who presented an intensity of depressive symptoms that ranged from mild to severe (Table 4).

DISCUSSION
People with wounds might isolate themselves; this occurs when the patient is moved by fear to suffer as a result of skin injury, pain, odor, and exudate.
Consequently, because of the difficulties of facing this inconvenience, patients suffering from injuries avoid social contact, become more isolated, and thus develop anxiety, depression, and mental disorders that affect their physical and psychological functioning5.
Depressive disorder is very prejudiced in terms of personal and familiar life, affecting twice as many women as men10. In 1990, depression was estimated to be the fourth-most-common specific cause of disability when a global scale of comparison between various diseases was used. The estimate for 2020 is that it will be the second-leading cause in developed countries and first-place in developing countries10.
In this study, 39 patients presented mild to moderate depression; this constitutes an incidence rate that is higher than the one shown by Duarte & Rego11, who found that 10-20% of patients with clinical diseases present depressive symptoms and about 5% have serious complications.
Using a version of the Beck survey validated by Gorestein and Andrade12 in patients with chronic indiscriminate wounds, it was found that the majority of individuals presented depression ranging from mild to moderate.
Other researchers have reported that when a patient gets an ulcer, several changes occur in his/her lifestyle regarding leisure, pain, social restriction, school, locomotion, and alteration in physical appearance that might lead the patient to experience depression13-15. Several studies of venous ulcer patients reveal that over 50% presented depression, results that confirm the findings of this study13-15.
Depressive symptoms manifested by negative body image, sadness, self-depreciation, and decreased libido shown in this study were similar to those identified in a previous work that investigated the relationship between depression and chronic comorbidities, although using different evaluation methods3,16.
In this research, the majority of the patients were elderly (71.67%) females (58.35%) who presented intensities of depressive symptoms that ranged from mild to severe.
Currently, it is known that depression is 50-75% more diagnosed in women than in men; however, the causes of this difference are unknown. Hormonal factors, genetic predisposition linked to the X chromosome, and even cultural factors are associated with causes of depression, which is more detectable in females given their higher tendency to express emotions and search for treatment14. However, this study found no significant differences in depression rates on the basis of gender or depressive symptoms.
Studies have shown that ulceration affects work productivity and functional capacity, sometimes leading to disability retirement or restriction of the activities of daily life and leisure.
For many patients, chronic diseases associated with wounds cause pain, loss of mobility/functional capacity, and decreased quality of life, resulting in anxiety and depression5,13,15,17.
Several authors have found a correlation between functional disability and health factors, among other correlations. Health self-perception seems to be the factor most strongly related to functional disability in Brazilian elderly people, followed by chronic diseases15.
In this context, it is worth emphasizing that humor-related depressive disorders are more frequent in elderly, being the fourth-leading cause of disability in the social world.
The growth of the elderly population is a factor of increasing importance, as it already exceeds the growth rate of the total population.
In a study in which depression was assessed in patients with leg ulcers, the authors found that women aged above 60 years presented alterations in the level of depression3,14,16,18. Depression appeared elevated in all of the age groups, which demonstrated that the environment and their expectations of the procedures might be considered stressful factors by this population. Health care in this age group has become a global concern.
There were no statistically significant differences in the presence of ulcers and age among patients with depressive symptoms. The elderly with wounds are precisely in whom this disorder occurs.
The elevated rate of wounds in this population is a circumstance that is known by health professionals and has generated several discussions. Health care of people with wounds is a significant problem that represents a challenge to be faced daily by patients and their caregivers.
Having an ulcer provokes a series of changes in peoples' lives and, consequently, in their relatives' lives, creating difficulties for which they are often not prepared3,14,15.
Ulceration in the lower limbs of the elderly is a condition that leads the patient to social isolation as a result of worsening mobility, reduced functional ability, and pain, causing decreased quality of life, low self-esteem, compromised self-image, and depression3,19.
Depression in the elderly is an important problem in public health given its high prevalence, frequent association with chronic diseases, negative impact on quality of life, and risk of suicide.
In keeping with this notion, clinical diseases might contribute to the pathogenesis of depression via direct modulation of brain function or psychological or psychosocial effects3,5,9-17.
The increased frequency of depressive symptoms among the widowed, divorced, and separated (compared to that among the single and married) suggests a correlation between living without a partner and high incidence of depression. In addition, people who live alone appear to be more vulnerable.
It was found in this sample that most of the patients with depressive symptoms were separated or single women (68.98 %), whereas among married people, the incidence rate of depression was 21.98%, a difference that presented statistical difference (P = 0.001).
People with wounds need to be helped to understand that the lesion is not a restriction against a social and sexual life but needs to be seen as a new condition that requires adaptation.
Because it is difficult to coexist with a situation that involves changes, it becomes necessary to seek the help of a professional to make the patient feel supported and motivated to seek further help.
The results of this study indicate the need to redirect assistance to patients with wounds. A search for and identification of emotional disorders among these patients is recommended in health services, hospitals, outpatient clinics, and home care.
Considering the needs arising in past decades, the increase in chronic diseases and the number of people with wounds makes it necessary to redirect academic training and qualification of health professionals, valuing not only content but also care practice.
This initial contribution to a theme suggests that future studies need to be performed that increase the sample size in order to describe the influence of other variables and understand the magnitudes and consequences of possible changes in the emotional sphere for patients with venous ulcers.
Actions to address chronic diseases and mental health will certainly contribute to the welfare and quality of life of people who live with chronic ulcers, especially the elderly.
CONCLUSIONS
The results obtained when we administered the Beck Depression Inventory allow us to conclude that patients with venous ulcers present various levels of depressive symptoms.
REFERENCES
1. Reichenberg J, Davis M. Venous ulcers. Semin Cutan Med Surg. 2005;24(4):216-26.
2. Maffei FH, Magaldi C, Pinho SZ, Lastoria S, Pinho W, Yoshida WB, et al. Varicose veins and chronic venous insufficiency in Brazil: prevalence among 1755 inhabitants of a country town. Int J Epidemiol. 1986;15(2):210-7.
3. Jones J, Barr W, Robinson J, Carlisle C. Depression in patients with chronic venous ulceration. Br J Nurs. 2006;15(11):S17-23.
4. McMullen M. The relationship between pain and leg ulcers: a critical review. Br J Nurs. 2004;13(19):S30-6.
5. Finlayson K, Edwards H, Courtney M. The impact of psychosocial factors on adherence to compression therapy to prevent recurrence of venous ulcers. J Clin Nurs. 2010;19(9-10):1289-97.
6. Guarnera G, Tinelli G, Abeni D, Di Pietro C, Sampogna F, Tabolli S. Pain and quality of life in patients with vascular leg ulcers: an Italian multicentre study. J Wound Care. 2007;16(8):347-51.
7. Peluso ETP, Blay SL. Percepção da depressão pela população da cidade de São Paulo. Rev Saúde Pública. 2008;42(1):41-8.
8. McQuaid JR, Stein MB, Laffaye C, McCahill ME. Depression in a primary care clinic: the prevalence and impact of an unrecognized disorder. J Affect Disord. 1999;55(1):1-10.
9. Beck AT, Ward CH, Mendelson M, Mock J, Erbaugh J. An inventory for measuring depression. Arch Gen Psychiatry. 1961;4(6):561-71.
10. Calil HM, Pires MLN. Aspectos gerais das escalas de avaliação da depressão. Rev Psiq Clin. 1998;25(5):240-4.
11. Duarte MB, Rego MAV. Comorbidade entre depressão e doenças clínicas em um ambulatório de geriatria. Cad Saúde Pública. 2007;23(3):691-700.
12. Gorenstein C, Andrade L. Validation of a Portuguese version of the Beck Depression Inventory and the State-Trait Anxiety Inventory in Brazilian subjects. Braz J Med Biol Res. 1996;29(4):453-7.
13. Mapplebeck L. Case study: psychosocial aspects of chronic bilateral venous leg ulcers. Br J Community Nurs. 2008;13(3):S33-4, S36, S38.
14. Jones JE, Robinson J, Barr W, Carlisle C. Impact of exudate and odour from chronic venous leg ulceration. Nurs Stand. 2008;22(45):53-4.
15. Pieper B, Vallerand AH, Nordstrom CK, DiNardo E. Comparison of bodily pain: persons with and without venous ulcers in an indigent care clinic. J Wound Ostomy Continence Nurs. 2009;36(5):493-502.
16. Palfreyman S. Assessing the impact of venous ulceration on quality of life. Nurs Times. 2008;104(41):34-7.
17. Salomé GM, Blanes L, Ferreira LM. Capacidade funcional dos pacientes com diabetes mellitus e pé ulcerado. Rev Acta Paul Enferm. 2009;22(4):412-6.
18. Longo Jr. O, Buzatto SHG, Fontes OA, Miyazaki MCO, Godoy JMP. Qualidade de vida em pacientes com lesões ulceradas crônicas na insuficiência venosa de membros inferiores. Cir Vasc Angiol. 2001;17(1):21-6.
19. Alves LC, Leite IC, Machado CJ. Fatores associados à incapacidade funcional dos idosos no Brasil: análise multinível. Rev Saúde Pública. 2010;44(3):468-78.
1. Nurse on the Faculty of Nursing and Obstetrics of Passos, nursing specialist in the Intensive Care Unit of the University Center of São Camilo, stomal therapy specialist at the University of Taubaté, professor on Nurse Graduation Course at Universidade do Vale do Sapucaí, master's and doctorate in Health Science from the Universidade Federal de São Paulo (Federal University of São Paulo), São Paulo, SP, Brazil.
2. Nurse at the Universidade Federal de São Paulo (Federal University of São Paulo), stomal therapy specialist at the Universidade de São Paulo (University of São Paulo), master's and doctorate in science from the post-graduate program in plastic surgery of the Universidade Federal de São Paulo (Federal University of São Paulo), assistant professor at the Universidade Federal de São Paulo (Federal University of São Paulo), São Paulo, SP, Brazil.
3. Full Professor of plastic surgery at the Universidade Federal de São Paulo (Federal University of São Paulo), São Paulo, SP, Brazil.
Geraldo Magela Salomé
Av. Francisco de Paula Quintaninha Ribeiro, 280 - ap. 134 - Jabaquara
São Paulo, SP, Brazil - CEP 04330-020
E-mail: salomereiki@yahoo.com.br
Submitted to SGP (Sistema de Gestão de Publicações/Manager Publications System) of RBCP (Revista Brasileira de Cirurgia Plástica/Brazilian Journal of Plastic Surgery).
Article received: January 14, 2012
Article accepted: March 7, 2012
Study conducted in the Outpatient Wound Clinic of the Hospital Set of Sorocaba, Sorocaba, SP, Brazil.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter