

Original Article - Year 2026 - Volume 41Issue 1
Retrospective Analysis of the Use of Steel Wires and Dermotraction for Gradual Closure of Complex Wounds in a Reference Trauma Hospital in Paraná
Análise retrospectiva do uso de fios de aço e dermotração para fechamento gradual de feridas complexas em um hospital de referência em trauma do Paraná
ABSTRACT
Introduction Materials and
Methods We evaluated 64 medical records of patients undergoing dermotraction with steel wires or ES for the treatment of complex wounds. The study involved 58 patients undergoing dermotraction, including 50 with KWs, 6 with ES, and 2 using KWs plus ES.
Results The average length of stay was 82.54 days for patients using KWs, 26.8 daysfor those using ES, and 20 days for those using a combination of KWs and ES. In terms of complications, 6% of the patients using KWs suffered loss of traction, 2% presented with suture dehiscence, and 2% had deep vein thrombosis. Patients undergoing treatment with ES or KWs plus ES presented no complications.
Conclusion In the present study, patients using KWs, ES, or both achieved complete closure of the lesions. These techniques were cheap and highly effective in closing complex lesions.
Keywords: wound healing; surgery; plastic; wound closure techniques; suture techniques; traction
RESUMO
Introdução Feridas complexas consistem em perda de substância cutânea associada à grande extensão, infecção, inviabilidade de tecidos ou associadas a doenças sistêmicas. A dermotração é feita coma colocação de fios de aço, como os de Kirschner (FKs), paralelos aos bordos da ferida, com tração distribuída igualmente, a cada 24 a 48h. A sutura elástica (SE) é a colocação de fios elásticos nas bordas da ferida com tração contínua, permitindo um fechamento de forma gradual, quando não é possível fechar por primeira intensão.
Materiais e Métodos Foram avaliados 64 prontuários de pacientes que tenham passado pela dermotração comfios de aço ou SE para tratamento de feridas complexas. Ao todo, foram incluídos 58 pacientes no estudo, sendo que, destes, 50 pacientes utilizaram FKs para dermotração, 6 usaram SE e 2 usaram ambas as técnicas.
Resultados Para os pacientes que usaram FKs, a média de internamento em dias foi de 82,54; para os que usaram SE, foi de 26,8; e para os que usaram tração mista, 20. Quanto às complicações, no grupo FK observou-se perda de tração em 6%, 2% com deiscência de sutura e 2% com caso de trombose venosa profunda (TVP). Não foram descritas complicações nas demonstrações mistas e por SE.
Conclusão Neste estudo, tanto os pacientes com FKs quanto os que tiveram suas suturas realizadas com SE obtiveram fechamento total das lesões, e ambas as técnicas demonstraram baixo custo e alta efetividade para o fechamento de lesões complexas.
Palavras-chave: cicatrização; cirurgia plástica; técnicas de fechamento de ferimentos; técnicas de sutura; tração
Introduction
Complex wounds involve extensive skin loss associated with infection, lack of viability of superficial tissues, or systemic diseases. These wounds do not follow the expected, orderly, and timely repair sequence and do not present anatomical and functional integrity restoration after three months of proper treatment. They are more common in trauma, diabetes, pressure ulcers, and chronic venous ulcers with necrosis or autoimmunity.1,2 They carry a high risk of complications, including amputations and death.2
In this regard, achieving safe, functional, aesthetic, and system-friendly outcomes requires creativity in making technical decisions between treatment options, with a special emphasis on cost reduction.1
In addition to flaps and grafts, tissue expansion is an alternative closure method. In reconstructive surgery, this model maintains the form and function of the affected site. As such, elastic sutures and traction wires, such as Kirschner wires (KWs) and steel wires, can successfully close complex wounds.3
Elastic sutures (ESs) involve placing elastic threads between knots tied at the wound edges, creating a crisscross effect similar to a shoelace knot, with continuous tension. Two to three days after placement, the surgeon increases the elastic tension by stretching and tying the elastic thread. This adjustment allows for gradual wound closure with reduced morbidity and may be an alternative to grafts or microsurgery. However, despite its applicability in fasciotomies and laparotomies, its use in larger wounds remains uncertain, mainly due to the small number of studies.4
Dermotraction involves the subdermal placement of steel wires, such as KW, parallel to the wound edges. Next, tension bands are placed around the two interposed steel wires to apply an evenly distributed traction to approximate the wound edges. Retraction can occur every 24 to 48 hours, often within 24 hours. Wire removal occurs after edge approximation with no tension.5 This technique has been described as being used in wounds resulting from infection, bone fractures, fasciotomies, pressure ulcers, flap closure (potentially avoiding the use of a graft or flap), and in one case of bilateral mastectomy undergoing intraoperative traction.6 However, established guidelines and indications for this technique are still lacking.
Objectives
The present study aimed to report the outcomes of patients with complex wounds who underwent dermotraction using steel wires and ES, including the treatment’s cost-effectiveness and the length of postoperative hospital stay. Moreover, the study aimed to describe the surgical technique used at a referral trauma hospital and analyze the progress and outcomes of patients who used steel wires for the gradual closure of complex wounds compared with those who used other materials.
Materials and Methods
The Research Ethics Committee CEPSH-SESA/HT approved the current study under number CAAE 64890722.0.0000.5225.
Sixty-four patients underwent treatment at the Department of Plastic Surgery of Complexo Hospitalar do Trabalhador from 2012 to 2022. The study included patients aged 18 or older undergoing complex wound treatment with dermotraction using steel wire or ES, who had signed the free informed consent form (ICF). We excluded underage subjects and those who did not undergo dermotraction with KW or ES.
From the selected sample, we performed a retrospective, descriptive cross-sectional study by collecting and reviewing data from electronic medical records of patients admitted to Complexo Hospitalar do Trabalhador for complex wound treatment with dermotraction. Complex wounds included fasciotomies, pressure, diabetic, venous, venous insufficiency, and infected ulcers, or lesions with a closure period longer than 3 weeks.
We collected the following data from medical records: medical record number, age, gender, wound etiology, wound classification, lesion size, lesion location, exposure time before plastic surgery intervention, type of surgery, material used in surgery (thread), anesthesia, number of surgical approaches, number of cycles for tension increase, time until closure, length of hospital stay, whether the closure was successful, associated complications, comorbidities (diabetes, systemic arterial hypertension [SAH], venous insufficiency, HIV, autoimmune disease, heart failure, coagulopathy), cost of materials, and case outcome.
Data analysis included descriptive and exploratory statistics, with calculations of absolute and relative frequencies, measures of central tendency (mean and median), and dispersion (standard deviation). This analysis was performed using the IBM SPSS Statistics for Windows (IBM Corp.) software, version 25.0.
Results
Table 1 shows the clinical characteristics, demographics, and outcomes of patients undergoing dermotraction with each technique.
| Variable | Total (n = 58) | KW (n = 50) | ES (n = 6) | KW plus ES (n = 2) | Notes |
|---|---|---|---|---|---|
| Gender (male/female) | 46/12 | 40/10 | 4/2 | 2/0 | - |
| Average age (years) | 37.88 ± 13.27 | 37.88 ± 12.91 | 35.6 ± 17.67 | 43.5 | Age range: 19-75 |
| Comorbidities | - | SAH (2), DM1 (1), DM2 (1), other (4) |
SAH (2), DM2 (1) | - | Includes CAD, AMI, Crohn’s disease, stroke, and obesity |
| Wound location | - | LLL (36%), RLL (28%), other |
LLL (50%), RLL (33%), foot (17%) |
LLL (1), RLL (1) |
- |
| Averagae wound size (cm) | - | 17.7 ± 5.68 | 15.33 ± 8.08 | 22 | - |
| Time until dermotraction (days) | - | 22.76 | 34 | 41.3 | Preoperative |
| Length of stay (days) | - | 82.54 | 26.8 | 20 | - |
| UCI admission (%) | - | 28% | 16.6% | 50% | - |
| Previous infection (%) | - | 42% | 50% | 100% | - |
| Number of surgeries (average) | - | 3 | 3 | 2 | - |
| Outpatient procedures | - | 1 | 0 | 0 | - |
| Number of tractions | - | 1 | 1 | 2 | - |
| Complications | - | Loss of traction (6%), dehiscence (2%), DVT (2%) |
None | None | - |
| Wound closure | 100% | 100% | 100% | 100% | In all groups |
Abbreviations: CAD, Chronic arterial disease; DM1/DM2, type 1/type 2 diabetes mellitus; KW, Kirschner wire; SAH, systemic arterial hypertension; AMI, acute myocardial infarction; LLL/RLL, left/right lower limb; ES, elastic suture; DVT, deep vein thrombosis; UCI, intensive care unit.
Note: Mean values.
The study included 58 patients undergoing dermotraction, 50 with KW, 6 with ES, and 2 with KW plus ES. The sample comprised 12 women and 46 men, with a mean age of 37.88 years (± 13.27), ranging from 19 to 75 years old. The average age per technique was 37.88 years (± 12.91; range: 19-75) for KW, 35.6 years (± 17.67; range: 19-58) for ES, and 43.5 years (range: 35-48) for KW plus ES. Regarding comorbidities, among the patients undergoing elastic suture, 2 had systemic arterial hypertension (SAH) and 1 had type-2 diabetes mellitus (DM). Of those who underwent dermotraction with KW, 2 had SAH, 1 had type-2 DM, 1 had type-1 DM, 1 had Crohn’s disease, 1 had grade-II obesity, 1 had had a stroke, and 1 had chronic arterial disease and an acute myocardial infarction with previous revascularization.
Wound etiology included 28 cases of traumatic soft-tissue injuries, 19 fasciotomies, 5 surgical wound infections, 3 nonsurgical soft-tissue infections, 1 burn, 1 dog bite, 1 surgical access, and 1 flap donor site complication. Therefore, approximately 80% of the injuries presented a traumatic origin.
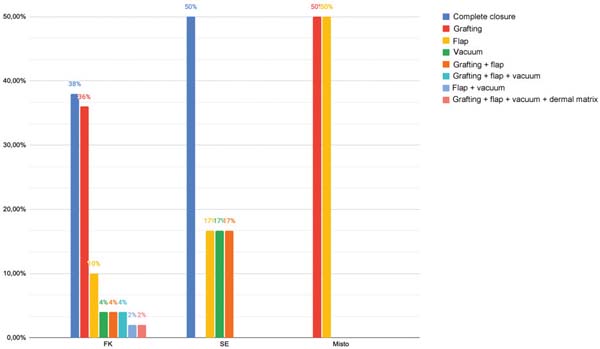
Lesion location in patients receiving KW included 36% cases on the left lower limb, 28% on the right lower limb, 6% on the right foot, 6% on the chest, 4% on the abdomen, 4% on the head, 4% on the left upper limb, 2% on the right upper limb, 2% on both lower limbs, 2% on the left foot, and 2% on the sacrum. In subjects receiving ES, 50% of the wounds were on the left lower limb, 33.3% on the right lower limb, and 16.67% on the left foot. In patients undergoing both techniques, one case affected the left lower limb and another, the right lower limb.
The mean documented wound length was 17.7 ± 5.68 cm in patients undergoing dermotraction with KW, 15.33 ± 8.08 cm in subjects undergoing ES, and 22 cm in patients submitted to the combined technique. The mean preoperative time until dermotraction plastic surgery was 22.76 days in subjects receiving KW, 34 days in those receiving ES, and 41.3 days in patients undergoing dermotraction with KW plus ES.
Regarding hospitalization time, the average length of stay was 82.54 days for patients undergoing dermotraction with KW, 26.8 days for those undergoing dermotraction with ES, and 20 days for those receiving both KW and ES. However, 50% of patients treated with KW plus ES required admission to the intensive care unit (ICU) compared with 16.6% of those treated with ES and 28% of cases using KW. In addition, 42% of wounds treated with KW traction presented with a previous infection, compared with 50% of those treated with ES and 100% of those undergoing treatment with KW plus ES.
Furthermore, regarding the number of surgical procedures, patients who underwent traction with KW had an average of three surgical procedures and one outpatient procedure. Patients undergoing ES treatment had on average three surgical procedures, and none of them required outpatient treatment in the emergency room. The number of traction procedures using KW plus ES was two, while patients who underwent KW and ES underwent, on average, one wire traction procedure during treatment.
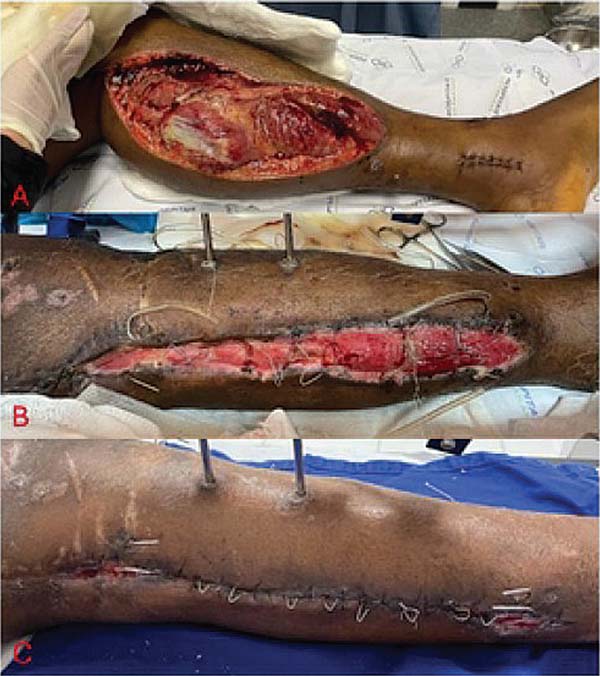
Concerning complications, subjects treated with KW presented traction loss in 6% of cases, suture dehiscence in 2%, and femoropedal deep vein thrombosis (DVT) in 2%. There were no complications in patients undergoing ES or KW plus ES treatment. All subjects presented complete wound closure (►Fig. 1).
Discussion
Indications for steel wire or elastic suture use
In plastic surgery, complex wounds are injuries requiring a longer time to heal (often with no spontaneous closure up to 3 months after trauma). These wounds may also present infection, compromised viability of superficial tissues, association with systemic diseases impacting proper wound healing (including DM and venous diseases), or significant and extensive loss of the integument.7
The first step in treating these extensive wounds is cleaning and debridement, followed by the creation of flaps or skin grafts. However, the need for a donor site for tissue removal often leads to local complications such as hypertrophic scars, skin retraction, local infection, or cosmetic deformities in a previously healthy area.8 In this context, the skin’s high elasticity can be an ally in the adoption of other therapeutic methods to aid the healing of large wounds, including the use of ES, since primary wound closure should be the first choice whenever possible.9
The ES suture technique involves attaching an elastic band to the wound edges with suture for skin traction due to its elasticity and cutaneous compliance, resulting in subsequent healing of the treated lesion. This technique is low-cost and relatively simple to perform, making it a good alternative for complex wounds.9 Anchoring the ES thread to the wound edges allows for better redistribution of forces during skin traction, minimizing tissue ischemia at the wound edges and, consequently, local necrosis. Furthermore, the tension applied to the skin enhances local metabolism, resulting in neovascularization and increased collagen fiber production, which in turn boosts the skin’s capacity for expansion. As such, the ES technique is widely indicated for medium to large complex wounds, especially in difficult-to-heal sites, including those with poor vascularization, as the distal third of the leg or the foot. Therefore, this technique is a good alternative for lesion resolution without the need to compromise another donor site for wound coverage.10
Another well-regarded, widely used technique for closing large, complex lesions is intermittent skin traction with KW. This technique is low-cost, has low morbidity, and is easy to apply. It offers good outcomes in preventing the development of new dysfunctional scars compared with flaps, which are more likely to result from ischemia and subsequent tissue necrosis, as well as in dysfunctional scars due to tissue retraction.9 Therefore, wire traction is a good technique for wound closure, especially in the lower and upper limbs, and it is also widely used for closing fasciotomies. The mechanism of action of wire traction is the drag forces applied to the skin’s collagen fibers, which elongate them and, when combined with displacement of the cutaneous ground substance, allow for an increase in the surface area for local coverage5 (►Fig. 2).
One of the key points for comparison when evaluating the applicability of steel wire traction with the ES technique seems to be the ability to use the steel wires in a controlled manner. The correct use of steel wires enables the adjustment of skin traction according to specific needs and potential for tissue expansion to accommodate the deformity. This approach helps minimize the risk that the inability of neovascularization to keep pace with tissue expansion will limit the effectiveness of the traction. As a result, this was the main reason why most patients included in the present study were candidates for wire traction rather than the ES technique.11
Relationship of the wound size with the technical choice and follow-up
Olsson et al.7 (2018) stated that the selection of a surgical technique considers several variables, including safety, aesthetics, functionality, favorable results for the system, and lower costs. In the present study, we observed that wound size influenced the choice of therapeutic approach, with larger wounds (mean length, 17.7 ± 5.68 cm) being frequently treated with KW and smaller wounds (mean length, 15.33 ± 8.08 cm) with ES.
It is worth noting that our patients had different trauma mechanisms, ages, and comorbidities, resulting in variations in preoperative time, hospital stay, and complications. Moreover, there was no standard protocol for selecting the surgical approach. The preoperative time was shorter in patients receiving KW (22.76 days) than those receiving ES (34 days) or KW plus ES (41.3 days). Patients undergoing dermotraction with KW plus ES had a shorter hospital stay (average of 20 days) compared with those receiving KW (82.54 days) and ES (26.8 days).
Concerning complications, dermotraction with KW resulted in loss of traction in 6% of patients, suture dehiscence in 2%, and femoropedal DVT in 2% of cases. There were no complications after dermotractions using ES or KW plus ES, consistent with the findings by Santos and Oliveira (2012), who evaluated ES in the closure of 14 wounds and reported no intercurrences.
Cost-effectiveness of each technique
In our study, both patients treated with KW and ES presented complete wound closure. The complication rate was 10%, with loss of traction in 6% of patients, suture dehiscence in 2%, and femoropedal DVT in 2% of cases. These data are consistent with those described by Jauregui et al.8 (2017) in both effectiveness and complication rates.
Kirschner wire and ES are low-cost and highly effective in closing complex or difficult-to-manage lesions. Both are safe and inexpensive options, available through the Brazilian Unified Health System (SUS, Sistema Único de Saúde, in Portuguese),whichfacilitatestheresolutionof these lesions as they do not require expensive equipment for follow-up.5 In a systematic review, Obuh et al.12 (2023) reinforced the cost-effectiveness of dermotraction, especially in resource-limited settings. The technique is cheap, provides good aesthetic outcomes, and requires fewer additional interventions. Therefore, it is indicated as an initial approach for closing complex wounds, such as those from fasciotomy.7,12
Challenges in dermotraction techniques
Dermotraction is a surgical procedure for optimal wound closure that uses traction to unite lesion edges by applying tangential forces to the skin surface. Today, the most widely used and studied dermotraction technique employs KW.4 Compared with tissue expansion using silicone rods, steel wires allow for greater preservation of healthy periwound tissue due to the controlled cutaneous traction. However, this does not exclude the possibility of rupture of the skin anchored to the traction wires, a potential complication of this technique.10
Regarding techniques that use internal devices or balloons for tissue expansion, the implant may still present areas of pericapsular fibrosis. Nevertheless, these disadvantages do not imply a lesser recommendation for the adoption of steel wire or ES techniques for closing complex wounds. Their low cost, ease of application, and aesthetic-functional outcomes are more promising than other approaches to treat these lesions.1
Benefits of dermotraction as an initial approach
Góes et al. (2004) reported that closure by tissue expansion allows traction and mechanical drag forces to lead to the stretching of the skin and collagen fibers. As such, it maintains the shape and function of the affected site, making dermotraction a useful tool in reconstructive surgery.
The dermotraction technique reduces hospitalization and treatment costs. Moreover, it does not require high-cost equipment and is a safe and functionally effective technique according to Figueiredo et al.6 (2011). Compared to flaps, dermotraction lowers the risk of tissue necrosis by maintaining vascularization through progressive traction, preventing tissue retraction, and minimizing the likelihood of dysfunctional scars.s
Furthermore, as reported by Santos et al. (2019), skin retraction and muscle protrusion due to high-energy traumas and in some postfasciotomy cases prevent primary wound closure. In these lesions, tissue expansion is an essential and advantageous alternative, with a good costbenefit ratio.
Conclusion
Experience with dermotraction for complex wounds has demonstrated that both KW and ES are effective and viable alternatives for closing these lesions. Both techniques have yielded good functional and aesthetic outcomes, with a low complication rate and without the need for flaps or grafts in most cases.
The choice between techniques was closely related to the size and complexity of the wound, with steel wires being preferred in larger injuries or those requiring greater traction control, and ES use in smaller wounds, resulting in reduced hospital stay and good evolution.
Thus, our findings reinforce the cost-effectiveness of dermotraction as an initial approach for complex wounds, highlighting its safety, simplicity, and accessibility within SUS. Further comparative and prospective studies are recommended to standardize indications, techniques, and follow-up protocols for optimizing surgical outcomes and resource allocation.
References
1. Ferreira MC, Tuma P Jr, Carvalho VF, Kamamoto F. Complex wounds. Clinics (Sao Paulo) 2006;61(06):571-578. Doi: 10.1590/s1807-59322006000600014 PubMed
2. Bowers S, Franco E. Chronic wounds: evaluation and management. Am Fam Physician 2020;101(03):159-166
3. xPetragliaA Neto, TavaresFilho JM. Sutura elástica como alternativa para o primeiro atendimento da ferida na urgência. Rev BrasCirPlást2016;31(01):118-122.Doi:10.5935/2177-1235.2016RBCP0018
4. Lee C, Wang T, Chen C. Vessel loop shoelace technique followed by keystone flap to treat a large mid-back defect. . Plast Reconstr Surg Global Open. 2022;10(01):40-49. Doi: 10.1097/GOX.0000 000000004049 PubMed
5. Ismavel R, Samuel S, Boopalan PR, Chittaranjan SB. A simplesolution for wound coverage by skin stretching. J Orthop Trauma 2011;25 (03):127-132. Doi: 10.1097/BOT.0b013e318206f556 PubMed
6. Figueiredo JCA, Rosique RG, Maciel PT. Tração cutânea intraoperatória para fechamento de ferida após mastectomia bilateral higiênica: relato de caso. Rev Bras Cir Plást 2011;26(01):164-166. Doi: 10.1590/S1983-51752011000100029
7. Olsson M, Järbrink K, Divakar U, et al. The humanistic and economic burden of chronic wounds: A systematic review. Wound Repair Regen 2019;27(01):114-125. Doi: 10.1111/wrr.12683
8. Jauregui JJ, SJ Yarmis, Tsai J, Onuoha KO, Illical E, Paulino CB. Fasciotomy closure techniques: A meta-analysis. J Orthop Surg (Hong Kong) 2017;25(01):23-24. Doi: 10.1177/2309499016684724 PubMed
9. Bashir AH. Wound closure by skin traction: an application of tissue expansion. Br J Plast Surg 1987;40(06):582-587. Doi: 10.1016/0007-1226(87)90151-2 PubMed
10. Wagstaff MJ, Rozen WM, Whitaker IS, Schneider TN, Audolfsson T, Acosta R. Kirschner wires: a novel technique to assist abdominal closure utilising the viscoelastic properties of skin. J Plast Reconstr Aesthet Surg 2009;62(05):e115-e116. Doi: 10.1016/j.bjps.2008.09.007 PubMed
11. Park H, Copeland C, Henry S, Barbul A. Complex wounds and their management. Surg Clin North Am 2010;90(06):1181-1194. Doi: 10.1016/j.suc.2010.08.001 PubMed
12. Obuh OO, Esomu EO, Sydney RO. Suturing dermatotraction techniques in closing fasciotomy wounds: a systematic review. Cureus 2023;15(04):e37550. Doi: 10.7759/cureus.37550
1. Plastic Surgery, Medicine Program, Faculdades Pequeno Príncipe, Curitiba, PR, Brazil
2. Plastic Surgery Service, Medicine Program, Faculdade Evangélica Mackenzie do Paraná,
Curitiba, PR, Brazil
3. Plastic Surgery Clinic, Medicine Program, Universidade Positivo, Curitiba, PR,
Brazil
4. Plastic Surgery, Department of Medical Residency, Universidade Federal do Paraná,
Curitiba, PR, Brazil
5. Plastic Surgery Service, Universidade Federal do Paraná, Curitiba, PR, Brazil
Address for correspondence Giovana Knapik Batista, Disciplina de Cirurgia Plástica, Curso de Medicina, Faculdades Pequeno Príncipe, Curitiba, PR, Brazil (e-mail: giovanaknapikbatista@gmail.com ligas.cht@gmail.com).
Artigo submetido: 07/10/2024.
Artigo aceito: 14/07/2025.
Conflict of Interests
The authors have no conflict of interests to declare.





 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter