

Review Article - Year 2025 - Volume 40Issue 1
Limitations and Challenges in the Incorporation of Artificial Intelligence in Plastic Surgery: A Systematic Review
Limitações e desafios na incorporação da inteligência artificial em cirurgia plástica: Uma revisão sistemática
ABSTRACT
The present systematic review provides a comprehensive analysis of the current role of artificial intelligence (AI) in plastic surgery, focusing on its applications, outcomes, challenges, and limitations. Out of an initial pool of 213 articles, 74 studies were included after a rigorous selection process based on relevance and methodological quality. Among the AI technologies evaluated, augmented reality (AR) stands out as an emerging tool with significant potential to enhance visualization and planning in esthetic and reconstructive procedures. The use of AR facilitates advancements in volume projection, shape, and symmetry, helping to reduce patient anxiety and better align surgical expectations by offeringmore precise preoperative visualization. Despite the identified benefits, the implementation of these technologies faces considerable challenges. The lack of specific regulations and the need for adequate technical training for healthcare professionals are significant barriers to the full integration of AI into clinical practice. Additionally, the heterogeneity of studies and the lack of standardized outcomes make it difficult to generalize the observed benefits. The review concludes that, although the advances are promising, there is a critical need for further studies that address existing gaps and for robust regulations to ensure the safe and effective adoption of AI in contemporary plastic surgery.
Keywords: artificial intelligence; diagnosis; computer-assisted; machine learning; plastic surgery procedures; surgery; plastic
RESUMO
Esta revisão sistemática oferece uma análise abrangente do papel atual da inteligência artificial (IA) na cirurgia plástica, com ênfase em suas aplicações, resultados, desafios e limitações. A partir de uma base inicial de 213 artigos, 74 estudos foram incluídos após uma seleção rigorosa, considerando critérios de relevância e qualidade metodológica. Entre as tecnologias de IA avaliadas, a realidade aumentada (RA) destaca-se como uma ferramenta emergente com potencial significativo para melhorar a visualização e o planejamento de procedimentos estéticos e reconstrutivos. A utilização de RA permite avanços na projeção de volume, formato e simetria, e auxilia na redução da ansiedade dos pacientes e no alinhamento das expectativas cirúrgicas, ao oferecer uma visualização pré-operatória mais precisa. Apesar dos benefícios identificados, a implementação dessas tecnologias enfrenta desafios consideráveis. A ausência de regulamentação específica e a necessidade de treinamento técnico adequado para profissionais de saúde são barreiras significativas para a integração plena da IA na prática clínica. Além disso, a heterogeneidade dos estudos e a falta de padronização nos resultados dificultam a generalização dos benefícios observados. Conclui-se que, embora os avanços sejam promissores, há uma necessidade crítica de estudos adicionais que abordem as lacunas existentes e que sejam acompanhados por regulamentações robustas para assegurar uma adoção segura e eficaz da IA na cirurgia plástica contemporânea.
Palavras-chave: aprendizado de máquina; cirurgia plástica; diagnóstico por computador; inteligência artificial; procedimentos de cirurgia plástica
Introduction
Artificial intelligence (AI) has emerged as a new tool in several fields of medicine. Its ability to analyze large volumes of data and provide advanced decision-making support can transform clinical practices, improve surgical precision, and optimize patient outcomes.1-3Within plastic surgery, the incorporation of AI could theoretically improve diagnoses, surgical planning, and postoperative outcomes.
In recent years, the application of AI in plastic surgery has expanded significantly, ranging from preoperative planning, with the optimization of surgical design and planning, to intraoperative guidance, treatment decisions, and postoperative management of patients, denoting its versatility.4,5 Some of the technologies that have been explored to improve the surgical practice include machine learning models, convolutional neural networks to assess mammograms and distinguish benign from malignant tumors, and natural language processing.6-8 The use of neural networks to evaluate mammograms and differentiate benign from malignant tumors has shown results comparable to those obtained by medical experts, for example.5
The incorporation of AI also raises significant ethical and regulatory issues. Patient autonomy, respect for the general data processing law, informed consent, confidentiality, and proper metadata use are crucial considerations to ensure the ethical and effective implementation of AI in plastic surgery.2,4 Collaboration between plastic surgeons and computer scientists is essential to develop clinically-relevant and interpretable algorithms, minimizing systematic biases and assuring data representativeness.5,9 Transitioning these technologies into the daily clinical practice will require collaborative and ongoing efforts to validate performance and address recognized limitations.6
The present systematic review aims to explore the current AI applications in plastic surgery, discuss outcomes, challenges, and limitations, and outline future directions to integrate this technology into the daily clinical practice to understand its implementation within procedures and assess the quality and effectiveness of its interventions, as well as the potential limitations in the current literature. By providing a comprehensive overview of the capabilities and implications of AI, the current study aims to contribute to the advancement of plastic surgery and promote the safe and effective adoption of this emerging technology.
Materials and Methods
The present systematic review is registered in the International Prospective Register of Systematic Reviews (PROSPERO; ID 585318). A comprehensive search in the PubMed and LILACS databases was conducted in March 2024. The search strategy combined the descriptors Artificial Intelligence and Plastic Surgery to capture relevant articles in Portuguese, English, and Spanish on AI applications in plastic surgery, covering esthetic and reconstructive procedures.
Inclusion Criteria
The present review included articles meeting the following criteria:
Publication period - only articles published between January 2023 and March 2024 were eligible, ensuring that the studies reflected the most recent and relevant developments in AI applications in plastic surgery.
Language - we restricted inclusion to studies published in Portuguese, English, or Spanish, as long as they were available in full text, to enable a critical analysis with no language barriers.
Thematic relevance - we included only studies directly addressing the application of AI tools in plastic surgery procedures, such as augmented reality (AR), predictive algorithms, and machine-learning techniques.
Availability - we included only articles whose full text could be accessed, to ensure the availability of all relevant information for a detailed analysis.
Exclusion Criteria
We excluded articles that fell within the following categories: Thematic relevance - we excluded studies that did not directly address the application of AI tools in plastic surgery, such as manuscripts that did not specifically focus on plastic surgery or did not provide significant empirical data to the analysis.
Methodological quality - we excluded opinion articles, editorials, and correspondences to ensure the quality of the data for analysis.
Article selection occurred in two sequential stages. In the first, we identified 213 potentially-relevant articles for an initial screening of titles and abstracts. The second consisted of the full-text review of articles meeting the inclusion criteria. The application of the inclusion and exclusion criteria led to the selection of 74 articles for a detailed analysis. This careful process ensured that the review only included studies with good methodological quality, providing a comprehensive and up-to-date overview of AI use in plastic surgery.
Results
During the systematic review process, we initially identified 213 potentially-relevant articles for analysis. A rigorous screening based on the inclusion and exclusion criteria resulted in the selection of 74 articles suitable to compose the final analysis. This significant reduction reflects the application of rigorous methodological criteria, ensuring the inclusion of relevant andhigh-qualitystudies alone. ►Figure 1 details the flow of the screening process, from the initial identification to the final article selection.
We carefully extracted, synthesized, and organized the data from the selected studies. ►Table 1 presents the relevant information for each study, including the title, authors, study type, sample size, interventions, main outcomes, and limitations. This synthesis provides a comprehensive overview of the available evidence on AI application in plastic surgery, enabling a critical analysis of the methodological quality and the impacts of the reported interventions. Data organization aims to facilitate comparisons between studies and identify gaps in current knowledge, contributing to a deeper understanding of AI implications in this medical field. ►Table 1 compiles information from the 74 articles.
| Article | Author | Year | Study type | Sample size | Interventions | Outcomes | Complications |
|---|---|---|---|---|---|---|---|
| Artificial Intelligence | Mohd Altaf Mir | 2023 | Editorial | Not applicable, as | The author analyzed AI’s | The author highlighted that AI could analyze a | The author highlighted the views |
| Revolutionizing Plastic | this is an editorial | impact on plastic surgery | large amount of data, including medical | against AI use: it can undermine the | |||
| Surgery Scientific | about AI’s impact | publications, highlighting its | images, patient records, and surgical | significance of skilled surgeons, the | |||
| Publications | on plastic surgery | precision, accuracy, and | outcomes, and identify patterns, predict | ethical concerns about privacy, | |||
| publications that | efficiency, revolutionizing the | potential complications, and suggest | consent, and potential cultural | ||||
| did not involve | field by improving patient | optimized treatments. Through image | biases, the need for transparency | ||||
| patients. | outcomes and providing | analysis, a surgeon can evaluate the potential | and accountability in algorithms, | ||||
| valuable information for | esthetic outcome, generating simulations and | the potential dehumanization of | |||||
| surgeons and researchers. | helping in decision-making. The author also | health care, and the limited and | |||||
| highlighted the ease with which AI can provide | biased data. | ||||||
| information by selecting published articles | |||||||
| and providing key points, in addition to | |||||||
| potential solutions to the ethical problems | |||||||
| resulting from AI use. | |||||||
| Artificial Intelligence in | Elizabeth Choi | 2023 | Review of | Not applicable, as it | The authors reviewed articles | The current AI applications include optimizing | The authors highlighted points of |
| Facial Plastic Surgery: A | et al. | articles on | is a review of | trying to elucidate the | nonclinical tasks, such as documentation, to | ethical concern with AI use, | |
| Review of Current | current AI | current and future | current AI applications, future | increase efficiency in the workplace; | including legal liability for AI-based | ||
| Applications, Future | applications | AI applications that | uses, and existing ethical | contributing to preoperative decision- | medical recommendations, | ||
| Applications, and | did not involve | concerns. | making; creating more objective methods to | amplification of racial, | |||
| Ethical Considerations | patients. | assess postoperative outcomes; and surgical | socioeconomic, and gender biases, | ||||
| training and research. In the future, the | explainability of the AI model, and | ||||||
| authors predict that AI applications will | concerns about data security. | ||||||
| continue to grow per advances in quality and | |||||||
| accuracy and, in alignment with medical | |||||||
| judgment, AI software can provide significant | |||||||
| contributions to workflow and facial plastic | |||||||
| surgery. | |||||||
| Face the Future- | Maximilian F. | 2023 | Systematic | Not applicable, as it | The authors thoroughly | According to the literature, AI is under use in | The authors highlighted the debate |
| Artificial Intelligence in | Miragall et al. | review | is a literature review | reviewed English-language | certain areas of oral and maxillofacial surgery, | over AI limitations involving ethical | |
| Oral and Maxillofacial | based on database | PubMed/MEDLINE and | such as improving radiographic image quality, | considerations and data privacy. | |||
| Surgery | articles, with no | Embase articles from their | diagnosing cysts and tumors, and locating | They discussed the Black Box | |||
| direct patient | inception to December 1, | cephalometric landmarks. Through further | problem, i.e., not knowing how AI | ||||
| involvement. | 2022. They adapted the | research, it may provide different | makes its decisions, which | ||||
| search format to each | professionals with additional assistance to | contributes to distrust. | |||||
| database syntax. To find | improve preoperative planning, | ||||||
| pertinent material, they | intraoperative screening, and postoperative | ||||||
| thoroughly examined each | monitoring. In addition, the analysis of | ||||||
| retrieved article and the | complex medical imaging data can support | ||||||
| systematic review reference | surgeons in preoperative assessments, virtual | ||||||
| list. | surgical simulations, and individualized | ||||||
| treatment strategies. AI also assists surgeons | |||||||
| in intraoperative decision-making through | |||||||
| immediate feedback and guidance to improve | |||||||
| surgical accuracy and reduce complication | |||||||
| rates. | |||||||
| Aesthetic Surgery | Yi Xie et al. | 2023 | Observational | Not applicable, as it | This observational study | ChatGPT provided coherent and easy-to- | The study highlighted ChatGPT’s |
| Advice and Counseling | study | was based on nine | evaluated ChatGPT’s ability | understand answers to the questions, | limitations in providing more | ||
| from Artificial | questions to | to provide informative and | demonstrating its understanding of natural | detailed and personalized advice to | |||
| Intelligence: A | ChatGPT about | accurate answers to a set of | language in a specific healthcare context. The | the patient, essential factors in a | |||
| Rhinoplasty | rhinoplasty, and it | hypothetical questions | answers emphasized the significance of an | cosmetic surgery visit. | |||
| Consultation with | did not involve | simulating an initial | individualized approach, especially in | ||||
| ChatGPT | patients. | rhinoplasty visit. | cosmetic plastic surgery. | ||||
| Evaluation of Artificial | Libby R. | 2023 | Exploratory | Not applicable, as | The authors asked 10 | Bing and ChatGPT answers were as accurate as | None of the AIs consistently |
| Intelligence- | Copeland- | study to assess | this study did not | questions about breast | those of the United States Food and Drug | answered correctly questions | |
| generated Responses | Halperin et al. | the feasibility | involve patients. | implant-associated diseases, | Administration (FDA) and the American | requiring differentiated decision- | |
| to Common Plastic | of a larger | large anaplastic lymphoma, | Society of Plastic Surgeons (ASPS). Regarding | making. | |||
| Surgery Questions | research | and squamous cell carcinoma | the 30 multiple-choice questions, Bing | ||||
| project | to Bing using the “most | answered 10 correctly, 9, incorrectly, and did | |||||
| balanced” option and to | not answer 11. ChatGPT answered 16 | ||||||
| ChatGPT, and 10 multiple- | correctly and 14, incorrectly. In both cases, | ||||||
| choice questions from the | Bing’s answers were shorter, less detailed, and | ||||||
| 2022 plastic surgery in- | used verified and unverified sources as | ||||||
| service examination to Bing | references; ChatGPT did not provide citations. | ||||||
| using the “most accurate” | |||||||
| option and to ChatGPT. The | |||||||
| authors repeated the | |||||||
| questions three times in | |||||||
| consecutive weeks and used | |||||||
| the AI-generated answers to | |||||||
| assess their accuracy and | |||||||
| validity. | |||||||
| ChatGPT in Plastic and | Sanjeev Chaand | 2023 | Literature | Not applicable, as | Based on a bibliographic | The research revealed several ChatGPT | The authors demonstrated the |
| Reconstructive Surgery | Sharma et al. | review on | the study did not | review, the authors attempt | applications in plastic surgery, including the | literature concerns regarding the | |
| ChatGPT use in | involve patients. | to summarize existing | ability to create academic literature and aid in | ethical implications of chatbot use | |||
| plastic surgery. | applications of ChatGPT in | research production. ChatGPT can also | in scientific writing. In addition, they | ||||
| plastic surgery. | generate high-quality patient discharge | highlighted questions about the | |||||
| summaries in seconds, freeing up busy junior | accuracy of the AI-generated | ||||||
| doctors to complete other tasks. However, the | answers, since the current versions | ||||||
| need to enter clinical information manually | of ChatGPT cannot access the most | ||||||
| remains, and doctors must consider data | up-to-date sources. | ||||||
| privacy implications. In addition, the literature | |||||||
| widely reports AI use to aid in patient | |||||||
| communication, education, and training. | |||||||
| Use of Artificial | Ishith Seth et al. | 2023 | Narrative | Not applicable, as | The study explored the role of | AI can play a crucial role in advancing breast | The authors raised issues on data |
| Intelligence in the | review of the | the study did not | AI in breast reconstruction | reconstruction by facilitating preoperative | quality, privacy, and ethical | ||
| Advancement of Breast | current | involve patients. | through a systematic search | planning (breast volume, shape, and | considerations as obstacles to | ||
| Surgery and | literature | in MEDLINE, Cochrane | symmetry), surgical precision, personalizing | seamless AI integration into the | |||
| Implications for Breast | Library, Web of Science, | reconstructions, and assisting in | medical field. The study contains | ||||
| Reconstruction: A | Google Scholar, Clinical Trials, | postoperative care by early complication | information bias. | ||||
| Narrative Review | and Embase databases from | detection. The authors highlighted the | |||||
| January 1901 to June 2023, | primary role of AI in breast cancer screening, | ||||||
| outlining its potential to | currently involving objective detection and | ||||||
| refine surgical procedures, | tumor classification as benign or malignant | ||||||
| improve outcomes, and | per the Breast Imaging Reporting and Data | ||||||
| streamline decision-making. | System (BIRADS). | ||||||
| Artificial Intelligence for Plastic Surgeons | Gloria R. Sue | 2023 | Opinion article | Not applicable, as the study did not involve patients. | The article did not discuss a specific intervention, but rather how AI can be a tool to support and improve plastic surgery practice. | The author described the different current AI applications, i.e., diagnosis and treatment planning, surgical simulation, outcome prediction, helping in decision-making, and personalized medicine. | The author highlighted several limitations to AI use, i.e., bias propagation, dependence
on quality data, limitations in interpretation, and implementation challenges. Furthermore, since the article writing used ChatGPT, an AI system, there may be an inherent bias in the way AI processes and presents information, depending on the training data. The author acknowledged AI’s contribution in the preparation of the article, but also emphasized that AI should not replace the experience and judgment of plastic surgeons. |
| The future of artificial | Mariella | 2023 | A short paper | Not applicable, as | In the article, the authors | The outcomes discussed included | The study discussed potential |
| intelligence in facial | Fortune-Elya | discussing the | the study did not | discuss the application of AI in | postoperative outcome assessment using | biases, such as training data that | |
| plastic surgery | et al. | emerging role | involve patients. | facial plastic surgery, | learning algorithms, such as convolutional | may not adequately represent | |
| of AI in facial | exploring aspects such as | neural networks, identification of attractive | ethnic and gender diversity, cultural | ||||
| plastic surgery | personalized preoperative | facial features, personalization, and | and social influences resulting in | ||||
| assessment, surgical | simulation, helping to reduce anxiety about | bias in data collection, and human | |||||
| planning, outcome | uncertainty regarding surgical outcomes and | biases in data collection and | |||||
| simulation and postoperative | improving decision-making. | outcome interpretation. | |||||
| monitoring. | |||||||
| Using Generative | Bryan Lim et al. | 2023 | Systematic | Not applicable, as | The study analyzed the | The study indicated that generative AI tools, | The study identified some |
| Artificial Intelligence | review | the study did not | applications of generative AI | such as DALL-E 2, Midjourney, and Blue Willow, | limitations and challenges in image | ||
| Tools in Cosmetic | involve patients. | tools, such as generative | had significant potential to improve education | quality. Although some tools | |||
| Surgery: A Study on | adversarial networks (GANs), | and training in cosmetic surgery, each with its | showed promising results, the lack | ||||
| Rhinoplasty, Facelifts, | i.e., DALL-E 2, Midjourney, and | unique strengths. Additionally, AI’s ability to | of representations from multiple | ||||
| and Blepharoplasty | Blue Willow, in cosmetic | create personalized patient images can | angles and the emphasis on lighter | ||||
| Procedures | surgery. The goal was to | improve the viewing experience by enabling | skin tones limited the usefulness of | ||||
| explore how these | subjects to see a projection of their | these images for a comprehensive | |||||
| technologies can improve | postoperative results, which is crucial to | assessment. In addition, the study | |||||
| surgical practices, procedure | manage expectations and can help alleviate | highlighted the lack of image | |||||
| planning, and patient | anxiety about procedures. | diversity, with a predominance of | |||||
| education, in addition to | female faces and lighter skin tones, | ||||||
| discussing the challenges and | potentially affecting medical | ||||||
| future perspectives of this | education and practice. | ||||||
| integration in plastic surgery. | |||||||
| Robotic Microsurgery | Hussain S. H. | 2023 | Literature | Not applicable, as | This study discussed the | The authors found 19 relevant articles, | The limitations to this study included |
| in Plastic and | Ghandourah | review | the study did not | potential advantages of | including 5 directly comparing robotic and | the small amount of available research | |
| Reconstructive | et al. | involve patients. | robotics in plastic and | manual approaches. The robotic groups had | on robotic microsurgery in plastic and | ||
| Surgery: A Literature | reconstructive surgery | longer surgical times and higher learning | reconstructive surgery and the | ||||
| Review | through literature reviews | curves. The reported advantages of the sue of | heterogeneous results of the | ||||
| investigating “robotic | robotics included increased accuracy, | reviewed articles, hindering the | |||||
| microsurgery in plastic and | precision, and flexibility, in addition to tremor | statistical analysis. Furthermore, this | |||||
| reconstructive surgery” using | elimination and ergonomic improvement. | review aimed to study the effect of | |||||
| the PubMed and Cochrane | robotic microsurgery in a direct | ||||||
| Library databases. | comparison with the traditional | ||||||
| approach. However, due to the lack of | |||||||
| such articles, it is difficult to provide a | |||||||
| solid conclusion on the topic. | |||||||
| Artificial Intelligence in Plastic Surgery: Insights from Plastic Surgeons, Education Integration, ChatGPT’s Survey Predictions, and the Path Forward | Yasser Farid et al. | 2023 | Cross-sectional observational study | 153 plastic surgeons answering 34 questions. | The authors sent a 34- question survey to 564 plastic surgeons worldwide to assess the views of plastic surgeons and residents on the role of AI in plastic surgery. The survey explored aspects such as experience with AI use, data sources, ethical considerations, and future perspectives regarding AI. The researchers compared these responses with AI predictions using the same questions answered by ChatGPT. | The study found that most participants had little or no experience with AI. While some believed that AI could improve accuracy and visualization, opinions about its impact on surgical time, patient recovery, and satisfaction were mixed. Concerns included patient privacy, data security, costs, and informed consent. The authors identified valuable sources of AI training data and agreed on the significance of standards and transparency. The respondents anticipated the growing role of AI in reconstructive and cosmetic surgery, suggesting its integration into residency programs, and addressing administrative challenges and patient complications. They expressed their confidence in the enduring importance of human providers and interest in further AI research. | The study had some limitations, such as geographic bias, since most of the 153 surgeons answering the questionnaire were from South America, hindering the generalization of the findings. In addition, the study raised concerns about the difficulty that ChatGPT may have with moral decisions and individual patient preferences (data bias). |
| Artificial Intelligence Language Model Performance for Rapid Intraoperative Queries in Plastic Surgery: ChatGPT and the Deep Inferior Epigastric Perforator Flap | Connor J. Atkinson et al. | 2024 | Case study | Four plastic surgeons evaluated ChatGPT’s performance in providing accurate, relevant,
and specific answers. This study did not involve patients directly. |
The authors proposed a series of six intraoperative questions specific to the deep inferior epigastric perforator (DIEP) flap procedure, derived from real-world clinical scenarios, to ChatGPT. The goal was to investigate the potential of ChatGPT to address intraoperative questions during this procedure. | Generative AI tools, such as ChatGPT, can act as supplementary tools for surgeons
to provide valuable insights and foster intraoperative problem-solving skills. However, they lack consideration of individual patient factors and surgical nuances. Nevertheless, further refinement of their training data and rigorous scrutiny by experts to ensure the the accuracy and up-to-date nature of the information may lead to their use in the surgical field. |
The authors highlighted existing limitations in terms of comprehensiveness, context specificity, and real-time audio feedback. |
| Evaluation of the Artificial Intelligence Chatbot on Breast Reconstruction and Its Efficacy in Surgical Research: A Case Study | Yi Xie et al. | 2023 | Observational case study | Two plastic surgeons as evaluators, with no patients involved. | The authors asked six questions to ChatGPT about postmastectomy breast reconstruction. The first two focused on current evidence and options for postmastectomy breast reconstruction, and the remaining four focused on autologous breast reconstruction. The goal of the study was to assess the accuracy and comprehensiveness of ChatGPT’s answers and determine their suitability for use in esthetic plastic surgery research. | ChatGPT provided relevant and accurate information; however, it lacked depth. It could not provide more than a cursory overview in response to more esoteric questions, and it generated incorrect references. It created non-existing references and cited the wrong journal and date. All these mistakes pose a significant challenge in maintaining academic integrity, so its use must be cautious. | - |
| Exploring artificial | Meng M. Zhang | 2023 | Retrospective | The study involved | The study intervention | The study demonstrated that AI-based facial | Uneven gender and age |
| intelligence from a | et al. | study | 1,821 patients aged | consisted of collecting facial | age estimation models, specifically deep- | distributions, limited size of the | |
| clinical perspective: A | from 18 to 80 years, | images of patients who had | learning models, could accurately predict | apparent age database, lack of | |||
| comparison and | from whom 10,529 | undergone plastic surgery to | facial age. This fact suggests that AI can be an | interpretability, dependence on | |||
| application analysis of | facial images were | train AI models to predict | effective tool to assist plastic surgeons in | training data, and challenges in | |||
| two facial age | collected. | facial age. | assessing facial age before and after cosmetic | database building. | |||
| predictors trained on a | procedures. Furthermore, using AI to estimate | ||||||
| large-scale Chinese | facial age offers a more objective approach | ||||||
| cosmetic patient | compared with traditional subjective | ||||||
| database | assessments. | ||||||
| Facial Feminization | Sarah L. Barnett | 2023 | Systematic | Not applicable, as | The study discussed the | AI plays significant roles in FFS, including | - |
| Surgery: Anatomical | et al. | review | the study did not | intervention called facial | virtual surgical planning, outcome | ||
| Differences, | involve patients. | feminization surgery (FFS). The | assessment, patient satisfaction analysis, and | ||||
| Preoperative Planning, | article explored the surgical | pattern identification, leading to | |||||
| Techniques, and | techniques to align the facial | improvements in surgical techniques and | |||||
| Ethical Considerations | features of transwomen with | treatment personalization. | |||||
| their gender identity. In | |||||||
| addition, it addressed | |||||||
| preoperative planning, | |||||||
| anatomical differences | |||||||
| between male and female | |||||||
| faces, and FFS-related ethical | |||||||
| considerations. | |||||||
| Application | Leonard | 2023 | Review article | Not applicable, as | This study had no specific | The authors discussed the possibility of | - |
| possibilities of artificial | Knoedler et al. | the study did not | intervention. It aimed to | simulating outcomes with AI, which is difficult | |||
| intelligence in facial | involve patients. | outline the possibilities of | in FVCA because it requires the simultaneous | ||||
| vascularized composite | applying AI in facial | integration of the facial characteristics of the | |||||
| allotransplantation-a | vascularized composite | donor and the patient; as such, reliable | |||||
| narrative review | allotransplantation (FVCA) | predictions are only possible after the | |||||
| and discuss the use of AI | identification of a donor. The study also | ||||||
| technology to simulate FVCA | discussed AI-assisted intraoperative imaging | ||||||
| outcomes, diagnosis, | guidelines, rejection prediction, and | ||||||
| prediction of rejection | malignancy tracking. The authors raised | ||||||
| episodes, and malignancy | concerns about data security, since FVCA | ||||||
| screening. | involves highly-confidential information. | ||||||
| Estimating apparent | Kendall | 2023 | Observational | The study sample | Patients underwent | AI results indicated that the deep-learning | The study did not detail |
| age using artificial | Goodyear et al. | study using AI | contained 103 | blepharoplasty, including | model was effective in estimating the | complications, but highlighted | |
| intelligence: | methods to | patients, including | upper, lower, and | apparent age of the patients before and after | some AI limitations, including the | ||
| Quantifying the effect | quantify the | 29 men and 74 | quadrilateral procedures, i.e., | blepharoplasty. The AI model could accurately | small data set, the discrepancy | ||
| of blepharoplasty | rejuvenating | women. The | cosmetic surgeries, to | predict the apparent age of the patients, also | between age groups, focus on facial | ||
| effect of | patients underwent | remove excess skin and fat | providing an objective measure of the | features, and variability in | |||
| blepharoplasty | different | from the eyelids, improve | rejuvenating effect of blepharoplasty. The | treatment response (however, it did | |||
| blepharoplasty | facial appearance, and | model also enabled the analysis of different | not discuss surgical complications | ||||
| types: 28 upper | potentially rejuvenate their | patient groups, revealing that men showed an | or patient dissatisfaction with | ||||
| blepharoplasties, | appearance. The study | apparent reduction of 3.37 years and women, | esthetic outcomes). The study also | ||||
| 33 lower | analyzes preoperative and | a reduction of 2.19 years. | had some biases, including selection | ||||
| blepharoplasties, | postoperative photographs | bias to train and validate the model, | |||||
| and 42 quadrilateral | to estimate the apparent age | measurement bias of photograph | |||||
| blepharoplasties | of the patients before and | quality (affecting visual perception), | |||||
| (simultaneous | after the surgical intervention | confirmation bias, generalization | |||||
| upper and lower | using AI methods. | bias, and analysis bias. | |||||
| blepharoplasties). | |||||||
| Enhancing Complex | Subhas Gupta | 2023 | Observational | 80 patients | The patients underwent a | The AI chatbot accurately identified the most | It is worth noting that AI chatbots, |
| Wound Care by | et al. | study | comprehensive assessment by | appropriate treatment plan for 91% of the | including the software from this | ||
| Leveraging Artificial | a wound care provider who | patients, with a correlation higher than 90% with | study, are limited by the information | ||||
| Intelligence: An | established a diagnosis and | the initial assessment by the wound care | in their history and that they receive in | ||||
| Artificial Intelligence | treatment plan based on their | provider. | a specific scenario. | ||||
| Chatbot Software | clinical expertise; next, the | ||||||
| Study | authors introduced an AI | ||||||
| chatbot software as a | |||||||
| supplementary tool to provide | |||||||
| personalized treatment and | |||||||
| lifestyle recommendations. | |||||||
| Transforming breast | Cevik J et al. | 2023 | Brief report | Not applicable. | The authors discussed the | The authors highlighted some positive points | The authors concluded that the power |
| reconstruction: the | challenges, opportunities, and | consistent with a study showing that the AI | of AI requires careful implementation, | ||||
| pioneering role of | future directions of AI in | algorithm reduced the time analyzing | robust regulations, and ethical | ||||
| artificial intelligence in | preoperative planning for | perforating vessels for implants from 2 to | guidelines to ensure fair benefit | ||||
| preoperative planning | autologous breast | 3 hours to approximately 30 minutes per scan. | distribution and mitigate potential | ||||
| reconstruction. | misuse. | ||||||
| Artificial Intelligence as a | Carter J. Boyd | 2024 | Observational | 40 questionnaires | This study assessed the | Of the 40 questionnaires, 97.5% were on the | With further calibration, AI interfaces |
| Triage Tool during the | et al. | study | information, accuracy, and | appropriate topic. Medical counseling was | could act as a tool to answer patient | ||
| Perioperative Period: | accessibility of AI-generated | considered reasonable in 100% of cases. | queries in the future. However, | ||||
| Pilot Study of Accuracy | content regarding common | General consultations most frequently | patients should always maintain the | ||||
| and Accessibility for | perioperative issues in breast | reported comprehensive basic information, | ability to bypass the technology and | ||||
| Clinical Application | reduction surgery. | while specific consultations more often | contact their surgeons. | ||||
| The authors accessed ChatGPT | provided prescriptive information | ||||||
| in February 2023 and used it to | (P <0.0001). Specific consultations | ||||||
| ask 20 common patient | recommended discussion with the surgeon in | ||||||
| questions or complications | 100% of cases, whereas general consultations | ||||||
| arising in the perioperative | recommended the same in 95% of cases. | ||||||
| period of breast reduction | |||||||
| surgery. | |||||||
| Role of Robotics in | Krishan Mohan | 2023 | Narrative | Not applicable. | The authors evaluated the | The introduction of robots can revolutionize the | Not applicable. |
| Neuromodulator and | Kapoor et al. | review study | advantages and disadvantages | field, offering several potential benefits, | |||
| Filler Injections of Face | in the field of facial esthetics, | including increased precision, accuracy, and | |||||
| particularly in the injection of | outcome consistency. However, significant | ||||||
| facial fillers and | disadvantages of robots are their high cost, lack | ||||||
| neuromodulators. | of flexibility and personal touch, limited | ||||||
| experience, and risk of injury due to malfunction. | |||||||
| Predicting the severity | Jemin Kim et al. | 2023 | Retrospective | 1,283 patients, | Analysis of postthyroidectomy | The performance of the AI model to predict the | The study identified complications |
| of postoperative scars | study | including 1,043 in | scars in patients referred for | severity of postoperative scars was significant. | associated with postoperative scars, | ||
| using artificial | the main dataset and | scar minimization treatment. | Furthermore, the analysis revealed that, among | such as itching/pain, | |||
| intelligence based on | 240 in an external | The study used high-resolution | the 1,043 patients in the main dataset, 10.5% | adhesion/tightness, and | |||
| images and clinical data | dataset. | medical images to classify scar | had mild scars, 67.6% had moderate scars, and | induration/edema. The analysis of | |||
| severity. | 22.0% had severe scars, with clinical variables, | these complications concerning scar | |||||
| such as body mass index, time after surgery, and | severity revealed some significant | ||||||
| scar characteristics, showing significant | associations. For example, | ||||||
| differences among severity groups. The | itching/pain had a positive correlation | ||||||
| algorithm’s performance was consistent with | with severe scar severity, and | ||||||
| that of 16 dermatologists, indicating the | adhesion/tightness and | ||||||
| induration/edema showed negative | |||||||
| potential use of the model in the clinical practice for scar management. | associations with high severity. Furthermore, the incidence of hypertrophic scars after surgical procedures can range from 40% to 70% without appropriate management. | ||||||
| Can a Machine Ace the | Al Qurashi AA | 2023 | Observational | 50 questions from | The authors selected 50 | GPT-4.0 showed strong performance with high | Performance variability across |
| Test? Assessing GPT- | et al. | study | 19 different chapters | questions and asked them to | average scores for accuracy (2.88), clarity (3.00), | chapters indicates potential model | |
| 4.0’s Precision in Plastic | of a widely-used | GPT-4.0. The GPT-generated | completeness (2.88), and conciseness (2.92) on | limitations when dealing with some | |||
| Surgery Board | plastic surgery | answers were evaluated | a 3-point scale. The completeness of the model’s | complex plastic surgery topics. | |||
| Examinations | reference textbook. | according to four parameters: | answers had a significant correlation with | ||||
| accuracy, clarity, | accuracy (p < 0.0001), but there was no | ||||||
| completeness, and | significant correlation between accuracy and | ||||||
| conciseness. Correlation | clarity or conciseness. | ||||||
| analyses verified the | |||||||
| relationship involving these | |||||||
| parameters and the overall | |||||||
| performance of the model. | |||||||
| Risk predictions of | Zhang H et al. | 2023 | Systematic | Not applicable, as it | The study intervention focuses | The study revealed that ML is an effective tool to | The study had some limitations; the |
| surgical wound | review | was a systematic | on the application of machine- | manage surgical wounds, including in plastic | systematic review relied exclusively on | ||
| complications based on | review of nine | learning (ML) algorithms for | surgery. SSI evaluation in seven of the reviewed | English-language sources, which may | |||
| a machine learning | articles. | the assessment and prediction | studies demonstrated its effectiveness in | have led to the omission of relevant | |||
| algorithm: A systematic | of surgical wound | identifying risk factors. The most used | articles in other languages, limiting | ||||
| review | complications. The study | algorithms were the Support Vector Machine | the comprehensiveness and | ||||
| reviewed nine articles using ML | (SVM) and Convolutional Neural Network (CNN), | generalization of the results. In | |||||
| to analyze different aspects of | with the Artificial Neural Network (ANN) | addition, there was a risk of | |||||
| wound management, | achieving 96% of accuracy in wound | publication bias, since the study did | |||||
| including surgical site infection | management in facial plastic surgery. The study | not address this issue, meaning that | |||||
| (SSI) prediction, and wound | also highlighted that CNN showed good | there may be a tendency to publish | |||||
| classification. | accuracy in multiple surgeries, while SVM | positive results alone, distorting the | |||||
| showed high accuracy in multiple surgeries and | perception of the effectiveness of ML. | ||||||
| plastic surgery for burns. These results indicate | The study also relied exclusively on | ||||||
| that ML can lead to significant improvements in | open-access sources, which may result | ||||||
| postoperative management and the | in the exclusion of a significant | ||||||
| development of improved care techniques, | amount of data relevant to the | ||||||
| especially concerning surgical wounds. | analysis. Another point is that, | ||||||
| although ML has shown potential, the | |||||||
| practical implementation of AI-based | |||||||
| tools in the clinical practice may face | |||||||
| challenges, such as the need for | |||||||
| adequate training for healthcare | |||||||
| professionals and integration with | |||||||
| existing systems. The effectiveness of | |||||||
| ML algorithms can vary depending on | |||||||
| the surgery type and patient | |||||||
| characteristics. | |||||||
| Implementing AI Models | Chin-Choon Yeh | 2023 | Retrospective | 224 patients | The study analyzed burn | The random forest model produced the highest | The study did not discuss limitations. |
| for Prognostic | et al. | analysis | patients admitted to Chi Mei | area under the curve to predict prolonged | |||
| Predictions in High-Risk | Medical Center from 2010 to | hospital stays (> 14 days) at 81.1%, followed by | |||||
| Burn Patients | 2019 and addressed | the XGBoost (79.9%) and LightGBM (79.5%) | |||||
| supplementary information, | models. The AI techniques demonstrated | ||||||
| such as previous comorbidities | exceptional capabilities in predicting prolonged | ||||||
| and laboratory results, to build | hospital stays, the need for skin grafting, and the | ||||||
| models to predict graft | occurrence of overall adverse complications in | ||||||
| surgery, prolonged hospital | burn patients. | ||||||
| stay, and overall adverse | |||||||
| outcomes using AI. | |||||||
| Implementing AI Models for Prognostic Predictions in High-Risk Burn Patients | Yeh CC et al. | 2023 | Retrospective analysis | 224 patients | AI use to predict hospital stays, skin graft needs, and general adverse complications in burn patients. | AI techniques have demonstrated exceptional capabilities in predicting prolonged hospital stays, the need for a skin graft, and the occurrence of general adverse complications in burn patients. | - |
| Does medication- | Bittrich M et al. | 2023 | Retrospective | 52 patients. | AI use to analyze the long-term | Patients in the MRONJ group had a considerably | - |
| related osteonecrosis of | analysis | effects of medication-related | longer survival time than those in the control | ||||
| the jaw affect survival of | osteonecrosis of the jaw | group (126 versus 86 months). | |||||
| patients with Multiple | (MRONJ). | ||||||
| Myeloma?: Exploring a | |||||||
| large single center | |||||||
| database using artificial | |||||||
| intelligence | |||||||
| Deciphering the | Song B et al. | 2023 | Case-control | 11 hypertrophic scar | First-time investigation of the | The study revealed that cuproptosis may play a | - |
| contributions of | study | (HS) tissue samples | relationship between the | significant role in the development of HSs. Using | |||
| cuproptosis in the | occurrence and development | machine-learning techniques to analyze single- | |||||
| development of | of HS and cuproptosis, | cell data, the researchers identified patterns and | |||||
| hypertrophic scar using | deepening our understanding | specific contributions of cuproptosis to HS | |||||
| single-cell analysis and | of the underlying mechanisms | formation. | |||||
| machine learning | of these scars and providing | ||||||
| techniques | new potential therapeutic | ||||||
| strategies and research bases | |||||||
| to inhibit scar formation. | |||||||
| Detecting Distal Radius Fractures Using a Segmentation-Based Deep Learning Model | Anttila TT et al. | 2023 | Diagnostic validation study | 758 patients | The intervention was technical and involved the development and application of a segmentation-based deeplearning model. | The deep-learning model developed demonstrated effectiveness in detecting distal radius fractures. The study reported good model performance in terms of accuracy, sensitivity, and specificity to identify fractures in medical images. | No clinical comparisons or associated adverse effects. |
| A comprehensive | Yun JY et al. | 2023 | Comparative | The study involvred | The study evaluated the quality | The study found that ChatGPT provided | The study did not directly report |
| evaluation of ChatGPT | cross-sectional | 60 participants, | of ChatGPT-generated queries | information of acceptable quality, with positive | complications, but it did mention | ||
| consultation quality for | study | including plastic | regarding breast | reviews from surgeons and laypeople. However, | concerns about the accuracy and | ||
| augmentation | surgeons and | augmentation surgery. The | plastic surgeons were more critical of the | depth of information provided by | |||
| mammoplasty: A | laypeople. | comparative analysis involved | technical accuracy of the answers, while | ChatGPT, especially on complex topics | |||
| comparative analysis | plastic surgeons and laypeople, | laypeople found them clearer and more | like plastic surgery. | ||||
| between plastic | who evaluated the accuracy, | understandable. The study highlighted that | |||||
| surgeons and laypersons | clarity, and usefulness of the | ChatGPT can be a useful tool to provide initial | |||||
| information provided by | information about medical procedures, but | ||||||
| ChatGPT about breast | emphasized the need for supervision by | ||||||
| augmentation surgery. | healthcare professionals. | ||||||
| A History of Innovation: | Cevik J et al. | 2023 | Historical | Not applicable, as | The study reviews the | The review highlighted how innovations in | While the study does not directly |
| Tracing the Evolution of | review | the study is a | evolution of imaging | imaging techniques, such as the introduction of | address complications in patients, it | ||
| Imaging Modalities for | literature review that | modalities used in the | high-resolution computed tomography | mentions how limitations of previous | |||
| the Preoperative | did not directly | preoperative planning for | angiography and magnetic resonance imaging, | imaging techniques, such as low | |||
| Planning of | involve patients. | microsurgical breast | have revolutionized surgical planning, enabling | resolution and lack of vascular detail, | |||
| Microsurgical Breast | reconstruction. | better visualization of blood vessels and tissues. | could lead to intraoperative and | ||||
| Reconstruction | This has resulted in improved surgical outcomes, | postoperative complications. | |||||
| with reduced complications and improved | |||||||
| viability of flaps for breast reconstruction. | |||||||
| Can AI Think Like a | Leypold T et al. | 2023 | Cross-sectional | The study involved | The study evaluated the ability | The results showed that GPT-4 could provide | - |
| Plastic Surgeon? | study | 10 plastic surgeons | of the GPT-4 AI model to | reasonable clinical recommendations in many | |||
| Evaluating GPT-4’s | who evaluated GPT- | perform clinical judgments in | cases, demonstrating a good understanding of | ||||
| Clinical Judgment in | 4’s performance. It | upper extremity reconstructive | basic reconstructive practices. However, the | ||||
| Reconstructive | did not involve | procedures. | study also highlighted significant limitations, | ||||
| Procedures of the Upper | patients directly. | especially in complex cases in which human | |||||
| Extremity | clinical judgment, based on experience and | ||||||
| intuition, was superior. AI was useful as a | |||||||
| supportive tool, but it did not replace the expert | |||||||
| clinical judgment of surgeons. | |||||||
| Accuracy and safety of | Zhang Z et al. | 2023 | Method | Four cases | The researchers evaluated the | The results showed that robotic-assisted | The study reported no major |
| robotic navigation- | validation study | accuracy and safety of robotic- | navigation significantly improved the accuracy | complications when using robotic- | |||
| assisted distraction | assisted navigation to perform | of the distraction osteogenesis procedure. The | assisted navigation. However, as with | ||||
| osteogenesis for | distraction osteogenesis (a | mean positioning error of the osteotomy plane | any surgical procedure, there was the | ||||
| hemifacial microsomia | surgical procedure for bone lengthening) in patients with hemifacial microsomia. | was of 1.77 ± 0.12 mm, and the mean angular error was of 8.94° ± 4.13°. The mean positioning error of the distractor was of 3.67 ± 0.23 mm, and the mean angular error was of 8.13° ± 2.73°. | possibility of minor complications, such as infections or postoperative discomfort, although these were not significant issues in the study. | ||||
| Postoperative patient satisfaction was high, and | |||||||
| no adverse events occurred. | |||||||
| Machine learning for | Ren Y et al. | 2023 | Cohort study | 518 patients | The researchers used machine- | The machine-learning model showed high | The study reported no complications |
| prediction of delirium in | learning techniques to develop | accuracy in predicting postoperative delirium in | when using the machine-learning | ||||
| patients with extensive | a predictive model of | patients with extensive burns. The random | model. | ||||
| burns after surgery | postoperative delirium in | forest (RF) model outperformed the other eight | |||||
| patients with extensive burns. | models in terms of predictive performance | ||||||
| (receiver operating characteristic curve: | |||||||
| 84.00%). In an external validation, RF performed | |||||||
| well (accuracy: 77.12%; sensitivity: 67.74%; and | |||||||
| specificity: 80.46%). | |||||||
| ChatGPT’s quiz skills in | Hoch CC et al. | 2023 | Observational | ChatGPT answered | The study evaluated ChatGPT’s | ChatGPT had a mixed performance across | The study reported no complications, |
| different otolaryngology | study of AI | 2,576 questions. The | abilities to answer questions | subspecialties. In some fields, such as otology, | but highlighted the limitations of | ||
| subspecialties: an | performance | study did not involve | regarding several | the model showed a high accuracy rate, and, in | ChatGPT in dealing with issues | ||
| analysis of 2,576 single- | patients. | otolaryngology subspecialties. | others, such as head and neck surgery, its | requiring complex clinical | |||
| choice and multiple- | performance was less effective. Overall, | interpretation or practical application | |||||
| choice board | ChatGPT could answer a significant proportion | of medical knowledge. | |||||
| certification preparation | of questions correctly, but with variations | ||||||
| questions | depending on the topic. | ||||||
| Machine-Learning | Chen Y et al. | 2023 | Cohort study | 209 patients | The study applied machine- | The machine-learning model demonstrated | The study did not report clinical |
| Prediction of Capsular | learning techniques to develop | good predictive ability for capsular contracture, | complications directly associated with | ||||
| Contraction after Two- | a predictive model for the | with high accuracy in identifying patients at risk. | the machine-learning model. | ||||
| Stage Breast | occurrence of capsular | It identified several risk factors, including patient | |||||
| Reconstruction. | contracture after two-stage | characteristics, surgical details, and | |||||
| breast reconstruction. | postoperative variables. | ||||||
| Risk predictions of | Tehrany PM et al. | 2023 | Systematic | The authors did not | The researchers used a | The machine-learning model showed a high | The study did not report clinical |
| hospital-acquired | review | specify the number | machine-learning algorithm to | predictive ability to identify patients at risk of | complications directly associated with | ||
| pressure injury in the | of patients. | predict the risk of developing | developing pressure injuries. The accuracy of the | the machine-learning model. | |||
| intensive care unit based | hospital-acquired pressure | model was significant, with good sensitivity and | |||||
| on a machine learning | injuries in intensive care unit | specificity in predicting risk. | |||||
| algorithm | patients using the PubMed and | ||||||
| ISI databases and the keywords | |||||||
| intensive care unit, bedsore, | |||||||
| pressure injury, and machine | |||||||
| learning from November 1, | |||||||
| 2022, to January 11, 2023. | |||||||
| Workflow assessment of an augmented reality application for planning of perforator flaps in plastic reconstructive surgery: Game or game changer? | Berger MF et al. | 2023 | Cross-sectional study | 7 patients | The researchers evaluated the application of augmented reality (AR) to plan perforator flaps in reconstructive plastic surgery. | AR was an innovative tool that could transform the planning and execution of reconstructive surgical procedures. According to the study, AR provided significant improvements in flap visualization and planning, offering a better anatomical understanding and facilitating procedural accuracy. | The study reported no complications. |
| HI-MViT: A lightweight | Ding Y et al. | 2023 | Comparative | The study did not | The researchers developed and | The HI-MViT model had effective performance in | The study did not report clinical |
| model for explainable | cross-sectional | specify an exact | tested a low-weight, high- | classifying skin diseases, with high accuracy and | complications in direct association | ||
| skin disease | study | number of patients, | accuracy model to classify skin | explanatory power. The study highlighted the | with the model. | ||
| classification based on | but used a dataset of | diseases called Hierarchical | model’s efficiency in processing and its ability to | ||||
| modified MobileViT | skin images to train | Image Transformer with | provide explanations for classification decisions. | ||||
| and evaluate the | MobileViT (HI-MViT). | ||||||
| model. | |||||||
| Quantization of | Hsu SY et al. | 2023 | Cohort study | 122 patients | The researchers developed and | The app showed high accuracy in detecting | The study did not report any direct |
| extraoral free flap | evaluated a deep learning- | venous congestion compared with traditional | complications in association with the | ||||
| monitoring for venous | integrated application to | monitoring methods. The integration of deep | app. | ||||
| congestion with deep | monitor venous congestion in | learning technology with mobile devices | |||||
| learning integrated iOS | extraoral-free grafts using iOS | enabled more accessible and real-time | |||||
| applications on | smartphones. | monitoring. | |||||
| smartphones: a | |||||||
| diagnostic study | |||||||
| Machine learning | Yang SY et al. | 2023 | Cohort study | 341 patients | The researchers developed and | The machine-learning model had good accuracy | The study reported no direct |
| approach for predicting | validated a machine-learning | in predicting inhalation injuries, with a | complications associated with the | ||||
| inhalation injury in | model to predict inhalation | significant ability to identify patients at risk. The | model. | ||||
| patients with burns | injuries in burn patients. | approach helped improve patient screening and | |||||
| management, enabling earlier and more | |||||||
| targeted interventions. | |||||||
| Application of multiple | Chang CW et al. | 2023 | Comparative | 4,991 initial burn | The researchers applied | Deep-learning models demonstrated effective | The study did not report clinical |
| deep learning models | cross-sectional | images and 1,050 | multiple deep-learning models | performance in the automatic assessment of | complications in direct association | ||
| for automatic burn | study | palm images | for the automatic assessment | burns. The combination of multiple models | with the models. | ||
| wound assessment | of burn wounds. | helped improve the accuracy and consistency of | |||||
| the assessments, providing a valuable tool to | |||||||
| monitor and manage burn wounds. | |||||||
| Finetuning of GLIDE | Shavlokhova V | 2023 | Comparative | 10,015 dermoscopic | The researchers fine-tuned the | The results indicated that the images generated | The study reported no clinical |
| stable diffusion model | et al. | cross-sectional | images | Guided Language to Image | had varying degrees of quality and realism. | complications. | |
| for AI-based text- | study | Diffusion for Education (GLIDE) | Melanocytic nevi and melanoma presented | ||||
| conditional image | stable-diffusion model to | higher similarity to actual images than other | |||||
| synthesis of | generate dermoscopic images | conditions. Synthetic image integration | |||||
| dermoscopic images | from textual descriptions. The | improved the model’s classification | |||||
| goal was to create a system | performance and resulted in higher accuracy | ||||||
| that produces realistic and | and precision. The AI evaluation showed superior | ||||||
| accurate images of skin lesions | classification performance compared with the | ||||||
| based on textual inputs | dermatologist. | ||||||
| describing specific | |||||||
| dermatologic features. | |||||||
| Feeling the beat: a smart | Lin M et al. | 2023 | Clinical trial | The study did not | The researchers developed a | The smart exoskeleton was effective in guiding | The study did not report clinical |
| hand exoskeleton for | specify the number | smart hand exoskeleton to aid | users through specific movement patterns, | complications. However, users may | |||
| learning to play musical | of human | in learning how to play musical | helping them learn to play musical instruments | have difficulties in adaptation, | |||
| instruments | participants, as the | instruments. | more quickly andaccurately. This technology has | comfort, and calibration. | |||
| main focus was | shown potential as a supportive tool in music | ||||||
| developing and | learning, especially for beginners or subjects | ||||||
| evaluating robotic | with motor difficulties. | ||||||
| exoskeleton | |||||||
| technology to learn | |||||||
| how to play musical | |||||||
| instruments. | |||||||
| Construction and | Sakakibara S | 2023 | Cohort study | 50 patients | The researchers developed and | The algorithm showed high accuracy in | The main complications or limitations |
| Validation of an Image | et al. | validated a machine-learning | discriminating between necrosis and other | reported in the study included image | |||
| Discrimination | algorithm to discriminate | wounds in pressure ulcers. The model validation | variability (which may influence the | ||||
| Algorithm to | between necrosis and wounds | indicated that it could be a useful tool for | accuracy of the algorithm), model | ||||
| Discriminate Necrosis | in pressure ulcer images. The | healthcare professionals, aiding in the fast and | generalization (algorithm training | ||||
| from Wounds in | goal was to improve accuracy | accurate assessment of wound conditions and | used a specific dataset), and the need | ||||
| Pressure Ulcers | in identifying necrosis in ulcers, | facilitating clinical decision-making. | for further validation (on a larger scale | ||||
| which is crucial for proper | and in different clinical scenarios to | ||||||
| treatment. | confirm its robustness and practical | ||||||
| applicability). | |||||||
| Analysis of Watson for | Park H et al. | 2023 | Comparative | 183 patients | The researchers compared | The study found a 73% overall agreement rate | The study identified the following |
| oncology and clinicians’ | observational | treatment recommendations | between recommendations from the WFO and | major complications or limitations: | |||
| treatment | study | provided by the Watson for | oncologists. The field with the highest | recommendation disagreements, | |||
| recommendations for | Oncology (WFO) AI system | disagreement was the chemotherapy choice, | training data reliance (which may not | ||||
| patients with breast | with recommendations from | since the WFO often suggested regimens | fully reflect local populations or | ||||
| cancer in Korea: A single | human oncologists for breast | different from those suggested by the | clinical practices), and acceptance by | ||||
| center experience | cancer patients. | physicians. Disagreements also occurred in | physicians (depending on trust in AI | ||||
| more complex cases with multiple treatment | systems and experiences with their | ||||||
| lines available. | suggestions) | ||||||
| The Composition of | Man-Lok L et al. | 2023 | Observational | The study did not | The researchers used an AI | AI enabled a more accurate and objective | Generalization limitations (i.e., |
| Antiaging Scales for | study using AI | directly specify the | system to evaluate and develop | analysis of facial rejuvenation scales, resulting in | limitation to generalize data to all | ||
| Facial Rejuvenation: | number of patients, | facial rejuvenation scales. | a better understanding of the critical | populations), dependence on input | |||
| Assessed with Artificial | as the focus was the | components to consider when assessing the | data, data interpretation (which | ||||
| Intelligence | analysis of facial | success of facial rejuvenation procedures. | should be performed by | ||||
| rejuvenation scales | professionals), and analysis biases (if | ||||||
| using AI rather than | the AI training data contains biases, | ||||||
| objective clinical | they may negatively affect the | ||||||
| assessment of | composition and interpretation of the | ||||||
| subjects. | facial rejuvenation scales.) | ||||||
| Infrared spectroscopic | Yeh K et al. | 2023 | Experimental | The study did not | The study developed and | The results showed that the ISLSCM technique | Technical challenges (requires careful |
| laser scanning confocal | study on | involve patients | evaluated a new imaging | can perform high-resolution chemical imaging | calibration to ensure accuracy and | ||
| microscopy for whole- | technological | directly. | technique called Infrared | on whole-tissue slides, overcoming the | reproducibility), applicability | ||
| slide chemical imaging | development | Spectroscopic Laser Scanning | limitations of traditional chemical imaging | limitations, and processing time. | |||
| Confocal Microscopy (ISLSCM), | techniques, such as low resolution and long | ||||||
| which was used to perform | acquisition time. | ||||||
| chemical imaging on wholetissue slides samples to identify and map chemical components at highresolution. | |||||||
| Unsupervised anomaly | Hayajneh A et al. | 2023 | Study on | The study did not | The study applied a model- | The StyleGAN2-based model could effectively | Technical complexity, model |
| appraisal of cleft faces | technological | involve human | adaptation technique based on | detect and evaluate anomalies in faces with cleft | generalization (the study used a single | ||
| using a StyleGAN2- | development | patients directly. | StyleGAN2 to perform an | lip and palate. The technique demonstrated the | database, requiring validation in all | ||
| based model adaptation | Instead, it used a | unsupervised assessment of | ability to identify anomalous facial features, | patients), and data interpretation by a | |||
| technique | dataset of facial | anomalies in cleft faces. The | which may help to improve the diagnosis and | professional. | |||
| images for AI model | model was trained to generate | surgical planning for these patients. | |||||
| training and testing. | facial representations and | ||||||
| identify anomalies compared | |||||||
| to regular faces with no need | |||||||
| for explicit anomaly labels. | |||||||
| Convolutional neural | Sun J et al. | 2023 | Comparative | Use of 71 images for | The researchers used | The approach correctly identified all grade-IV | Generalization limitations, |
| network models for | cross-sectional | training. | convolutional neural network | frostbite lesions (18/18, 100%), but with 1 error | dependence on training data, data | ||
| automatic diagnosis and | study | models to analyze images of | in grade diagnosis. The accuracy of the approach | interpretation by healthcare | |||
| graduation in skin | skin frostbite and compared | on the entire test set was of 97.39% (112/115). | professionals, and potential analysis | ||||
| frostbite | their performance with those | The accuracy of the two residents was of 77.39% | biases. | ||||
| of two residents from the burn | and 73.04%. | ||||||
| department. | |||||||
| Comparative study of | Roberts RH et al. | 2023 | Comparative | The study did not | The researchers used ChatGPT | Human raters provided more detailed and | ChatGPT may not capture all the |
| ChatGPT and human | cross-sectional | directly involve | and human raters to analyze | contextual assessments, reflecting a deeper | nuances and complexities of medical | ||
| evaluators on the | study | patients, as it | and evaluate medical literature | understanding of the nuances of medical | studies, resulting in less accurate or | ||
| assessment of medical | focused on | articles based on established | studies. The study highlighted that, while | detailed assessments. | |||
| literature according to | evaluating medical | reporting standards, such as | ChatGPT can be a useful tool in the initial | ChatGPT’s effectiveness depends on | |||
| recognised reporting | literature rather than | Consolidated Standards of | screening and evaluation of medical literature, | the quality of its training data and | |||
| standards | on clinical | Reporting Trials (CONSORT), | the review and final judgment still rely heavily on | underlying algorithms, which may | |||
| interventions. | Preferred Reporting Items for | human expertise to ensure accuracy and a | limit its ability to accurately assess the | ||||
| Systematic Reviews and Meta- | comprehensive understanding of quality | medical literature. | |||||
| Analyses (PRISMA), and other | standards. | The final assessment interpretation | |||||
| quality criteria. | still requires human judgment to | ||||||
| ensure the correct application of | |||||||
| reporting standards and the | |||||||
| consideration of all nuances. | |||||||
| Efficacy of navigation | Liu X et al. | 2024 | Single-blinded, | 22 patients | Intervention group: patients | Primary: evaluation of the effectiveness of the | Potential adverse events: the |
| system-assisted | randomized, | submitted to distraction | AI-assisted navigation system based on | potential risks and complications | |||
| distraction osteogenesis | controlled | osteogenesis using an AI- | parameters such as the accuracy of the surgical | associated with the AI-assisted | |||
| for hemifacial | clinical trial | assisted navigation system that | procedure, facial deformity improvement, and | navigation system may included | |||
| microsomia based on | aims to help in the accuracy | postoperative clinical outcomes. | technology failures, navigation errors, | ||||
| artificial intelligence for | and effectiveness of the | Secondary: comparison of surgical times, | or surgical complications. | ||||
| 3 to 18 years old: study | surgical procedure by guiding | complication rates, and quality of life | Implementation challenges: the | ||||
| protocol for a | the surgeon during bone | assessment. | study faced challenges in | ||||
| randomized controlled | distraction. | implementing and integrating the AI | |||||
| single-blind trial. | Control group: patients | technology into the surgical | |||||
| submitted to the same | environment and maintaining the | ||||||
| distraction osteogenesis | blinding to ensure outcome | ||||||
| procedure but with no AI- | impartiality. | ||||||
| assisted navigation system. | |||||||
| Predicting overall | Cheng P et al. | 2023 | Cohort study | 724 patients | Development and testing of | Machine-learning models had a significant ability | Data quality: the quality and |
| survival in chordoma | several machine-learning | to predict the overall survival of patients with | completeness of the clinical and | ||||
| patients using machine | models to predict the overall | chordoma. Their accuracy varied depending on | demographic data can influence the | ||||
| learning models: a web- | survival of patients with | the model and variables. | model accuracy. | ||||
| app application | chordoma. These models used | The web application provided a practical and | Model generalization, technological | ||||
| clinical and demographic data | accessible interface to use predictive models, | dependence: the web application | |||||
| from patients. | facilitating the integration of the results into the | requires access to technology and | |||||
| A web application integrated | clinical practice. | training so that health professionals | |||||
| the models, enabling clinicians | can adequately interpret and use the | ||||||
| and researchers to use the tool | model-generated predictions. | ||||||
| to predict patient survival | |||||||
| based on their individual data. | |||||||
| Applications of the | Schopow N et al. | 2023 | Comparative | The study did not | The study evaluated and | ChatGPT had the potential to improve efficiency | Accuracy and reliability: the accuracy |
| Natural Language | study and | involve a specific | compared ChatGPT in different | and accuracy across several clinical tasks, | of ChatGPT-generated answers may | ||
| Processing Tool | systematic | number of patients, | clinical applications, including | although some challenges and limitations need | vary. ChatGPTuse should be careful to | ||
| ChatGPT in Clinical | review | as it focused on | decision-making support, | to be addressed. | ensure that the information provided | ||
| Practice: Comparative | analyzing ChatGPT | reporting, and assistance with | Integrating ChatGPT into clinical practices could | is accurate and reliable. | |||
| Study and Augmented | applications the in | administrative tasks. | offer significant benefits but requires ongoing | Data security: ChatGPT use in the | |||
| Systematic Review | clinical practice, not | Through a systematic review, | evaluation to ensure that applications are | clinical practice raises concerns about | |||
| on a clinical trial. | the authors compiled and | accurate and safe. | the security and privacy of patient | ||||
| evaluated the existing | data, especially regarding sensitive | ||||||
| literature on ChatGPT in the | information. | ||||||
| clinical practice, highlighting | |||||||
| its applications and limitations. | |||||||
| Feasibility of intra- | Yu S et al. | 2024 | Viability study | The study did not | Technology: multispectral | The technology helped to improve the accuracy | Clinical adaptation: implementing |
| operative image | specify directly the | imaging plus deep learning. | in identifying and removing burn tissue, | technologyin real clinical settings may | |||
| guidance in burn | number of patients, | Procedure: the technology | providing better intraoperative outcomes. Its | face challenges related to surgical | |||
| excision surgery with | as it focused on the | provided intraoperative | application could increase surgical efficiency by | team adaptation and integration with | |||
| multispectral imaging | feasibility and | guidance during burn excision | facilitating a more targeted and less invasive | existing systems. | |||
| and deep learning. | application of the | to improve the accuracy and | approach. | ||||
| technology during | effectiveness of burn-tissue | ||||||
| burn excision | removal. | ||||||
| surgery performed | |||||||
| on six pigs. | |||||||
| Validation of ChatGPT | Vallurupalli M | 2024 | Technology | - | This study aimed to evaluate | ChatGPT 3.5 helped improve the readability of | Dependence on AI quality: |
| 3.5 as a Tool to Optimize | et al. | validation study | ChatGPT 3.5 as a tool to | educational materials, making them more | AI may present limitations in its ability | ||
| Readability of Patient- | optimize patient-oriented | understandable for the target audience. | to capture specific nuances or detailed | ||||
| facing Craniofacial | craniofacial education | The authors assessed the readability of the | medical contexts significant for | ||||
| Education Materials | materials. | materials before and after AI intervention and | patient education. | ||||
| observed significant improvements in text | Continued validation of optimized | ||||||
| comprehension. | materials with direct feedback from | ||||||
| patients and healthcare professionals | |||||||
| is required to ensure that the | |||||||
| materials are appropriate and | |||||||
| effective. | |||||||
| Deep Learning-Based | Ha JH et al. | 2023 | Comparative | 714 cases | The researchers developed and | The deep learning-based system demonstrated | Dependence on large data volumes: |
| Diagnostic System for | cross-sectional | applied a diagnostic system to | high precision in detecting VPI, with higher | the system requires large volumes of | |||
| Velopharyngeal | study | assess velopharyngeal | accuracy, sensitivity, and specificity rates than | annotated data for proper training, | |||
| Insufficiency Based on | insufficiency (VPI) in patients | those of the conventional methods. | which may not be available in all | ||||
| Videofluoroscopy in | with repaired cleft palate. The | healthcare centers. | |||||
| Patients With Repaired | intervention consisted of | Clinical integration: implementing | |||||
| Cleft Palates | analyzing videofluoroscopy | the system the in clinical practice | |||||
| scans using a deep-learning | requires adaptation by healthcare | ||||||
| model to identify and classify the presence and severity of VPI. | professionals and integration with existing workflows. | ||||||
| Wearable Prophylaxis Tool for AI-Driven Identification of Early Warning Patterns of Pressure Ulcers | Gruenerbel L et al. | 2023 | Cohort study | 60 patients | The researchers developed an AI-powered wearable tool for continuous monitoring of the patient’s vital signs and movement patterns. The goal was to identify early patterns indicating the imminent development of pressure ulcers, enabling preventative interventions. | AI application as a wearable tool was effective in the early detection of patterns preceding the development of pressure ulcers. The system could identify risk situations accurately, providing an opportunity for early interventions to prevent the formation of these ulcers. | Several patients withdrew from the study due to discomfort with the sensor system. |
| Introduction of Deep Learning-Based Infrared Image Analysis to Marginal Reflex Distance 1 Measurement Method to Simultaneously Capture Images and Compute Results: Clinical Validation Study | Song B et al. | 2023 | Cohort study | 77 patients | The researchers introduced a Marginal Reflex Distance 1 (MRD1) measurement method using infrared image analysis with a deep learning system. This method enabled simultaneous image capture and automatic result calculation. | The proposed method underwent clinical validation, and it was accurate and effective in measuring MRD1. The technology enabled process automation, improving the consistency and speed of the assessment compared with traditional methods. Furthermore, its application in clinical settings was easy. | Dependence on image quality: the system’s accuracy depends on the quality of the infrared
image captured. Problems with image capture may affect the results. Need for continuous validation: although the results are promising, the system’s effectiveness requires continuous validation in different clinical settings to ensure broad applicability. |
| Comparison of large language models in management advice for melanoma: Google’s AI BARD, BingAI and ChatGPT | Mu X et al. | 2023 | Comparative cross-sectional study | The researchers asked five questions to different AIs (ChatGPT, BARD, and BingAI). |
The intervention consisted of testing and comparing the AI answers regarding melanoma management. The researchers analyzed how each model addressed different aspects of melanoma treatment and counseling. | The study demonstrated that ChatGPT marginally outperforms BARD and BingAI in providing reliable, evidence-based clinical advice. However, the models still faced limitations in depth and specificity. Future research should improve the performance of LLM by integrating specialized databases and expert knowledge to support patient-centered care. | Answer variability: the quality and accuracy of the answers varied among the models,
which may negatively influence clinical decision-making. Dependence on model training: the effectiveness of the answers depends on the dataset training each model, which may not cover all the nuances of melanoma management. Risk of inaccurate information: there is an inherent risk that the models will provide inaccurate or outdated information, potentially affecting patient care if not properly verified by healthcare professionals. |
| The effect of double W tension-reduced suture technique on the abdominal scars following the da Vinci robot-assisted gastrectomy for severely obese patients | Chen W et al. | 2023 | Cohort study | Comparison of 40 incisions. | The study analyzed the effect of a new type of reduced tension suture, called the “double W reduced-tension suture technique,” on abdominal scars after Da Vinci robot-assisted gastrectomy in severely-obese patients, and compared it with the conventional technique. | The results showed that the double W reducedtension suture technique significantly decreased tension on the wound edges, resulting in more esthetic scars and fewer healing complications, such as wound dehiscence or hypertrophic scar formation. | Although it was not the primary focus, it was critical to monitor the suture technique
for the risk of infection, which can be a common complication in obese patients. The technique may have different efficacy depending on the obesity severity. Need for adequate surgical training. |
| Bard Versus the 2022 | Najafali D et al. | 2023 | Comparative | 231 questions. | The intervention consisted of | The study included 231 questions. Bard | No clinical complications. |
| American Society of | cross-sectional | testing the Bard AI with | answered 143 questions correctly, | Clinical practice applicability: while | |||
| Plastic Surgeons In- | study | questions from the American | corresponding to a 62% accuracy rate. The best- | AI may perform well on theoretical | |||
| Service Examination: | Society of Plastic Surgeons | performing section was the comprehensive | examinations, the practical | ||||
| Performance on the | (ASPS) examination to assess | portion (73%). When compared with integrated | application of medical knowledge | ||||
| Examination in Its Intern | its performance concerning the | residents nationally, Bard scored in the 74th | may require skills and clinical | ||||
| Year | actual examination for plastic | percentile for postgraduate year (PGY)-1, in the | judgment that an AI does not have yet. | ||||
| surgery residents. | 34th percentile for PGY-2, in the 20th percentile | Question interpretation: AI may face | |||||
| for PGY-3, in the 8th percentile for PGY-4, in the | challenges in correctly interpreting | ||||||
| 1st percentile for PGY-5, and in the 2nd | questions or applying clinical | ||||||
| percentile for PGY-6. | knowledge to specific scenarios. | ||||||
| Bard outperformed over half of the integrated | |||||||
| first-year residents (74th percentile). | |||||||
| Validating a novel | Ali SR et al. | 2023 | Retrospective, | 34,955 lesions in | The intervention applied AI to | The study validated AI effectiveness, | Natural language processing |
| natural language | multicentric, | 15,657 patients. | analyze medical records and | demonstrating its potential use for automatic | accuracy: the accuracy of natural | ||
| processing pathway for | pan-specialized | identify incomplete excision | assessment of incomplete excision rates of basal | language processing depends on the | |||
| automated quality | analysis | rates in surgeries for the | cell carcinomas, which can help improve surgical | quality of the input dataand the ability | |||
| assurance in surgical | removal of basal cell | quality and patient follow-up. | of the algorithm to correctly interpret | ||||
| oncology: incomplete | carcinoma. | the information. | |||||
| excision rates of 34,955 | |||||||
| basal cell carcinomas | |||||||
| Robotic Microsurgery in | Besmens IS et al. | 2023 | Evaluation | 6 patients. | Use of the Symani Surgical | Microvascular anastomoses were slower than | Currently, the system has a narrow |
| Extremity | study on the use | System for extremity | with conventional microsurgery, but all | field of application. Although it can | |||
| Reconstruction - | of a new system | reconstruction. | anastomoses were patent. The platform’s | effectively suture vessels and nerves, | |||
| Experience with a Novel | for robotic | motion scaling enabled the surgeon to perform | it cannot dissect these structures. | ||||
| Robotic System | microsurgery | precise micromovements with minimal tissue | Surgeons must still rely on established | ||||
| manipulation alone, and difficult-to-reach | microsurgical techniques for surgical | ||||||
| anatomy became more easily accessible. | approaches and preparation of vessels | ||||||
| and nerves. | |||||||
| Computer-aided | Mattavelli D | 2024 | Preclinical study | 6 cadaver heads. | Reconstruction algorithm with | The reconstructive algorithm was feasible and | The limited sample size prevented any |
| designed 3D-printed | et al. | to investigate | 3 phases: 1) scaffold | reproducible in a preclinical setting. Functional | statistical analysis, and the | ||
| polymeric scaffolds for | the feasibility, | production (computer-aided | and esthetic results were satisfactory regardless | reconstruction algorithm test could | |||
| personalized | reproducibility, | design and three-dimensional | of the complexity of the defect. | only be performed twice for each | |||
| reconstruction of | and efficacy of a | printing in polylactic acid); 2) | defect type, i.e., the minimum to | ||||
| maxillary and | reconstruction | surgical simulation on cadaver | verify reproducibility. This small | ||||
| mandibular defects: a | algorithm | heads (navigation-guided | sample size limited the validity of the | ||||
| proof-of-concept study | osteotomies and scaffold | mechanical stress tests and prevented | |||||
| fixation); and 3) reconstruction | further analyses on the risk of | ||||||
| evaluation (bone and occlusal | infections, assessment of new bone | ||||||
| morphological conformity, | formation, and long-term integration | ||||||
| symmetry, and mechanical | of the scaffold. | ||||||
| stress tests). | |||||||
| VGG19 demonstrates | Lee JW et al. | 2024 | Study of | 8,173 training data | Establishment, training, and | The overall accuracy ranged from 74.0% to | A critical limitation was that wound |
| the highest accuracy | development | images and 904 | testing of 6 deep learning | 82.4%. VGG19 achieved the highest accuracy | photography was performed at a | ||
| rate in a nine-class | and validation | testing data images. | networks based on VGG16, | (82.4%) among all networks. | single institution under the same | ||
| wound classification | of a | VGG19, EfficientNet-B0, | settings (e.g., lighting, distance from | ||||
| task among various | classification | EfficientNet-B5, RepVGG-A0, | lens to objects). This system may | ||||
| deep learning networks: | system | and RepVGG-B0 on the same | demonstrate lower accuracy for | ||||
| a pilot study | wound images (divided into 9 | wound photographs in different | |||||
| classifications). | settings at different institutions. | ||||||
| Further research is required involving | |||||||
| a larger dataset from multiple | |||||||
| hospitals. | |||||||
| Robot-Assisted Pelvic Dissection for Enlarged Lymph Nodes in Melanoma Improves Recovery with Equivalent Oncological Outcomes to Open Pelvic Dissection | Roshan A et al. | 2024 | Retrospective observational cohort study | 22 patients. | The authors reviewed all patients who underwent pelvic lymph node dissection for macroscopic melanoma at a single institution and the methods used (open pelvic lymph node dissection [oPLND] or robot-assisted pelvic lymph node dissection [rPLND]). | rPLND is an effective way to remove bulky pelvic lymph nodes in patients with melanoma, with shorter recovery time and shorter interval to initiate adjuvant therapy compared with oPLND. | There were no statistical differences between the groups regarding the overall reported postsurgical complication rate. |
| Natural language processing to automate a web-based model of care and modernize skin cancer multidisciplinary team meetings | Ali SR et al. | 2024 | Analysis and validation study of informationextraction model | 893 patients (1,045 lesions). |
The authors used a web application with a custom application programming interface to provide an automated clinical decision support system for skin cancer. | Theaccuracy of the natural language processingbased tool was higher than human predictions, with an overall value of 0.92. | The article highlighted that these findings are preliminary and hypothesis-generating. As such, the next essential step in establishing the validity of this tool would be to apply it prospectively in an independent cohort, enabling a real-time assessment of its performance and reliability. |
| Revisiting basal cell carcinoma clinical margins: Leveraging natural language processing and multivariate analysis with updated Royal College of Pathologists histological reporting standards | Ali SR et al. | 2023 | Consecutive, multicentric, and panspecialized retrospective analysis study | 1,447 basal cell carcinomas. | The authors used a validated natural language processing information extraction model to analyze basal cell carcinomas treated with surgical excision using a predetermined clinical margin. | Larger clinical peripheral margins than those indicated by current guidelines may be required to achieve excision rates ::: 95%. | Although the study used natural language processing on more than 34 thousand basal cell carcinomas throughout 17 years, only 5% had complete data, limiting the credibility of the results. Therefore, result interpretation should be made with an additional degree of caution. |
| Easing the Burden on Caregivers- Applications of Artificial Intelligence for Physicians and Caregivers of Children with Cleft Lip and Palate | Chaker, Sara C et al. | 2024 | Analysis and validation study of an AI tool for patient assistance | 13 questions. | The authors asked questions about cleft lip, palate, or both to ChatGPT and compared the answers with those generated by senior pediatric plastic surgeons. | ChatGPT presented a 69% accuracy rate in answering postoperative questions when compared with experts; the major errors were regarding information. | Not applicable. |
| Artificial Intelligence in Plastic Surgery: Insights from Plastic Surgeons, Education Integration, ChatGPT’s Survey Predictions, and the Path Forward | Farid, Yasser et al. | 2024 | Qualitative analysis of knowledge research | 153 plastic surgeons. | The authors sent a 34-question survey on the role of AI in plastic surgery for plastic surgeons worldwide. | A significant proportion of plastic surgeons had limited experience with AI, with only 17.3% reporting moderate or extensive experience with AI in plastic surgery. One of the concerns raised by plastic surgeons is the potential overreliance on AI technology and its impact on clinical judgment. | Most respondents were from South America, limiting the generalization of the findings. Regional disparities in healthcare infrastructure, economic factors, and educational resources may influence plastic surgery practices and the integration of AI technologies. |
| Artificial Intelligence in Plastic Surgery: ChatGPT as a Tool to Address Disparities in Health Literacy | Wang, Anya et al. | 2024 | AI tool analysis study | Not applicable. | The authors used ChatGPT to transform informative material available on the internet about “breast reconstruction” into a 5th-grade language level. | ChatGPT could not unequivocally simplify health-related articles from a wide range of websites or replace physician-patient interactions. However, its ability to significantly increase the readability of patient resources led the authors to recommend ChatGPT as a tool for patients searching for information about plastic and reconstructive procedures and as an aid to medical professionals in understanding how to simplify their explanations of medical procedures to patients. | Not applicable. |
| Expanding Cosmetic Plastic Surgery Research with ChatGPT | Gupta, Rohun et al. | 2023 | Case study | Not applicable. | The authors asked ChatGPT to “give new systematic review ideas” for the top 6 surgical procedures and top 6 nonsurgical procedures in esthetic plastic surgery. | ChatGPT was a viable tool to help clinicians develop new systematic review ideas. The overall accuracy was of 55%. Furthermore, ChatGPTwas significantly more accurate when receiving specific prompts, resulting in an accuracy rate of 35% for general topics and 75% for specific topics. | The study had limitations, since the program training used a dataset that was last updated in September 2021. Some previously unpublished proposed systematic review topics were published in late 2021 or after that. |
Abbreviation: AI, artificial intelligence.
Discussion
The use of AI in surgical procedures has undergone significant developments in recent years. The studies in the current review show that integrating machine-learning methods with surgeons’ practices helps to achieve better outcomes in routine surgery. Four studies10-12 addressed AI integration in breast reconstruction surgery. This technology improved the visualization of blood vessels and tissues compared with reconstructions performed without the use of AI. As such, AI enabled the earlier identification of risk factors for the procedure, reducing intraand postoperative complications.10-12
Another significant issue is the evaluation of the performance of ChatGPT (OpenAI, Inc., San Francisco, CA, United States) in the provision of answers about plastic surgery.13-15 Fourteen studies reported on counseling provided by AI and demonstrated that ChatGPT can act as a supplementary tool for surgeons, offer crucial information to patients, and solve problems related to the surgical procedure.16 Studies13-15 also analyzed the surgeons’ view regarding the answers provided by ChatGPT when asked about daily procedures within plastic surgery. The surgeons pointed out that the answers provided by ChatGPT were relevant and accurate for simple questions. However, ChatGPT provided superficial answers for highly-complex topics, that is, a mere general overview.13-15
One topic worth highlighting is the use of deep learning, that is, machine learning based on algorithm predictive analysis, deemed an efficient tool for surgical wound management. Using this evaluation method, AI could identify infections and predict complications of postoperative wounds with a 96% accuracy rate.17 Furthermore, one article analyzing this same tool in burn patients demonstrated AI’s ability to predict graft-requiring sites, complication occurrence, and prolonged hospital stays due to skin lesions.18-20 Regarding the intraoperative period, the articles mostly addressed AI-provided AR. This tool significantly improves the visualization and planning of perforating flaps in reconstructive plastic surgery for a better understanding of the anatomy to increase the accuracy of the procedure. It is also worth noting that this visualization enables a projection of the volume, shape, and symmetry of the structures for reconstruction, rejuvenation, or beautification in the preoperative period.21,22
Although the current study presented promising results on AI use in plastic surgery, some critical limitations remain. First, AI is an emerging technology, and the lack of specific regulation represents a significant challenge. The absence of clear and standardized guidelines can compromise the safety and reliability of the data processed by AI tools, raising questions about result validation.23
Another relevant limitation is the bias associated with ethical and legal responsibility in AI-based medical decisions. The lack of regulation by health agencies leaves the role of AI in supporting clinical decisions undefined, creating uncertainty about liability in cases of errors or undesirable outcomes. This scenario highlights the urgent need for a regulatory framework considering patient protection and the legal security of health professionals.24-26
Furthermore, the effective use of AI tools in plastic surgery requires a high level of technical knowledge by medical teams, limiting its widespread adoption. The need for specialized training can create barriers to technology implementation in clinics and hospitals without sufficient resources for ongoing training.27,28
Finally, the black box concept inherent in many AI algorithms represents another crucial limitation. The lack of transparency in automated decision-making processes hinders the understanding of the origin and reason for certain recommendations. This opacity limits control over data and interferes with a critical result evaluation, potentially reducing the confidence of healthcare professionals in applying these tools.23
In summary, despite the advances, the full integration of AI in plastic surgery faces significant challenges that need to be addressed through adequate regulation, specialized training, and greater transparency in decision-making processes.
Conclusion
The analysis of the results highlights the growing incorporation of AI in plastic surgery. In different subspecialties, AI has shown its potential, such as in breast reconstruction, in which machine-learning techniques are used to improve the visualization of anatomical structures and identify risk factors early, contributing to the reduction of intraand postoperative complications. The reduction in the time required for the analysis and selection of recipient vessels, demonstrated in one of the studies, illustrates the efficiency AI can provide to surgical planning.
In addition, the assessment of ChatGPT’s performance revealed its value as a supplementary tool, providing support in clinical decision-making and improving communication with the patients. However, its limitations in more complex topics highlight the need for careful and judicious integration of this technology into the clinical practice. Other innovations, such as deep learning in surgical wound management and AR in reconstructive plastic surgery, have demonstrated positive impacts in optimizing clinical outcomes and improving the patient experience. Thus, AI adoption, with adequate regulation and ongoing training of healthcare professionals, can transform the practice of plastic surgery, leading to significant advances in esthetic and reconstructive medicine.
REFERENCES
1. Liang X, Yang X, Yin S, Malay S, Chung KC, Ma J, Wang K. Artificial Intelligence in Plastic Surgery: Applications and Challenges. Aesthetic Plast Surg 2021;45(02):784-790. Doi: 10.1007/s00266-019-01592-2
2. Jarvis T, Thornburg D, Rebecca AM, Teven CM. Artificial Intelligence in Plastic Surgery: Current Applications, Future Directions, and Ethical Implications. Plast Reconstr Surg Glob Open 2020;8 (10):e3200. Doi: 10.1097/GOX.0000000000003200
3. Spoer DL, Kiene JM, Dekker PK, Huffman SS, Kim KG, Abadeer AI, Fan KL. A Systematic Review of Artificial Intelligence Applications in Plastic Surgery: Looking to the Future. Plast Reconstr Surg Glob Open 2022;10(12):e4608. Doi: 10.1097/GOX.0000000000004608
4. Reyes JAE, Romero MP, Cobo R, Heredia N, Ruiz LAS, Zuluaga DAC. Artificial Intelligence in facial plastic and reconstructive surgery: a systematic review. Facial Plast Surg 2024;40(05):615-622. Doi: 10.1055/a-2216-5099
5. Murphy DC, Saleh DB. Artificial Intelligence in plastic surgery: What is it? Where are we now? What is on the horizon?. Ann R Coll Surg Engl 2020;102(08):577-580. Doi: 10.1308/rcsann.2020.0158
6. Abi-Rafeh J, Xu H, Kazan R, Tevlin R, Furnas H. Large Language Models and Artificial Intelligence: A Primer for Plastic Surgeons on the Demonstrated & Potential Applications, Promises, and LimitationsofChatGPT.AesthetSurgJ2023;•••;.Doi: 10.1093/asj/sjad260
7. Zhou XY, Guo Y, Shen M, Yang GZ. Application of artificial intelligence in surgery. Front Med 2020;14(04):417-430. Doi: 10.1007/s11684-020-0770-0
8. Chandawarkar A, Chartier C, Kanevsky J, Cress PE. A Practical Approach to Artificial Intelligence in Plastic Surgery. Aesthet Surg J Open Forum 2020;2(01):ojaa001. Doi: 10.1093/asjof/ojaa001
9. Hashimoto DA, Rosman G, Rus D, Meireles OR. Artificial Intelligence in Surgery: Promises and Perils. Ann Surg 2018;268(01): 70-76. Doi: 10.1097/SLA.0000000000002693
10. Seth I, Bulloch G, Joseph K, Hunter-Smith DJ, Rozen WM. Use of Artificial Intelligence in the Advancement of Breast Surgery and Implications for Breast Reconstruction: A Narrative Review. J Clin Med 2023;12(15): 5143. Doi: 10.3390/jcm12155143
11. Cevik J, Seth I, Hunter-Smith DJ, Rozen WM. A History of Innovation: Tracing the Evolution of Imaging Modalities for the Preoperative Planning of Microsurgical Breast Reconstruction. J Clin Med 2023;12(16): 5246. Doi: 10.3390/jcm12165246
12. Xie Y, Seth I, Rozen WM, Hunter-Smith DJ. Evaluation of the Artificial Intelligence Chatbot on Breast Reconstruction and Its Efficacy in Surgical Research: A Case Study. Aesthetic Plast Surg 2023;47(06):2360-2369. Doi: 10.1007/s00266-023-03443-7
13. Roberts RH, Ali SR, Hutchings HA, Dobbs TD, Whitaker IS. Comparative study of ChatGPT and human evaluators on the assessment of medical literature according to recognised reporting standards. BMJ Health Care Inform 2023;30(01):e100830. Doi: 10.1136/bmjhci-2023-100830
14. Chaker SC, Hung Y-C, Saad M, Golinko MS, Galdyn IA. Easing the Burden on Caregivers- Applications of Artificial Intelligence for Physicians and Caregivers of Children with Cleft Lip and Palate. Cleft Palate Craniofac J 2024;10556656231223596. Doi: 10.1177/10556656231223596
15. Farid Y, Fernando Botero Gutierrez L, Ortiz S, Gallego S, Zambrano JC, Morrelli HU, Patron A. Artificial Intelligence in Plastic Surgery: Insights from Plastic Surgeons, Education Integration, ChatGPT’s Survey Predictions, and the Path Forward. Plast Reconstr Surg Glob Open 2024;12(01):e5515. Doi: 10.1097/GOX.0000000000005515
16. Wang A, Kim E, Oleru O, Seyidova N, Taub PJ. Artificial Intelligence in Plastic Surgery: ChatGPT as a Tool to Address Disparities in Health Literacy. Plast Reconstr Surg 2024;153(06):1232e-1234e. Doi: 10.1097/PRS.0000000000011202
17. Gupta S, Gupta SS, McMath K, Sugandh S. Enhancing complex wound care by leveraging artificial intelligence: an artificial intelligence chatbot software study. Wounds 2023;35(08): E265-E267. Doi: 10.25270/wnds/23073
18. Zhang H, Zhao J, Farzan R, Alizadeh Otaghvar H. Risk predictions of surgical wound complications based on a machine learning algorithm. Syst Rev 2023;•••;. Doi: 10.1111/iwj.14665
19. Chang CW, Ho CY, Lai F, Christian M, Huang SC, Chang DH, Chen YS. Application of multiple deep learning models for automatic burn wound assessment. Burns 2023;49(05):1039-1051. Doi: 10.1016/j.burns.2022.07.006
20. Yeh CC, Lin YS, Chen CC, Liu CF. Implementing AI Models for Prognostic Predictions in High-Risk Burn Patients. Diagnostics (Basel) 2023;13(18):. Doi: 10.3390/diagnostics13182984
21. Qin F, Gu J. Artificial intelligence in plastic surgery: current developments and future perspectives. Plast Aesthet Res 2023; 10(01):1-8. Doi: 10.20517/2347-9264.2022.72
22. Berger MF, Winter R, Tuca AC, Michelitsch B, Schenkenfelder B, Hartmann R, et al. Workflow assessment of an augmented reality application for planning of perforator flaps in plastic reconstructive surgery: Game or game changer? Digit Health 2023; 9:20552076231173554. Doi: 10.1177/20552076231173554
23. Miragall MF, Knoedler S, Kauke-Navarro M, Saadoun R, Grabenhorst A, Grill FD, et al. Face the Future-Artificial Intelligence in Oral and Maxillofacial Surgery. J Clin Med 2023;12(21):6843. Doi: 10.3390/jcm12216843
24. Cevik J, Seth I, Rozen WM. Transforming breast reconstruction: the pioneering role of artificial intelligence in preoperative planning. Gland Surg 2023;12(09):1271-1275. Doi: 10.21037/gs-23-265
25. Mir MA. Artificial Intelligence Revolutionizing Plastic Surgery Scientific Publications. Cureus 2023;15(06):e40770. Doi: 10.7759/cureus.40770
26. Choi E, Leonard KW, Jassal JS, Levin AM, Ramachandra V, Jones LR. Artificial Intelligence in Facial Plastic Surgery: A Review of Current Applications, Future Applications, and Ethical Considerations. Facial Plast Surg 2023;39(05):454-459. Doi: 10.1055/s-0043-1770160
27. Hayajneh A, Shaqfeh M, Serpedin E, Stotland MA. Unsupervised anomaly appraisal of cleft faces using a StyleGAN2-based model adaptation technique. PLoS One 2023;18(08):e0288228. Doi: 10.1371/journal.pone.0288228
28. Yu S, Dwight J, Siska RC, Burkart H, Quan P, Yi F, et al. Feasibility of intra-operative image guidance in burn excision surgery with multispectral imaging and deep learning. Burns 2024;50(01): 115-122. Doi: 10.1016/j.burns.2023.07.005
1. Medicine Department, Universidade Federal de Ciências da Saúde de Porto Alegre,
Porto Alegre, RS, Brazil
2. Surgical Clinics Department, Universidade Federal de Ciências da Saúde de Porto
Alegre, Porto Alegre, RS, Brazil
Address for correspondence Carolina Guimarães Herzog, Departamento de Medicina, Universidade Federal de Ciências da Saúde de Porto Alegre, Porto Alegre, RS, Brazil (e-mail: carolinagherzog@gmail.com).
Article received: September 01, 2024.
Article accepted: November 16, 2024.
Conflict of Interests
The authors have no conflict of interests to declare.



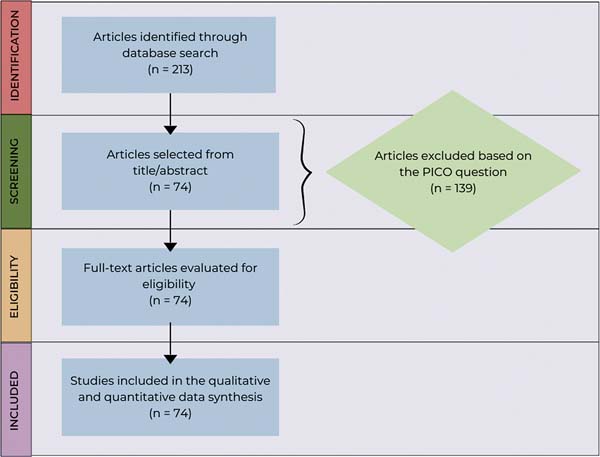

 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter