

Case Report - Year 2018 - Volume 33 -
Post-mammoplasty symmastia augmentation with silicone implants: treatment with quilting sutures
Simastia pós-mamoplastia de aumento com implantes de silicone: tratamento com suturas de adesão
ABSTRACT
Introduction: Augmentation mammoplasty is the most commonly performed esthetic surgical
procedure in the United States and second in Brazil. Symmastia is one of its
possible complications. This is defined as incorrect medial positioning of
the breast implants, which cross the midline, losing the intermammary
sulcus.
Methods: Work type, series of cases. Two patients underwent symmastia repair after
breast augmentation. The access route used was the previous inframammary
incision. The repair of the intermammary sulcus was performed by
scarification of the anterior and posterior capsule surfaces, associated
with adhesion suture with non-absorbable monofilament threat (4 lines with 6
points each, comprising a vertical band of approximately 4 cm wide in the
presternal region). In one of the cases, the implant was immediately
replaced, and in the other, the procedure was done 3 months later.
Results: In both cases, we obtained a new satisfactory intermammary sulcus, with
proper esthetic result. No recurrence was observed on follow-ups at 9 and 11
months.
Conclusions: The approach with adhesion sutures to redefine the intermammary sulcus was
effective in the treatment of symmastia after breast augmentation.
Keywords: Breast implants; Mammoplasty; Mammary diseases; Breast; Prostheses and implants
RESUMO
Introdução: A mamoplastia de aumento é o procedimento cirúrgico estético mais realizado
nos EUA e o segundo no Brasil. Simastia é uma de suas possíveis
complicações. Esta é definida como o mal posicionamento medial dos implantes
mamários, que cruzam a linha média, com perda do sulco intermamário.
Métodos: Trabalho tipo série de casos. Duas pacientes foram submetidas à correção de
simastia pós-mamoplastia de aumento. A via de acesso utilizada foi a incisão
inframamária prévia. A correção do sulco intermamário foi realizada por
escarificação das superfícies anterior e posterior da cápsula, associada a
pontos de adesão com fio monofilamentar não absorvível (4 linhas com 6
pontos cada, compreendendo uma faixa vertical de aproximadamente 4 cm de
largura na região pré-esternal). Em um dos casos o implante foi recolocado
imediatamente e, no outro, em procedimento realizado 3 meses após.
Resultados: Obtivemos um novo sulco intermamário satisfatório, com adequado resultado
estético em ambos os casos. Não se observou recorrência após 9 e 11 meses de
observação.
Conclusões: A abordagem com suturas de adesão para a redefinição do sulco intermamário
foi efetiva para o tratamento da simastia pós-mamoplastia de aumento.
Palavras-chave: Implantes de mama; Mamoplastia; Doenças mamárias; Mama; Próteses e implantes
INTRODUCTION
Breast augmentation is the most commonly performed cosmetic surgery in the United States and second in Brazil and worldwide1,2. Although symmastia might have rare congenital causes, it usually results from a complication of breast augmentation due to incorrect medial placement of implants, which approach too closely or cross the midline, causing intermammary sulcus loss3-5.
There are no reports in the literature regarding the incidence of iatrogenic symmastia5. The diagnosis is essentially clinical. It has a spectrum of intensity of symptoms, from mild cases that go unnoticed to severe cases presenting important psychosocial repercussions.
The main associated factors are excessive dissection of the implant plane toward the sternum, excessive division of the medial insertion of the pectoralis major muscle, use of implants with excessive diameter or volume, congenital symmastia, and presence of lateral anomalous bundles of the pectoralis minor muscle4. Some factors can generally be controlled by the surgeon, and iatrogenic symmastia can be prevented through subtle medial dissection, which thereby prevents excessive volume or very close positioning to the midline4-6.
Complications such as seromas, hematomas, infections, or other factors that lead to an increase in the pressure of plane or even a tissue adhesion rupture in the medial region of the plane also increase the risk of symmastia.
ObjeCtivE
To describe the experience and approach for the surgical treatment of iatrogenic symmastia.
CASE REPORT
Work type: case series. Two patients underwent surgical symmastia repair after breast augmentation with implants.
Patient 1
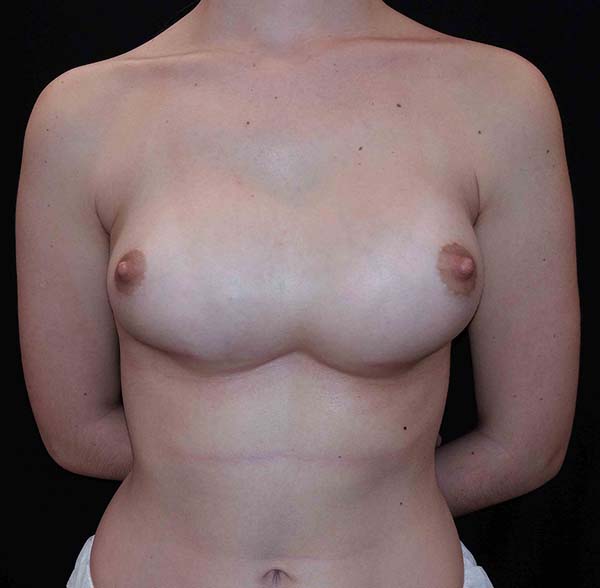
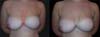
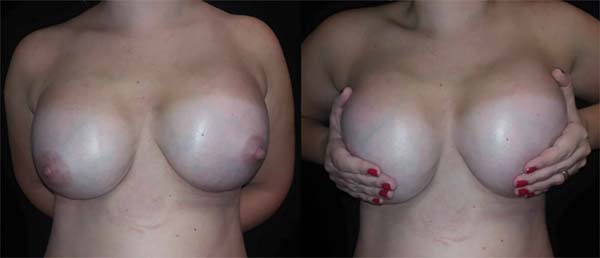
A 28-year-old patient underwent breast augmentation performed by another surgeon with 280-mL high-profile silicone implants (retroglandular) in 2008, and symmastia occurred. In 2009, the same surgeon changed the plane to retromuscular, and the symmastia recurred (Figures 1 and 2).
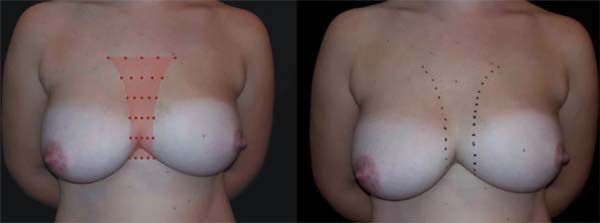
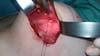
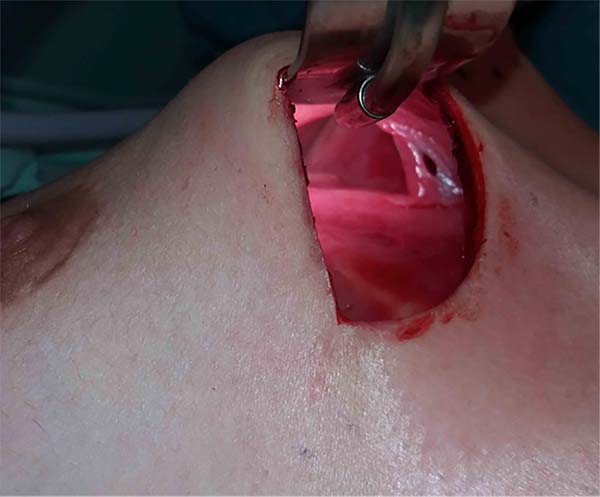
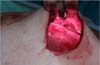
In 2016, she underwent surgical symmastia repair performed by the senior author of this article. A vertical band on the sternum, approximately 4 cm wide, was drawn (Figure 3). The access route used was the inframammary sulcus, over a previous scar. The implants were removed (Figure 4), and the capsule on its anterior and posterior bands was scarified by electrocautery (power 40, cauterization mode, electrocautery brand Valleylab®).
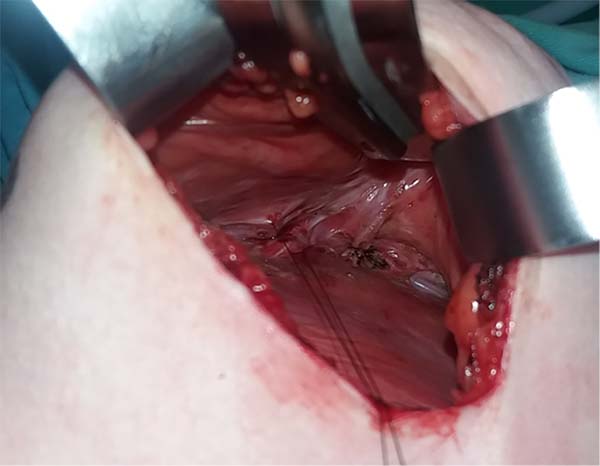
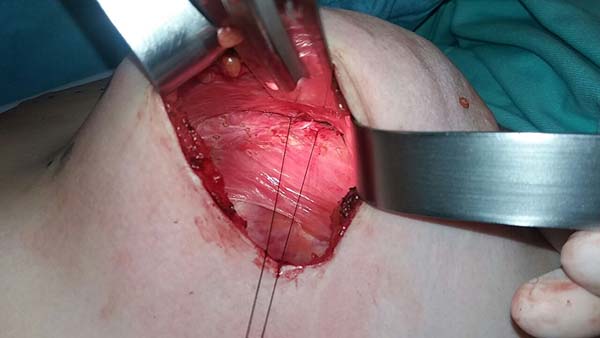
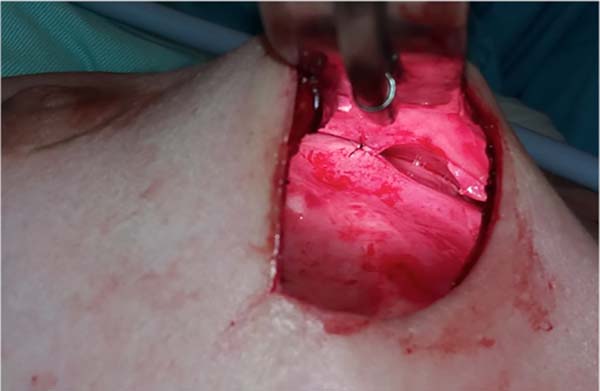
Adhesion sutures were made with 3-0 nylon thread between the anterior and posterior capsule surfaces (close to the sternum fascia) (Figure 5). Four lines with 6 sutures each were made, comprising a vertical band approximately 4 cm wide; 420-mL round, super-high-projection implants were inserted in the same plane (Figure 6). Delimitation and separation of the planes was obtained, with an improved positioning of the implants, 60 days post-operatively (Figure 7).
Patient 2
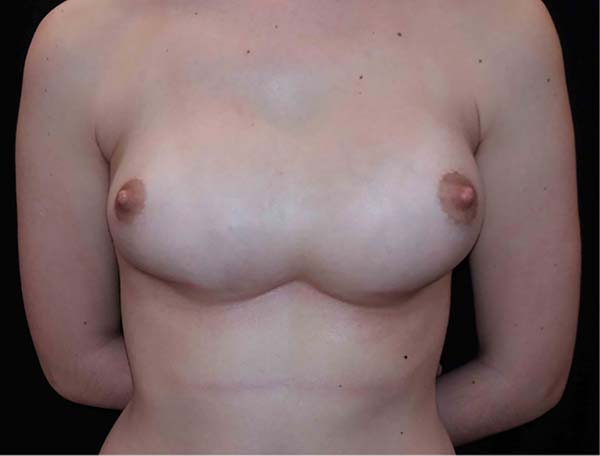
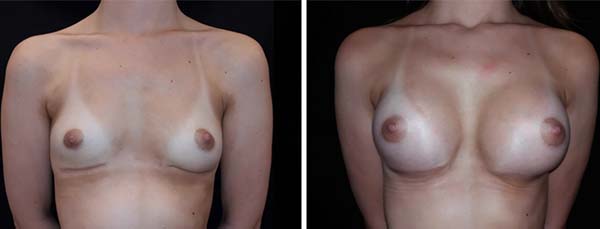
A 19-year-old patient underwent breast augmentation with 300-mL retromuscular, round, high-projection implants in January 2016. This procedure was performed by the senior author of the article. The patient developed seroma and infection of the surgical site, requiring the removal of the implants. Six months later, after she underwent new breast augmentation, with implants of the same volume and maintaining the retromuscular plane, symmastia occurred (Figure 8).
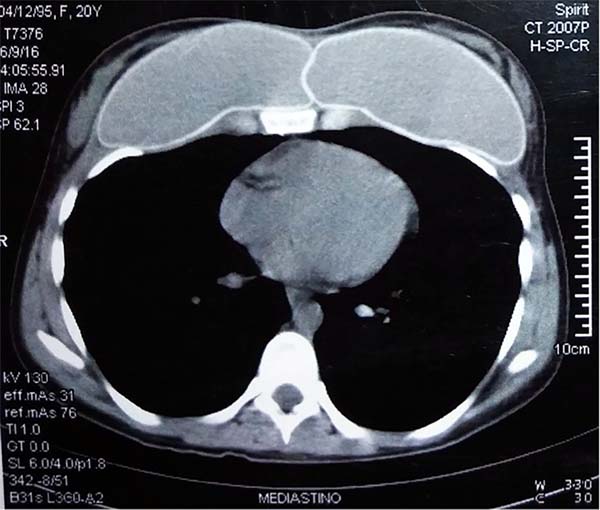
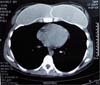
Computed tomographic examination showed total union of the planes and medialization of the implants (Figure 9). A 2-step approach was proposed: in the first procedure, the implants were removed, with the creation of a new medial sulcus using the same technique (scarification of the capsule surfaces, creation of a separation band approximately 4 cm between the planes, and creation of adhesion sutures with nylon 3-0 thread) (Figures 10 and 11). After 3 months, 280-mL round, super-high-projection breast implants were placed in the same plane, achieving symmastia repair and appropriate esthetic outcome (Figure 12).
For both patients, there was no recurrence during follow-ups at 9 and 11 months, respectively, for cases 1 and 2.
DISCUSSION
Identification of risk factors for preoperative symmastia and transoperative care are fundamental to avoid symmastia. Medial dissection should not exceed the horizontal distance of 1.5 to 3 cm from the midpoint between the sternum angle and the xiphoid process5.
Implants should not have dimensions that are extrapolated, as the literature shows that most symmastia cases are associated with implants with excessive diameter or volume4,5,7. The defect causing symmastia is usually found in the central part. Cases of symmastia in the upper and lower parts are rarer5.
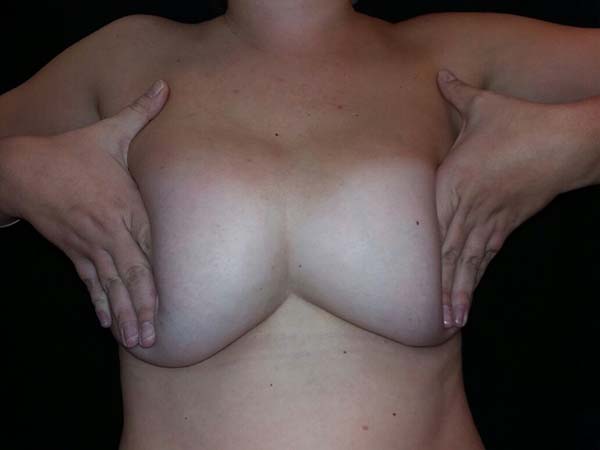
The diagnosis, in most of the cases, is evident and well defined, within 6 months after the primary procedure. In milder cases, maneuvers such as application of lateral pressure to both implants emphasize their anterior projection in the presternal region4,5. There are few studies in the literature on symmastia, and most of them are case series (Table 1).
| Author | Year | Journal | Number of cases |
|---|---|---|---|
| Becker | 2005 | Plastic Reconstrutive Surgery | 5 |
| Spear | 2006 | Plastic Reconstrutive Surgery | 20 |
| Spear et al.13 | 2009 | Plastic Reconstrutive Surgery | 23 |
| Moliver et al.4 | 2015 | Aesthetic Surgery Journal | 18 |
These works proposed different surgical techniques for the treatment. There is some agreement that the approach should be performed in a periareolar or inframammary manner, depending on the previous incision, for adequate operative field. Simple capsulorrhaphy may be effective and consists basically of a medial suture between the anterior and posterior edges of medial capsule, but despite its simplicity, its use is not very recommended due to the large number of recurrence cases reported7,8.
Lateral and/or upper capsulotomy may be associated with decreased tension at the medial edge. Another simple surgical option is the use of presternal transcutaneous sutures. Their use is debatable, since the area is at high risk for keloid formation, especially in patients with darker skin tones, despite being recommended to minimize scars in the region.
More complex capsulorrhaphy techniques have been described to decrease the risk of recurrence. Instead of a simple suture, using anterior and posterior flaps that overlap on the medial breast edge, providing greater support, is possible. However, the execution depends on a well-defined and mature capsule8,9. Another option for greater medial support is the use of a C-shaped acellular dermal matrix in the band, which is medially fixed. Such a technique is simple, but it adds cost to the procedure, despite its questionable benefits10.
Replacing the implant plan can be a treatment strategy. Retroglandular implants can be relocated to the retromuscular plane, providing better implant coverage11,12. Retromuscular implants can be relocated to the retroglandular plane if there is enough subcutaneous coverage6.
When there is insufficient coverage, repositioning the implants in an intermediate plane can be attempted. Spear et al.13 described good esthetic results in their series of 23 patients with subpectoral implants, which they attributed to the creation of neo-subpectoral regions, a new anterior and posterior plane to the capsule to the pectoralis major muscle, with no cases of recurrence.
Our repair procedure proposal used sutures between the anterior and posterior capsules under the medial sulcus, which is associated with the scarification of their surfaces and results in a good adherence between planes. Since there are no transcutaneous sutures, we avoided the risk of keloid formation. We believe that promoting adhesion between capsule surfaces, i.e., their scarification, is important. Electrocauterization was used with the aim of promoting local inflammation and increasing the possibility of adhesions.
The patient in case 1, who had mammary ptosis, was evaluated for the need for simultaneous mastopexy. Because of the complexity of managing several variables and to prevent the risk of breast devascularization, we chose to correct only symmastia and proposed to perform mastopexy at another time, depending on the need.
We observed that skin adhesion to the presternal region in the medial portion of the breasts and the creation of a new sulcus reduced excess skin, which we attribute to a mathematical explanation: the skin, in a situation of symmastia detected in a tomographic position (caudo-cranial), forms an almost straight line between the nipples. With symmastia repair, part of the excess skin is used when remaking the correct curvature of the medial poles of the breasts. We also observed a medialization of the areola-papillary complex. Such management proved to be successful and led to good esthetic results, with the patient being satisfied after the first surgery, with no need for a second intervention thus far.
Patient 2 presented with significant psychological impairment, due to 3 unsuccessful surgical interventions. Thus, the maintenance of a good doctor-patient relationship was fundamental for the therapeutic success of the case.
The literature suggests that in certain cases of difficult resolution of symmastia, the removal of the implants is primarily the best option, as it can immediately improve the esthetic aspect, giving the patient the closest semblance to the anatomy she had before breast augmentation13. When replacing the implants, we chose to use super-high-projection ones because they have a smaller base diameter, compared with high-projection implants, and thus occupy a smaller horizontal space.
CONCLUSION
Iatrogenic symmastia is a rare condition that has serious repercussions for the patient; hence, its prevention is fundamental. It is difficult to conclude which is the best technique for the correction of this condition because few studies were published, with only a small number of cases. Although our case series is modest, considering that this is a relatively rare condition, we believe the technique we described can be used in the treatment of this condition, which is complex and has a high rate of recurrence.
COLLABORATIONS
|
MP |
Analysis and/or interpretation of data; statistical analyses; final approval of the manuscript; conception and design of the study; completion of surgeries and/or experiments; writing the manuscript or critical review of its contents. |
|
FBF |
Analysis and/or interpretation of data; statistical analyses; final approval of the manuscript; conception and design of the study; completion of surgeries and/or experiments; writing the manuscript or critical review of its contents. |
|
EMZ |
Analysis and/or interpretation of data; statistical analyses; final approval of the manuscript; conception and design of the study; completion of surgeries and/or experiments; writing the manuscript or critical review of its contents. |
|
BDMG |
Analysis and/or interpretation of data; statistical analyses; final approval of the manuscript; conception and design of the study; completion of surgeries and/or experiments; writing the manuscript or critical review of its contents. |
|
FMFN |
Analysis and/or interpretation of data; statistical analyses; final approval of the manuscript; conception and design of the study; completion of surgeries and/or experiments; writing the manuscript or critical review of its contents. |
|
LMP |
Analysis and/or interpretation of data; statistical analyses; final approval of the manuscript; conception and design of the study; completion of surgeries and/or experiments; writing the manuscript or critical review of its contents. |
|
RSW |
Analysis and/or interpretation of data; statistical analyses; final approval of the manuscript; conception and design of the study; completion of surgeries and/or experiments; writing the manuscript or critical review of its contents. |
|
PBE |
Analysis and/or interpretation of data; statistical analyses; final approval of the manuscript; conception and design of the study; completion of surgeries and/or experiments; writing the manuscript or critical review of its contents. |
REFERENCES
1. American Society of Plastic Surgeons [Internet]. American Society of Plastic Surgeons. 2017 [cited 24 May 2017]. Available from: https://www.plasticsurgery.org
2. Surgery I. ISAPS - Sociedade Internacional de Cirurgia Plástica Estética (ISAPS) [Internet]. Isaps.org. 2017 [cited 24 May 2017]. Available from: http://www.isaps.org/pt/
3. Brown MH, Somogyi RB, Aggarwal S. Secondary Breast Augmentation. Plast Reconstr Surg. 2016;138(1):119e-35e. PMID: 27348674 DOI: http://dx.doi.org/10.1097/PRS.0000000000002280
4. Moliver CL, Sanchez ER, Kaltwasser K, Sanchez RJ. A Muscular Etiology for Medial Implant Malposition Following Subpectoral Augmentation. Aesth Surg J. 2015;35(7):NP203-10. DOI: http://dx.doi.org/10.1093/asj/sjv072
5. Selvaggi G, Giordano S, Ishak L. Synmastia: prevention and correction. Ann Plast Surg. 2010;65(5):455-61. DOI: http://dx.doi.org/10.1097/SAP.0b013e3181d37648
6. Lesavoy MA, Trussler AP, Dickinson BP. Difficulties with subpectoral augmentation mammaplasty and its correction: the role of subglandular site change in revision aesthetic breast surgery. Plast Reconstr Surg. 2010;125(1):363-71. PMID: 20048627 DOI: http://dx.doi.org/10.1097/PRS.0b013e3181c2a4b0
7. Foustanos A, Zavrides H. Surgical reconstruction of iatrogenic symmastia. Plast Reconstr Surg. 2008;121(3):143e-144e. PMID: 18317108 DOI: http://dx.doi.org/10.1097/01.prs.0000300199.69982.48
8. Yoo G, Lee PK. Capsular flaps for the management of malpositioned implants after augmentation mammoplasty. Aesth Surg J. 2010;34(1):111-5. DOI: http://dx.doi.org/10.1007/s00266-009-9456-3
9. Parsa FD, Koehler SD, Parsa AA, Murariu D, Daher P. Symmastia after breast augmentation. Plast Reconstr Surg. 2011;127(3):63e-65e. PMID: 21364388 DOI: http://dx.doi.org/10.1097/PRS.0b013e31820635b5
10. Curtis MS, Mahmood F, Nguyen MD, Lee BT. Use of AlloDerm for correction of symmastia. Plast Reconstr Surg. 2010;126(4):192e-193e. DOI: http://dx.doi.org/10.1097/PRS.0b013e3181ea92a3
11. Harley OJ, Arnstein PM. Retrocapsular pocket to correct symmastia. Plast Reconstr Surg. 2011;128(1):329-31. PMID: 21701362 DOI: http://dx.doi.org/10.1097/PRS.0b013e3182174661
12. Parsa FD, Parsa AA, Koehler SM, Daniel M. Surgical correction of symmastia. Plast Reconstr Surg. 2010;125(5):1577-9. PMID: 20440189 DOI: http://dx.doi.org/10.1097/PRS.0b013e3181d513f0
13. Spear SL, Dayan JH, Bogue D, Clemens MW, Newman M, Teitelbaum S, et al. The "neosubpectoral" pocket for the correction of symmastia. Plast Reconstr Surg. 2009;124(3):695-703. PMID: 19363454 DOI: http://dx.doi.org/10.1097/PRS.0b013e3181a8c89d
1. Universidade Federal de Ciências da Saúde de
Porto Alegre, Porto Alegre, RS, Brazil.
2. Santa Casa de Misericórdia de Porto Alegre,
Porto Alegre, RS, Brazil.
3. Universidade de Passo Fundo, Passo Fundo, RS,
Brazil.
4. Pontifícia Universidade Católica do Rio Grande
do Sul, Porto Alegre, RS, Brazil.
5. Universidade Federal de São Paulo, São Paulo,
SP, Brazil.
Corresponding author: Felipe Bilhar
Fasolin
Rua General Lima e Silva, 757, apto 1207 - Cidade Baixa
Porto Alegre, RS, Brazil Zip Code 90050-101
E-mail: felipefasolin@hotmail.com
Article received: October 09, 2017.
Article accepted: May 17, 2018.
Conflicts of interest: none.








 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter