

Ideas and Innovation - Year 2013 - Volume 28 - Issue 4
Practical model for tenorrhaphy training
Modelo prático para treinamento em tenorrafias
ABSTRACT
INTRODUCTION: The training of residents in surgical specialties is a challenge, since psychomotor skills are eventually acquired and developed in vivo in the very first attempt. The simulation techniques through practical models allows the resident's prior training, so that motor skills can be enhanced and evaluated in vivo before surgery. In the context of Plastic Surgery, the repair of tendons, especially flexors, presents technical difficulties during the first attempts of the resident.
OBJECTIVE: The proposed model is designed for practicing tenorraphies, designed to be easy reproducibility and low cost.
METHODS: We used a simulator using fixed mount, PVC pipe, pig tendons of legs and elastic envisioned to mimic the natural tension exists in the flexor tendons.
RESULTS: The model was satisfactory in the intention of allowing the simulation of tenorraphies, due to the similarities between human and pig tendons, and conferred by the elastic tension.
CONCLUSIONS: The model provided adequate training of motor skills in tendon sutures. This is an interesting option to be used in the early learning curve.
Keywords: Sutures. Training. Simulation. Tendons.
RESUMO
INTRODUÇÃO: O treinamento dos residentes de especialidades cirúrgicas representa um desafio, uma vez que as habilidades psicomotoras são, eventualmente, adquiridas e desenvolvidas in vivo já nas primeiras tentativas. A simulação das técnicas com o uso de modelos práticos permite o treinamento prévio do residente, de forma que as habilidades motoras possam ser incrementadas e avaliadas antes da cirurgia in vivo. No âmbito da Cirurgia Plástica, o reparo de tendões, em especial dos flexores, apresenta dificuldades técnicas durante as primeiras tentativas do residente.
OBJETIVO O modelo proposto foi idealizado para a prática de tenorrafias, idealizado para ser de fácil reprodutividade e baixo custo.
MÉTODO: Foi utilizado um simulador de tenorrafias utilizando suporte fixo, tubos de PVC, tendões de patas de suínos e elásticos idealizados para imitar a tensão natural existente nos tendões flexores.
RESULTADOS: O modelo utilizado mostrou-se satisfatório na intenção de permitir a simulação de tenorrafias, devido às semelhanças entre tendões humanos e suínos, além da tensão conferida pelos elásticos.
CONCLUSÕES: O modelo propiciou adequado treinamento de habilidades motoras nas suturas tendinosas. Trata-se de uma opção interessante a ser utilizada no início da curva de aprendizado.
Palavras-chave: Suturas. Treinamento. Simulação. Tendões.
To train residents in surgical specialties is a challenge because psychomotor skills should be readily acquired and developed in vivo right in the first attempt. The traditional educational structure of surgery, including clinical sessions, conferences, and classical principles such as "See it once, do it once, teach once," has no scientific basis to suport its implementation1.
At the beginning of their learning curve, residents tend to commit technical errors owing to surgical inexperience, which can potentially result in injury to the patient. Simulation techniques using practical models allow residents prior training so that motor skills can be enhanced and evaluated before surgery in vivo. Several training models have been described in several areas such as laparosco-py, and vascular and microsurgical anastomoses. Experimental animal or cadaveric models are also used but are more expensive and require appropriate physical space and approval by ethics committees, which often discourages residents in training. Within the context of plastic surgery, tendon repair, particularly of the flexor tendon, presents technical difficulties for residents during their first surgical attempts. Moreover, the functional result is closely related to the quality of the suture performed. Thus, the importance of previous training using practical models is fully justified.
OBJECTIVE
This paper aimed to present a practical training model in tenorrhaphy that is designed to have easy reproducibility and low cost.
METHODS
The training model that was idealized consisted of a simulator with the following components: 1) a wooden stand that measures 40 ' 10 ' 1.5 cm (length ' width ' height); 2) two "hook" screws that measure 0.75 in (20 mm); 3) two polyvinyl chloride (PVC) tubes that measure 10 ' 2.5 cm (length ' diameter); 4) two simple latex tourniquets 15 cm in length; 5) flexor tendons dissected from swine legs; 6) 3-0 nylon suture; 7) two 40 ' 12-mm needles; and 8) surgical suture instruments (needle holders, tweezers, and scissors). First, the simulator was assembled by fixing the hook screws to the ends of the stand at approximately 4.0 cm from the edge in the midline. Subsequently, the PVC pipes were fixed using bolts and nuts 6.0 cm from the edge of the stand, in the midline. The tourniquets were then bent at the distal 5.0 cm and tied tightly with nylon. The pig tendons were sutured to the tourniquets and passed inside the PVC pipe, and knotted to the hook of the screw. Any excess tendon was resected so that a gap of 1.0 cm remains to allow the elastic tourniquet to simulate the natural tension of the flexor tendons. After proper installation, tenorrhaphic simulation was performed by the residents and students of the Department of Plastic Surgery using the various simulation techniques described, along with appropriate surgical instruments.
RESULTS
The simulator satisfactorily simulated tenorrhaphy. The pig tendon presents a consistency, elasticity, and diameter very close to those of the human tendon, enabling realistic sutures. The tourniquet sutured to the tendon was enough to mimic the tension in the flexor tendons in vivo. The wooden stand, hook screws, and PVC pipes were low-cost and easy to install. Assessment of the effectiveness of training is subjective and difficult, and we suggest the implementation of a protocol that employs multiple variables for evaluation, preferably by an experienced surgeon. Nevertheless, we noted a subjective increase in the confidence level of the residents and academics who underwent training using our simulation model, particularly with regard to their skill in suturing.

Figure 1 - The tenorrhaphic simulator and materials necessary for practice in suturing.

Figure 2 - The simulator fitted with swine tendons already in place.

Figure 3 - Tendons transfixed by needles, ready for suturing.

Figure 4 - Performing the tenorrhaphy with nylon thread.
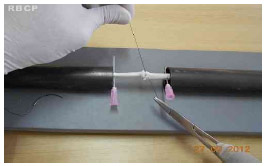
Figure 5 - Completing the tenorrhaphy.

Figure 6 - Final aspect of the simulator after the suture .
DISCUSSION
Surgical simulation of tenorrhaphy using practical models has been poorly described in the literature. Prior resident training in suturing techniques for flexor tendon repair using such simulators increases confidence level, reduces anxiety, and improves the quality of suture of residents during their first attempt at surgery in vivo2. The importance of a well-performed tendon suture is apparent in the low rate of adhesion and improved functional outcome. The proposed model features easy assembly and handling, low cost, and excellent simulation capability.
Swine tendons kept in saline solution have a consistency that is very close to that of human tendons. The diameter of the swine Achilles tendon is also similar to that of the finger flexor tendon. Elastic tourniquets exert a continued tension in the suture zone, which is relieved by the passage of needles, which are retained in the PVC pipe. That this step is also commonly performed in sutures in vivo is worth noting; the needle is passed through the skin or phalanges. The PVC tubes also act as centralizers, simulating, in a way, the sheaths and pulleys. The sutures can then be performed using the various techniques described earlier. A total of 10 sutures were performed by each resident, for a total of only 90 min of training, which is considered sufficient for the purpose of introductory training2.
CONCLUSION
Our proposed simulation model of tenorrhaphy provided the residents in this study adequate training of motor skills in tendon suturing. The materials used in devising the model are easily accessible, low-cost, and in line with the aim of the proposed model. The flexor tendons in vivo were well simulated by the swine tendons simulated. According to the literature, prior training using simulation models makes it easier for residents to begin their learning curve, and our proposed model is an interesting option for use in tenorrhaphy training.
REFERENCES
1. Dunkin B, Adrales GL, Apelgren K, Mellinger JD. Surgical simulation: a current review. Surg Endosc. 2007;21(3):357-66.
2. Ingraham JM, Weber RA 3rd, Weber RA. Utilizing a simulated tendon to teach tendon repair technique. Hand (N Y). 2009;4(2):150-5.
3. Gomes AAR, Soares FVC, Pessoa SGP. Modelo de treinamento em palatoplastia. Rev Bras Cir Plást. 2011;26(4):691-
4. McLarney E, Hoffman H, Wolfe SW. Biomechanical analysis of the cruciate four-strand flexor tendon repair. J Hand Surg Am. 1999;24(2):295-301.
5. Dias IS, Pessoa SGP, Benevides AN, Macêdo JE. Treinamento inicial em microcirurgia. Rev Bras Cir Plást. 2010;25(4):595-9.
1. General Surgeon, Physician-Resident in Plastic Surgery
2. MSc in Surgery (UFC), Full Member of the SBCP, Head of the Plastic Surgery Service of the Walter Cantídio University Hospital (UFC), and Head of Plastic Surgery of the Surgery Department of UFC
3. Specialist Member of the SBCP, Plastic Surgeon at the Plastic Surgery and Reconstructive Microsurgery Department of the Walter Cantídio University Hospital, Fortaleza, CE, Brazil
4. Student, seventh semester, Medical School, Christus Faculty (Fortaleza-CE)
5. Student, fifth semester, Medical School, Federal University of Ceará (UFC)
6. Student, seventh semester, Medical School, Federal University of Ceará (UFC)
7. Specialist Member of the SBCP Plastic Surgeon, Department of Plastic Surgery and Reconstructive Microsurgery, University
Vitor De Vasconcellos Muniz
Rua Monsenhor Bruno 1101, apto 403 Bairro: Aldeota
Fortaleza - CE
Article received: 9/10/2013
Article accepted:23/11/2013
work performed at Instituto Nacional do Câncer, Rio de Janeiro, RJ, Brasil.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter