

Original Article - Year 2012 - Volume 27 -
Forehead reduction using precapillary incision: experience report and indications
Redução da região frontal com incisão pré-capilar: relato de experiência e indicações
ABSTRACT
BACKGROUND: A long forehead can give a less attractive and disproportionate appearance. It may also indicate aging. The objective of this study is to show the experience of the authors in forehead reduction using precapillary incision and to support the indications for this procedure.
METHODS: Patients who underwent precapillary incision for forehead reduction between 2005 and 2011 were retrospectively analyzed. The indications for an anterior hairline incision were eyebrow ptosis in patients with thin and sparse frontal hair, congenital long forehead, or extensive forehead wrinkles.
RESULTS: Precapillary incision was performed in 31 patients, who were followed up for an average of 1.5 years. No problems related to flap vascularization were detected. All patients reported temporary paresthesia, from which they recovered within 1 year. Three patients presented seromas during the postoperative period and were treated using puncturing. All patients reported that the benefits of altering the hairline were greater than the disadvantages of a possibly more visible scar.
CONCLUSIONS: Frontal rhytidectomy using precapillary incision is recommended in patients who wish to correct thin and sparse frontal hair, extensive forehead wrinkles, or congenital/ senile long forehead.
Keywords: Forehead/surgery. Rhytidoplasty. Rejuvenation.
RESUMO
INTRODUÇÃO: A testa longa pode dar uma aparência menos atraente, desproporcional e caracterizar o envelhecimento. O objetivo deste trabalho é demonstrar a experiência dos autores na redução da região frontal com incisão pré-capilar e reforçar as indicações desse procedimento.
MÉTODO: Foram estudados, retrospectivamente, pacientes submetidos a redução da região frontal por incisão pré-capilar, no período de 2005 a 2011. As indicações para incisão anterior na linha do cabelo foram ptose da sobrancelha, em pacientes que possuíam cabelos frontais finos e escassos, testa longa congênita ou enrugamento amplo de testa.
RESULTADOS: A incisão pré-capilar foi realizada em 31 pacientes, com acompanhamento médio de 1,5 ano. Não houve problemas relacionados à vascularização do retalho. Todos os pacientes relataram parestesia temporária, com recuperação em até 1 ano. Três pacientes apresentaram seromas no pós-operatório, tratados com punção. Todos os pacientes relataram que os benefícios da redução da linha do cabelo ultrapassaram as desvantagens de uma cicatriz possivelmente mais visível.
CONCLUSÕES: O procedimento de ritidectomia frontal com incisão pré-capilar é indicado para pacientes com cabelos frontais finos e escassos, com enrugamento amplo da testa ou com testa longa congênita/senil e que desejem reduzi-la.
Palavras-chave: Testa/cirurgia. Ritidoplastia. Rejuvenescimento.
In 1926, Hunt1 reported an anterior hairline incision with skin removal to correct forehead wrinkles. In 1961, Pangman & Wallace2 used the same approach for the correction of forehead wrinkles and eyebrow ptosis. In 1965, Uchida3 described an anterior hairline approach, with galeal and subcutaneous isolation of the frontal muscle. In this method, the upper portion of the skin was removed and the lower portion of the frontal muscle was sutured to the skin flap. In 1973, Rees & Wood-Smith4 reported the possibility of circulatory impairment and hair loss associated with subcutaneous dissection when a coronal approach was used. In 1982, Connell et al.5 recommended the anterior broken-hairline incision, with subgaleal dissection. The authors also emphasized the necessity of meticulous closure of the layers to obtain satisfactory results.
The normal proportions and the main aesthetic units of the face have already been defined and are used to evaluate the size of the forehead, which is the segment extending from the glabella to the frontal hairline6-8 (Figures 1 and 2). A long forehead can give a less attractive and disproportionate appearance. Moreover, it may indicate aging.
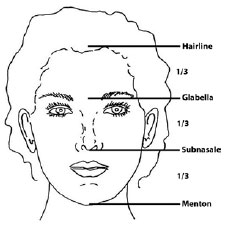
Figure 1 - For a proportional face, the height of the forehead should correspond to one-third of the total facial height. Reproduced from Marten17.
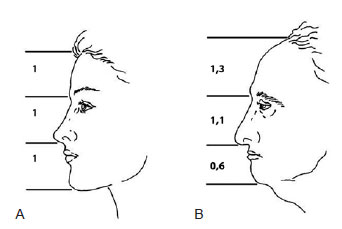
Figure 2 - Facial disproportion and aging. In A, the young face is divided into 3 equal parts. In B, the aged face, the superior one-third of the face (forehead) is generally larger than the medial and lower segments. Reproduced from Marten17.
Until 1990, most of the reports on forehead rhytidectomy described the use of coronal incision, with subgaleal or subcutaneous dissection6. Between 1980 and 1990, innovations in endoscopic approaches revolutionized orthopedics, general surgery, and gynecology, and reached plastic surgery, particularly procedures concerning forehead treatment9,10. However, coronal incisions or endoscopic procedures elevate the anterior hairline, which is one of the reasons why many surgeons do not routinely recommend these procedures11,12. These approaches are not suitable for patients with thin and sparse frontal hair, congenital/senile long foreheads, or extensive forehead wrinkles6,9-18.
The aim of this study is to report our experiences in forehead reduction using precapillary incision and to support the indications for this procedure.
METHOD
This is a descriptive retrospective study, which was performed by analyzing the medical records of patients who underwent facial rhytidectomy with forehead reduction using precapillary incision between 2005 and 2011.
Patients complaining of eyebrow ptosis and long foreheads were divided into 3 groups according to the length of their foreheads as follows: (1) patients with eyebrow ptosis and slight forehead elongation; (2) patients with moderate forehead elongation; and (3) patients with severe forehead elongation, who were candidates for forehead reduction using precapillary incision.
The primary indications for anterior hairline incision are eyebrow ptosis for patients with thin and sparse frontal hair, congenital long forehead, or extensive forehead wrinkles. Another indication is a clear interest shown by the patient for the procedure. Otherwise, a coronal approach is commonly used to obtain upper facial rejuvenation.
Procedure
To determine the severity of eyebrows ptosis and to plan the extent of forehead reduction desired, patients were examined in the orthostatic position. Surgeries were performed under general anesthesia and were performed along with other cosmetic procedures. A broken-line incision was marked in the anterior hairline, immediately behind the junction of the hair with the forehead (Figure 3).
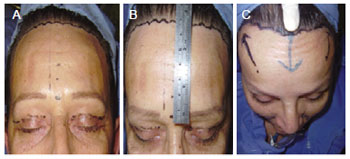
Figure 3 - In A, precapillary broken-line mark. In B, forehead size measurement. In C, advancement of the flap.
Local infiltration with 0.9% saline solution and epinephrine in a 1:200,000 proportion was applied to the incision site and the area to be dissected. As soon as the effect of epinephrine set in, a subgaleal incision was performed along the skin marks and the distribution of the hair follicles19 (Figure 4).
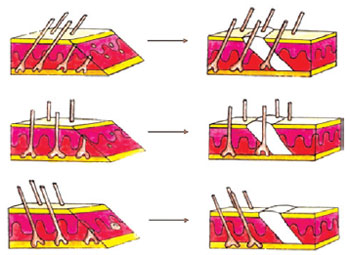
Figure 4 - Effect of hair follicle orientation in a visible scar with beveled incision. Figure extracted from Mowlavi et al.19.
Precise dissection with scissors was performed to separate the skin from the septa that strongly adheres to the frontal muscle (Figure 5). Then, after gaining access, the subgaleal plane could easily by was easily dissected. Atraumatic tissue handling was important to prevent vascular impairment. The dissection was extended up to the supraorbital bilateral rim, and if necessary, to the nasal dorsum. The scalp was dissected up to the parieto-occipital region to ensure easy advancement of the flap. At this point, an easy access to the frontal, procerus, and corrugator muscles rendered easy dissection possible, when necessary (Figure 6). The supratrochlear nerve and veins are located in this region; therefore, the surgeon should act cautiously to avoid inadvertent injury. Homeostasis was achieved, the region was irrigated, and the flap was subsequently repositioned. The excess skin was marked and gradually removed to avoid excessive tension on the scar (Figure 7). Suturing was performed in planes using 4.0 and 5.0 monofilament nylon threads.
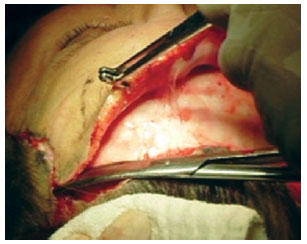
Figure 5 - Precise dissection of the frontal flap.
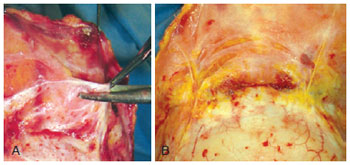
Figure 6 - In A, separate section of the frontal muscle. In B, final aspect after dissection of the frontal muscle, procerus, and corrugator, with preservation of the supratrochlear neurovascular bundle.
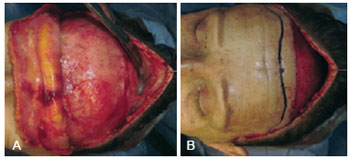
Figure 7 - In A, folded frontal flap and subgaleal parieto-occipital dissection. In B, excess skin mark after advancement of the flap.
The quantity of skin incised in the brow-lift varied. No drains were used; however, a pressure-dressing pad was applied. Because applying hot water or ice could cause injury to the dormant tissue, specific guidelines were provided to the patients to prevent possible complications. Stitches were removed 7 to 10 days after surgery.
RESULTS
Precapillary incision was performed in 31 patients, 30 women and 1 man, who were followed up for a period ranging from 3 months to 5 years, with an average follow-up of 1.5 years.
One patient complaining of a long forehead underwent a secondary rhytidectomy procedure, which was performed 3 years after treatment of the middle and lower one-third part of his forehead.
No patient in this study presented with flap vascularization complications. Hematomas, hypertrophic scars, facial nerve lesions, alopecia, or infections were not observed.
All patients reported temporary paresthesia, but 87% of them showed sensory recovery within 6 months and the rest within 1 year. Three patients (9.67%) presented with postoperative seromas, which were treated using puncturing. All patients reported that the benefits of forehead reduction were greater than the disadvantages of a possibly more visible scar (Figures 8 and 9).
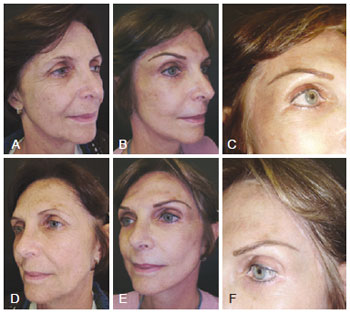
Figure 8 - In A and D, right and left preoperative profile, respectively. In B and E, right and left postoperative profile, respectively, 6 months after surgery. In C and F, precapillary aesthetic scar, easily concealed by hairs.
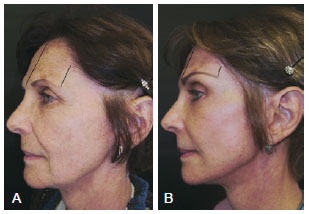
Figure 9 - In A, preoperative profile. In B, postoperative profile (6 months). Marks show reduction of forehead length and brow-lift.
DISCUSSION
Basic forehead-lift procedures have been reported since 1926. These procedures are similar to a mini facelift or early rhytidectomy, in which small ellipses of skin are resected, with minor or no morbidity. Currently, there is a better understanding of the periorbital aesthetic unit as well as the functional anatomy of the muscular groups in this region, which with the passage of time, results in the accumulation of muscular actions, thereby generating dynamic and static wrinkles. Dynamic wrinkles are efficiently treated and can be smoothened using botulinum toxin. However, there is a general consensus that treatment of static wrinkles requires the use of other techniques such as fillers and surgical procedures, which can be endoscopic or can involve conventional open surgery.
To optimize the results of surgery, an individualized approach becomes necessary. Therefore, the endoscopic procedure or bicoronal incision provides better cosmetic results in patients with standard normal hair and a low anterior hairline. In contrast, precapillary incision is the best indication in patients with a high anterior hairline insertion (long forehead), extensive wrinkling, or very thin skin6,9-18. In our experience, we have performed extensive subgaleal detachment, advancing the flaps from the forehead and scalp, without detecting cases of alopecia or flap necrosis. Moreover, we did not require to perform galeatomy or rigid fixation of the flap (with screws), as described by other authors15,17. The patients should be asked to stop smoking 30 days before the procedure and during the postoperative period.
The results obtained with the endoscopic procedure in the first 10 years of experience were satisfactory, although published studies suggested the existence of a learning curve and early recurrence of ptosis, which discouraged many surgeons9. However, recent advances in fixation techniques have led to longer lasting results and better acceptance of the procedure. Therefore, the endoscopic procedure is currently seen by many surgeons as the best option for forehead reduction, eyebrow ptosis correction, and periorbital and frontal muscle treatment, as it allows good visualization and minimal morbidity10-12.
In many institutions, the endoscopic technique has become the most commonly performed procedure, whereas the conventional open technique has assumed a lesser role, creating certain stereotypes that cannot replace the knowledge and pre-existing experience associated with open surgery.
Several difficulties associated with open procedures, which account for poor acceptance by the patient and high morbidity, are frequently described in the literature. However, during conventional open procedures, many experienced surgeons have reported patient satisfaction and a complication rate comparable to or lower than endoscopic techniques7,18.
Experienced surgeons require little special equipment to provide long lasting results with open procedures. For many patients, the benefits of forehead reduction, with hairline lowering, exceed the disadvantages of an anterior hairline position and the possibility of a more visible scar.
CONCLUSIONS
Frontal rhytidectomy using precapillary incision is commonly indicated in patients who wish to correct thin and sparse frontal hair, extensive forehead wrinkles, or a congenital/ senile long forehead. In these cases, a frontal facelift is recommended.
The technique of forehead reduction using precapillary incision is safe and enables an easy brow-lift, with tensionfree closure and acceptable scars. Moreover, it provides good access to treat the underlying muscles. The success rate that we have experienced with this approach has led us to recommend this procedure to selected patients.
REFERENCES
1. Hunt HL. Plastic surgery of the head, face, and neck. Philadelphia: Lea & Febiger; 1926.
2. Pangman WJ 2nd, Wallace RM. Cosmetic surgery of the face and neck. Plast Reconstr Surg. 1961;27:544-50.
3. Uchida JI. A method of frontal rhytidectomy. Plast Reconstr Surg. 1965;35:218-22.
4. Rees TD, Wood-Smith D. Cosmetic facial surgery. Philadelphia: WB Saunders; 1973.
5. Connell BF, Lambros VS, Neurohr GH. The forehead lift: techniques to avoid complications and produce optimal results. Aesthetic Plast Surg. 1989;13(4):217-37.
6. Guyuron B, Davies B. Subcutaneous anterior hairline forehead rhytidectomy. Aesthetic Plast Surg. 1988;12(2):77-83.
7. Farkas LJ, Kolar JC. Anthropometrics and art in the aesthetics of women's faces. Clin Plast Surg. 1987;14(4):599-616.
8. Powell H, Humphrieys B. Proportions of the aesthetic face. New York: Thieme-Stratton; 1984.
9. Chiu ES, Baker DC. Endoscopic brow lift: a retrospective review of 628 consecutive cases over 5 years. Plast Reconstr Surg. 2003;112(2):628-33.
10. Chadwell JB, Mangat DS. The endoscopic forehead-lift. Facial Plast Surg Clin North Am. 2006;14(3):195-201.
11. Dayan SH, Perkins SW, Vartarian AJ, Wiesman IM. The forehead lift: endoscopic versus coronal approaches. Aesthetic Plast Surg. 2001;25(1):35-9.
12. Puig CM, LaFerriere KA. A retrospective comparison of open and endoscopic brow-lifts. Arch Facial Plast Surg. 2002;4(4):221-5.
13. de la Torre JI, Paulsen SM, Decordier B, Al-Hakeem MS, Vasconez LO. Secondary endoscopic forehead lift in patients with previous coronal brow lift. Ann Plast Surg. 2005;54(3):251-5.
14. Cilento MD, Johnson CM Jr. The case for open forehead rejuvenation: a review of 1004 procedures. Arch Facial Plast Surg. 2009;11(1):13-7.
15. Guyuron B, Behmand RA, Green R. Shortening of the long forehead. Plast Reconstr Surg. 1999;103(1):218-23.
16. Guyuron B, Rowe DJ. How to make a long forehead more aesthetic. Aesthet Surg J. 2008;28(1):46-50.
17. Marten TJ. Hairline lowering during foreheadplasty. Plast Reconstr Surg. 1999;103(1):224-36.
18. De Cordier BC, de la Torre JI, Al-Hakeem MS, Rosenberg LZ, Gardner PM, Costa-Ferreira A, et al. Endoscopic forehead lift: review of technique, cases, and complications. Plast Reconstr Surg. 2002;110(6):1558-68.
19. Mowlavi A, Majzoub RK, Cooney DS, Wilhelmi BJ, Guyuron B. Follicular anatomy of the anterior temporal hairline and implications for rhytidectomy. Plast Reconstr Surg. 2007;119(6):1891-5.
1. Preceptor of the Serviço de Cirurgia Plástica do Hospital Daher Lago Sul (Plastic Surgery Service of the Hospital of Daher Lago Sul), full member of Sociedade Brasileira de Cirurgia Plástica (Brazilian Society of Plastic Surgery) - SBCP, Brasília, DF, Brazil.
2. Specialist in General Surgery, aspiring member of the SBCP, resident doctor at the Serviço de Cirurgia Plástica do Hospital Daher Lago Sul (Plastic Surgery Service of the Hospital of Daher Lago Sul), Brasília, DF, Brazil.
3. Preceptor of the Serviço de Cirurgia Plástica do Hospital Daher Lago Sul (Plastic Surgery Service of the Hospital of Daher Lago Sul) and Hospital das Forças Armadas (Armed Forces Hospital), full member of SBCP, Brasília, DF, Brazil.
Correspondence to:
José Nava Rodrigues
Hospital Daher
Lago Sul, SHIS, QI 7 - cjto. F
Brasília, DF, Brazil - CEP 71615-570
E-mail: navarodhot@yahoo.com.br
Article submitted to SGP (Sistema de Gestão de Publicações/Manager Publications System) of RBCP (Revista Brasileira de Cirurgia Plástica/Brazilian Journal of Plastic Surgery).
Article received: March 31, 2012
Article accepted: May 6, 2012
Study conducted at the Serviço de Cirurgia Plástica do Hospital Daher Lago Sul (Plastic Surgery Service of the Hospital of Daher Lago Sul), Brasília, DF, Brazil.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter