

Original Article - Year 2011 - Volume 26 -
Abdominoplasty after gastroplasty: evaluation of 100 cases operated on by the "fish" technique
Dermolipectomia abdominal pós-gastroplastia: avaliação de 100 casos operados pela técnica do "peixinho"
ABSTRACT
BACKGROUND: Morbid obesity is a worldwide endemic disease. Its growing incidence makes it a public health problem. Bariatric surgery is an alternative weight loss method with the objective of controlling obesity-associated diseases and improving quality of life. The surgical treatment of the deformities resulting from significant weight loss is a new challenge for plastic surgeons. This paper presents a new technique for abdominoplasty in formerly obese patients with a midline abdominal scar resulting from gastroplasty.
METHODS: A total of 28 men and 72 women who underwent abdominoplasty after gastroplasty by the "fish" technique described in this study were analyzed.
RESULTS: The results obtained with the technique presented were satisfactory, resulting in a new body contour and a low complication rate.
CONCLUSIONS: Abdominoplasty with markings forming a fish shape is successful for the removal of excess abdominal skin in patients who underwent bariatric surgery.
Keywords: Surgery, plastic/methods. Abdomen/surgery. Gastroplasty. Bariatric surgery.
RESUMO
INTRODUÇÃO: A obesidade classe III é uma doença endêmica em todo o mundo. Trata-se de problema de saúde pública em decorrência de sua incidência progressiva. A cirurgia bariátrica oferece alternativa de redução ponderal, visando ao melhor controle das doenças que têm a obesidade como fator de risco e à melhoria da qualidade de vida. O tratamento cirúrgico das deformidades secundárias a grandes emagrecimentos é um novo desafio ao cirurgião plástico. O objetivo deste trabalho é apresentar uma nova técnica para abdominoplastia do paciente ex-obeso, portador de cicatriz abdominal mediana decorrente de gastroplastia.
MÉTODO: Foram analisados 28 homens e 72 mulheres, submetidos a dermolipectomia abdominal pós-gastroplastia, segundo a técnica do "peixinho", apresentada neste trabalho.
RESULTADOS: A técnica apresentada demonstrou-se satisfatória, resultando em novo contorno corporal, com baixo índice de complicações.
CONCLUSÕES: A abdominoplastia com marcação em peixe é mais uma opção no arsenal do cirurgião plástico para tratamento do excedente cutâneo do abdome de pacientes submetidos a cirurgia bariátrica.
Palavras-chave: Cirurgia plástica/métodos. Abdome/cirurgia. Gastroplastia. Cirurgia bariátrica.
Morbid obesity is a worldwide endemic disease. It is related to genetic, endocrine, behavioral, and environmental factors. Morbidly obese patients are at an increased risk of developing diabetes, cardiovascular diseases, and the condition can also be fatal. There are about 15 million obese people in the United States and among them approximately 5 million are morbidly obese. In Brazil, it is estimated that there are about 10 million obese people, of which 100 thousand are morbidly obese. Bariatric surgery was developed with the purpose of reducing the risk factors associated with obesity and to improve the quality of life of these individuals.
Specialized centers and multi-specialty teams have developed specific treatment protocols, including surgical, nutritional, and psychological management of obese patients. Candidates for surgery should have a body mass index (BMI) > 40 or BMI > 35 along with comorbidities. As the bariatric surgery technique evolved, malabsorptive procedures were replaced by mixed techniques (restrictive and malabsorptive), which offer a better nutritional prognosis for the patient1.
The plastic surgeon is responsible for removing the cutaneous excess skin arising from significant weight loss2. Vertical and horizontal skin sagging and a supraumbilical median scar are common consequences of gastroplasty. Initially, the plastic surgeon is responsible for advising the formerly obese patient with regard to the patient's expectations3 of the outcome of plastic surgery. The reconstructive character of the surgery, the possible generation of new scars, and the limitations of the classic abdominoplasty should be emphasized4,5.
Abdominoplasty for the treatment of excess skin in formerly obese patients began with Kelly6, at the beginning of the 20th century. In the 1960s, several variations of the procedure were proposed by authors such as Castañares & Goethel7, who described a vertical and horizontal resection resulting in an anchor-like final scar. In the 1970s, Regnault8,9 advocated the removal of the cutaneous excess with an incision in a "fleur-de-lis" pattern. Pitanguy10 developed the method of transverse abdominoplasty, with large detachment of the abdominal flap and plication of the rectus abdominis muscle for diastasis correction. These techniques are still in use by many surgeons. Procedures that combine the use of dermolipectomy, in which large detachments are made, are recommended for improvement of the excess skin. These procedures require two highly skilled surgeons with their associated staff, and result in large, round, and vertical scars11-13.
In 2003, we introduced a new option for abdominoplasty in post-bariatric surgery with the purpose of improving body contour and minimizing scarring and blood loss14,15. This paper describes the results of this novel abdominoplasty technique in formerly obese patients with a median abdominal scar resulting from gastroplasty.
METHODS
Abdominoplasties were performed in 100 formerly obese patients with median xyphoumbilical scars resulting from gastroplasties. All patients were operated on by the same general surgery team using the technique of Fobi-Capella. A total of 28 men and 72 women who participated in the study were operated between June 2003 and June 2008. The average age of the patients at the time of the plastic surgery procedure was 34 years. The average weight loss was 51 kg.
The weight of the patients had stabilized over 5 months with a BMI < 34. Abdominoplasty was performed after an average of 17 months after the bariatric surgery procedure.
Surgical Technique
Surgical markings were performed with the patient in an upright position. A transverse line with the umbilical scar at the center was drawn, and the horizontal cutaneous excess was estimated at this level by means of bi-digital clamping (Figure 1A). This measurement ranged, on average, from 20 to 30 cm. The distance between the umbilical scar and the origin of the vertical scar from the previous laparotomy, which was close to the xiphoid appendix, was noted. This segment was divided into three equal parts, each measuring about 5 cm. A transverse line was drawn between the lower and intermediate segments with the median line at the center, measuring 70% of the length of the line drawn at the level of the umbilical scar (Figure 1B).
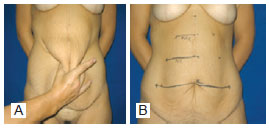
Figure 1 - A, marking of the cutaneous excess by bi-digital clamping. B, marking of the area to be resected by means of horizontal lines.
A new transverse line was drawn between the intermediate and upper segments with the median line at the center, measuring 70% of the length of the previously drawn line (for example, 1st = 20 cm, 2nd = 14 cm, 3rd = 9.8 cm).
In the natural crease of the abdomen, about 6 cm above the pubis, a line of similar length was traced to the most cranial line marked out (Figure 2A). The horizontal lines were joined at the ends and up to the median point at the origin of the vertical scar close to the xiphoid appendix, to determine the region to be removed. Two triangles between the pubic bone and the iliac fossa determined the region of additional skin removal for the correction of "dog-ears" and sagging in the pubic region (Figure 2B).
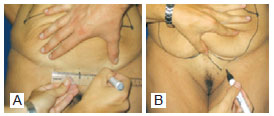
Figure 2 -A, marking of the lower line at the natural crease of the abdomen. B, marking of dog ears and rising of the pubis.
The final markings resemble the shape of a fish, giving this technique its name. The markings were confirmed with the patient in the supine position (Figure 3).
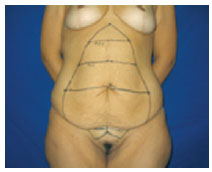
Figure 3 - Final marking: summarized scheme of the procedure.
The patients were operated on under epidural anesthesia, and received cefazolin (2 g) as antibiotic prophylaxis and low molecular weight heparin (20 mg) as thromboembolic prophylaxis, from the eve of the surgery up to the 5th postoperative day. The subcutaneous cellular tissue was infiltrated along the markings with a 1:200000 adrenaline solution and saline. The umbilical scar was isolated from the abdominal flap and maintained attached to the aponeurosis. Broken blood vessels were cauterized concomitantly to the removal of the dermal-adipose excess to minimize blood loss. The removed excess skin was weighed. Plication of the rectus abdominis muscles was performed by approximating the sides to the median line in two planes of continuous 1-0 nylon sutures. The umbilical scar was attached to the abdominal aponeurosis with separate 3-0 nylon sutures. After revision of hemostasis, reconstruction was performed with Vicryl® 2-0 sutures at the Scarpa's fascia. The pubic region was attached at the most caudal line previously drawn. Sagging of the skin in the pubic region and the need for correction of skin excess in the lower abdomen were assessed, and excess skin was removed when necessary using the previously delineated compensation triangles. Skin removal at the pubic region was prioritized to ensure that the resulting scar would be formed around it without extending laterally at the thighs or iliac fossa, leaving a final appearance of an inverted "Y". In cases of pronounced pubic lipodystrophy, liposuction was performed with a 3 mm gauge "Mercedes" type cannula. The periumbilical skin was sutured to the aponeurosis with four to six 3-0 nylon sutures to avoid umbilical traction and consequent scar enlargement. The isolated umbilical scar was sutured to the abdominal skin using 4-0 nylon sutures. Reconstruction was performed in three planes with separate 3-0 Vicryl® sutures and colorless 4-0 Vicryl subdermal and 4-0 nylon intradermal sutures in a sequence. Sterile gauze dressings and hypoallergenic tape were used at the end of the procedure. A surgical compression mesh was used for 30 days.
RESULTS
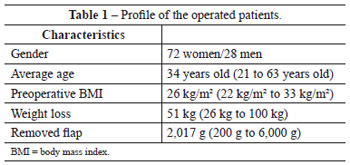
The weight of the excess dermal adipose tissue removed ranged between 200 g and 6,000 g, with an average of 2,017 g. All patients were discharged one day after surgery, with weekly follow-up for 30 days and revision 6 and 12 months after surgery (Table 1).
The complications involved scar enlargement, especially at the umbilical scar, in 9% of the patients (observed in the first cases that did not undergo fixation of the periumbilical skin to the aponeurosis), seroma in 6%, and hematoma in 1% of the cases.
All patients considered the scar to be of acceptable size and were satisfied with the overall result, and 8% of the patients expressed a desire to undergo a "retouch" to improve scar appearance.
All patients were able to carry out their daily activities 20 days after the operation.
The final result was a new body contour, a xyphopubic vertical scar, and an inverted "Y" scar at the suprapubic region.
Figures 4 to 9 show the results obtained with some patients included in the study.
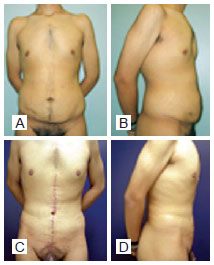
Figure 4 - A and B, preoperative images. C and D, postoperative period of 2 years; weight loss of 53 kg; flap of 22 cm x 29 cm; flap weight, 1,100 g.
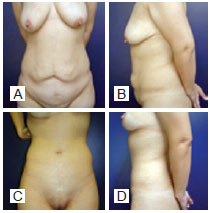
Figure 5 - A and B, preoperative images. C and D, postoperative period of 3 years; weight loss of 40 kg; flap of 33 cm x 23 cm; flap weight, 1,450 g.
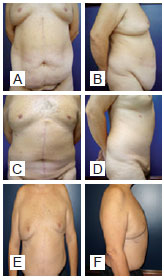
Figure 6 - A and B, preoperative images. C and D, postoperative period of 1 year. E and F, postoperative period of 5 years; weight loss of 58 kg; flap of 30 cm x 45 cm; flap weight, 4,500 g.
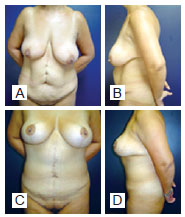
Figure 7 - A and B, preoperative images. C and D, postoperative period of 2 years; weight loss of 51 kg; flap of 33 cm x 24 cm; flap weight, 1,750 g.
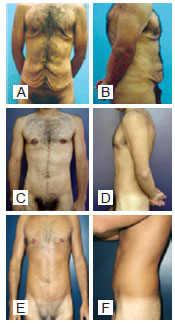
Figure 8 - A and B, preoperative images. C and D, postoperative period of 17 months. E and F, postoperative period of 6 years; weight loss of 55 kg; flap weight, 700 g.
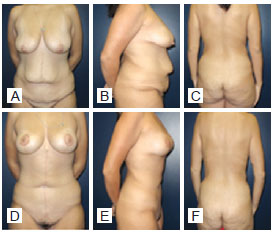
Figure 9 - A, B and C, preoperative images. D, E and F, postoperative period of 8 months; weight loss of 50 kg; flap of 20 cm x 28 cm; flap weight, 1,200 g.
DISCUSSION
The significant weight loss of patients undergoing bariatric surgery results in great distortion of body contour. Restrictions in movement and personal hygiene may result in cutaneous infections. A surgical approach is necessary to restore function and for aesthetic purposes.
The surgical approach proposed in this study is indicated in cases of vertical scars and significant sagging as a consequence of bariatric surgery. This approach has the advantage of generating smaller scars and is accompanied by reduced blood loss due to the smaller detachment compared with the techniques commonly used.
This technique showed satisfactory results, even in patients with an abdominal apron. The compensation and rise of the pubis, which results in a scar over the pubic region (instead of horizontal compensation), is questionable, but is very well accepted by patients.
The rate of complications among patients in the present study was comparable to those of other techniques reported in the medical literature16,17.
CONCLUSIONS
Abdominoplasty with markings in the shape of a fish is an option for the removal of excess abdominal skin in patients who underwent bariatric surgery.
REFERENCES
1. Capella JF, Capella FF. The weight reduction operation of choice: vertical banded gastroplasty or gastric bypass? Am J Surg. 1996;171(1):74-9.
2. Rohrich RJ. Body contouring after massive weight loss supplement. Plast Reconstr Surg. 2006;117 Suppl. 1:1S-86S.
3. Kaluf R, Júnior DF, Nascimento CL. Perfil psicológico dos pacientes submetidos à terapia cirúrgica para obesidade. In: Heck JN, Ribeiro BG, eds. Estudos vida e saúde: Universidade Católica de Goiás. Goiânia: Editora da Universidade Católica de Goiás; 2005.
4. Kaluf R, Azevêdo FN, Rodrigues LO. Sistemática cirúrgica em pacientes ex-obesos. Rev Soc Bras Cir Plást. 2006;21(3):166-74.
5. Furtado IR, Nogueira CH, Lima Júnior EM. Cirurgia plástica após gastroplastia redutora: planejamento das cirurgias e técnicas. Rev Soc Bras Cir Plást. 2004;19(2):35-40.
6. Kelly HA. Excision of the fat of the abdominal wall lipectomy. Surg Gynecol Obstet. 1910;10:229-31.
7. Castañares S, Goethel JA. Abdominal lipectomy: a modification in technique. Plast Reconstr Surg. 1967;40(4):378-83.
8. Regnault P. Abdominoplasty by the W technique. Plast Recontr Surg. 1975;55(3):265-74.
9. Regnault P. Abdominal dermolipectomies. Plast Reconstr Surg. 1975;2(3):411-29.
10. Pitanguy I. Abdominal lipectomy. Clin Plast Surg. 1975;2(3):401-10.
11. Pitanguy I. Contour surgery in the patient with great weight loss. Aesthetic Plast Surg. 2000;24(6):406-11.
12. Roxo CDP, Pinheiro O, Almeida D. Abdominoplastia multifuncional. Rev Soc Bras Cir Plást. 2004;19(3):53-74.
13. Modolin M, Cintra W Jr, Gobbi CI, Ferreira MC. Circumferential abdominoplasty for sequential treatment after morbid obesity. Obes Surg. 2003;13(1):95-100.
14. Lage RR. In: Uma nova opção de abdominoplastia pós-cirurgia bariátrica. In: XII Jornada Mineira de Cirurgia Plástica, III Simpósio de Abdominoplastia; 2003 Out 16-18; Araxá, MG, Brasil.
15. Lage RR. In: Abdominoplastia pós-cirurgia bariátrica: uma nova opção. In: XXV Jornada Paulista de Cirurgia Plástica; 2005 Jun 9-11; São Paulo, SP, Brasil.
16. Schechener SA, Jacobs JS, O'Loughlin KC. Plastic and reconstructive body contouring in the pos-vertical banded gastroplasty patient: a retrospective review. Obes Surg. 1991;1(4):413-7.
17. Costa LF, Manta AM, França AS, Cavalcante HA, Nahon M. Abdominoplastia vertical modificada em pacientes ex-obesos. Rev Soc Bras Cir Plást. 2003;18(3):67-74.
1. Full member of the Brazilian Society of Plastic Surgery (SBCP), specialist member of the Brazilian Association of Cranio-Maxillofacial Surgery (ABCCMF), medical coordinator of the Center for Treatment and Rehabilitation of Cleft Lip and Palate and Craniofacial Deformities (CENTRARE), plastic surgeon, head and coordinator of the Plastic Surgery Service of Hospital da Baleia, Belo Horizonte, MG, Brazil.
2. Full member of SBCP, plastic surgeon at Hospital Mater Dei, Belo Horizonte, MG, Brazil.
3. Specialist member of SBCP, plastic surgeon at Hospital das Clínicas of Universidade Federal de Minas Gerais, Belo Horizonte, MG, Brazil.
4. Specialist member of SBCP, specialist member of ABCCMF, plastic surgeon at Hospital Santa Genoveva, Uberlândia, MG, Brazil.
5. Specialist member of SBCP, plastic surgeon at Hospital da Baleia, Belo Horizonte, MG, Brazil.
Correspondence to:
Renato Rocha Lage
Rua Domingos Vieira, 319 - sala 701 - Santa Efigênia
Belo Horizonte, MG, Brazil - CEP 30150-240
E-mail: renatorochalage@hotmail.com
Submitted to SGP (Sistema de Gestão de Publicações/Manager Publications System) of RBCP (Revista Brasileira de Cirurgia Plástica/Brazilian Journal of Plastic Surgery).
Paper received July 01, 2011
Paper accepted: October 31, 2011
Study conducted at Clínica Vitória, Belo Horizonte, MG, Brazil.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter