

Case Report - Year 2026 - Volume 41Issue 1
Case Report: Use of Dermal Matrix after Forehead Skin Avulsion in a Public Healthcare System Patient
Relato de caso: uso de matriz dérmica após avulsão de pele da fronte em paciente da saúde pública
ABSTRACT
Introduction Acellular dermal matrix (ADM) is a high-cost material for dermis replacement. It allows the regeneration of the remaining tissue, with minimal risk of immunological rejection. The present study reports a case of ADM use to treat a skin avulsion affecting the forehead, eyebrow, and upper eyelid at a plastic surgery service from the Brazilian Unified Health System.
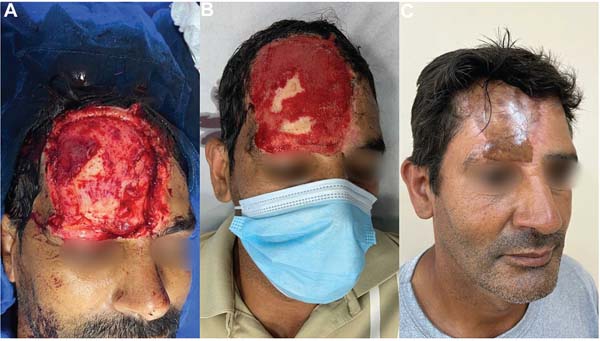
Case Report A 47-year-old male patient suffered a traffic accident and presented loss of substance in the right frontal region, with total avulsion of the skin from the scalp to the right eyebrow, with bone exposure but no fractures. We opted for hemostasis and dressing changes every 3 days. We placed ADM with a tie-over dressing on the wound 15 days after the trauma, when it presented granulation tissue. The patient progressed well and returned 1 month later for ADM removal and partial skin graft. After 2 days, the patient suffered a fall from his own height that resulted in the detachment of the lower third of the graft. Then, we performed a total skin graft from the right supraorbital region. After 11 months of this procedure, the ADM graft led to an excellent reconstructive outcome.
Discussion The use of ADM enabled the appropriate maintenance of facial functionality without retraction. Postoperative care also influenced procedural success. The patient's fall from his own height compromised part of the skin graft, but the reapproach ensured complete wound closure with no further complications.
Conclusion The benefits of ADM use outweigh its financial limitations.
Keywords: acellular dermis; allografts; plastic surgery; plastic surgery procedures; Unified Health System
RESUMO
Introdução A matriz dérmica acelular (MDA) é um material de alto custo que substitui a derme, permitindo a regeneração do tecido remanescente, com mínimo risco de rejeição imunológica. O presente trabalho relata um caso de uso de MDA em avulsão de pele da fronte, sobrancelha e pálpebra superior em um serviço de cirurgia plástica do SUS.
Relato de Caso Um paciente do sexo masculino, com 47 anos de idade, sofreu um acidente envolvendo uma colisão entre automóveis e apresentou perda de substância na região frontal direita, com avulsão total da pele do couro cabeludo até o supercílio direito, com exposição óssea, sem fraturas. Optou-se por hemostasia e troca de curativos a cada 3 dias. A MDA com curativo compressivo de Brown foi colocada sobre a ferida após 15 dias do trauma, que apresentava formação de tecido de granulação. O paciente evoluiu bem e retornou 1 mês depois para retirada da MDA e enxertia parcial de pele. Após 2 dias, o paciente sofreu uma queda da própria altura que resultou no descolamento de terço inferior do enxerto. Emseguida, realizamos um enxerto de pele total da região supraorbital direita. Após 11meses deste procedimento, o enxerto com MDA levou a um ótimo resultado reconstrutivo.
Discussão A utilização da MDA permitiu a manutenção apropriada da funcionalidade da face sem retrações. Os cuidados pós-operatórios também impactaram no sucesso do procedimento. A queda de mesmo nível do paciente comprometeu parte do enxerto de pele, mas a reabordagem assegurou o fechamento completo da ferida sem complicações posteriores.
Conclusão Os benefícios da MDA se sobrepõem às limitações financeiras do uso do material.
Palavras-chave: aloenxertos; cirurgia plástica; derme acelular; procedimentos em cirurgia plástica; Sistema Único de Saúde
Introduction
Advances in reconstructive plastic surgery techniques have allowed numerous patients to survive extensive skin loss, such as that resulting from burns and trauma.1-3 The higher survival rate led to a proportional increase in patients presenting with unsatisfactory outcomes, including esthetic and functional sequelae.1 The use of dermal matrices has become increasingly common to improve the outcomes from this type of reconstruction.
Acellular dermal matrices (ADMs) are biotechnology products that replace the dermis, the deepest layer of the skin,1 allowing for the regeneration of remaining tissue, its revascularization, and providing support to the region. They are tissues composed of a substance similar to the dermis, with processed skin, or manufactured with dermal collagen matrix and other matrix proteins.3 As it is acellular, the risk of immunological rejection is virtually nil.
Dermal matrices can consist of only collagen and glyco-saminoglycans (GAGs), mimicking the dermis, or of a colla-gen layer and a second layer formed by a silicone sheet mimicking the temporary epidermis,4 as is the case with the ADM used in the present study. Fabrication of the dermal matrix can use porcine collagen membranes (derived from the jejunal submucosa or dermal collagen and elastin), bovine dermal matrices (composed of extracellular proteins and collagen), ovine dermal matrices, and human dermal matrices derived from cadaver skin. The latter, however, is not approved by the Brazilian National Health Regulatory Agency (ANVISA, from the Portuguese Agência Nacional de Vigilância Sanitária) for use in the country.3 The selection of a skin substitute relies on wound type, size, and depth, any comorbidities present, the patient’s preferences, and the surgeon’s experience.3
In the healing process, the dermis undergoes gradual replacement by the patient’s fibroblasts, which infiltrate the matrix to produce collagen. Neovascularization of the dermis occurs, and the silicone layer (present in some dermal matrices) prevents fluid loss and blocks bacterial proliferation. After the integration of the neodermis, which takes, on average, 3 weeks, a thin, partial-thickness skin graft replaces this silicone layer and integrates favorably with the dermal bed.2 However, studies show that vacuum therapy on the matrix decreases the integration time from 3 weeks to just 10 to 15 days. This reduction occurs because the combination helps keep the matrix immobilized, prevents wound infections, and minimizes fluid accumulation in the matrix bed.5
Full-thickness skin loss can complicate lesions and impair healing, increasing the recovery time in the absence of proper treatment.6,7 The use of dermal matrices also reduces fibrotic scars, minimizing scar retraction and facilitating movement.1 In addition, they provide better skin coverage with lower donor site morbidity.6
Despite its benefits, the Brazilian Unified Health System (SUS, from the Portuguese Sistema Único de Saúde) does not cover treatment with dermal substitutes in most hospitals. Burn treatment centers can use dermal matrices for burn sequelae under SUS coverage. Therefore, in the public health-care system, treatment with dermal substitutes occurs when SUS provides these materials, companies donate them, or they are included in research protocols from reference services.
The present study reports a case treated with a dermal matrix in a patient with skin avulsion affecting the forehead, eyebrow, and upper eyelid, treated at a Plastic Surgery Service of SUS. The Research Ethics Committee of Complexo Hospitalar do Trabalhador approved this study under proto-col number 80029624.8.0000.5225.
Case report
A 47-year-old male patient arrived at the emergency room (ER) after a car collision. The tissue loss resulting from the right frontal region injury measured approximately 11.4 x 9.7 cm, with total skin avulsion from the scalp up to the right eyebrow, with bone exposure, but no visible frac-tures or crepitus on palpation. Hemostasis and dressing were applied to the wound. After discharge from the ER, the patient returned for outpatient follow-up every 3 days to change the petroleum jelly dressings. Fifteen days after the trauma, the lesion had progressed with the formation of well-formed granulation tissue, and the patient underwent surgical regularization and meticulous hemostasis.
Next, we placed an ADM using continuous suture with 5.0 nylon thread and tie-over compression dressings. The ADM used, Nevelia By-layer Matrix (SYMATESE), consisted of a silicone layer and a purified, stabilized type-1 bovine colla-gen layer. A sales representative donated the ADM, resulting in no financial costs for the patient or the Plastic Surgery Service.
The patient progressed well and without complaints. He returned to the service one month later, when we removed the silicone sheet covering the matrix and performed a partial skin graft below the well-integrated ADM using tissue from the right thigh. We applied a cellulose acetate mesh dressing to the donor area and a tie-over dressing over the recipient area.
Two days later, the patient returned to the outpatient clinic due to a fall from his own height resulting from a seizure, presenting detachment of the lower third of the graft. The non-detached matrix remained in the correct position. Due to graft loss near the eyelid and to prevent eyelid retraction, we performed a full-thickness skin graft at the right supraorbital region, using the right inguinal area as the donor site.
Results
Eleven months after the last procedure, the ADM graft led to an adequate reconstructive outcome, with no major scar retraction (►Fig. 1).
Discussion
Local or pedicled flaps are the first-line treatment for wounds with inadequate beds and cranial vault exposure with no periosteum involvement.7 Esthetically and function-ally, the morbidity of donor sites for cutaneous, muscular, and myocutaneous flaps is typically higher compared with donor sites for partial-thickness skin grafts. However, since the patient presented with a large area of tissue loss, free or microsurgical flaps would be considerably thicker and po-tentially have a different color from the surrounding skin of the recipient area, a crucial factor for a satisfactory esthetic outcome.4,8
One of the most popular free flaps for scalp reconstruction is the anterolateral thigh flap. However, as our patient had a thick layer of adipose tissue in this region, the tissue in the recipient area would be too large. We also considered microsurgical reconstruction and thinner flaps, such as the inguinal and Chinese (radial forearm) flaps, but they would increase the hospital stay and recovery time. The first option for scalp avulsion would be replantation, but we did not consider it due to the tissue loss at the scene of the trauma. Local scalp flaps would also allow for the reconstruction of the lost hair area. After discussing these options with the patient, we selected a less invasive surgery.8
In autologous grafting approaches, vacuum-assisted clo-sure (VAC) can accelerate tissue granulation. However, ap-plying negative pressure therapy to bone with little periosteal area does not result in adequate granulation. Furthermore, since the lesion area was too close to the eyeball, achieving a proper hermetic seal would require covering the patient’s eyeball with transparent film or using strategies such as hydrocolloid pastes, which would cause greater discomfort. We ruled out VAC due to the rapid development of granulation in this patient, as it would require a longer hospital stay.5
The combination of dermal matrices and skin grafts can provide excellent results in the reconstruction of complex wounds with exposure of the cranial vault. In this case, the main advantage of the ADM application would be its sim-plicity as a procedure, which can be performed in secondary centers where more complex reconstructions are not avail-able.7,9 In the case presented, the choice of the combined therapeutic plan (ADM and partial skin graft) is consistent with the literature, given the limitation of adjacent tissue for skin coverage via local flaps and the good wound evolution, with adequate granulation tissue growth for grafting after 2 weeks. We waited for the development of a granular wound because ADM requires a well-vascularized bed for host cell infiltration, such as fibroblasts and keratinocytes, which increases the chances of proper matrix integration.4,6 In this scenario, we decided to associate ADM with partial-thickness skin grafting to avoid dermal retractions or path-ological scars, allowing the proper functional maintenance of a sensitive area such as the face.6
Considering that the decrease in the total dermal thick-ness tends to transform wounds into difficult-to-heal chronic lesions, prolonging the recovery time if their management is not correct, and that some disorders or specific conditions cause partial or complete compromise of the anatomical structures of the skin,4 the use of ADM has proven to be an alternative for a safer and more effective treatment.
Nevertheless, the challenges of this technique include the high costs of the materials, the need for professionals trained in their proper use, and the prolonged time for integration. These aspects increase the financial burden on the healthcare system. Moreover, the technique requires additional surgery when compared with flaps.3,9
The accidental fall sustained by the patient caused partial graft detachment and significant hyperpigmentation of the affected area, resulting in a more apparent color discrepancy than any donor flap area would have pre-sented. This occurrence highlights the direct impact of postoperative care on procedural success. Although the fall compromised part of the skin graft, the reintervention ensured complete wound closure with no further compli-cations. The long-term functional and esthetic outcome was satisfactory.
Further research is needed to develop a less expensive ADM and make it an economical and applicable choice in the Brazilian context, as this is the key challenge to implement-ing this technique. As reports and case series on ADM in facial wound reconstruction remain scarce, more studies are re-quired, especially in reconstructive plastic surgery.
Conclusion
We described the surgical technique for ADM use and postoperative care. Although this material still presents financial limitations, the benefits of using biotechnology in reconstructive plastic surgery outweigh the disadvantages.
REFERENCES
1. Stella R. Matriz dérmica regenera com melhor qualidade lesão por queimadura. Jornal da USP; 2017. Disponível em: https://jornal.usp.br/?p=69000
2. Aldunate JLCB, Milcheski DA, Chang AA, Nakamoto HA, Tuma P Junior, Ferreira MC. Utilização de matriz dérmica associada à terapia a vácuo e enxertia de pele em queimaduras profundas. experiência inicial. Rev Bras Queimaduras 2013;12(02):83-86
3. Ferreira MC, Paggiaro AO, Isaac C, Teixeira Neto N, Santos GBd. Substitutos cutâneos: conceitos atuais e proposta de classificação. Rev Bras Cir Plást 2011;26(04):696-702. Doi: 10.1590/S1983-51752011000400028
4. Cruz LGB. Uso de matriz dérmica acelular heteróloga em cirurgia plástica reparadora. Rev Bras Cir Plást 2016;31(01):88-94. Doi: 10.5935/2177-1235.2016RBCP0013
5. Jeschke MG, Rose C, Angele P, Füchtmeier B, Nerlich MN, Bolder U. Development of new reconstructive techniques: use of Integra in combination with fibrin glue and negative-pressure therapy for reconstruction of acute and chronic wounds. Plast Reconstr Surg 2004;113(02):525-530. Doi: 10.1097/01.PRS.0000100813.39746.5A
6. Gierek M, Łabuś W, Kitala D, et al. Human Acellular Dermal Matrix in Reconstructive Surgery-A Review. Biomedicines 2022;10(11): 2870. Doi: 10.3390/biomedicines10112870
7. Desai SC, Sand JP, Sharon JD, Branham G, Nussenbaum B. Scalp reconstruction: an algorithmic approach and systematic review. JAMA Facial Plast Surg 2015;17(01):56-66. Doi: 10.1001/jamafa-cial.2014.889
8. Innocenti A, Menichini G, Innocenti M. Six-years experience in major scalp defect reconstruction with free flap: analysis of the results. Acta Biomed 2022;92(06):e2021301. Doi: 10.23750/abm.v92i6.10089
9. Milcheski DA, Lobato RC, Jesus MNdSd, Mota WM, Chi A, Gemperli R. Lesão complexa e auto-infligida de couro cabeludo secundária a delírio de infestação parasitária tratada com matriz dérmica e enxertia. Disponível em: https://cdn.publisher.gn1.link/relatos-docbc.org.br/pdf/n8a18.pdf
1. Faculdade Evangélica Mackenzie do Paraná, Curitiba, PR, Brazil
2. Faculdades Pequeno Príncipe, Curitiba, PR, Brazil
3. Universidade Positivo, Curitiba, PR, Brazil
4. Plastic Surgery Service, Complexo Hospitalar do Trabalhador, Curitiba, PR, Brazil
Address for correspondence Anna Heloisa Tavares, Rua Bruno Filgueira, 369 - sala 1402 - Batel, Curitiba - PR, 80010-010, Brazil (e-mail: annahelotavares@gmail.com).
Article received: October 23, 2024.
Article accepted: October 13, 2025.
Editor-in-Chief: Dov Charles Goldenberg.
Conflict of Interests
The authors have no conflict of interests to declare.



 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter