

Original Article - Year 2026 - Volume 41Issue 1
Subcutaneous Gluteal Fat Grafting: The Role of Intraoperative Ultrasound in the Safe Determination of the Plane
Lipoenxertia glútea subcutânea: O papel do ultrassom intraoperatório na determinação segura do plano
ABSTRACT
Introduction Materials and
Methods From April 2022 to December 2024, 148 female patients who underwent ultrasound-guided gluteal fat grafting were analyzed. The patients with gluteal implants, a history of filler injections, or vascular diseases were excluded. The data collected included age, grafted volume, and complications. The procedure followed the static injection, migration, and equalization (SIME) methodology, enabling real-time visualization of anatomical structures to ensure safe fat deposition above the muscular fascia.
Results The mean age of the patients was of 33.7 (range: 23-45) years, and the mean fat volume grafted per buttock was of 350 (range: 300-600) mL. No patients experienced severe complications, such as fat or pulmonary embolism. There were two cases of wound dehiscence, three cases requiring additional grafting for symmetry, two cases of seroma, and two cases of fat necrosis.
Conclusion Ultrasound-guided fat grafting using the SIME method proved to be a safe and effective technique, significantly reducing the risk of severe complications. The ultrasound provides enhanced control over fat deposition, improving the predictability and safety of the procedure.
Keywords: buttocks; lipectomy; safety; surgery; plastic; ultrasonography
RESUMO
Introdução A lipoenxertia glútea é amplamente utilizada para a remodelação corporal, impulsionada por padrões estéticos e pelas redes sociais. No entanto, complicações como embolia gordurosa têm sido relatadas, especialmente nos Estados Unidos. Para aumentar a segurança do procedimento, desenvolveu-se a técnica guiada por ultrassonografia, que permite a deposição precisa da gordura na região subcutânea profunda sem alcançar a camada muscular, o que reduz os riscos.
Materiais e Métodos Entre abril de 2022 e dezembro de 2024, foram analisadas 148 pacientes submetidas à lipoenxertia glútea guiada por ultrassom. Pacientes com prótese glútea, histórico de aplicação de substâncias preenchedoras e doenças vasculares foram excluídas. Os dados coletados incluíram idade, volume enxertado e complicações. A técnica seguiu a metodologia de injeção estática, migração e estabilização (static injection, migration, and stabilization, SIME, em inglês), que permite a visualização em tempo real das estruturas anatômicas para garantir a deposição segura da gordura acima da fáscia muscular.
Resultados A idade média das pacientes foi de 33,7 (variação: 23-45) anos, com enxertia média de 350 (variação: 300-600) mL por nádega. Nenhuma paciente apresentou embolia gordurosa ou pulmonar. Foram registrados dois casos de deiscência de pontos, três de enxertia adicional para simetrização, dois de seroma e dois de necrose gordurosa.
Conclusão A técnica de lipoenxertia guiada por ultrassonografia que utiliza o método SIME demonstrou-se segura e eficaz, pois reduziu significativamente o risco de complicações graves. O uso do ultrassom permite maior controle da deposição da gordura, o que aumenta a previsibilidade e segurança do procedimento.
Palavras-chave: cirurgia plástica; lipectomia; nádegas; segurança; ultrassonografia
Introduction
Gluteal fat grafting is a widely-publicized and -practiced technique today, especially in Western culture. Volumization of the buttocks is associated with concepts of beauty and femininity, reflecting historical patterns that consider this area a symbol of fertility. Throughout history, larger buttocks have referred to the idea of a fertile woman, contributing to the popularity of procedures that increase the volume in this area.1
The harmony between waist and hips confers an attractive erotic capital for the female population, and the proportional size of these regions has a ratio closer to 0.7. Many Latin American women desire this standard.2
In recent years, the beauty ideal driven by social media has generated a significant increase in esthetic procedures targeting the gluteal region.3-5 According to data from the International Society of Aesthetic Plastic Surgery (ISAPS),4 the popularity of this procedure increased by 137% from 2018 to 2022. Gluteal lipofilling plays a significant role in body contouring surgery, and studies, such as those by Cansancao et al.6 and Pazmiño and Del Vecchio,7 demonstrate the use of ultrasound for proper fat positioning during the procedure.
However, the increased practice of fat grafting also raises concerns about fat embolism, a severe, life-threatening complication reported in studies conducted in the United States of America (USA).8,9
Given such a scenario, the present study aimed to describe the lipofilling technique in the deep subcutaneous region, using ultrasound to enhance the precision of the grafting plane and, consequently, the safety of the procedure.
Materials and Methods
The current study is a prospective, observational case series. Female patients who underwent gluteal fat grafting after liposuction from April 2022 to December 2024 were selected. Subjects with gluteal implants, a history of substance application in the gluteal region (such as polymethylmethacrylate), or those with vascular diseases and procoagulant syndromes were excluded from the study. The initial sample size calculation resulted in 140 patients for a 95%CI.
The collected data included gender, age, graft volume, and complications, which were expressed in terms of mean and range values, as well as absolute and relative frequencies. The data were tabulated in the Excel (Microsoft Corp.) software and analyzed using the IBM SPSS Statistics for Windows (IBM Corp.) software, version 23.0. The study was approved by an ethics committee via Plataforma Brasil, under CAAE 89713625.3.0000.0237.
Regional anatomy
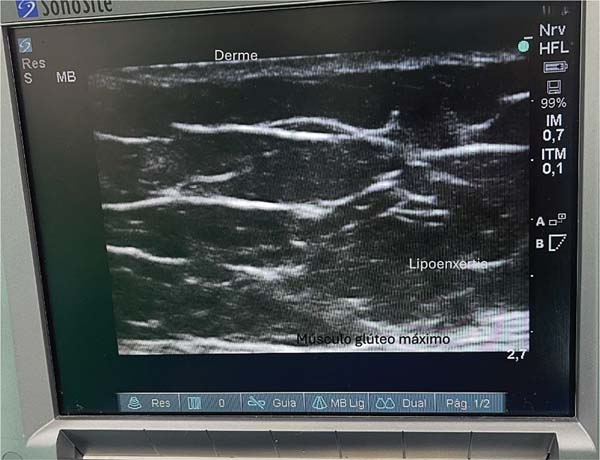
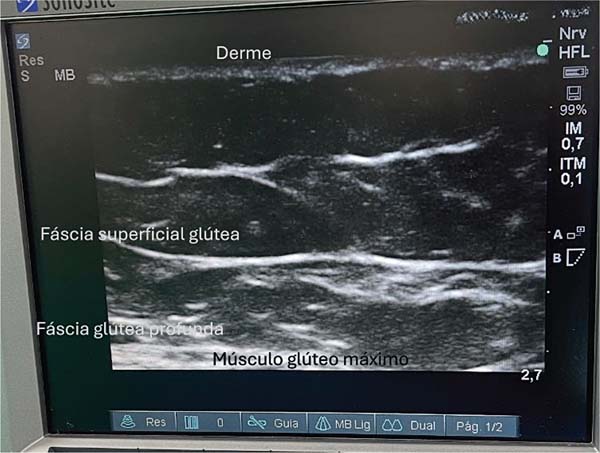
Classically, this region features two fascial layers and two fatcontaining subcutaneous tissue layers. The ultrasound evaluation reveals a thinner, more elastic fascial layer, as well as a thicker one. The thinner fascia divides the subcutaneous tissue into two layers, and fat deposition occurs in the space between them (►Fig. 1).
Description of the technique
After liposuction, the fat is collected in a sealed container and prepared by decantation until the procedure is complete.
With the patient in the prone position, a portable ultrasound equipped with a linear probe and at a 10-Hz frequency examines the superficial layers for subcutaneous tissue identification.9
The anatomical structures of the gluteal region are visualized on a tenth-generation iPad (Apple Inc.) using Wi-Fi ultrasound. This examination enables the identification of the following layers: skin, dermis, superficial fat, superficial gluteal fascia (or Scarpa’s fascia), deep fat, and deep gluteal fascia. The latter lies just above the muscle, and it should be avoided at all costs. Ideally, fat grafting occurs in the deep fat layer. Preservation of the deep gluteal fascia, combined with incisions shorter than 1 cm, prevents fat migration into the muscle plane.9,10
The procedure follows the technique described by Pazmiño and Del Vecchio,7 which involves static injection, migration, and equalization (SIME), under direct visualization with a number-3 lipofilling cannula. With the left hand, the surgeon manipulates the ultrasound probe to view the grafting area, while the right hand injects the fat into the deep layer with a syringe (►Fig. 2). Alternatively, an assistant can hold the probe while the surgeon performs the fat injection.
Results
A total of 148 female patients who underwent ultrasoundguided gluteal lipofilling were analyzed. Their mean age was of 33.7 (range: 23-45) years.
The patients received a mean of 350 (range: 300-600) mL of fat grafted into each buttock (►Table 1). None of the patients presented complications such as hematoma, necrosis, or infection. However, two subjects presented suture dehiscence in the intergluteal region, and three required additional grafting for symmetrization. Moreover, there were two cases of seroma and two of fat necrosis. No patient had fat embolism or pulmonary embolism.
| Mean | Range | |
|---|---|---|
| Age (years) | 33.7 | 23-45 |
| Grafted volume per area (mL) | 350 | 300-600 |
| Complications | N (absolute frequency) | % (relative frequency) |
| Suture dehiscence | 2 | 1.35 |
| Asymmetry | 3 | 2.02 |
| Seroma | 2 | 1.35 |
| Fat necrosis | 2 | 1.35 |
Discussion
Mortality in plastic surgery is an extremely-relevant topic, as it impacts the patients’ families as well as the surgeons and their teams, regardless of the causes involved. The publication of studies on fat embolism-related mortality increased from 2015 onwards; Astarita et al.,11 for example, described a case that had occurred in California, USA. Subsequently, Cárdenas-Camarena et al.12 published one of the most comprehensive forensic studies on the subject, analyzing cases in Mexico and Colombia and identifying the presence of fat in the pulmonary vessels as a key finding.
In recent years, due to the increased mortality in Florida, USA, several studies have been conducted to investigate the causes of deaths and provide relevant information for surgeons and patients interested in this lipofilling.8,13 The investigations have highlighted the importance of performing fat grafting in the gluteal region above the muscle fascia, that is, exclusively in the subcutaneous area, to avoid fat embolism resulting from fat entering the gluteal vessels.
The Aesthetic Surgery Education and Research Foundation (ASERF) Task Force on Gluteal Fat Grafting8 made several recommendations, including avoiding intramuscular fat grafting, using injection cannulas with a diameter greater than 4 mm, avoiding the downward angulation of the cannula, and positioning the patient to minimize the risk of deep injection. However, these guidelines proved insufficient to completely prevent fat embolism, especially after the episodes that occurred in Miami, which spurred the search for safer and more effective approaches. In this context, Cansancao et al.6 and Pazmiño and Del Vecchio,7 described techniques aimed at improving the safety of the procedure by using intraoperative ultrasound to ensure that the grafted fat will remain in the subcutaneous plane.
The current study is based on ultrasound use following the SIME methodology,7 which enables direct observation of ultrasound-guided lipofilling. This method precisely identifies the anatomical divisions and compartments of the gluteal region and requires detailed knowledge of local anatomy. It ensures fat graft deposition exclusively in the subcutaneous plane, above the muscle fascia. This direct visualization14 provides a superior level of safety, as the fat graft’s positioning is monitored in real time, avoiding blind application.
When describing fat grafting, Carpaneda and Ribeiro15 highlighted that cylindrical grafts of up to 2 mm in diameter reduce reabsorption rates. In contrast, in the technique introduced by Pazmiño and Del Vecchio,16 fat is retroinjected in higher volumes, exceeding the recommended thickness, enabling the application of large amounts with reasonable absorption rates without compromising the graft viability. Apparently, with this approach, the grafted tissue survives even when applied as a bolus in the subcutaneous tissue.
Studies on fat embolism prevention7,8,16,17 guide surgeons on how to avoid the infusion of fat into venous capillaries, which could lead to pulmonary vessel obstruction and respiratory compromise. Medical societies should focus on safety in lipofilling, ensuring fat deposition in the appropriate plane using direct ultrasound visualization, and training medical teams to recognize signs of fat embolism syndrome. It is important to emphasize that, specifically in liposuction and lipofilling, this complication occurs during the intraoperative period, but it may arise days after a bone fracture.
Conclusion
The SIME technique of ultrasound-guided lipofilling is a safe and effective approach for gluteal lipofilling in the deep subcutaneous region, as it enables direct real-time observation. This method, described as significantly reducing the risk of fat embolism, can provide greater predictability and safety for plastic surgeons and their patients. Multicenter studies are required to establish this technique as a gold standard in gluteal lipofilling.
References
1. De la Peña JA, Rubio OV, Cano JP, Cedillo MC, Garcés MT. History of gluteal augmentation. Clin Plast Surg 2006;33(03):307-319. Doi: 10.1016/j.cps.2006.04.003
2. Singh D. Universal allure of the hourglass figure: an evolutionary theory of female physical attractiveness. Clin Plast Surg 2006;33 (03):359-370. Doi: 10.1016/j.cps.2006.05.007
3. Vendramin FS, Soares DAdS, Dias MDS, Costa LDd. Gluteoplastia com enxerto de gordura: experiência em 137 pacientes. Rev Bras Cir Plást 2022;37(02):169-176. Doi: 10.5935/2177-1235.2022RBCP0028
4. International Society of Aesthetic Plastic Surgery (ISAPS) ISAPS International Survey on Aesthetic/Cosmetic Procedures. Amsterdam: ISAPS; 2023. Available from: https://www.isaps.org/media/a0qfm4h3/isaps-global-survey_2022.pdf
5. American Society of Plastic Surgeons (ASPS) 2018. Plastic Surgery Statistics Report. Arlington Heights, IL: ASPS; 2019. Available from:https://www.plasticsurgery.org/documents/News/Statistics/2018/plastic-surgery-statistics-full-report-2018.pdf
6. Cansancao AL, Condé-Green A, David JA, Vidigal RA. Subcutaneous-Only Gluteal Fat Grafting: A Prospective Study of the Long- Term Results with Ultrasound Analysis. Plast Reconstr Surg 2019; 143(02):447-451. Doi: 10.1097/prs.0000000000005203
7. Pazmiño P, Del Vecchio D. Static Injection, Migration, and Equalization (SIME): A New Paradigm for Safe Ultrasound-Guided Brazilian Butt Lift: Safer, Faster, Better. Aesthet Surg J 2023;43 (11):1295-1306. Doi: 10.1093/asj/sjad142
8. Mofid MM, Teitelbaum S, Suissa D, et al. Report on Mortality from Gluteal Fat Grafting: Recommendations from the ASERF Task Force. Aesthet Surg J 2017;37(07):796-806. Doi: 10.1093/asj/sjx004
9. Kenkel JM, Polo M, Pazmiño P, Garcia O. Brazilian Butt Lift Safety and Florida Legislature: What You Should Know, How You Can Help. Aesthet Surg J Open Forum 2023;5:ojad041. Doi: 10.1093/ asjof/ojad041
10. Frojo G, Halani SH, Pessa JE, et al. Deep Subcutaneous Gluteal Fat Compartments: Anatomy and Clinical Implications. Aesthet Surg J 2023;43(01):76-83. Doi: 10.1093/asj/sjac230
11. Astarita DC, Scheinin LA, Sathyavagiswaran L. Fat transfer and fatal macroembolization. J ForensicSci2015;60(02):509-510. Doi: 10.1111/1556-4029.12549
12. Cárdenas-Camarena L, Bayter JE, Aguirre-Serrano H, Cuenca- Pardo J. Deaths Caused by Gluteal Lipoinjection: What Are We Doing Wrong? Plast Reconstr Surg 2015;136(01):58-66. Doi: 10.1097/PRS.0000000000001364
13. Rapkiewicz AV, Kenerson K, Hutchins KD, Garavan F, Lew EO, Shuman MJ. Fatal Complications of Aesthetic Techniques: The Gluteal Region. J Forensic Sci 2018;63(05):1406-1412. Doi: 10.1111/1556-4029.13761
14. Kelishadi SS, Chiemi JA, Chowdhry S, et al. Accurate Plane Fat Grafting in Gluteal Augmentation: An Anatomic Study. Aesthet Surg J 2024;44(03):311-316. Doi: 10.1093/asj/sjad298
15. Carpaneda CA, Ribeiro MT. Percentage of graft viability versus injected volume in adipose autotransplants. Aesthetic Plast Surg 1994;18(01):17-19. Doi: 10.1007/BF00444242
16. Pazmiño P, Del Vecchio D. Safety in Gluteal Augmentation. Clin Plast Surg 2023;50(04):521-523. Doi: 10.1016/j.cps.2023.07.001
17. Freitas RS, Graf R, Ono MCC, et al. Profilaxia da síndrome de embolia gordurosa: uma análise atual. Rev Bras Cir Plást 2016;31 (03):436-441. Doi: 10.5935/2177-1235.2016RBCP0072
1. Instituto de Cirurgia Plástica Arruda, Hospital Santa Helena, Goiânia, GO, Brazil
Address for correspondence Fabiano Calixto Fortes de Arruda, Instituto de Cirurgia Plástica Arruda, Hospital Santa Helena, Goiânia, GO, Brazil (e-mail: dr.fabianoarruda@gmail.com).
Artigo submetido: 13/10/2024.
Artigo aceito: 13/10/2025.
Conflict of interests
The author has no conflict of interests to declare.




 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter