

Review Article - Year 2022 - Volume 37 -
Breast Implant Illness: where are we and where are we going?
Breast Implant Illness: onde estamos e para onde vamos?
ABSTRACT
Despite more than 60 years of history, numerous studies and large population samples, in recent years, several patients have returned to the plastic surgeons office. They have doubts about the silicone, some due to the recent reports of BIAALCL, but the vast majority due to the possibility of systemic symptoms related to the implants and which arouse the desire for its removal. Procedure known as explant. This phenomenon, whose doubts are numerous and the responses are minimal, is known in the world literature as Breast Implant Illness (BII). On the Internet and social networks, hundreds of signs and symptoms have been related to silicone implants, usually nonspecific. The most common symptoms reported by patients are chronic fatigue, arthralgia, mental confusion, myalgia, memory loss, difficulty concentrating and dry eyes. So far, there are no diagnostic tests for BII, no method based on scientific evidence to differentiate it from other conditions, and there is very little knowledge about its onset, course, risk factors, causes and proper management. The option for removing the implants has been growing dramatically in recent years, being one of the ten most performed surgeries in the United States last year. The literature shows variable improvement rates after the explantation and the patients are, as a rule, satisfied with their aesthetic result and have lower levels of anxiety and stress after the procedure. Prospective, well-designed randomized studies correlating different periods are necessary, from the preoperative period of the implant until after the explantation.
Keywords: Breast implantation; Mammaplasty; Silicone elastomers; Breast diseases; Reconstructive surgical procedures; Breast.
RESUMO
Apesar dos mais de 60 anos de história, dezenas de estudos e grandes amostras populacionais, nos últimos anos diversos pacientes têm retornado ao consultório do cirurgião plástico. Apresentam dúvidas a respeito do silicone, algumas devido aos relatos recentes de BIA-ALCL (Anaplastic Large Cell Lymphoma), mas a grande maioria pela possibilidade de sintomas sistêmicos relacionados aos implantes e que despertam o desejo da sua remoção. Procedimento conhecido como explante. Este fenômeno, cujas dúvidas são inúmeras e as respostas mínimas, é conhecido na literatura mundial como Breast Implant Illness (BII). Na Internet e redes sociais, centenas de sinais e sintomas têm sido relacionados às próteses de silicone, usualmente inespecíficos. Os sintomas mais comuns referidos pelas pacientes são fadiga crônica, artralgia, confusão mental, mialgia, perda de memória, dificuldade de concentração e olhos secos. Até o momento, não existem testes diagnósticos para BII, nenhum método baseado em evidência científica para diferenciá-la de outras condições e há muito pouco conhecimento a respeito do seu início, curso, fatores de risco, causas e manejo adequado. A opção pela retirada dos implantes vem crescendo vertiginosamente nos últimos anos, sendo uma das dez cirurgias mais realizadas nos Estados Unidos no ano passado. A literatura mostra taxas de melhora dos sintomas variáveis após o explante e as pacientes mostram-se, via de regra, satisfeitas com seu resultado estético e apresentam níveis de ansiedade e estresse menores após o procedimento. São necessários estudos prospectivos, randomizados bem desenhados correlacionando períodos distintos das pacientes, desde o pré-operatório do implante até o pós-explante.
Palavras-chave: Implante mamário; Mamoplastia; Elastômeros de silicone; Doenças mamárias; Procedimentos cirúrgicos reconstrutivos; Mama
INTRODUCTION
Silicone implants have been available on the world market since the mid-1960s, and, since then, many studies, questions and uncertainties have been in the air, from the silicone moratorium in the United States to the bankruptcy of Dow Corning and the worldwide scandal of PIP. Despite obstacles over the years, in 2019 alone, approximately 280,000 surgeries were performed with breast implants in the United States, totaling approximately 50 million women with silicone implants worldwide1,2.
Despite more than 60 years of history, dozens of studies, and large population samples, many patients have returned to the plastic surgeon’s office recently. They have doubts about silicone, some due to recent reports of BIA-ALCL (Anaplastic Large Cell Lymphoma), but the vast majority due to the possibility of systemic symptoms related to implants that arouse the desire to remove them. The procedure is known as explant. This phenomenon, whose doubts are numerous and the answers are minimal, is known in the world literature as Breast Implant Illness (BII)1,3,4.
ASIA syndrome
Due to the increase in the prevalence and incidence of autoimmune diseases in the world population, Yehuda Schoenfeld described in 2011 the ASIA syndrome (Autoimmune Syndrome Induced by Adjuvants), in which certain adjuvants (nonspecific stimulating agents of the immune system), such as alum, pristine, infection and also silicone would act as inducers of autoimmune symptoms in genetically predisposed patients. Thus, BII would be a subtype of the ASIA syndrome5,6.
Based on this publication and the diagnostic criteria proposed by the author, some studies with small series have tried to relate silicone implants to the presence of systemic symptoms directly. However, the association between silicone implants and symptoms is uncertain. It is unclear whether these symptoms would not have developed even if the implants had not been placed7-9.
The important thing to consider from these epidemiological studies is that, although an increased risk of implant-related connective tissue disease was excluded, the sample sizes were too small to exclude an increase in extremely rare connective tissue diseases5.
Silicone is not considered an inert material, as several immunological effects have been reported. Silicone gel can migrate through the rupture of the elastomer or even with its membrawne intact - a phenomenon called gel bleed, which clinically may be detectable through axillary and mediastinal adenomegaly, with well-described characteristics of silicone gel accumulation (siliconomas), regardless of cohesiveness and elastomer type2,10.
Silicon particles can be phagocytosed by macrophages and trigger an immune response through the activation of B and T lymphocytes. The mechanisms by which an autoimmune phenomenon develops are numerous and include dysregulation of innate and adaptive immunity in those patients genetically predisposed to autoimmunity. It is currently difficult to identify such patients at risk. However, the silicone implant should be carefully analyzed in those patients with a previous history of disease induced by another adjuvant, established autoimmune disease, severe allergies or important family history of diseases. autoimmune5,10.
Breast Implant Illness
Although the ASIA syndrome was described a decade ago, we are experiencing a new moment in recent years. There is a great demand for patients who already have silicone implants and report systemic symptoms. Today, the reach and influence of TV have been reduced by the Internet, especially social networks, where discussion groups on various medical problems have become popular. While some forums may indeed be fruitful, others may promote the sharing of incorrect information by unqualified people11.
With the “boom” - or “viralization” - of the subject on the Internet and social networks, hundreds of signs and symptoms have been related to silicone implants, usually nonspecific (Chart 1). According to Lee et al.12, the most common symptoms reported by patients are chronic fatigue, arthralgia, mental confusion, myalgia, memory loss, difficulty concentrating and dry eyes.
| Anxiety | Depression | Weight gain |
|---|---|---|
| Loss of hair | Chronic fatigue | Visual changes |
| Sleep disorders | Tinnitus | Premature aging |
| Drop in libido | Arthralgia | Myalgia |
| Urinary urgency | Fibromyalgia | Skin rash |
| Palpitations | Fever | Raynaud’s Syndrome |
| Panic Syndrome | Irritable bowel syndrome | Lactose intolerance |
| Thyroiditis | Memory loss | Dry mouth |
There are no diagnostic tests for BII, no scientific evidence-based method to differentiate it from other conditions that share similar symptoms (irritable bowel syndrome and fibromyalgia, for example) and very little knowledge about its onset, course, risk factors, causes and appropriate management.
A small study analyzed capsules after explantation and showed that there seems to be a relationship between the presence of biofilm - mainly due to the P. acnes bacteria. This bacterium, which has been linked to the development of other rheumatic diseases, would cause chronic irritation in the capsule and serve as a trigger for symptoms1,12,13.
Although the surgeon’s impulse is to dissuade the patient and discourage implant removal, we must remember that this right is hers, just as she had when she chose to have her implant included. When a patient comes to their doctor to inquire about their implants, it is an opportunity to address their concerns, provide scientific education and treat if there is a problem.
It is important to offer real assistance to those who need guidance and care. One of the main complaints of women diagnosed with BII is the lack of information at the time of implantation. Many reported that they were not instructed on the procedure’s risks, especially concerning the development of symptoms, BIA-ALCL and, mainly, that implants are not lifelong11,14,15.
Trust is the foundation for a good doctor-patient relationship, and it is based on the belief that the doctor is working for the best of the patient. The break occurs when the patient realizes that her doctor has made a technical or judgment error. Not listening to patients’ complaints, labeling them or assuming an unfriendly attitude will drive them away from the plastic surgeon’s office, discredit the specialty and increase litigation rates11,14.
It is important to remember that, despite being extensively studied from different perspectives, the scientific community has never looked specifically at the direct relationship between silicone implants and systemic symptoms. So far, there are no prospective studies with good scientific evidence to confirm or refute this hypothesis. Until then, we must be doctors above plastic surgeons and treat our patients with all the attention and respect they deserve9.
Although we have few answers at the moment, the role of the plastic surgeon is to try to differentiate patients who may actually be developing an autoimmune disease due to the breast implant from those who were induced to be diagnosed with symptoms. The lack of diagnostic methods reinforces the importance of careful anamnesis and clinical examination and understanding the patient’s life context. Such differentiation is extremely important in order to avoid unnecessary surgical interventions1,16.
Newby et al.1, when applying questionnaires to three different groups of women (with BII; undergoing explants; without symptoms), found that 98% of the participants use support networks on the Internet, such as Facebook and Instagram groups, and that 62 % reported that the groups made them more alert to the diagnosis and fearful of the possibility of developing symptoms. In addition, they showed that self-reported patients with BII have higher rates of anxiety and depression than women undergoing explantation and asymptomatic women, respectively. The same authors report that patients opt for the explant on average 10 years after the primary surgery, despite reporting the onset of symptoms within the first 2 years, which worsen over time1.
Explant
The option to remove implants has been growing dramatically in recent years, one of the ten most performed surgeries in the United States last year. In the same way that the diagnosis is commonly made through social network groups, the treatment is also indicated by this means, so it is common for patients to arrive at the office requesting the performance of the “explant with capsulectomy en bloc.” The terminology “en bloc” is restricted to oncological pathologies, and, in the context of silicone implants, it is indicated only in cases of anaplastic cell lymphomas (BIA-ALCL)15-17.
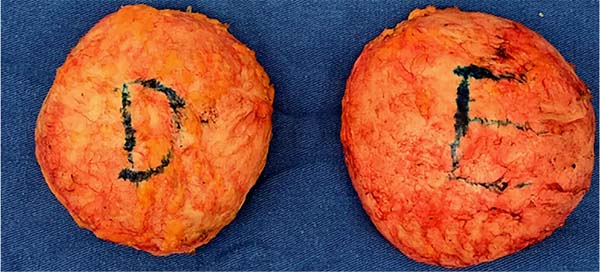
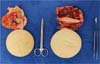
En bloc resection consists of resection of the implant, its capsule and adjacent tissues (safety margin) without capsule violation. In the context of BII, there is no evidence of capsule disease, and the incidence of capsular pathologies is extremely low (0.2%). Total capsulectomy should be performed preferably (Figures 1 and 2), as long as it is technically feasible and safe. Special attention should be given to implants in the retromuscular plane, always weighing the risk-benefit ratio, given the possibility of chest wall perforation, pneumothorax and even death17.
The literature shows variable symptom improvement rates after explantation. Rohrich et al.8 showed a progressive improvement in quality of life and body pain indices in patients undergoing explantation in the first 6 months after surgery compared to the control group. De Boer et al.18 showed a symptom improvement rate of 63% after observation of 14 months after explantation.
Magnusson et al.3, in turn, stratified patients into three distinct prognostic categories after explantation. Patients without evidence of rheumatic or autoimmune disease (type A) have the best prognosis, improving up to 80% of physical symptoms and 93% of psychological factors. Women with evidence of rheumatic disease, without the autoimmune disease (type B), tend to have a brief improvement in symptoms but experience a recurrence of symptoms after 6 to 12 months (“Honeymoon period”). On the other hand, women who have a confirmed diagnosis of autoimmune disease (type C) have the worst evolution, with no improvement in symptoms or serological markers. Likewise, Lee et al.12 showed that some patients showed improvement in the most common symptoms after explantation with capsulectomy, except for patients diagnosed with autoimmune disease.
On the other hand, Newby et al.1 demonstrated that women who underwent explant surgery had more severe physical symptoms and worse mental health than the control group, although the symptoms were milder than patients with BII and those with their implants. The authors conclude that these results suggest that explantation may not be a cure for BII and that symptoms may not resolve completely1.
After explantation, patients are generally satisfied with their aesthetic results and have lower anxiety and stress levels after the procedure3,8.
CONCLUSION
The relationship between silicone breast implants and systemic diseases, including autoimmune diseases, has been postulated, studied and discussed since the 1960s, but the debate continues today. Prospective, randomized, well-designed studies are needed, correlating different periods of patients, from the preoperative period of the implant to the post-explant period.
Although we live in a world of lives, 5G and instant responses, good science continues to move slower. The answers that everyone, doctors and patients, aspire to will take a few years to arrive, as studies are developed specifically to look at symptoms and their direct relationship to silicone implants.
Until then, we must be calm and considerate. There is no room for sensationalism, fads, or panic in serious medicine. Our fundamental role is to welcome patients, listen to their complaints, and explain what evidence is available at the moment and the risks of the explant procedure. The decision is up to them.
The impulse must not be part of the decision-making process. The implant should not be performed, nor should it be explanted by external pressure or by an anonymously authored post on social networks. All information, risks, outcome expectations, and possible benefits must be clarified preoperatively and a well-written consent form. The omission of some information can be fatal in the doctor-patient relationship and the loss of trust in the specialty. It is a surgical procedure and, as such, must be respected, as it is not without risks.
REFERENCES
1. Newby JM, Tang S, Faasse K, Sharrock MJ, Adams WP. Commentary on: Understanding Breast Implant Illness. Aesthet Surg J. 2021;41(12):1367-79.
2. Bozola A. Past, present and future using silicone breast implants in Brazil, a 45-year report. Rev Bras Cir Plást. 2020;35(4):505-13.
3. Magnusson MR, Cooter RD, Rakhorst H, McGuire PA, Adams WP Jr, Deva AK. Breast Implant Illness: A Way Forward. Plast Reconstr Surg. 2019;143(3S):74S-81S.
4. Sánchez-Guerrero J, Colditz GA, Karlson EW, Hunter DJ, Speizer FE, Liang MH. Silicone breast implants and the risk of connective-tissue diseases and symptoms. N Engl J Med. 1995;332(25):1666-70.
5. Fuzzard SK, Teixeira R, Zinn R. A Review of the Literature on the Management of Silicone Implant Incompatibility Syndrome. Aesthetic Plast Surg. 2019;43(5):1145-9.
6. Shoenfeld Y, Agmon-Levin N. ‘ASIA’ - autoimmune/inflammatory syndrome induced by adjuvants. J Autoimmun. 2011;36(1):4-8.
7. Miseré RML, Colaris MJL, van der Hulst RRWJ. The Prevalence of Self-Reported Health Complaints and Health-Related Quality of Life in Women With Breast Implants. Aesthet Surg J. 2021;41(6):661-8.
8. Rohrich RJ, Kenkel JM, Adams WP, Beran S, Conner WC. A prospective analysis of patients undergoing silicone breast implant explantation. Plast Reconstr Surg. 2000;105(7):2529-37.
9. Barbosa MR, Makris UE, Mansi IA. Association of Breast Implants with Nonspecific Symptoms, Connective Tissue Diseases, and Allergic Reactions: A Retrospective Cohort Analysis. Plast Reconstr Surg. 2021;147(1):42e-9e.
10. Watad A, Rosenberg V, Tiosano S, Cohen Tervaert JW, Yavne Y, Shoenfeld Y, et al. Silicone breast implants and the risk of autoimmune/rheumatic disorders: a real-world analysis. Int J Epidemiol. 2018;47(6):1846-54.
11. Mcguire PA, Haws MJ, Nahai F. Breast Implant Illness: How Can We Help? Aesthet Surg J. 2019;39(11):1260-3.
12. Lee M, Ponraja G, McLeod K, Chong S. Breast Implant Illness: A Biofilm Hypothesis. Plast Reconstr Surg Glob Open. 2020;8(4):e2755.
13. Dush DM. Breast implants and illness: a model of psychological factors. Ann Rheum Dis. 2001;60(7):653-7.
14. Steve AK, Temple-Oberle C, Yeung JK, Lafreniere AS, Harrop AR. “You Helped Create This, Help Me Now”: A Qualitative Analysis of Patients’ Concerns about Breast Implants and a Proposed Strategy for Moving Forward. Plast Reconstr Surg. 2021;147(1):16e-24e.
15. Jewell ML, Jewell HL. Breast Implant-Associated Illness: Medicine by Belief, So Says Dr. Google. Aesthet Surg J. 2019;39(4):NP87-9.
16. Calobrace MB, Mays C. An Algorithm for the Management of Explantation Surgery. Clin Plast Surg. 2021;48(1):1-16.
17. Johal KS, Floyd D. To Bloc or Not to Bloc: Challenges in the Management of Patients Requesting “En-Bloc Capsulectomy”. Aesthet Surg J. 2020;40(9):NP561-3.
18. de Boer M, Colaris M, van der Hulst RRWJ, Cohen Tervaert JW. Is explantation of silicone breast implants useful in patients with complaints? Immunol Res. 2017;65(1):25-36.
1. Federal University of Santa Catarina, Department of Plastic Surgery and Burns,
Florianópolis, SC, Brazil.
2. Erasto Gaertner Hospital, Curitiba, Paraná, Brazil.
Corresponding author: Ricardo Votto Júnior, Avenida Osvaldo Rodrigues Cabral 1570, sala 208, Florianópolis, SC, Brazil, Zip Code 88015-710, E-mail: ricardo.votto@ufsc.br
Article received: April 14, 2021.
Article accepted: October 15, 2021.
Conflicts of interest: none.







 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter