

Case Report - Year 2021 - Volume 36 -
Dynamic eyelid reconstruction with temporal muscle transfer: a case report
Reconstrução palpebral dinâmica com transferência do músculo temporal: relato de caso
ABSTRACT
Surgical excisions of skin neoplasms mainly cause defects in the eyelid region. The objectives of eyelid reconstruction are based on the restoration of this anatomical unit’s functionality to maintain eye protection and recovery from a normal appearance due to the critical importance of the periocular region in facial aesthetics. Repair of eyelid defects begins with a careful evaluation of the anatomical components that have been resected and need to be reconstructed; the extent and location of the defect will guide the reconstruction. Large defects compromising the entire body thickness are a challenge for plastic surgeons. Thousands of surgical techniques have been described for the reconstruction of total thickness eyelid defects; we present in this article the description of a case of dynamic eyelid reconstruction with an association of a frontal flap with temporal muscle transposition after resection of a recurrent infiltrative basal cell carcinoma.
Keywords: Temporal muscle; Recovery of physiological function; Ocular neoplasms; Myocutaneous flap; Plastic surgery.
RESUMO
Os defeitos na região palpebral são causados principalmente por excisões cirúrgicas de neoplasias cutâneas. Os objetivos da reconstrução palpebral estão fundamentados na restauração da funcionalidade desta unidade anatômica para manter a proteção ocular e a recuperação de uma aparência normal devido à importância crítica da região periocular na estética facial. O reparo dos defeitos palpebrais começa com uma cuidadosa avaliação dos componentes anatômicos que têm sido ressecados e precisam ser reconstruídos; a extensão e a localização do defeito guiarão a reconstrução. Grandes defeitos comprometendo a totalidade da espessura palpebral são um desafio para os cirurgiões plásticos. Milhares de técnicas cirúrgicas têm sido descritas para a reconstrução de defeitos palpebrais de espessura total; apresentamos neste artigo a descrição de um caso de reconstrução dinâmica da pálpebra com associação de um retalho frontal com transposição do músculo temporal após ressecção de um carcinoma basocelular infiltrativo recidivado.
Palavras-chave: Músculo temporal; Recuperação de função fisiológica; Neoplasias oculares; Retalho miocutâneo; Cirurgia plástica.
INTRODUCTION
Eyelids are delicate structures and constitute a fundamental aesthetic and functional component of the face; they are the structures in charge of covering and protecting the eyeball and play a critical role in lubricating the eye. Perhaps no other human body region provides such a delicate interaction between anatomy, functionality, and aesthetics.
The primary objective in eyelid reconstruction is to restore this facial unit’s functionality to maintain eye protection, thus ensuring the preservation of vision; the most important secondary objective is to achieve a normal appearance due to the critical importance of the periocular region in social relations1. The restoration of the eyelids’ appearance and normal function requires the reconstruction of each of its components: conjunctiva, tarsus, and myocutaneous layer2.
Surgical excisions of skin neoplasms mainly cause tissue loss in the eyelid region; there are some other, less common etiologies, such as trauma, infections, congenital malformations, complications secondary to medical interventions, cryotherapy and irradiation3. Malignant tumors of the eyelid constitute about 40% of all carcinomas in the orbital region4. According to epidemiological studies, basal cell carcinoma is the most common eyelid tumor, followed by squamous cell carcinoma5. Approximately 90% of cases affect the lower eyelid and the medial corner region6 and are characterized by a constant and progressive growth that tends to infiltrate the underlying tissues2.
Eyelid reconstruction after resection of a malignant tumor is planned based on the size and depth of the defect, involvement of the medial or lateral corner, and the presence or absence of lesion of the lacrimal system7. Lesions with less than 25% involvement can be resolved with primary closure of the defect in most cases8. However, eyelid defects covering more than a quarter of the eyelid width cannot be treated with primary closure and require a more complex reconstructive approach9. For deep and wide defects, with both the anterior and posterior lamella involvement, multiple therapeutic options have been described with local skin flaps associated with cartilaginous or mucoperiosteal grafts that provide adequate coverage, support and similarity of the skin, but with the absence of functioning muscles on restored eyelids. Dynamic eyelid reconstruction through muscle transposition or functioning free muscle flaps provides an optimal solution for the recovery of eyelid functionality and subsequent eye protection.
This work aims to report a case of dynamic reconstruction of the eyelid complex, immediately after the resection of an infiltrative basal cell carcinoma, with the restitution of the different layers previously described.
CASE REPORT
A 55-year-old male patient from the interior of the state of Rio Grande do Sul, a merchant, with arterial hypertension with adequate pharmacological control. It presents a clinical picture of plaque-like cutaneous lesion, erythematous, non-desquamative, progressive growth in the upper eyelid, with extension and involvement of the inner corner and medial third of the ipsilateral lower eyelid. Initially evaluated by dermatology, the lesion was biopsied with an anatomopathological result of infiltrative basal cell carcinoma, before which treatment with Mohs micrographic surgery and immediate reconstruction was decided.

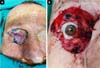
The patient was taken to surgery under general anesthesia for resection of the lesion with safety margins, according to the technique previously described (Figure 1) and periorbital reconstruction of soft tissues at the same surgical time. The compromised region was infiltrated with 2% lidocaine with adrenaline. With the lesion’s exeresis, there was a loss of the total thickness of the upper and lower eyelid structures (anterior and posterior lamella) and destruction and disinsertion of the inner corner of the eye with partial preservation of the tear duct by cannulation with Silastic®. After the detailed evaluation of the described defect, it was decided to perform a dynamic reconstruction through combined surgery of temporal muscle transposition, cartilage graft of the auricular concha and rotation of the contralateral frontal flap for skin coverage.
First, a graft of cartilage from the ear shell was performed to mimic the tarsus and support the lower eyelid. Subsequently, using a pre-capillary incision with extension to the temporal region, the ipsilateral temporal muscle flap (Gillies) was made with distal bifurcation, by removing the muscle from its origin in the temporal fossa and preserving its insertion at the level of the coronoid process, thus guaranteeing the maintenance of muscle functionality for later mimicking of the function of the eyelid orbicularis muscle. After the preparation, the flap was transposition and positioning for the reconstruction of the muscle layer, both of the upper eyelid and the lower eyelid; the apex of the bifurcation was located at the lateral corner level, and the positioning of the cephalic and caudal divisions in the upper and lower eyelids, respectively (Figure 2). Subsequently, the inner corner was reconstructed by canthopexy with steel wire (fixed to the orbit’s superomedial edge by perforation).
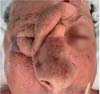
Finally, to restore the outermost layer and cover the previously described structures, a contralateral frontal flap was made “in mask” to mimic the eyelid rhyme’s opening, with anti-clockwise rotation (Figure 3).
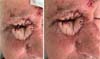
The patient evolved adequately in the postoperative period, performing weekly follow-up with the assistant team, confirming the flaps’ viability. Approximately six weeks after the initial procedure, a second surgical time was performed for sectioning the pedicle of the frontal flap, remodeling and repositioning the edges of the donor area, and refinement of the reconstructed periocular region. The eyelid region’s suture threads were left long enough to reduce the risk of corneal injury (Figure 4). Postoperative recovery was adequate, with excellent healing and maintenance of eyelid dynamics with complete closure of the cleft, thus ensuring ocular protection and lubrication.
DISCUSSION
Repair of eyelid defects begins with a careful evaluation of the anatomical components that have been resected and need to be reconstructed; the extent and location of the same will guide the reconstruction. In patients with full-thickness defects, the size of the defect and the degree of laxity in the periocular soft tissues are critical determinants of the best reconstructive procedure or the combination of procedures necessary to restore palpebral anatomy, functionality and aesthetics.
The reconstruction options are summarized, according to the affected layer, as follows: anterior lamella: cutaneous flap, myocutaneous flap, full-thickness skin graft; support/structure: fascial flap, periosteal flap, fascia sling, cartilaginous graft; lining: oral mucosa, local conjunctiva flap; or composite flaps such as mucoperichondrial graft or tarsoconjunctival flap10.
It is important to follow a systematic approach to eyelid reconstruction. Small defects of the anterior lamella, with preservation of the tarsus, can occasionally be treated with healing by the second intention11. The best results observed with this type of approach are evidenced in superficial lesions in the region of the inner corner due to the resistance of the nasal bone to contracture, thus limiting the risk of scar ectropion; however, it can take several weeks, increasing the risk of infection, eye irritation and the need for occlusive dressings that obstruct the patient’s vision during the healing process12. If the defect involves less than 20% of the upper or lower eyelid margin in young individuals and up to 30% in older individuals, primary closure may be performed. A gain in horizontal stretching can be obtained through canthotomy or lateral cantholysis11. Superficial defects of the upper eyelid, limited to the anterior lamella, are better repaired by performing a full-thickness skin graft of the contralateral eyelid; in general, there is less secondary contracture with full-thickness skin grafts than with partial-thickness grafts13. In defects greater than 50%, reconstructions with local composite flaps such as frontal flap, Cutler-Beardflap, Mustardé flap or zygomatic region feed/rotation flaps are traditionally required of which need a second surgical time for the reconstruction of each of the affected layers14,15.
As reported, in large defects in which resection of the tarsal plate without preservation of the medial and lateral borders is necessary, it is necessary to provide structural stability to the reconstructed eyelid by performing a cartilaginous graft, usually of the auricular concha, a closed palate mucosa graft or a chondromucoid graft of the nasal septum16,17. Then, for the protection of the tarsal neo plate, a cover is needed to ensure the blood supply for the graft’s viability, which in the case reported was obtained with the transposition of the temporal muscle. This type of flap receives its vascularization of the anterior and posterior deep temporal artery, thus having two vascular territories that allow the separate use of the fascia or temporal muscle to elevate the flap, making it very versatile in the reconstruction of the head and neck18. In the case reported, this flap also favored the eyelid’s dynamic reconstruction by contraction of the temporal muscle fiber that countered the opening and closure of the eyelid cleft.
The reconstruction of total eyelid defects represents a significant challenge in recreating a cosmetically acceptable eyelid with a degree of dynamic function capable of providing adequate protection to the eyeball, preventing dry eye and secondary risk corneal ulcer19. Several treatment methods have been proposed to restore eyelid functionality, such as free myocutaneous flaps with transference and nerve anastomosis and local muscle or myocutaneous flaps. Eyelid resuscitation by temporal muscle transfer was initially described by Gilliesin 193420 and has undergone multiple modifications over time to improve the efficacy of the technique21. The Gillies flap allows the creation of a functional eye covering of both the upper and lower eyelids, with the mimic of the lateral corner and the eyelid cleft by bifurcation of its most distal portion; it is a useful procedure, versatile, effective and, with adequate knowledge of anatomy, technically easy to perform. Additionally, compared to microsurgery is a fast and less complex procedure, which can be an advantage in certain patients.
Finally, despite all technical dexterity and proper planning, total thickness palpebral reconstruction may not be functionally successful. The patient may remain with significant eye discomfort and irritation due to the cornea’s contact with the structures used for reconstruction. The problem of ocular lubrication should also be mentioned. In extreme situations, there are reports of patients opting for enucleation. Thus, the resolution of these potential postoperative problems remains a reason for the study.
CONCLUSION
Due to its eye protection function and aesthetic impact, the importance of eyelid reconstruction is well established among plastic surgeons. Each eyelid component should be carefully evaluated and, if necessary, reconstructed with the most indicated surgical technique. Obtaining a dynamic upper eyelid is a differential in the quality of eye protection, having as therapeutic options the realization of local or locoregional flaps, simple or composed, single or combined or, if necessary and available, microsurgical reconstruction. Temporal muscle transfer is a versatile, effective, fast and long-term durability option for reconstructing large eyelid defects.
REFERENCES
1. Lo Torto F, Losco L, Bernardini N, Greco M, Scuderi G, Ribuffo D. Surgical treatment with locoregional flaps for the eyelid: a review. Biomed Res Int. 2017;2017:6742537. DOI: https://doi.org/10.1155/2017/6742537
2. Wójcicki P, Zachara M. Surgical treatment of eyelid tumors. J Craniofac Surg. 2010 Mar;21(2):520-5. DOI: https://doi.org/10.1097/SCS.0b013e3181d023eb
3. Fante R. Reconstruction of the eyelids. In: Baker S, ed. Local flaps in facial reconstruction. 2nd ed. Philadelphia: Mosby Elsevier; 2007. p. 387-413.
4. Hałoń A, Błazejewska M, Sabri H, Rabczyński, J. Tumors and tumor-like lesions of eyelids collected at Department of Pathological Anatomy Wroclaw Medical University, between 1946 and 1999. Klin Oczna. 2005;107:475-8.
5. Cook Junior BE, Bartley GB. Epidemiologic characteristics and clinical course of patients with malignant eyelid tumours in an incidence cohort in Olmsted County, Minnesota. Ophthalmology. 1999 Abr;106(4):746-50. DOI: https://doi.org/10.1016/S0161-6420(99)90161-6
6. Papadopoulus O, Konofaos P, Chrisostomides C, Georgiou P, Frangoulis M, Cahmpsas G, et al. Orbitopalpebral repair after 835 excision of malignant tumors. Scand J Plast Reconstr Surg. 2005;39(6):353-9. DOI: https://doi.org/10.1080/02844310500228167
7. Hayano S, Whipple K, Korn B, Kikkawa D. Principles of periocular reconstruction following excision of cutaneous malignancy. J Skin Cancer. 2012;2012:438502. DOI: https://doi.org/10.1155/2012/438502
8. O’Donnell BA, Mannor GE. Oculoplastic surgery for upper eyelid reconstruction after cutaneous carcinoma. Int Ophthalmol Clin. 2009;49(4):157-72. DOI: https://doi.org/10.1097/IIO.0b013e3181b88b2d
9. Spinelli HM, Jelks GW. Periocular reconstruction: a systematic approach. Plast Reconstr Surg. 1993 Mai;91(6):1017-24;discussion:1025-6.
10. Haykal S, Antonyshyn O, Gill H. The temporalis muscle flap: a useful adjunct in reconstruction of combined defects of the upper and lower eyelids. Plast Surg Case Studies. 2015 Jun;1(1):19-23. DOI: https://doi.org/10.1177/2513826X1500100108
11. Chang E, Esmaeli B, Butler C. Eyelid reconstruction. Plast Reconstr Surg. 2017 Nov;140(5):724e-35e. DOI: https://doi.org/10.1097/PRS.0000000000003820
12. Mathijssen IM, Van Der Meulen JC. Guidelines for reconstruction of the eyelids and canthal regions. J Plast Reconstr Aesthet Surg. 2010 Set;63(9):1420-33. DOI: https://doi.org/10.1016/j.bjps.2009.05.035
13. Shorr N, Goldberg RA, McCann JD, Hoenig JA, Li TG. Upper eyelid skin grafting: an effective treatment for lagophthalmos following blepharoplasty. Plast Reconstr Surg. 2003 Out;112(5):1444-8. DOI: https://doi.org/10.1097/01.PRS.0000081477.02812.C9
14. Alghoul M, Pacella S, McClellan T, Codner M. Eyelid reconstruction. Plast Reconstr Surg. 2013 Ago;132(2):288e-302e. DOI: https://doi.org/10.1097/PRS.0b013e3182958e6b
15. Gündüz K, Demirel S, Günalp I, Pola B. Surgical approaches used in the reconstruction of the eyelids after excision of malignant tumors. Ann Ophthalmol. 2006 Set;38(3):207-12. DOI: https://doi.org/10.1007/s12009-006-0006-1
16. Li TG, Shorr N, Goldberg RA. Comparison of the efficacy of hard palate grafts with acellular human dermis grafts in lower eyelid surgery. Plast Reconstr Surg. 2005 Set;116(3):873-8. DOI: https://doi.org/10.1097/01.prs.0000177694.39466.b2
17. Lalonde DH, Osei-Tutu KB. Functional reconstruction of unilateral, subtotal, full-thickness upper and lower eyelid defects with a single hard palate graft covered with advancement orbicularis myocutaneous flaps. Plast Reconstr Surg. 2005 Mai;115(6):1696-700. DOI: https://doi.org/10.1097/01.prs.0000161455.07552.48
18. Birt BD, Antonyshyn O, Gruss JS. The temporalis muscle flap for head and neck reconstruction. J Otolaryngol. 1987 Jun;16(3):179-84.
19. Stewart C, Tan LT, Johnson D, Norris J. Key Issues when reconstructing extensive upper eyelid defects with description of a dynamic, frontalis turnover flap. Ophthalmic Plast Reconstr Surg. 2016 Jul;32(4):249-51. DOI: https://doi.org/10.1097/IOP.0000000000000721
20. Gillies H. Experiences with fascia lata grafts in the operative treatment of facial paralysis: (section of otology and section of laryngology). Proc R Soc Med. 1934 Ago;27(10):1372-82.
21. Evrenos M, Bali Z, Yaman M, Yoleri L. Modified temporalis muscle flap for eyelid reanimation. J Craniofac Surg. 2018 Out;29(7):e649-e54. DOI: https://doi.org/10.1097/SCS.0000000000004692
1. Hospital de Clinicas de Porto Alegre, Plastic
and Craniomaxillofacial Surgery Service, Porto Alegre, RS,
Brazil.
2. Hospital Sao Lucas, PUC, Dermatological Surgery
Service, Porto Alegre, RS, Brazil.
MAJZ Analysis and/or data interpretation, Conceptualization, Final manuscript approval, Methodology, Writing - Original Draft Preparation, Writing - Review & Editing
CPP Analysis and/or data interpretation, Conceptualization, Final manuscript approval, Writing - Review & Editing
SVH Conceptualization, Methodology, Writing - Review & Editing
ICS Conceptualization, Writing - Original Draft Preparation
EMZ Conceptualization, Writing - Original Draft Preparation
JJCR Conceptualization, Writing - Original Draft Preparation
Corresponding author: Mônica Alexandra Jimenez Zerpa, Avenida Ipiranga, 7464, Sala 1118, Jardim Botânico, Porto Alegre, RS, Brazil., Zip Code: 91530-000, E-mail: monijimenezz@gmail.com
Article received: July 06, 2020.
Article accepted: January 10, 2021.
Conflicts of interest: none
Institution: Hospital de Clinicas de Porto Alegre, Porto Alegre, RS, Brazil.







 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter