

Original Article - Year 2021 - Volume 36 -
Mammoplasty with mirrored "D" technique and laser-assisted liposuction
Mamoplastia com técnica em "D" espelhado e lipoaspiração assistida por laser
ABSTRACT
Introduction: Mammoplasty is an aesthetic and functional procedure, considered an arduous surgery, intending to improve the breasts’ shape with a minimum of apparent scarring and reposition the nipple-areola complex. There is no standard procedure, and a technique’s choice depends on different factors, which justifies the diversity of techniques described. We will present the mirrored “D” technique broadly in different (anatomical) scenarios, together with laser-assisted liposuction with standard marking, which facilitates the surgical procedure with final symmetry and maintenance of aesthetic results, correcting the recurrences.
Methods: Technique performed in 46 patients, female, without exclusion of race, between 20 and 66 years old, operated by the authors between January 2017 and March 2020, at the Hospital Antoninho da Rocha Marmo - São José dos Campos - Brazil. Retrospective work with the application of the validated Breast-QTM questionnaire to assess the degree of satisfaction.
Results: There was no surgical revision, postoperative infection or necrosis of the papillary areolar plaque, 5 cases of papillary areolar plaque epidermolysis, treated with flavonoids and horse chestnut (linfa creamTM), without sequelae. Parenchyma resection from 80 to 1,100g, average 477.1g. Laser-assisted liposuction between 150 to 790ml, average 438.6ml. The final vertical scar averaged 6.7cm, stable after two years, with Breast-QTM evaluation of very satisfied (86%).
Conclusion: We consider the mirrored “D” technique and laser-assisted liposuction a good surgical option due to its systematization and versatility in different mammoplasty scenarios, maintaining a coniform shape with a smaller scar and maintaining the validated results.
Keywords: Breast; Lasers; Skin; Plastic surgery; Mammoplasty.
RESUMO
Introdução: A mamoplastia é um procedimento estético e funcional, considerada uma cirurgia árdua, com o objetivo de melhorar as mamas na sua forma com o mínimo de cicatriz aparente e reposicionar o complexo areolopapilar. Não existe um procedimento padrão e a escolha de uma técnica depende de distintos fatores, o que justifica a diversidade de técnicas descritas. Apresentaremos a técnica em “D” espelhado, de uma maneira ampla em distintos cenários (anatômicos), junto à lipoaspiração assistida por laser com marcação padrão, o que facilita o procedimento cirúrgico com uma simetria final e manutenção de resultados estéticos, corrigindo as recidivas.
Métodos: Técnica realizada em 46 pacientes, do sexo feminino, sem exclusão de raça, entre 20 a 66 anos, operadas pelos autores entre janeiro de 2017 a março 2020, no Hospital Antoninho da Rocha Marmo - São José dos Campos - Brasil. Trabalho retrospectivo com aplicação do questionário validado Breast-Q® para avaliar o grado de satisfação.
Resultados: Não teve revisão cirúrgica, sem infecção pós-operatória ou necrose da placa areolopapilar, 5 casos de epidermólise da placa areolopapilar tratados com flavonoides e castanha da índia (linfa cream®), sem sequelas. Ressecção do parênquima de 80 a 1.100g média 477,1g. LAL entre 150 a 790ml, média 438,6ml. A cicatriz vertical final média 6,7cm, estável após 2 anos, com avaliação Breast-Q® de muito satisfeito (86%).
Conclusão: Consideramos a técnica em “D” espelhado e lipoaspiração assistida por laser uma boa opção cirúrgica pela sistematização e versatilidade em diferentes cenários de mamoplastia, mantendo formato coniforme com cicatriz menor e manutenção dos resultados validados.
Palavras-chave: Mama; Lasers; Pele; Cirurgia plástica; Mamoplastia.
INTRODUCTION
Currently, Brazil ranks second in the world ranking of plastic surgeries and first in non-surgical procedures, according to the latest statistic from the International Society of Aesthetic Plastic Surgery (ISAPS), in 2019. In the last census carried out by the Brazilian Society of Plastic Surgery (SBCP - Sociedade Brasileira de Cirurgia Plástica) from 20181, we found that the most performed procedures are breast augmentation in the first place, representing 18.8% of surgeries, followed by liposuction with 16.1%, abdominal dermolipectomy with 15.9%, mastopexy with 11.3% and breast reduction with 9.9% of procedures; equating with the reference of statistics worldwide.
Mammoplasty is an aesthetic and functional procedure aimed at replacing the nipple-areola complex, reducing the size of the breasts, and improving its shape with minimal scarring. However, there is no consensus on an ideal technique2-5, justifying the diversity of techniques described.
Patients who seek a mammoplasty do it intending to relieve physical and emotional discomfort, according to Sabino Neto et al. (2008)6. When choosing the technique for successful breast surgery, we must reflect between the shape and the final scar3-5 and consider several important points in the assessment: the type of breast, shape, size and degree of ptosis. Decide on the type of areolopapillary pedicle (superior, inferior, lateral, medial, or central) in gland resection (medial, lateral, superior, inferior or peripheral). Analyze the final scar whether inverted “T,” periareolar, vertical or L5. Think about combined treatments with or without the inclusion of prostheses, lipotransfer or use of laser, as well as considering skin and scar care (drug delivery).
Instruments that assess patients’ satisfaction and quality of life are increasingly used in breast surgeries, both aesthetic and reconstructive. The PRO measures (patient-reported outcomes) offer the possibility of objectively quantifying the results from the patient’s point of view. Breast-QTM is a PRO-designed instrument, a questionnaire considered to be an internationally known tool developed to assess the results of breast surgeries, specifically to measure the quality of life and satisfaction of patients undergoing this surgery7,8.
Spear et al. (2004)4 report that after an analysis of 6 years in their practice, their indexes showed post-surgical revisions in 54% of patients, for various reasons, the most common being the desire for higher breasts.
Liposuction is the second most performed procedure globally, liposculpture that remodels specific areas of the body, removing excess and often replacing fat in areas of depression or restoring the convexity of a region. The objective of liposuction is to leave the body harmonious (concave and convex), sometimes following the musculature or eliminating shadow triangles (accumulations) and leaving the light (convexity).
In the last three decades, new technologies such as ultrasound and laser were developed to improve liposuction and used to increase the effectiveness, safety, and reduce the time of the procedure, benefiting patients and surgeons without neglecting the contour result.
In the literature, laser-assisted liposuction (LAL) was first described by Dressed (1990) apud Apfelberg et al. (1994)9. Shortly after that, Apfelberg et al. (1994, 1996)9,10 reported using a 1,064nm light source during liposuction in 51 patients.
LAL photothermal energy melts fat11, making this procedure ideal for technically difficult cases, such as fibrous areas in the breast, abdomen, back, male flanks10, and surgical revisions, where the tissue is difficult to access or access presents irregularities12,13.
Compared with traditional liposuction (LT), LAL can reduce postoperative pain and edema and hematomas14-18 due to thrombosis of blood vessels and laser-induced closure of lymphatic channels18. Several studies demonstrate the use of LAL, with good aesthetic results described, with an important skin retraction, less blood loss, decreased physician fatigue, justified by the easy emulsification of fat, which allows quick, efficient and less efficient time13,18.
Other studies claim important collagen production stimulated by the heating of the deep dermis and the connective septa of the subcutaneous tissues, inducing collagen denaturation (neo-synthesis) and protein production, followed by vascular proliferation19,20.
Jean et al. (2015)20 suggest potential advantages of LAL over LT, preserving nerve endings and better blood vessel clotting with less blood loss and mild ecchymosis.
The coagulation-modified collagen observed in microscopy could explain the great aesthetic benefit in skin retraction, increasing its tone and texture, with considerable improvement in flaccidity16,21,22. This is the specific clinical indication that makes LAL a superior choice compared to TL14,22. LAL can also be considered a complement and, by some colleagues, a substitute for traditional liposuction15. Regarding the learning curve, it is indisputable that there is more specific training with LAL when compared to LT15. Wolfenson et al. (2015)23 described the various regions that can be treated with (LAL): flanks (31.5%), face/submental (28%), abdomen (19.5%), breasts (male) (14%) and other regions (7%).
In the literature, the LAL technique has also been used to treat gynecomastia24; in a study carried out by Kwang et al. (2015),24, 13 patients with gynecomastia underwent LAL. Before the procedure, chest circumference measurements were recorded, and breast thickness was controlled with CT images. Twelve weeks later, the patients were again reviewed using the same measurements, and both the mean chest circumference and breast thickness decreased significantly24. This type of study opened the range of indications for LAL in different body regions and among them the breast, not only for the treatment of gynecomastia but also as a supporting procedure in reconstructive and aesthetic breast surgery.
LAL is based purely on a thermal effect13,17,23,25,26, the following properties should be considered when determining the effectiveness of laser lipolysis: the wavelength used and the energy released17, as well as the time applied to the tissue. The laser light energy is converted into thermal energy inside the adipose tissue; it diffuses to the dermis and probably to the skin surface, reaching 48°C - 50°C to induce collagen contraction and strengthening of the cutaneous tissue16,22. This shrinkage effect is continuous and can be identified for up to 3 to 6 months after the procedure12,22; therefore, continuous thermal monitoring is necessary, as the damage directly depends on the applied energy21,27.
According to Badin et al. (2005)12, in their study, 3,000 joules of energy per area resulted in significant irreversible damage compared to an area treated with lower power (1,000J). In other publications, adipocyte liquefaction, tissue carbonization and epidermal damage were observed with higher energy settings22,27-29.
Seeking better results in the treatment of breasts and their recurrences, a combination of considerations, adaptations and new technologies is acceptable. The mirror “D” mammoplasty technique described by the authors30,31, originally indicated for primary mastopexy and inclusion of silicone implants in hypoplastic breasts associated with moderate to severe ptosis. In this paper, we will present our experience of a systematic procedure in all our breast surgeries to treat primary and secondary mastopexies without implants, in association with LAL with maintenance and satisfaction of results, and validation with the Breast-QTM questionnaire.
OBJECTIVES
To present a reduction mammoplasty technique with the procedure’s systematization, use of LAL, and maintenance of results validated with Breast-QTM.
METHODS
We performed the lipomammoplasty technique using the mirrored “D”7,8 and laser in 46 female patients, without exclusion by race, aged between 20 and 66 years, operated by the authors between January 2017 and March 2020. The authors performed the procedures at the Hospital Antoninho da Rocha Marmo - São José dos Campos (CEP: 005/ADM/ARM/2020). The main complaint was breast ptosis. We used proper marking to determine the areas of decortication, skin resection, medial bipartite flap, assembly with crossed flaps and resection of the excess lateral flap to achieve breast harmonization—the flap with medial pedicle and vertical scar as the final result.
In all patients, to infiltrate and remove the emulsified fat, we used the technique of vibrolipoaspiration with a device branded vibrolipoTM registered by Anvisa.
Since 2015, in our In practice, we introduced the use of the DeligthTM brand laser registered at Anvisa, which has two wavelengths that we use according to the purpose of the treatment.
The laser at 915nm (for lipolysis) has selectivity on adipocytes, making the converted heat absorbed by the fat, causing its emulsification and subsequent excretion by the body.
In the laser at 980nm (for skin retraction), the selectivity is given by water, whose intense heating causes the retraction of collagen and elastin fibers, stimulating their regeneration and returning the tissue to a firm and delineated appearance, a key effect for the treatment of flaccidity.
The infiltration must be carried out in the same region to be aspirated, always in the intermediate subcutaneous layer (between the lamellar and areolar layers).
All patients were evaluated weekly during the first month, monthly until the sixth month and every three months until completing one year postoperatively (PO). After that, every six months until completing 24 months PO. The Brest-QTM questionnaire was applied preoperatively, at 12 months and 24 months.
Surgical technique
1. Marking
Mirrored “D” technique
The marking of the patient is performed in the supine position and arms close to the trunk. There is a difference of up to 1cm in the breast crease when compared to the crease marked in the standing position, which, in our experience, is reflected in a more appropriate and natural shape in the final result. In this position, the breasts naturally assume a symmetrical spatial adjustment, easily visualized in the positioning of the nipple-areola plate (NAP), canceling out the visible asymmetries in the orthostatic position, justified by the action of the volume and gravity binomial, which facilitates marking, resulting in naturally occurring breasts symmetrical.
With the patient in the supine position, a midline is marked from the sternal notch to the umbilical scar and the submammary crease, formed naturally by the positioning of the breasts in decubitus (Figure 1):
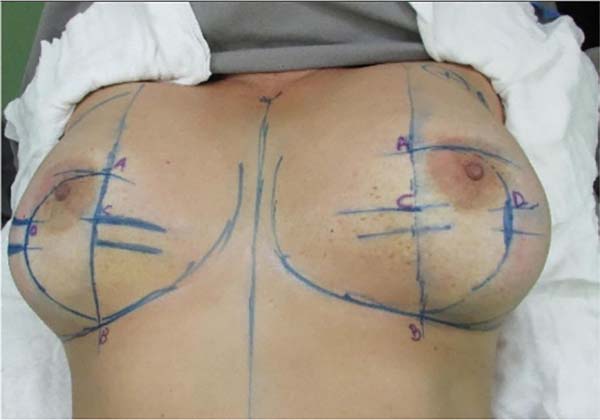
POINT A: This point is marked 10cm from the inframammary crease and 9cm from the midsternal line; the place of the intersection of these lines, we call point A.
POINT B: Considering the submammary crease naturally formed in the decubitus, point B is marked at 10cm from the midsternal line.
The union of points A and B determines the straight part of the “D” design.
POINT C: Point C is marked 3cm from point A on the straight-line joining A and B.
POINT D: With a bidigital block maneuver, point D corresponding to the maximum point of skin resection is marked.
DRAWING of the “D”: The mirrored “D” closure occurs by joining in a straight line between points A and B, and an arc laterally, from point A to point B, passing through D, including the areola superiorly, wherever it is located and respecting the limit of point D for the lower continuation of the arc.
The junction of points C and D at the end of the surgery will coincide with the lower edge of the new positioning of the areola. The beginning of the final vertical scar, which will be approximately 6 to 7 cm in length to the inframammary fold, being the point B is the end of the vertical scar, which provides symmetrical parallel vertical scars due to the 1cm difference in the marking between points A and B (Figure 1).
The mirror marking of the “D” on the other side is done in the same way. The “D” arch is different in most cases, depending on the asymmetry of the breasts.
Laser-Assisted Liposuction (LAL) technical marking
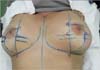
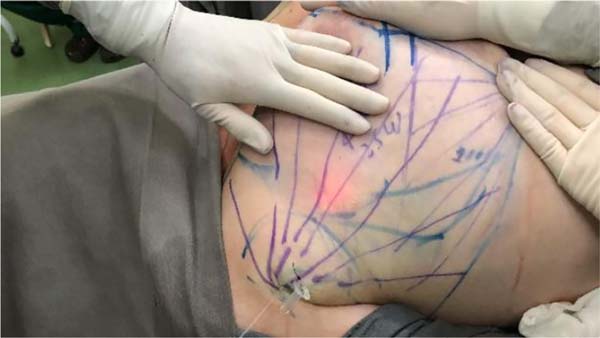
We divided the breast into four quadrants and marked the excess fat in the breast extension (anterior axillary line to posterior axillary line), including the axillary region (Figure 2).
2. Infiltration used
We infiltrate with the vibrolipo with a Klein 4mm cannula; we always recommend that it is wet with a solution of 1,000ml of saline solution + 4 ampoules of adrenaline (1:250,000).
3. Laser-Assisted Liposuction (LAL)
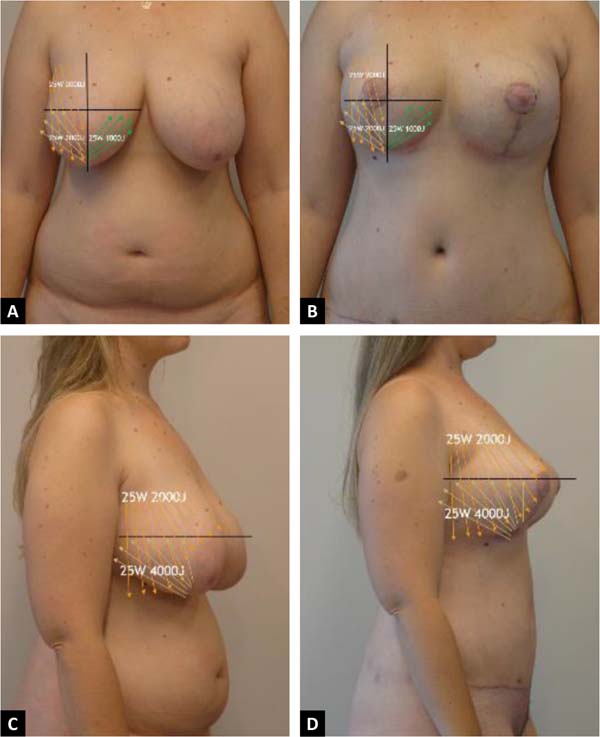
It is important to emphasize that we never aspire to the superior interior quadrant. We applied lipolaser in the superior and inferior external and inferior interior quadrants (Tables 1 and 2). In contrast, the vibrolipo is performed in the superior and inferior exterior quadrants, respecting the inferior interior.
| Region | Power |
|---|---|
| Superior exterior quadrant | 2000J |
| Inferior exterior | 1000J |
| Inferior interior | 1000J |
| Breast extension | 1000J |
| Total energy used 915nm 25W of power | 5000J |
| Region | Power |
|---|---|
| Superior exterior quadrant + exterior inferior | 3000J |
| Inferior interior | 500J |
| Breast extension | 1000J |
| Total energy used 980nm 25W of potency | 4500J |
Procedure steps and care
a. We use skin protectors.
b. The fiber must always be introduced into the fat tissue in the intermediate plane, tunneling the tissue (Figure 3). If the fiber is superficial, there is a risk of burning, and if it is too deep, in addition to losing the plane, it may have the risk of affecting organs. In inexperienced hands, it is very easy to transfix the fascia or the pleura in the thoracic region.
c. Always follow the fiber light(Figure 3). When the light is barely visible, it is in a deep plane; if it is very strong, it is in a superficial plane.
d. The fiber should always be parallel to the skin tissue.
e. The infiltration needs to be moist; we do not recommend tumescent, as it could lose the result of skin retraction.
f. Infiltration plan: infiltrate in the intermediate plan, which is the same plan we apply LAL.
g. At any sign of vascular alteration of the tissue, take the following measures: we use moist compresses and apply a cream with flavonoids in the affected region, helping the tissue flow (linfa creamTM registered at Anvisa), improving edema, pain and hyperchromic stains, in case of hematomas due to hemosiderin accumulation. We also prescribe for home use. We use this product in all our surgical procedures in the immediate postoperative period (dressing).
4. Technique in “D”: procedure
Schwartzman Maneuver:
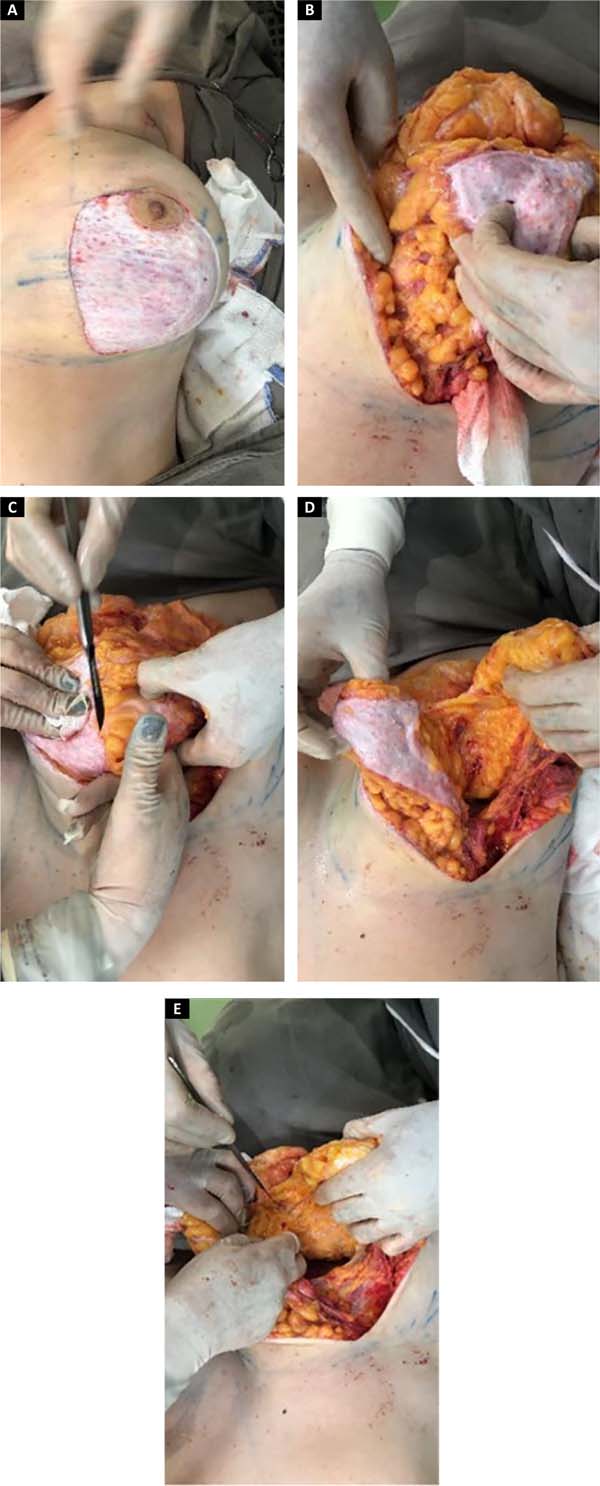
The surgery begins with marking the areola with a 4cm areolotome, followed by decortication of the skin over the tissue, in the extension of the marking of the “D” (Figure 4A).
Making the flap p. medial:
The medial flap is marked with a 5cm base and at least 1cm around the areola. The tissue is detached, maintaining a thickness of +2cm from the lateral edge to the base of the flap (Figure 4B).
Split flaps:
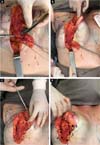
It starts with the demarcation from the “D” to the subcutaneous tissue and subsequent detachment of the skin with a dermofat flap of approximately 2cm, following a plane below the lipolaser and close to the breast parenchyma to the anterior axillary line and medially to the parasternal line. We continued with constructing a subglandular pocket, preserving the parenchyma implantation at point B and following the AB line to the second costal arch superiorly, avoiding wide detachment and thus creating only a central tunnel, maintaining the medial implantation of the breast. After gland release, we started making bipartite flaps, using the “D” arch to define the beginning of the perpendicular dissection up to the muscle fascia, thus preserving the “D” arch and decorticated in the medial flap (Figures 4C, D and E).
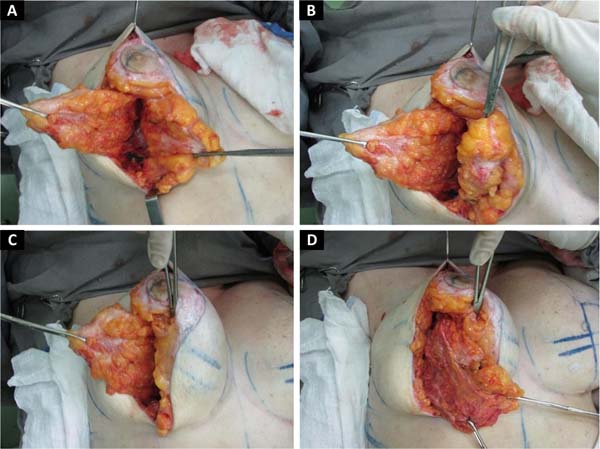
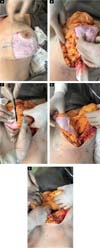
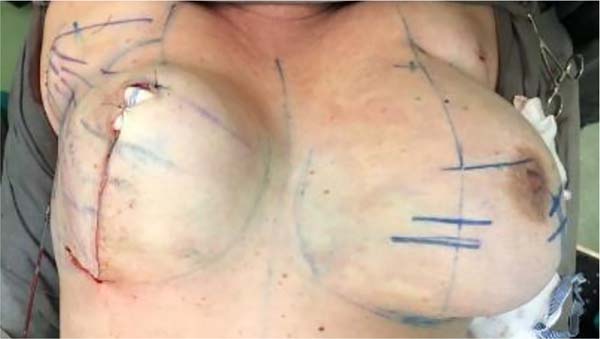
Mounting:
The medial flap is folded over itself, supero medially. Keeping the insertion of the parenchyma at point B (Figures 5A,5B and 5C). The lateral flap is pulled medially inferiorly, towards the xiphoid appendix (Figure 5D). All parenchyma beyond the AB line is resected; we continue with the inferolateral resection, thus creating the new inframammary fold.
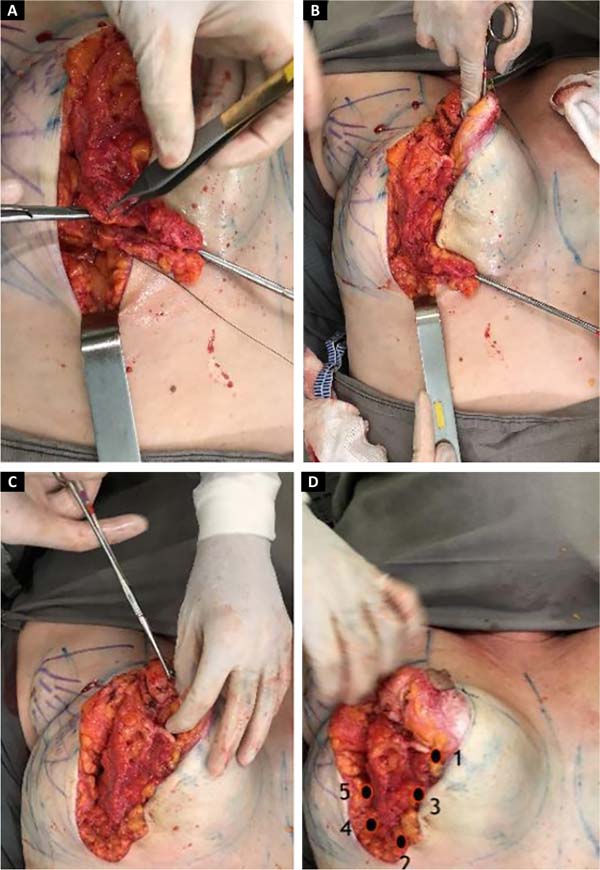
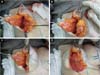
The medial flap will be the same on both sides, and the lateral flap will vary upon resection, depending on previous breast asymmetry; resected in bands (Figures 6A and 6B).
Sutures with five fixation points:
Suture of the breast parenchyma is performed with 2.0 mononylon thread, joining the stitches with inferomedial traction of the lateral portion for medialization of the same:
First point: approaching the medial pillars and lateral at the junction of points CD, (beginning of the column);
Second point: keeping the medial traction, joining the parenchyma with the fascia of the m. serratus at point B level coinciding with the beginning of the inframammary fold (end of the spine);
Third point: performed on the middle of the AB line between the first and second points, used for lateral support of the spine;
Fourth and fifth points: fixing the lateral parenchyma with the muscle fascia, defining the end of the new inframammary fold (Figure 6).
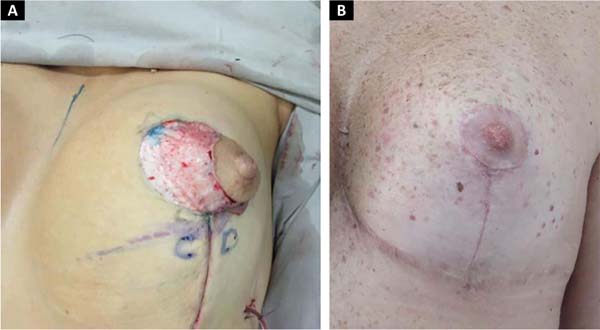
After fixation, closure is continued by planes, mononylon 3.0 superficial parenchyma, colorless mononylon 4.0 subcutaneous and, finally, intradermal with 4.0 monocryl (Figure 7).
Areola marking:
The junction of points C and D will coincide with the lower edge of the new positioning of the areola and the beginning of the vertical scar (Figure 8).
Areola suture in two planes, subcutaneous with mononylon 4-0 colorless and intradermal with monocryl 4.0.
RESULTS
Surgical revision was not required in any of the cases presented. There was no occurrence of post-surgical infection or necrosis of the papillary areolar plaque and the scar.
There were 5 cases of epidermolysis of the papillary areolar plaque, successfully treated with flavonoids and horse chestnut (linfa cream - Claremom), without sequelae.
The average resection of the parenchyma was 477.1g ranging from 80 to 1100g.
The amount of liposuction (LAL) was on average 438.6ml between 150 to 790ml.
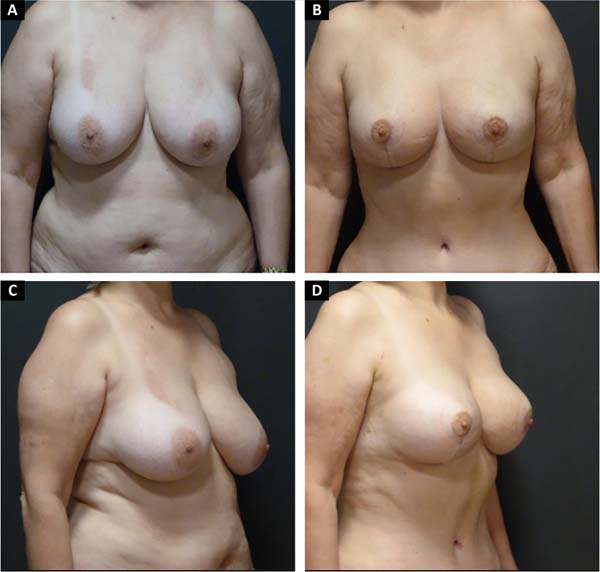
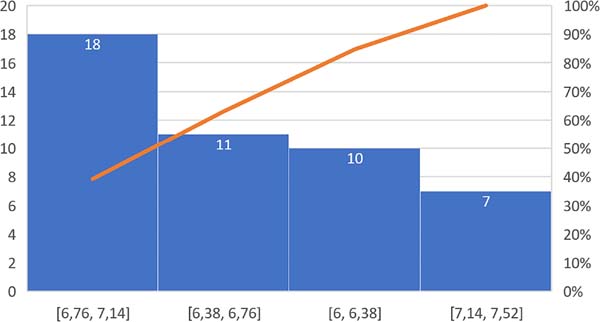
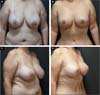
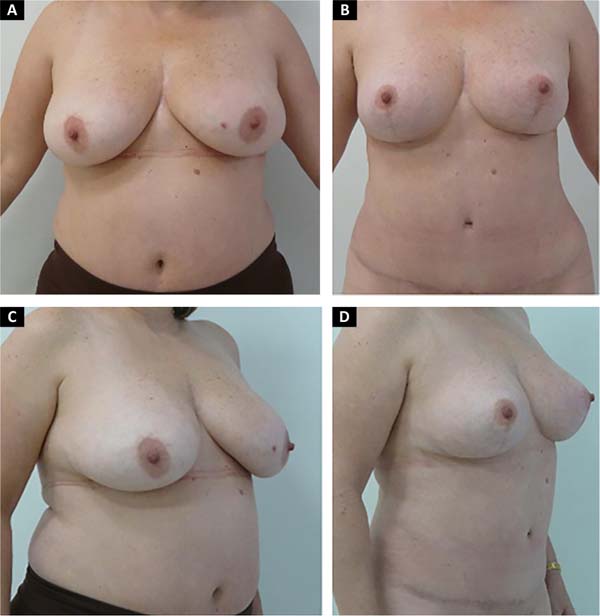
The length of the vertical scar was stable at an average of 6.7 cm (between 6.1-7.5) after two years (Figure 9).
The results with this technique were considered satisfactory, validated with the Breast-QTM questionnaire, reduction/mastopexy module (pre and postoperative), the evaluation percentages were described in Table 3.
Currently, the combination with laser is used in all our breast procedures and body treatment (abdomen, buttocks, arms, thighs and face/submental). Its combination brought us greater benefits in terms of surgical time and results (Figures 2, 10 and 11).
| Postoperative module | Very satisfied | 88% |
|---|---|---|
| Result of your surgery | I totally agree | 72% |
| How do you feel after surgery | All the time | 82% |
| How often do you feel | Most of the time | 83% |
| Last two weeks | in no time | 96% |
| Information obtained from your surgeon | Very satisfied | 74% |
| Satisfaction | Very satisfied | 86% |
| About your plastic surgeon | Completely agree | 73% |
| About the medical team | Completely agree | 92% |
| Office professionals | Completely agree | 92% |
DISCUSSION
The mirrored “D” technique has been used for 15 years, showing benefits such as reducing the tension of the papillary areolar plate (PAP) and, mainly, parallel vertical scars7,8. With the association of laser liposuction since 2015, with an improvement in the definition of the inframammary fold and a reduction in breast changes.
Its aesthetic results with smaller scars regardless of breast size, with an average final vertical scar of 6.7cm after two years of follow-up, and a reduction in breast ptosis recurrences, strengthen what has been described in the literature.
The degree of patient satisfaction was an important benefit for the advancement of the technique, especially concerning harmony, homogeneous skin retraction and better breast contour. The maintenance of the results was longer lasting when compared to the results obtained with other vertical scar techniques previously performed in our service, with a degree of satisfaction of very satisfied, representing 86% in the questionnaire applied (Breast-QTM).
Statistically combined surgeries present greater complications compared to isolated surgeries, which is a controversy among authors. With the mirrored “D” technique, we found a significant reduction in complications, especially in surgical revision, compared to 54% found in the literature4, an important factor that favored the evolution, maintenance and indication of the technique.
The amount of energy applied in the wrong way in the same place can produce direct damage to the fat and skin tissue. In our experience, we recommend not using more than 4000J per region. The poor clinical indication of energy (LAL) in the different areas and the surgeon’s lack of experience and learning in performing the laser could bring serious complications, which can be prevented. And it is also important to have a good evaluation of the fat tissue, its diameter, and the quality and type of skin in the region to be treated.
CONCLUSION
The mirrored “D” technique proved to be a good surgical option due to its versatility in different mammoplasty scenarios.
Its ease of execution has increased its indications for all types of breast ptosis, primary or secondary mammoplasty, with or without implants.
The combination of the mirrored “D” technique with laser-assisted liposuction is a procedure that is considered routine in our surgical planning every day—resulting in significant homogeneous skin retraction, favoring the conical shape of the breast, and maintaining the validated results.
REFERENCES
1. Sociedade Brasileira de Cirurgia Plástica (SBCP). Censo 2018 - Análise comparativa das pesquisas 2014, 2016 e 2018 [Internet]. São Paulo: SBCP; 2018. Disponível em: http://www2.cirurgiaplastica.org.br/wp-content/uploads/2019/08/Apresentac%CC%A7a%CC%83o-Censo-2018_V3.pdf
2. Souza Pinto EB, Erazo I, Muniz AC, Prado Filho FS, Alves MA, Salazar GH. Breast reduction: shortening scars with liposuction. Aesthetic Plast Surg. 1996 Nov/Dez;20(6):481-8.
3. Spear SL. Augmentation/mastopexy: surgeon, beware. Plast Reconstr Surg. 2006;118(Supl 7):133S-5S.
4. Spear SL, Pelletiere CV, Menon N. One-stage augmentation combined with mastopexy: aesthetic results and patient satisfaction. Aesthetic Plast Surg. 2004 Set/Out;28(5):259-67.
5. Cárdenas-Camarena L, Ramírez-Macías R. Augmentation/mastopexy: how to select and perform the proper technique. Aesthetic Plast Surg. 2006 Jan/Fev;30(1):21-33.
6. Sabino Neto M, Demattê MF, Freire MAMS, Garcia EB, Quaresma M, Ferreira LM. Self-esteem and functional capacity outcomes following reduction mammaplasty. Aesthet Surg J. 2008;28(4):417-20.
7. Sbalchiero JC, Cordanto-Nopoulos FR, Silva CHD, Caiado Neto BR, Derchain S. Tradução do questionário Breast-Q para a língua portuguesa e sua aplicação em mulheres com câncer de mama. Rev Bras Cir Plást. 2013;28(4):549-52.
8. Andrade AC. Breast-Q® na avaliação de resultados da mamoplastia redutora [dissertação]. São Paulo (SP): Universidade Federal de São Paulo (USP) - Escola Paulista de Medicina; 2015.
9. Apfelberg DB, Rosenthal S, Hunstad JP, Achauer B, Fodor PB. Progress report on multicenter study of laser-assisted liposuction. Aesthetic Plast Surg. 1994;18(3):259-64.
10. Apfelberg DB. Results of multicenter study of laser-assisted liposuction. Clin Plast Surg. 1996 Out;23(4):713-9.
11. Katz B, McBean J. Laser-assisted lipolysis: a report on complications. J Cosmet Laser Ther. 2008 Dez;10(4):231-3.
12. Badin AZED, Gondek LBE, Garcia MJ, Garcia MJ, Valle LC, Flizikowski FBZ, et al. Analysis of laser lipolysis effects on human tissue samples obtained from liposuction. Aesthetic Plast Surg. 2005;29:281-6.
13. Goldman A. Submental Nd:YAG laser-assisted liposuction. Lasers Surg Med. 2006 Mar;38(3):181-4.
14. Goldman A, Gotkin RH. Laser-assisted liposuction. Clin Plast Surg. 2009 Abr;36(2):241-53.
15. Badin AZD, Moraes LM, Gondek L, Chiaratti MG, Canta L. Laser lipolysis: flaccidity under control. Aesthetic Plast Surg. 2002 Set/Out;26(5):335-9.
16. Parlette EC, Kaminer ME. Laser-assisted liposuction: here’s the skinny. Semin Cutan Med Surg. 2008 Dez;27(4):259-63.
17. Sun Y, Wu SF, Yan S, Shi HY, Chen D, Chen Y. Laser lipolysis used to treat localized adiposis: a preliminary report on experience with Asian patients. Aesthetic Plast Surg. 2009 Set;33(5):701-5.
18. Reynaud JP, Skibinski M, Wassmer B, Rochon P, Mordon S. Lipolysis using a 980nm diode laser: a retrospective analysis of 534 procedures. Aesthetic Plast Surg. 2009 Jan;33(1):28-36.
19. Rocha RP, Pinto EBS, Saldanha OR, Rocha ELP, Missel J. Estudo histológico da derme humana de interesse para a lipoaspiração. Rev Bras Cir Plást. 2005;20(1):17-21.
20. Jecan CR, Hernic AD, Tianu EC, Florescu IP, Lascar I. Histological differences between laser-assisted and suction-as- sisted lipoplasty aspirates—a comparative study. Rom J Morphol Embryol. 2015;56(Supl 2):S797-S801.
21. Kim KH, Geronemus RG. Laser lipolysis using a novel 1064 nm Nd:YAG laser. Dermatol Surg. 2006 Fev;32(2):241-8.
22. DiBernardo BE, Reyes J, Chen B. Evaluation of tissue termal effects from 1064;1320-n laser assisted lipolysis and its clinical implications. J Cosmet Laser Ther 2009;11(2):62-9.
23. Wolfenson M, Hochman B, Ferreira LM. Laser lipolysis: skin tightening in lipoplasty using a diode laser. Plast Reconstr Surg. 2015 Mai;135:1369-77.
24. Yoo KW, Bae JM, Won CY, Chung YS, Goo B, Rho YK, et al. Laser-assisted liposuction using the novel 1,444-nm Nd:YAG laser for the treatment of gynecomastia: a pilot study. Dermatology. 2015;231(3):224-30. DOI: https://doi.org/10.1159/000430494:2015
25. Mordon S, Blanchemaison PH. Histologic evaluation of interstitial lipolysis comparing a 1064, 1320 and 2100 nm laser in an ex vivo model. Lasers Surg Med. 2008 Out;40(8):519.
26. Reszko AE, Magro CM, Diktaban T, Sadick NS. Histological comparison of 1064 nm Nd:YAG and 1320 nm Nd:YAG laser lipolysis using an ex vivo model. J Drugs Dermatol. 2009 Abr;8(4):377-82.
27. Mordon S, Eymard-Maurin AF, Wassmer B, Ringot J. Histologic evaluation of laser lipolysis: pulsed 1064-nm Nd:YAG laser versus CW 980-nm diode laser. Aesthetic Surg J. 2007;27(3):263-8.
28. Khoury JG, Saluja R, Keel D, Detwiler S, Goldman MP. Histologic evaluation of interstitial lipolysis comparing a 1064, 1320, and 2100 nm laser in an ex vivo model. Lasers Surg Med. 2008 Ago;40(6):402-6.
29. Ichikawa K, Miyasaka M, Tanaka R, Tanino R, Mizukami K, Wakaki M. Histologic evaluation of the pulsed Nd:YAG laser for laser lipolysis. Lasers Surg Med. 2005 Jan;36(1):43-6.
30. Sanchéz J, Carvalho AC, Erazo P. Mastoplasty with prosthesis: the mirror D technique. Rev Bras Cir Plást. 2008;23(3):200-6.
31. López JCS, Erazo P. Secondary mastopexy with exchange of prosthesis: mirror “D” technique. Rev Bras Cir Plást. 2018;33(3):324-32.
1. Juan Sánchez Clinic, São
José dos Campos, SP, Brazil.
2. Plastic Surgery Clinic Dr. Patricia J. Erazo,
Santos, SP, Brazil.
JCS Analysis and/or data interpretation, Conception and design study, Data Curation, Final manuscript approval, Investigation, Methodology, Project Administration, Realization of operations and/or trials, Resources, Supervision, Validation, Visualization, Writing - Original Draft Preparation, Writing - Review & Editing.
PJE Analysis and/or data interpretation, Conception and design study, Data Curation, Final manuscript approval, Formal Analysis, Investigation, Methodology, Project Administration, Realization of operations and/or trials, Supervision, Writing - Original Draft Preparation, Writing - Review & Editing.
PSLZ Data Curation, Formal Analysis, Investigation, Project Administration.
Corresponding author: Patricia Jacqueline Erazo, Rua Santa Clara nº 1035, Vila adyana, São José dos Campos, SP, Brasil, Zip Code 12243 630, E-mail: p.erazo@uol.com.br
Article received: April 22, 2020.
Article accepted: July 14, 2021.
Conflicts of interest: none.
Institution: Hospital Antoninho da Rocha Marmo, São José dos Campos, SP, Brazil.









 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter