

Original Article - Year 2020 - Volume 35 -
Evaluation of the use of tissue expander in a university service
Avaliação do uso de expansor de tecido em um serviço universitário
ABSTRACT
Introduction: Tissue expansion is an important reconstruction method to solve defects such as burns and giant nevi or breast reconstruction. This article aims to report the experience of the Plastic Surgery Service of the Hospital de Clínicas of the Federal University of Paraná (UFPR) with the use of expanders.
Methods: This is a retrospective, descriptive, and analytical study of patients who underwent tissue expansion for reconstructive surgery at the Hospital de Clínicas da UFPR, from January 2010 to December 2016.
Results: 61 patients and 80 surgeries were analyzed, including re-expansion procedures. Age ranged from 2 to 73 years (mean 31). The majority of patients were female (83.6%), aged over 40 years, undergoing breast reconstruction treatment after radical mastectomy (36%). The complications observed in these patients were: signs of infection (14.7%), suture dehiscence (3.2%), seroma (3.2%), defect in the expander (3.2%), exposure of the expander (3, 2%), necrosis (1.6%) and signs of hypoperfusion (1.6%). Patients undergoing breast reconstruction had the highest number of complications (40.1%). Reexpansion was necessary for 37.7% of patients.
Conclusion: The skin expansion technique is indicated for several pathologies' treatment. The tissue expansion procedure has high complication rates. Knowing the patient's profile, the main types of complications, and the factors associated with these complications can help prevent them.
Keywords: Devices for tissue expansion; Tissue expansion; Mammoplasty; Pigmented nevus; Burns.
RESUMO
Introdução: Expansão tecidual é um método de reconstrução importante para a cobertura de
defeitos como queimaduras e nevos gigantes ou na reconstrução mamária. Esse
artigo tem como objetivo relatar a experiência do Serviço de Cirurgia
Plástica do Hospital de Clínicas da Universidade Federal do Paraná (UFPR)
com o uso de expansores.
Métodos: Esse é um estudo retrospectivo, descritivo e analítico dos pacientes que
foram submetidos à expansão tecidual para cirurgia reconstrutora no Hospital
de Clínicas da UFPR, entre o período de janeiro de 2010 a dezembro de
2016.
Resultados: Foram analisados 61 pacientes e 80 cirurgias, incluindo os procedimentos de
reexpansão. A idade variou entre 2 a 73 anos (média 31). A grande maioria
dos pacientes pertenceu ao sexo feminino (83,6%), na faixa etária acima de
40 anos, sendo submetidos ao tratamento para reconstrução mamária após
mastectomia radical (36%). As complicações observadas nesses pacientes
foram: sinais de infecção (14,7%), deiscência da sutura (3,2%), seroma
(3,2%), defeito no expansor (3,2%), exposição do expansor (3,2%), necrose
(1,6%) e sinais de hipoperfusão (1,6%). Pacientes submetidos à reconstrução
mamária tiveram o maior número de complicações (40,1%). A reexpansão foi
necessária em 37,7% dos pacientes.
Conclusão: A técnica de expansão de pele é indicada para o tratamento de diversas
patologias. O procedimento de expansão tecidual apresenta taxas de
complicações altas e o conhecimento do perfil do paciente, dos principais
tipos de complicações e dos fatores associados a essas complicações podem
auxiliar na sua prevenção.
Palavras-chave: Dispositivos para expansão de tecidos; Expansão de tecido; Mamoplastia; Nevo Pigmentado; Queimaduras
INTRODUCTION
Tissue expansion is the technique that allows the reconstruction of defects by the gradual distension of a flexible skin area, preparing it for use in solving any defect such as breast reconstruction, burns, and giant nevi1. This reconstructive method has advantages such as the use of tissues of color and texture similar to the defect, less damage to the donor area, and aesthetic improvement.
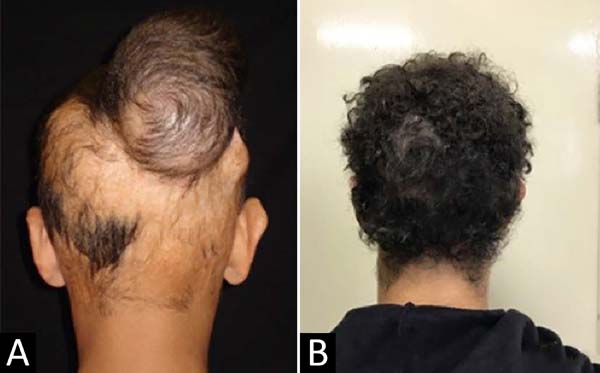
In burns, tissue expansion is indicated when the wounds have completely healed, and the resulting scars need to be treated. Patients with burn sequelae may have limited tissue availability for flaps. Specific areas such as the scalp benefit from tissue expansion by allowing the treatment of sequelae with similar tissue2 (Figure 1), as well as the head and neck region. The expansion can be done in tissues surrounding the wound, or donor areas of free flaps in situations that nearby regions are not available3.
Giant congenital nevus can be defined as an ectopic concentration of melanocytes of neuroectodermal origin with a diameter greater than 20 cm and affecting about 1 in every 20,000 live births4. Besides the aesthetic implications, patients with this type of anomaly need to deal with 5 to 12% associated risk of malignancy. Therefore, prophylactic excision is recommended4. The use of tissue expanders is frequent in this treatments5.
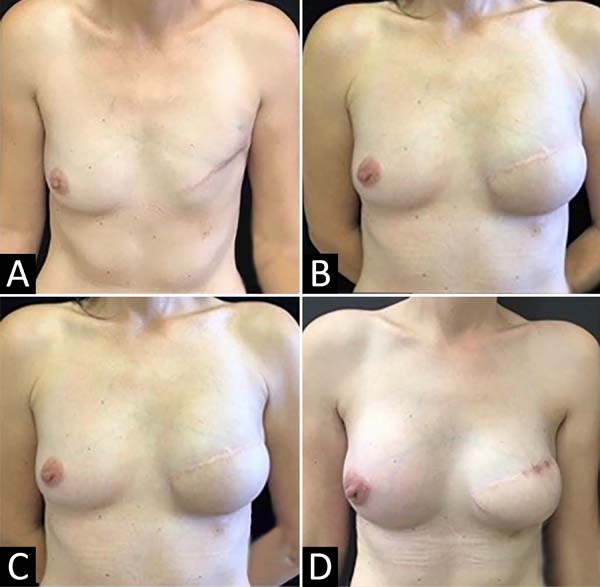
The number of procedures involving skin expanders for breast reconstruction has also been increasing. Statistics from the American Society of Plastic Surgeons, in 20166, show that approximately 90% of breast reconstructions with prostheses are performed in two stages, the first of which is tissue expansion (Figure 2). The use of expanders may also be required in breast agenesis. In Poland’s syndrome, there is a partial or total absence of the pectoralis major, pectoralis minor, serratus and breast muscles, and the nipple-areola complex; therefore, expansion is one of the techniques used in its treatment7
OBJECTIVE
This article has as main objective to report the experience of the plastic surgery service at the Hospital de Clínicas of the Federal University of Paraná (UFPR) with the use of expanders, emphasizing the complications found, their possible causes and management.
METHODS
This is a retrospective, descriptive, and analytical study of patients who underwent tissue expansion for reconstructive surgery at Hospital de Clínicas da UFPR. This study was submitted and approved by the Ethics and Research Committee of the Hospital de Clínicas da UFPR (approval number: 68550217.4.0000.0096).
Medical records of patients who underwent expansion between January 2010 and December 2016 were analyzed. All patients who underwent surgery for tissue expansion during this period were included. Exclusion criteria included the abandonment of treatment and the death of the patient during this period. The data obtained were age, gender, pathology indicative of the procedure, type of expander, insertion site, evolution, and complications.
From the data obtained, a descriptive statistical analysis was carried out, emphasizing the relationship between the complications found and parameters, such as the cause of treatment, the format of the expander, and the insertion site.
RESULTS
Sixty-one patients and 80 surgeries, including reexpansion procedures, were analyzed. The majority of patients were female (83.6%). The age at the first surgical stage of the patients analyzed was between 2 and 73 years (mean 31), with the majority in the age group above 40 years (41%), followed by young people between 11 and 20 years (27.9%). The main indication for surgery was breast reconstruction after mastectomy (36%), followed by a burn scar correction (31.1%) and giant nevi correction (14.7%). Other causes include post-trauma scar correction (6.6%), vascular malformation correction (4.9%), breast agenesis due to Poland’s syndrome (3.3%), microtia (1.6%), and resection of dermofibrosarcoma (1.6%).
Concerning the complications most seen in the procedures performed, signs of infection (14.7%) stand out. Other complications observed were: suture dehiscence (3.2%), seroma (3.2%), expander defect (3.2%), expander exposure (3.2%), necrosis (1.6%) and signs of hypoperfusion (1.6%).
Patients undergoing breast reconstruction had the highest number of complications. Considering the 22 patients who received treatment, four presented, in the first stage, infectious signs in the breast where the expander was placed, and another four presented the following complications each: exposure of the expander, dehiscence of the suture, seroma and signs of hypoperfusion. In five cases, it was necessary to remove the expander. Patients suffering from seroma, and exposure only needed to relocate the expanders. One of the patients died due to cancer complications.
Among patients undergoing expansion to correct burns, two showed signs of infection after surgery. Two others presented complications due to suture dehiscence and one due to defect in the expander. They all required the removal of the expander. Forty percent of the complications in patients with burn sequelae were in the lower limbs. The other correlations between the cause of treatment and the percentage of complications are shown in Table 1.
| Etiology | Number of patients | % Total | Number of complications | % Complications |
|---|---|---|---|---|
| Breast reconstruction | 22 | 36 | 9 | 40.1 |
| Burn sequel | 19 | 31.1 | 5 | 26.3 |
| Giant Nevus | 9 | 14.7 | 3 | 33.3 |
| Post-trauma scar sequel | 4 | 6.6 | 1 | 25.0 |
| Vascular malformation | 3 | 4.9 | 1 | 33.3 |
| Poland syndrome | 2 | 3.3 | 1 | 50.0 |
| Dermatofibrosarcoma resection | 1 | 1.6 | 1 | 100.0 |
| Microtia | 1 | 1.6 | 0 | 0 |
* If the same patient performed more than one surgery, the number of complications was counted in all procedures.
The chest region was associated with a higher number of complications than other parts of the body: 11 of the 28 patients who underwent the procedure in this region had some type of complication. The other correlations between the anatomical region submitted to expansion and complications are shown in Table 2.
| Anatomical region | Number of patients | % Total number of patients | Number of complications | % |
|---|---|---|---|---|
| Complications | ||||
| Chest | 28 | 45.9 | 11 | 39.3 |
| Lower limbs | 9 | 14.8 | 3 | 33.3 |
| Scalp | 9 | 14.8 | 2 | 22.2 |
| Face | 8 | 13.1 | 2 | 25.0 |
| Back | 7 | 11.5 | 1 | 14.3 |
| Abdomen | 2 | 3.3 | 0 | 0 |
| Upper limbs | 1 | 1.6 | 0 | 0 |
| Neck | 1 | 1.6 | 1 | 100.0 |
Regarding age, the greatest number of complications occurred in patients over 40 years of age. In this group, 36% had some type of complication (Table 3).
| Age (years) | Number of patients | % Total | Number of complications | % of Complications |
|---|---|---|---|---|
| 0-10 | 9 | 14.8 | 3 | 33.3 |
| 11-20 | 17 | 27.9 | 5 | 29.4 |
| 21-30 | 6 | 9.8 | 0 | 0 |
| 31-40 | 4 | 6.6 | 1 | 25.0 |
| >40 | 25 | 41.0 | 9 | 36.0 |
Reexpansion was necessary for 37.7% of patients. Of the 19 surgeries performed on these patients for reexpansion, two had complications. One of the patients who underwent breast reconstruction showed signs of infection, while the second surgery of a patient with a giant nevus had the expander’s exposure.
The majority of patients started the expansion during the intraoperative period (95%), and the time of evolution varied from 0 to 168 months, with an average of 58.9 months.
Table 4 shows the number of complications concerning the year.
| Year of surgery | Number of surgeries | Number of complications | % of complications |
|---|---|---|---|
| 2010 | 8 | 3 | 37.5 |
| 2011 | 11 | 2 | 18.2 |
| 2012 | 17 | 4 | 17.6 |
| 2013 | 17 | 4 | 23.5 |
| 2014 | 14 | 3 | 21.4 |
| 2015 | 7 | 2 | 28.6 |
| 2016 | 6 | 3 | 33.3 |
| Total | 80 | 21 |
DISCUSSION
In the mid-1950s, Neumann was the first surgeon to use an expander implant through a latex balloon to enlarge the periauricular region after an ear trauma8. Since then, skin expanders have been used for the most diverse procedures.
In terms of shape, an expander follows three patterns: round, rectangular, and semi-lunar (croissant). The rectangular is known for allowing additional tissue expansion, thus increasing the options for flap design. The valve can be integrated into the expander or attached via a silicone tube.
The content of the expanders available on the market is almost always a saline solution. Another option found is filling with carbon dioxide, recently approved by the “US - Food and Drug Administration (FDA)” 9.
In the Plastic Surgery Service of Hospital de Clínicas da UFPR, the three types of expanders are used, the round one being recommended in breast reconstructions and the croissant and rectangular types most used in other types of surgery, such as treating burn sequelae, for example. The contents of these expanders have always been a saline solution.
A critical point to be defined in the preoperative period is the expansion design. Attention should be paid to the donor site as infections, trauma, and unstable scarring can lead to implant failure or extrusion. The incision site must also be chosen with caution. For example, if the goal is to remove an injury, it is appropriate to position the incision at the edges of the injury.
The majority of expansions begin during the intraoperative period, when a volume is placed making a slight compression to avoid the hematoma formation, since in most cases - except for breast reconstruction - a vacuum suction drain is not used. Although there are many citations in the literature to start the expansion in one to three weeks after the expander is inserted, in our service, the scar is expected to mature more, and tissue expansion begins in about four weeks. If there are no complications, weekly expansion is performed, until the required volume is reached. The use of state-of-the-art or osmotic expanders with self-inflating expansion may eliminate the need for repeated injections, reducing the number of infections and other complications10. However, there are still no such devices commercially available in our market11.
The profile of patients, the number of surgeries, and the number of complications have changed in our department in recent decades if we compare it with a study by Freitas et al., from 2011. In the period from January 2005 to December 2009, most of these patients were in their second decade of life and underwent expansion due to burning sequelae. In the present study, we found a prevalence of women over the fourth decade of life undergoing breast reconstruction treatment after radical mastectomy, with the old profile of patients in the second position. This change in profile is consistent with the worldwide increase in the number of breast reconstruction procedures with prostheses performed in two stages, the first of which is tissue expansion6. In proportion to the number of surgeries performed in the last decades12, the number of complications has decreased.
In patients undergoing radical mastectomy for cancer treatment, a significant challenge is a need for post-surgical radiation. Radiation leads to fibrosis, which compromises the quality of the skin and subcutaneous tissue, resulting in higher incidences of complications and possibly impairing the final aesthetic result13. These complications may conduct to the need of the radiotherapy treatment interruption, thus compromising the final result. In other situations, it may be necessary to deflate the expander to allow adequate access to the chest wall and internal mammary lymph nodes.
In burns, the most common complications are infection, exposure, and expander malfunction. According to Bozkurt et al., N 200814, the highest number of complications in these patients occurs in the head region, and when using larger expansion volumes (400 and 800ml). However, the results obtained in this research are in line with LoGiudice and Gosain (2003)15, with more significant complications in the lower limbs, possibly due to less rich vascularization and the amount of tissue available region.
The highest incidence of complications with the age group is found in patients over 40 years old and those between 11 to 20 years old, coinciding with the age groups with the highest prevalence in patients after radical mastectomy and burn sequelae.
It is essential to know the types of complications, frequency, and associated factors to minimize them. Besides, the choice of the best expander option and the correct surgery technique and expansion are essential for a good result. The future of the skin expansion technique is auspicious. The increase in the number of studies observed in the last decades on expansion, not only of skin but also of nerves, bones, and other parts of the body, can be of great value to surgeons in the future16.
CONCLUSION
The skin expansion technique is indicated for several pathologies’ treatment. Besides, the patient profile treated at the Hospital de Clínicas da UFPR has changed in the last decades. Since 2010, there has been an increase in the number of patients who underwent treatment for breast reconstruction, exceeding the number of patients due to burning sequelae who underwent the same procedure. Most of the complications observed in these patients were infections related to the insertion of expanders in the chest region to perform the breast reconstruction procedure.
REFERENCES
1. Di Mascio D, Castagnetti F, Mazzeo F, Caleffi E, Dominici C. Overexpansion technique in burn scar management. Burns. 2006 Jun;32(4):490-8.
2. Tavares Filho JM, Belerique M, Franco D, Porchat CA, Franco T. Tissue expansion in burn sequelae repair. Burns. 2007 Abr;33(2):246-51.
3. Barret JP. ABC of burns: burns reconstruction. BMJ. 2004;329(7460):274-6.
4. Paschoal FM. Nevo melanocítico congênito. An Bras Dermatol. 2002 Nov/Dez;77(6):649-58.
5. Viana ACL, Gontijo B, Bittencourt FV. Giant congenital melanocytic nevus. An Bras Dermatol. 2013 Nov/Dez;88(6):863-78.
6. American Society of Plastic Surgeons (ASPS). Plastic surgery statistics [Internet]. Arlington Heights, IL: ASPS; 2016; [acesso em 2017 Abr 01]. Disponível em: https://www.plasticsurgery.org/news/plastic-surgery-statistics?sub=2016+Plastic+Surgery+Statistics
7. Araujo MP, Araujo AJ. Sindrome de Moebiüs-Poland: relato de caso. Rev Med. 1999;78(3):371-7.
8. Ashley KL, Bruce SB. Tissue expansion. In: Thorne CH, ed. Grabb and Smith’s Plastic Surgery. Philadelphia, PA: Lippincott Wilians Wilkins; 2013. p. 512-40.
9. Ascherman JA, Zeidler K, Morrison KA, Appel JZ, Berkowitz RL, Castle J, et al. Carbon dioxide-based versus saline tissue expansion for breast reconstruction: results of the XPAND prospective, randomized clinical trial. Plast Reconstr Surg. 2016 Dez;138(6):1161-70.
10. Chummun S, Addison P, Stewart KJ. The osmotic tissue expander: a 5-year experience. J Plast Reconstr Aesthet Surg. 2010 Dez;63(12):2128-32.
11. Pitanguy I, Radwanski HN, Amorim NFG, Lintz JE, Moraes Neto AEM. The use of tissue expanders in burn sequelae. Acta Med Misericordia. 2000;2(3):59-64.
12. Freitas RS, Oliveira e Cruz GA, Scomação I, Nasser IJG, Colpo PG. Tissue expansion at Hospital de Clínicas-UFPR: our experience. Rev Bras Cir Plást. 2011 Set;26(3):407-10.
13. Nano MT, Gill PG, Kollias J, Bochner MA, Malycha P, Winefield HR. Psychological impact and cosmetic outcome of surgical breast cancer strategies. ANZ J Surg. 2005 Nov;75(11):940-7.
14. Bozkurt A, Groger A, O’Dey D, Vogeler F, Piatkowski A, Fuchs PCH, et al. Retrospective analysis of tissue expansion in reconstructive burn surgery: evaluation of complication rates. Burns. 2008;34(8):1113-8.
15. LoGiudice J, Gosain AK. Pediatric tissue expansion: indications and complications. J Craniofac Surg. 2003 Nov;14(6):866-72.
16. Wood RJ, Adson MH, Van Breek AL, Peltier GL, Zubkoff MM, Bubrick MP. Controlled expansion of peripheral nerves: comparison of nerve grafting and nerve expansion/repair for canine sciatic nerve defects. J Trauma. 1991 Mai;31(5):686-90.
1. Hospital de Clínicas, Federal University
of Paraná, Curitiba, PR, Brazil.
KKTR Analysis and/or data interpretation, Conception and design study, Conceptualization, Data Curation, Final manuscript approval, Formal Analysis, Investigation, Methodology, Project Administration, Realization of operations and/or trials, Software, Validation, Visualization, Writing - Original Draft Preparation, Writing - Review & Editing
MCCO Analysis and/or data interpretation, Conception and design study, Conceptualization, Data Curation, Final manuscript approval, Formal Analysis, Funding Acquisition, Investigation, Methodology, Project Administration, Realization of operations and/or trials, Resources, Supervision, Validation, Visualization, Writing - Original Draft Preparation, Writing - Review & Editing
JRN Analysis and/or data interpretation, Conception and design study, Conceptualization, Data Curation, Formal Analysis, Investigation, Methodology, Writing - Original Draft Preparation, Writing - Review & Editing
IO Analysis and/or data interpretation, Conception and design study, Conceptualization, Methodology, Writing - Original Draft Preparation, Writing - Review & Editing
HCM Analysis and/or data interpretation, Conception and desig n study, Conceptualization, Software, Writing - Original Draft Preparation, Writing - Review & Editing
RSF Analysis and/or data interpretation, Conception and design study, Conceptualization, Data Curation, Final manuscript approval, Formal Analysis, Funding Acquisition, Investigation, Methodology, Project Administration, Realization of operations and/or trials, Resources, Supervision, Validation, Visualization, Writing - Original Draft Preparation, Writing - Review & Editing
Corresponding author: Kethelyn Keroline Telinski Rodrigues Avenida Presidente Getúlio Vargas ,1811, Apart. 41 , Rebouças, Curitiba, PR, Brazil. Zip Code: 80240-040, E-mail: kety.rodrigues@gmail.com
Article received: March 03, 2020.
Article accepted: July 15, 2020.
Conflicts of interest: none.







 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter