

Case Report - Year 2020 - Volume 35 -
Reverse frontal lifting: alternative for the treatment of pachydermoperiostosis
Lifting frontal reverso: alternativa para o tratamento da paquidermoperiostose
ABSTRACT
Introduction: Patient diagnosed with pachydermoperiostosis, presenting a strong cutaneous manifestation, making it impossible to correct the defect by the usual facial lifting techniques. The reverse frontal facelift was the idealized technique for this case. It is an innovative technique, there being no previous publication in the literature.
Case report: Italian male patient, 56 years old, with cutaneous manifestation syndrome, especially in the frontal region of the face, with leathery inelastic skin, which generated aesthetic discomfort, predisposing for a syndromic stigma.
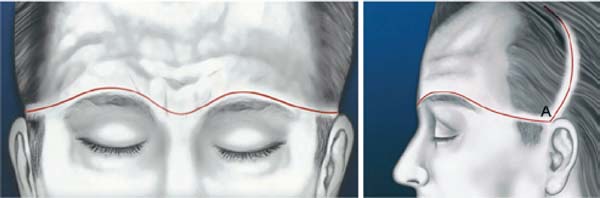
Methods: The technique developed for this case involves an incision, which starts at the root of the helix (point A), bypasses the eyebrow in a sinuous line distant half a centimeter from the implantation of the eyebrow hair, going to the glabella, curving towards the nasal root and going to meet identical dimensions on the other side. From point A, a curved line also leans towards the medial direction, at a distance of 2 cm. The intention is to reduce the distance between the area to be pulled and the incision area, in order to obtain more traction, thus enabling the correction of the aspect of the face in focus.
Results: Caudal traction of the flap by a supraciliary incision made it possible to correct the defect in the frontal region without altering the capillary implantation line or causing excessive eyebrow rise.
Conclusion: The reverse frontal lifting technique was created for a specific case of pachydermoperiostosis syndrome. When correctly indicated, this technique can be used to achieve good results.
Keywords: Face; Rhytidoplasty; Osteoarthropathy, Primary hypertrophic; Forehead; Surgery, Plastic.
RESUMO
Introdução: Paciente com diagnóstico de paquidermoperiostose, apresentando forte manifestação cutânea, impossibilitando a correção do defeito pelas técnicas usuais de lifting facial. O lifting frontal reverso foi a técnica idealizada para o caso. É uma técnica inovadora, não havendo publicação prévia na literatura.
Relato de caso: Paciente italiano, sexo masculino, 56 anos, apresentando síndrome de manifestação cutânea, em especial na região frontal da face, com pele inelástica de aspecto coriáceo, que gerava desconforto estético, ensejando um estigma sindrômico.
Métodos: A técnica elaborada para este caso envolve incisão, que se inicia na raiz da hélice (ponto A), contorna o supercílio em linha sinuosa distando meio centímetro da implantação dos pelos da sobrancelha, indo até a região da glabela, curvando para a raiz do nariz e indo se encontrar com dimensões idênticas do outro lado. Do ponto A, também ascende uma linha curva inclinando-se para o sentido medial, com uma distância de 2cm. A intenção é diminuir a distância entre a área a ser tracionada e a área de incisão, a fim de obter maior tração, possibilitando assim a correção do aspecto da face em foco.
Resultados: A tração caudal do retalho por incisão supraciliar possibilitou a correção do defeito em região frontal sem que houvesse alteração da linha de implantação capilar ou ascensão excessiva das sobrancelhas. Conclusão: A técnica de lifting frontal reverso foi criada para um caso específico de síndrome de paquidermoperiostose. Quando bem indicada esta técnica pode ser utilizada atingindo bons resultados.
Palavras-chave: Face; Ritidoplastia; Osteoartropatia hipertrófica primária; Testa; Cirurgia plástica
INTRODUCTION
Pachydermoperiostosis or Touraine-Solente-Golé syndrome is a rare inherited disease, predominant in males characterized by thickening of the skin (pachydermia), acropachy, periostosis of long bones, which may be associated with hyperhidrosis and seborrheic dermatitis1. Facial deformity is one of the main complaints of these patients, and surgical treatment is the best strategy for its correction. There are several surgical options, among which are conventional facelift techniques and local skin resections2.
Facelift techniques emerged in the early 20th century3. The first steps in the treatment of facial wrinkles were attributed to Charles Conrad Miller, due to his publication on the eradication of wrinkles, in which he proposed the subcutaneous section of the facial muscles4. Dissatisfied with the results of small skin extractions in front of the ear and on the edge of the scalp, Eugene Von Hollander, in 19015, was the first surgeon to perform a facelift using a long vertical incision in front of the ear and sideways to the neck3,4.
Later, Lexer at in 19316 suggested that the skin flaps be dissected in a subcutaneous plane. He was the first surgeon to perform an elevation of the frontal region7.
At the end of World War I, the high demand for repair surgeries was the basis for facelift. For instance, in 1926, Hunt8 described the coronal incision with resection of the scalp. Five years later, in 1931, Joseph9 reported using a capillary incision for the same purpose10. In 1960, Pagman et al.11 described frontal facelifts by a coronal incision in the hairline or the capillary insertion10.
From the 70’ onwards, greater emphasis is placed on technical refinements such as reduced scars, muscle manipulation, and musculoaponeurotic systems4. Skoog reported, in 197412, the elevation of the platysma of the neck and the lower third of the face without skin detachment4,7. This more profound dissection method, together with the description of the superficial aponeurotic muscular system (SAMS) by Mitz and Peyronie, in 197613, paved the way for modern facelift techniques3,10.
Pierce et al. em 194714 recognized the relationship between the corrugator muscles and vertical expression lines in the glabella area and advocated addressing these muscles through a supraciliary incision4. Castanhares, in 196415, proposed the resection of a cutaneous spindle by incision on the eyebrow to elevate the lateral portion10.
Many early frontal lifts involved resection of the skin on the forehead or scalp without weakening the strength of the frontal muscle. Regnault, in 197216, marked the frontal muscle; Skoog, in 197412 and Vinas et al., in 197617, defended the resection of the frontal strips to weaken the muscle10.
As in all scientific activities, the evolutionary process is continuous. Techniques and tactics continue to emerge, showing the importance of rhytidoplasties for the scene of plastic surgery4.
The case report, the object of this paper, has its peculiarity in the fact that it is a patient with syndromic facies, which presents a strong cutaneous manifestation, especially in the distal third in the frontal region, making it impossible to correct the defect using the usual facial lifting techniques, where the frontal flap is performed cranially. Therefore, it was necessary to make an atypical incision to help this European patient, who had emigrated to Brazil exclusively in an attempt to find treatment for his problem. Reverse frontal cosmetic surgery was the idealized surgical technique for the case. It is an innovative technique without prior publication in the literature.
CASE REPORT
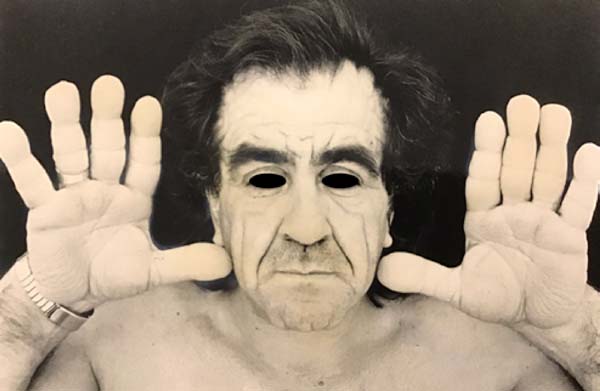
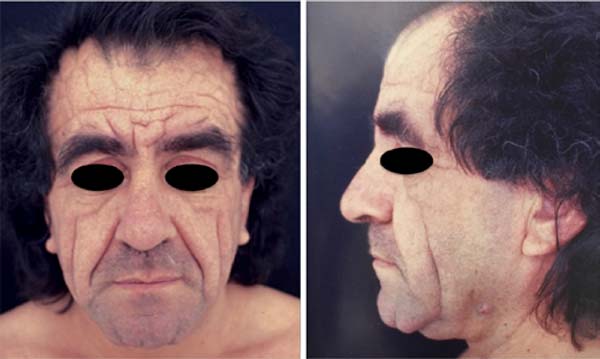
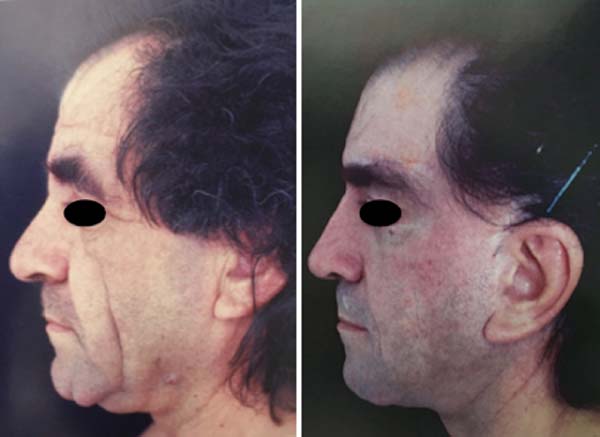
56-year-old Italian patient diagnosed with pachydermoperiostosis with thickening of the dermis and epidermis (pachydermia), acropachy, and periostosis (Figure 1). The cutaneous manifestation was more pronounced in the frontal region of the face with the presence of inelastic and redundant skin and with the formation of deep grooves, which generated aesthetic discomfort for the patient (Figure 2). Due to the characteristics of the skin and the distance from the coronal incision to the site to be treated, traction in the cranial direction would be ineffective. Therefore, an atypical facelift incision, called reverse frontal, was conceived, where the front flap is pulled in the caudal direction.
METHODS
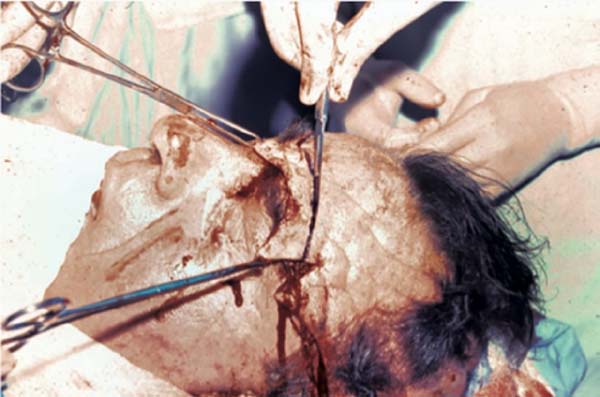
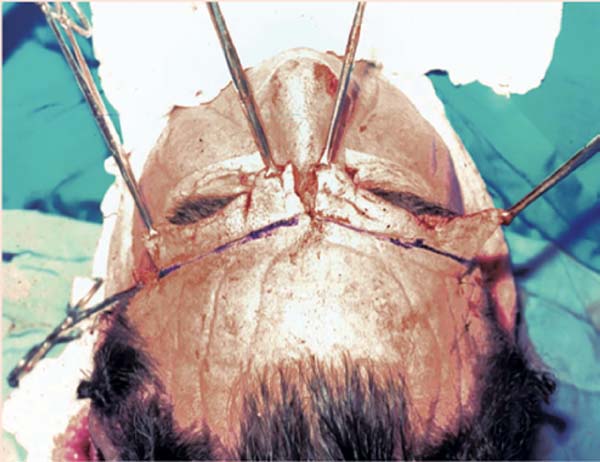
The incision begins at the root of the helix at point A, outlines the eyebrow in a sinuous line half a centimeter from the implantation of the eyebrow hairs, rises to the glabella region, curves towards the root of the nose, and it is found with identical dimensions on the other side (Figure 3). From point A, a curved line rises leaning towards the medial direction, at a distance of 2 cm, to allow a secure nutritional basis for the entire flap. The intention is to reduce the distance between the area to be pulled and the area of the incision, to obtain greater traction, thus allowing correction of the appearance of the face. After the incision, a cranial subgaleal detachment of the forehead was performed, and the frontal and interciliary muscles were treated. Flap traction is performed in the caudal (reverse) direction with subsequent marking and resection of the cutaneous excess in the frontal region, symmetrically, resulting in a supraciliary scar (Figures 4 and 5).
The middle and lower thirds of the face were treated through a pre-intracapillary, retroauricular, pre-auricular and pre-tragal MACE incision, reaching point A, with subsequent broad flap detachment, SAMS plication and medial platysma approach. Skin spindle resection was performed in the nasogenian grooves, which, being pronounced, required local traction following the same concept used in the upper third. A skin excision was performed on the submentum to treat excess skin in the mentonian region.
RESULTS
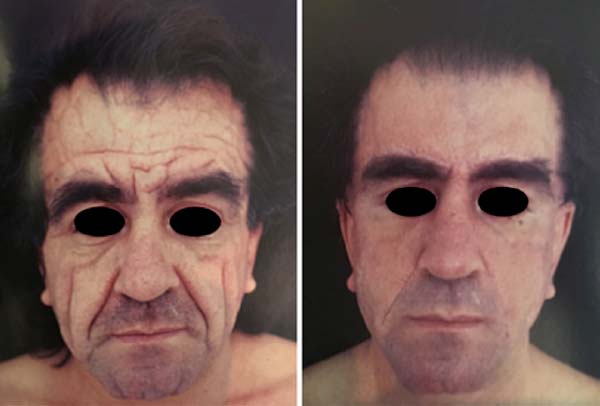
The caudal traction of the flap, made using a supraciliary incision, made it possible to correct the defect in the frontal region without altering the capillary implantation line or producing excessive eyebrow rise. The treatment of the middle and lower thirds of the face, added to the resection of the skin spindle in the nasogenian groove and submentum, also allowed the rejuvenation of the face in a broad aspect and the smoothing of the grooves (Figures 6 and 7).
However, preoperative counseling is essential so that the patient becomes aware that the scars will become more apparent, but are necessary to obtain a more effective result.
DISCUSSION
There is still no consensus for the treatment of frontal and nasoglabelar wrinkles, and the best surgical option for patients diagnosed with pachydermoperiostosis has not been established. Endoscopic lifting is one of the most used techniques because it has reduced surgical time and less apparent scarring. However, it presents as a disadvantage the difficulty in positioning the eyebrow and the persistence of redundant skin, since, with this technique, only the soft tissues are elevated, without performing skin resections4,18.
Transpalpebral approaches are another alternative for the treatment of the frontal region, but they are indicated only for small degrees of ptosis of the eyebrow and have frequent recurrence. More recently, the use of botulinum toxin, hyaluronic acid, support threads, and surgical techniques, such as gliding brow lifting, have been described as less invasive options for the treatment of the frontal region19,20,21,22. These techniques are also indicated for cases with less skin excess since the tissues are not resected.
In the case presented, the redundancy of the skin was more pronounced in the frontal region, mainly in the caudal third, near the eyebrow. Therefore, correction would not be possible using the existing coronal rhytidoplasty techniques, since the skin tissue had an inelastic characteristic. Traction of the flap in the cranial direction would be ineffective in this case due to the distance between the incision and the area to be corrected.
In the literature, there are descriptions of the treatment of the frontal region with the traditional coronal incision. However, this method has the disadvantage of the need to subject the patient to multiple surgical procedures to correct excess skin in the supraciliary region2,23.
Therefore, the author of this article developed the reverse frontal lift technique, which allows treating excess skin in the caudal third of the forehead, while attenuating frontal and nasoglabellar wrinkles. The same concept of local traction applies to the nasogenial sulcus region, which will not be corrected only with SAMS traction and overlying skin. The burden of local resections is the most apparent scarring, however, accepted by this patient without resistance.
CONCLUSION
Despite the wide range of facelift techniques, surgeons are not free to face challenging cases that must be addressed through atypical incisions. The reverse frontal elevation technique was created for a specific case of pachydermoperiostosis. When well indicated for application in rare cases, this technique can be used to achieve good results. Despite the increased exposure to the scar, with a layered suture and carefully coaptized skin, it is possible to achieve a satisfactory result.
REFERENCES
1. Supradeeptha C, Shandilya SM, Reddy KV, Satyaprasad J. Pachydermoperiostosis - a case report of complete form and literature review. J Clin Orthop Trauma. 2014 Mar;5(1):27-32.
2. Taichao D, Fuling L, Hengguang Z. Comprehensive surgical strategies for the management of pachydermoperiostosis. Facial Plast Surg. 2018 Jun;34(3):330-4.
3. Barrett DM, Casanueva FJ, Wang TD. Evolution of the rhytidectomy. World J Otorhinolaryngol Head Neck Surg. 2016;2(1):38-44.
4. Pontes R. O universo da ritidoplastia. Rio de Janeiro: Revinter; 2011.
5. Hollander E. In: Plastische(Kosmetische) Operation: KritischeDarstellungihresgegenwartigen, Stands. Berlin: Urban and Schwarzenberg; 1932:1e17.
6. Lexer E. Leipzig: JA Barth; 1931.
7. Kaplan JL. Skin only facelift. Medscape Drugs Dis. 2014.
8. Hunt HL. Plastic surgery of the head, face, and neck. Philadelphia: Lea & Febiger; 1926.
9. Joseph J. NasenplastiK und sonstige gesichtsplastik: nebst einem Anhang über mammaplastik. Ant Labitzsch Leipzig 1931:507-509
10. Liang MD. Temporal approach to corrugator laser ablation. In: Ramirez OM, Rollin DK, eds. Endoscopic plastic surgery. New York: Springer-Verlag; 1996. p. 28-35.
11. Pangman WJ 2nd, Wallace RM. Cosmetic surgery of the face and neck. Plast Reconstr Surg. 1961;27:544-50.
12. Skoog T. Plastic Surgery: New Methods and Refinements. Philadelphia: W.B. Saunders; 1974.
13. Mitz V, Peyronie M. The superficial musculo-aponeurotic system (SMAS) in the parotid and cheek area. Plast Reconstr Surg. 1976;58:80e88.
14. Pierce GW, Klabunde EH, Bergeron VL. Useful procedures in plastic surgery. Plast Reconstr Surg (1946). 1947;2(4):358-361.
15. Castañares S. Forehead wrinkles, glabellar frown and ptosis of the eyebrows. Plast Reconstr Surg.1964;34:406-13.
16. Regnault P. Complete face and forehead lifting, with double traction on "crow's-feet". Plast Reconstr Surg. 1972;49(2):123-129.
17. Vinas JC, Caviglia C, Cortinas JL. Forehead rhytidoplasty and brow lifting. Plast Reconstr Surg. 1976;57(4):445-454.
18. Chi JJ. Periorbital surgery forehead, brow, and midface. Facial Plast Surg Clin North Am. 2016 May;24(1):107-17.
19. Fattahi T. Open brow lift surgery for facial rejuvenation. Atlas Oral Maxillofacial Surg Clin North Am. 2016 Sep;24(2):161-4.
20. Moradi A, Watson J. Current concepts in filler injection. Facial Plast Surg Clin North Am. 2015 Nov;23(4):489-94.
21. Pedroza F, Anjos GF, Bedoya, Rivera M. Update on brow and forehead lifting. Curr Opin Otolaryngol Head Neck Surg. 2006 Aug;14(4):283-8.
22. Viterbo F, Auersvald A. Glinding brow lifting. Plast Reconstr Surg Glob Open. 2017 Sep;5(9 Suppl):186-7.
23. Lima JSF, Costa SM, Chiari Júnior A, Bezerra MM, Polizzi LQR, Polizzi RJ. Surgical treatment of primary pachydermoperiostosis: report of two cases. Rev Bras Cir Plást. 2014;29(1):165-8.
1. Serviço de Cirurgia Plástica Professor Ronaldo Pontes, Cirurgia Plástica, Niterói,
RJ, Brazil.
Corresponding author: Ronaldo Pontes, Av. Sete de Setembro, 301, Santa Rosa, Niterói, RJ, Brazil. Zipe Code: 24230-251. E-mail: servicopgronaldopontes@gmail.com
Article received: February 19, 2019.
Article accepted: February 29, 2020.
Conflicts of interest: none.







 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter