

Case Report - Year 2019 - Volume 34 -
Extended and pedicled pectoralis major flap for right orbitofrontal-parietal reconstruction following invasive squamous cell carcinoma resection
Retalho de peitoral maior estendido e pediculado para reconstrução de região orbito-fronto-parietal direita após exérese de carcinoma espinocelular invasivo
ABSTRACT
Introduction: The myocutaneous flap is often used in reconstruction of head and neck defects. However, it is restricted to the middle third of the face. Perforating artery dissection techniques allow further lengthening of the pedicle, thus achieving coverage of the orbitofrontal-parietal region.
Case report: A 63-year-old male with a poorly-differentiated invasive squamous cell carcinoma presented with a final defect of 12.0 × 18.0 cm in the right orbitofrontal-parietal region, with dura mater, frontal sinus, and right upper orbit exposure after resection. We designed a pectoralis major flap, with a cutaneous island equaling the defect in dimensions, in the right parasternal region, from the fourth intercostal space to the subcostal region (extended). The pedicle was sectioned after 4 weeks. The coverage was effective, with no major complications, and a satisfactory aesthetic result.
Conclusion: This flap can be an excellent option for reconstruction of the upper third of the head when there are limitations to microsurgery.
Keywords: Cutaneous neoplasia; Squamous cell neoplasia; Surgical flaps; Myocutaneous flap; Pectoral muscles
RESUMO
Introdução: O retalho miocutâneo de peitoral maior é um dos mais usados na reconstrução de defeitos da cabeça e pescoço, porém com restrição ao terço médio da face. Com técnicas de dissecção de perfurantes, consegue-se alongar mais o pedículo, obtendo coberturas da região orbito-fronto-parietal.
Relato de Caso: Paciente masculino de 63 anos apresentando carcinoma espinocelular invasivo pouco diferenciado, que após sua ressecção cirúrgica apresentou defeito final de 12,0 x 18,0cm na região órbito-fronto-parietal direita com exposição de dura-máter, seio frontal e órbita superior direita. Foi desenhado retalho de peitoral maior com ilha cutânea de dimensões iguais ao defeito na região paraesternal direita, desde o quarto espaço intercostal até a região subcostal (estendido). O pedículo foi seccionado após 4 semanas. A cobertura foi efetiva, sem complicações maiores e resultado estético satisfatório.
Conclusão: Este retalho mostrou ser uma excelente opção para reconstrução do terço superior da cabeça quando existam limitações para a realização de microcirurgia.
Palavras-chave: Neoplasias cutâneas; Neoplasias de células escamosas; Retalhos cirúrgicos; Retalho miocutâneo; Músculos peitorais
INTRODUCTION
The pectoralis major myocutaneous flap is often used in reconstruction after head and neck tumor resection. Ariyan et al. first described this technique in 19791.
Few reports have described the use of this flap in reconstruction above the orbits, due to the risk of necrosis and the difficulty of flap mobilization, rotation, and extension.
Defects in the scalp and upper third of the face remain a challenge for surgeons. Advances in surgery have included use of perforating arteries and improved techniques of dissection of the pectoral pedicle. These have allowed release and lengthening of the pectoralis major muscle, augmentation of its arc of rotation, and gain in the extension of the flap (cutaneous island) to obtain more distal coverage in the head and upper third of the face.
OBJECTIVE
This study reported the use of an extended pedicled muscle flap to cover defects in the right orbitofrontal-parietal region after resection of invasive squamous cell carcinoma.
CASE REPORT
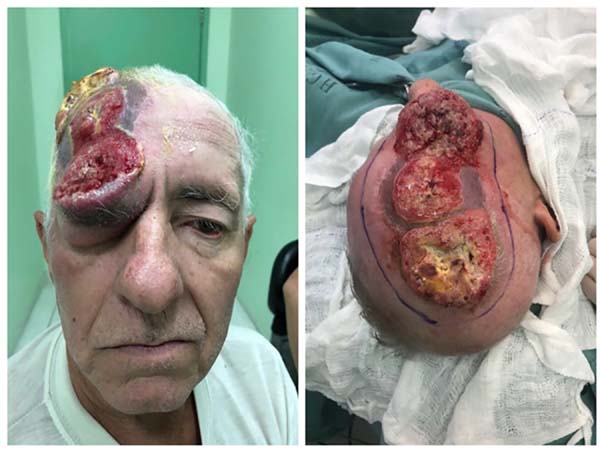
A 63-year-old male with an ulcerated, grade III, poorly-differentiated squamous cell carcinoma presented 6 months after initial resection and grafting with a recurrent tumor in the right parietal region. The patient had a 5.0-cm right parietal ulcerated lesion with an adjacent osteolytic component, another frontal lesion measuring 3.0 cm, and another 4.0-cm lesion in the right lower frontal region with signs of adjacent bone involvement. Invasion of the paranasal sinus and right superomedial orbit had occurred (Figure 1).
The case was evaluated by the oncological surgery and neurosurgery teams of the Guilherme Álvaro Hospital, Santos, SP, for tumor resection with curative intention, in collaboration with the plastic surgery team for immediate reconstruction. The lesion was resected with lateral margins of 15 mm, with resection of the affected bone in the parietal and upper frontal regions and anterior and posterior walls of the right frontal sinus, leaving the dura mater exposed.
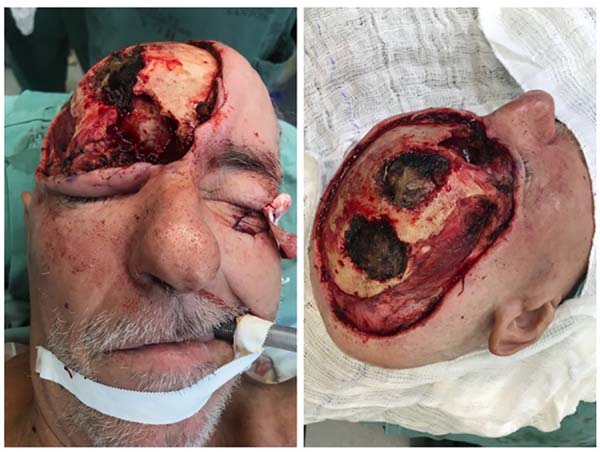
The superomedial bony portion of the right orbit was resected, revealing communication with the right frontal sinus and right nasal cavity; the globe, ocular muscles, and 1.0 cm of the upper eyelid were preserved. The final defect measured 12.0 × 18.0 cm in the right orbitofrontal-parietal region, with dura mater, frontal sinus, and right upper orbit exposure (Figure 2).
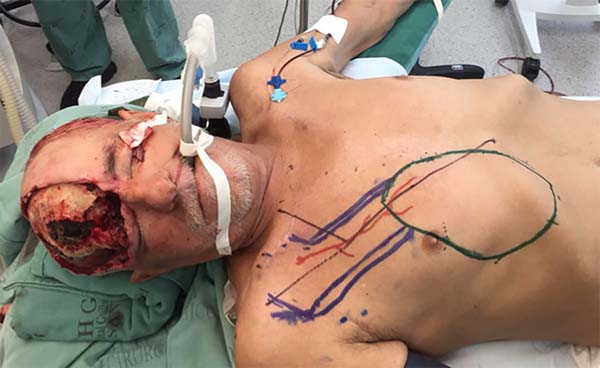
For reconstruction, we marked a pectoralis major flap measuring 12.0 × 18.0 cm in the right parasternal area, from the fourth intercostal space to the subcostal region (extended), to enable coverage of the defect without lateral traction on the head (Figure 3).
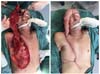
We detached the pectoralis muscle, while preserving the thoracoacromial pedicle, leaving only a long muscular band in the axis of the vascular pedicle, and performed total section of the muscle at the base of the flap; a cutaneous band on the pedicle was left for protection and maintenance of the perforating cutaneous thoracoacromial pedicle.
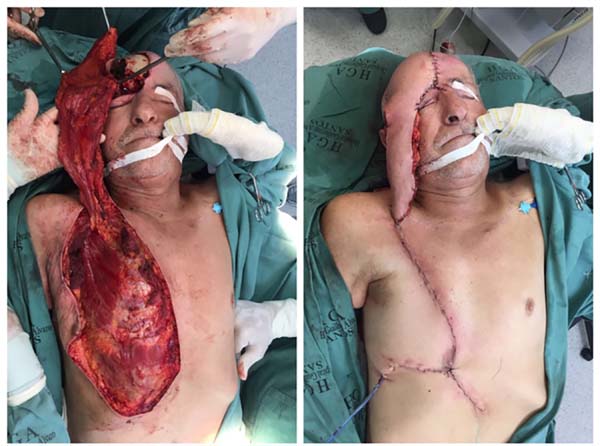
We performed total section of the superior pectoral nerve, partial section of the deltoid muscle insertion in the clavicle to reduce rotation tension in the external pedicle, and released the vascular pedicle to the thoracoacromial trunk at the origin of the axillary artery. The closure of the donor area was performed with tension-free advancement flaps (Figure 4).
To obliterate the frontal-orbital-nasal communication, a contralateral frontal muscle flap was created and sutured in place.
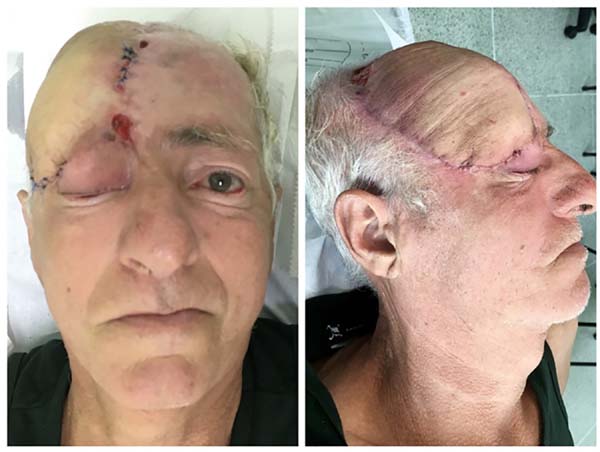
During recovery, the patient developed a 3.0-cm necrotic area at the distal edge of the flap; this was resected together with the pedicle 4 weeks later. Wet dressings were applied to the area of resected necrosis until granulation tissue was observed, with subsequent grafting. The coverage was effective, with no major complications or hematomas, and a satisfactory aesthetic result was achieved despite the extensive oncologic surgery. The patient remains under follow-up, and is receiving radiotherapy because of high risk of recurrence and infiltration of the dura mater and frontal sinus mucosa (Figure 5).
DISCUSSION
The pectoralis major flap is commonly used for head and neck reconstruction, but its applicability in the supraorbital area has a risk of failure and necrosis due to tension. Its use depends largely on patient anatomy. The cutaneous island on the pectoralis muscle typically measures 6.0 × 12.0 cm. The skin flap should not be extended more than 20% beyond the edge of the muscle2. This type IV flap with a thoracoacromial dominant pedicle is easy to monitor and dissect.
Most reports on this flap discuss a musculocutaneous or muscular type, with a mostly minor complication rate of 33% and a 2% risk of necrosis3.
Cadaver studies by Rikimaru et al.4,5 identified the main cutaneous perforating arteries of the second and third intercostal area using microvascular angiography. Based on these studies, Nishi et al.6 described flaps using pectoral and deltopectoral perforating arteries.
Zhang et al.7 described a pectoral region flap in an anatomical study of the perforating branches of the thoracoacromial artery, and reported the existence of 1 or 2 main perforators within 4.0 cm of the point of union of the acromioxiphoid and midclavicular lines. These perforators allowed a pedicle flap using thoracoacromial artery perforators to be performed. This flap can be performed with microsurgical technique for superior defects8-10.
With this anatomical knowledge of the perforators of the thoracoacromial vascular pedicle, a large cutaneous island can be maintained, and the muscle can be partially or totally resected. The flap rotation arc may improve with muscle detachment, careful dissection of the pedicle, and section of deltoid muscle bands, and infraclavicular tunneling has been described. Surgery is ideally performed in a single session, but an external pedicle is needed to obtain coverage distant from the donor bed, as in the present case. The literature to date has not reported a pedicled pectoralis major flap that has been extended this far while remaining viable.
The extended pedicle flap was an excellent surgical option for reconstruction of the upper third of the head following extensive tumor resection, in an area with limitations to microsurgery; with anatomical knowledge and careful dissection, we obtained a satisfactory result.
COLLABORATIONS
|
AOE |
Conception and design study, data curation, methodology, realization of operations and/ or trials, writing - original draft preparation. |
|
DCL |
Methodology, realization of operations and/or trials, writing - review & editing. |
|
AFC |
Data Curation, realization of operations and/ or trials, writing - review & editing. |
|
CFG |
Data curation, realization of operations and/or trials, writing - review & editing. |
|
LG |
Realization of operations and/or trials, writing - review & editing. |
|
RGN |
Writing - original draft preparation, writing - review & editing. |
|
ORS |
Final manuscript approval, methodology, writing - review & editing. |
REFERENCES
1. Ariyan S. The pectoralis major myocutaneous flap. A versatile flap for reconstruction in the head and neck. Plast Reconstr Surg. 1979;63(1):73-81. PMID: 372988
2. Part II Regional Flaps: Anatomy and Basic Techniques, section 6E: Pectoralis Major Flap. In: Zenn MR, Jones G. Reconstructive Surgery: Anatomy, Technique, and Clinical Applications. St. Louis: Quality Medical Publishing; 2012. p. 520-41.
3. Milenović A, Virag M, Uglesić V, Aljinović-Ratković N. The pectoralis major flap in head and neck reconstruction: first 500 patients. J Craniomaxillofac Surg. 2006;34(6):340-3. DOI: http://dx.doi.org/10.1016/j.jcms.2006.04.001
4. Rikimaru H, Kiyokawa K, Inoue Y, Tai Y. Three-dimensional anatomical vascular distribution in the pectoralis major myocutaneous flap. Plast Reconstr Surg. 2005;115(5):1342-52. DOI: http://dx.doi.org/10.1097/01.PRS.0000156972.66044.5C
5. Rikimaru H, Kiyokawa K, Watanabe K, Koga N, Nishi Y, Sakamoto A. New method of preparing a pectoralis major myocutaneous flap with a skin paddle that includes the third intercostal perforating branch of the internal thoracic artery. Plast Reconstr Surg. 2009;123(4):1220-8. PMID: 19337090 DOI: http://dx.doi.org/10.1097/PRS.0b013e31819f2967
6. Nishi Y, Rikimaru H, Kiyokawa K, Watanabe K, Koga N, Sakamoto A. Development of the pectoral perforator flap and the deltopectoral perforator flap pedicled with the pectoralis major muscle flap. Ann Plast Surg. 2013;71(4):365-71. DOI: http://dx.doi.org/10.1097/SAP.0b013e3182503c5d
7. Zhang YX, Yongjie H, Messmer C, Ong YS, Li Z, Zhou X, et al. Thoracoacromial artery perforator flap: anatomical basis and clinical applications. Plast Reconstr Surg. 2013;131(5):759e-70e. PMID: 23629115
8. Li Z, Cui J, Zhang YX, Levin LS, Zhou X, Spinelli G, et al. Versatility of the thoracoacromial artery perforator flap in head and neck reconstruction. J Reconstr Microsurg. 2014;30(7):497-503. DOI: http://dx.doi.org/10.1055/s-0034-1370359
9. Zhang YX, Li Z, Grassetti L, Lazzeri D, Nicoli F, Zenn MR, et al. A new option with the pedicle thoracoacromial artery perforator flap for hypopharyngeal reconstructions. Laryngoscope. 2016;126(6):1315-20. DOI: http://dx.doi.org/10.1002/lary.25675
10. Song D, Pafitanis G, Pont LEP, Yang P, Koshima I, Zhang Y, et al. Chimeric thoracoacromial artery perforator flap for one-staged reconstruction of complex pharyngoesophageal defects: A single unit experience. Head Neck. 2018;40(2):302-11. DOI: http://dx.doi.org/10.1002/hed.24962
1. Serviço de Cirurgia Plástica Osvaldo Saldanha,
Cirurgia Plástica Reconstrutiva e Estética, Santos, SP, Brazil
2. Hospital Santa Casa, Serviço de Cirurgia
Plástica, Santos, SP, Brazil.
Corresponding author: Andres Ordenes Evensen Av. Ana Costa, nº 146, conjunto 1201 - Santos, SP, Brazil Zip Code 11060-000 E-mail: aordenese@gmail.com / carlosgoye.m@gmail.com
Article received: April 8, 2018.
Article accepted: October 1, 2018.
Conflicts of interest: none.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter