

Original Article - Year 2018 - Volume 33 -
Reverse anterolateral thigh flap: a reconstruction option for the lower limbs
Retalho anterolateral da coxa reverso: uma opção de reconstrução para os membros inferiores
ABSTRACT
Introduction: Cutaneous and soft tissue reconstruction in the
region around the knee is often challenging for the plastic surgeon
and aimed at providing good knee joint function with acceptable
aesthetic appearance. Surgical planning requires considering
the simplest technique that leads to wound closure, with minimal
morbidity in the donor area. The literature has reported only
few cases of the use of the reverse anterolateral (ALT) flap for
defects in the popliteal fossa, knee, and leg proximal portion. The
objective is to describe a series of cases of patients who underwent
reconstruction with a reverse ALT flap for wounds in the popliteal
fossa, knee, and upper third of the leg.
Methods: Among four
patients, three received popliteal fossa reconstructions and one
received knee and leg proximal third reconstructions. All the
patients underwent wound/tumor extensive resection, dissection
of the reverse ALT flap, and transposition to the defect.
Results:
During follow-up for 2 to 18 months, minimal morbidity was
observed in the donor area, with a total coverage of the defect,
optimal functional result of the affected limb, and good aesthetic
result. Only one case had a partial necrosis (15%) of the flap due
to hematoma and pedicle compression. In the other patients, no
evidence of flap failure, dehiscence, seroma, or infection were found.
Conclusion: The reverse ALT flap was a viable option, presenting
good functional and aesthetic results for cutaneous and soft tissue
reconstructions in the popliteal fossa, knee, and upper third of the leg.
Keywords: Perforator flap; Reconstructive surgical procedures; Lower extremity; Surgical flaps
RESUMO
Introdução: A reconstrução cutânea e de tecidos moles na região ao redor do joelho é
frequentemente desafiadora para o cirurgião plástico e tem como objetivo
fornecer uma boa função articular do joelho com aparência estética
aceitável. O planejamento cirúrgico requer considerar a técnica mais simples
que leve ao fechamento da ferida, com mínima morbidade na área doadora. Há
poucos relatos do uso do retalho anterolateral (ALT) reverso na literatura,
em se tratando de defeitos na fossa poplítea, joelho e porção proximal da
perna. O objetivo é descrever uma serie de casos de pacientes submetidos à
reconstrução de ferida em fossa poplítea, joelho e terço superior da perna
com retalho ALT reverso.
Métodos: Quatro pacientes, dos quais 3 eram reconstruções de fossa poplítea e 1
reconstrução de joelho e terço proximal da perna. Todos submetidos à
ressecção ampla da ferida/tumor, dissecção do retalho ALT reverso, e
transposição para o defeito.
Resultados: Follow-up de 2 a 18 meses, evidenciando-se morbidade mínima para área
doadora, com cobertura total do defeito e ótimo resultado funcional do
membro afetado, com bom resultado estético. Apenas em um dos casos
evidenciou-se sofrimento e necrose parcial (15%) do retalho devido a
hematoma e compressão do pedículo, nos demais não foi evidenciado sofrimento
dos retalhos, deiscência, seroma ou infecção.
Conclusão: O retalho ALT da coxa reverso mostrou-se uma opção viável, apresentando bom
resultado funcional e estético para a reconstrução cutânea e de tecidos
moles na região de fossa poplítea, joelho e terço superior da perna.
Palavras-chave: Retalho perfurante; Procedimentos cirúrgicos reconstrutivos; Extremidade inferior; Retalhos cirúrgicos
INTRODUCTION
Cutaneous and soft tissue reconstruction in the region around the knee is often challenging for the plastic surgeon and aimed at providing an acceptable aesthetic appearance associated with good knee joint function1. A well-vascularized tissue is necessary to ensure good wound healing, with local and free flaps among the surgical options.
Local flaps are usually in or near the lesion and have limitations regarding the size and length of the vascular pedicle, which is relatively small2. As for the free flaps, besides being a more complex procedure in the reconstructive ladder of plastic surgery, microvascular anastomosis technical difficulty due to the depth of the recipient vessels3,4.
Surgery planning requires the simplest technique that will lead to wound closure, with the minimum morbidity in the donor area5. The fasciocutaneous reverse anterolateral thigh (ALT) flap, which was described first in 1990 by Zhang et al., seems to be an effective and lasting option for the reconstruction of defects around the knee. It has a long vascular pedicle and a large cutaneous portion1,4,5. Since then, some studies have been published in the literature with success on the use of the reverse ALT flap in the treatment of injuries around the knee; however, only few reports have described its use in defects located in the popliteal fossa6.
In this work, a series of cases of patients who underwent reconstruction with fasciocutaneous reverse ALT flap for defects in the popliteal fossa, proximal region, and leg is presented.
OBJECTIVE
To demonstrate the experience of the Reconstructive Plastic Surgery Service of the Workers’ Hospital in Curitiba, Paraná, with lower limb reconstruction using the reverse ALT thigh flap. This study aimed to verify the safety, versatility, and reproducibility of this flap for the reconstruction of large wounds in the regions of the lower thigh, knee, popliteal fossa, and proximal third of the leg.
METHODS
All cases were selected from among reverse ALT thigh flap reconstructions performed in the last 18 months in the plastic and reconstructive surgery service. Of the 4 cases selected, 3 were for reconstruction of the popliteal fossa and 1 was for reconstruction of the upper third of the leg. Follow-up for 2 to 18 months was conducted for the patients, and questions were asked about the member function, aesthetics, and overall satisfaction with the procedure. In addition, all surgical complications inherent to the procedure and other interventions needed were discussed.
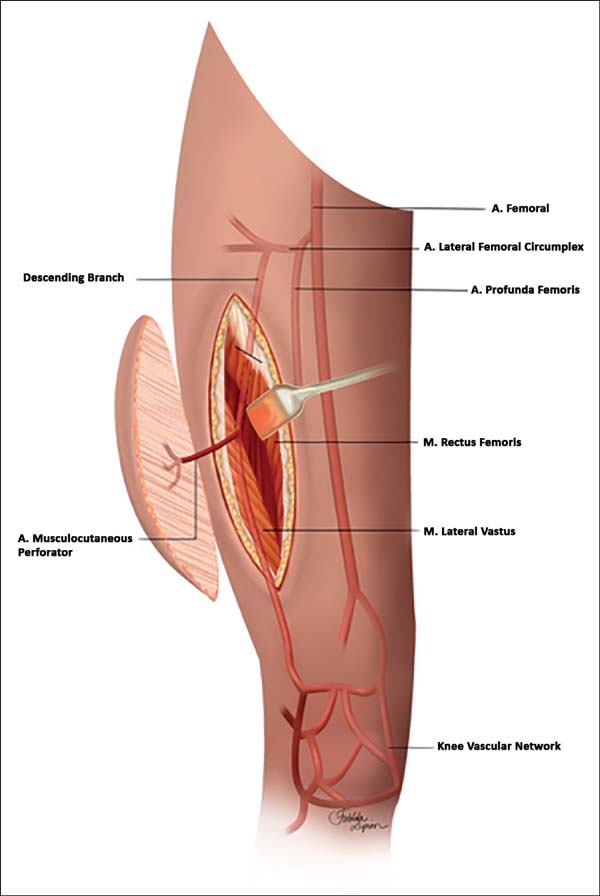
The technique of lifting the anterolateral flap of the reverse thigh was performed as described in the following steps: 1. Marking of the donor area was comprised of an ellipse of the previously debrided wound size in which the center was comprised of the midpoint of a traced line between the anterior superior iliac crest and the lateral border of the patella (Figure 1). 2. Incision of the medial portion of the marking. 3. Medial-to-lateral subfascial dissection, locating the perforator of the descending branch of the lateral femoral circumflex artery (LFCA). 4. Incision of the lateral portion of the flap and detachment of the fasciocutaneous flap. 5. Dissection of the perforator artery from the LFCA trunk to the lateral superior genicular artery (LSGA). 6. Clamping and sectioning of the proximal portion of the LFCA, with the flap fed by the LSGA. 7. Elaboration of the subcutaneous tunnel in the knee region.
This study was approved by the ethics and research committee of the Worker’s Hospital, with registration No. 69703617.9.0000.5225.
RESULTS
Case 1
A 24-year-old man fell from a 2-m height and incurred a tibial plateau fracture, which was surgically treated with placement of two plates through the posterior access, which evolved with infection and dehiscence of the surgical wound. After 8 months of conservative treatment, use of an anterolateral reverse thigh flap was proposed.
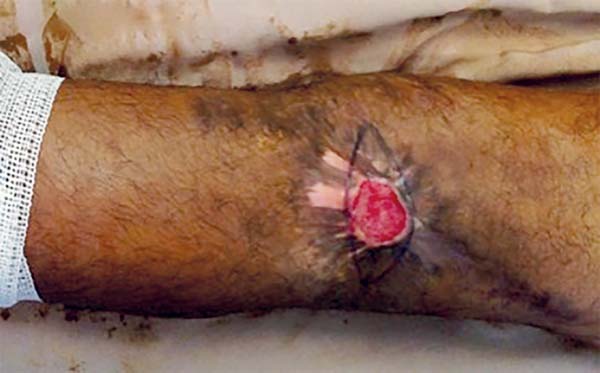
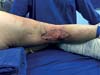
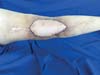
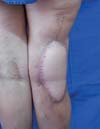
Physical examination revealed an unstable wound of 3 × 3 cm in size in the popliteal fossa region with adjacent tissue contraction (Figure 2).
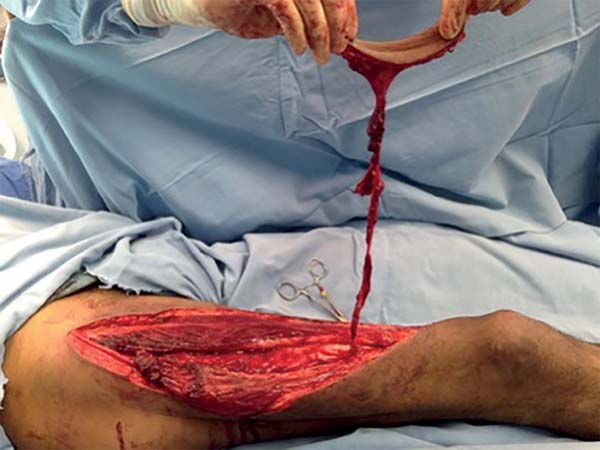
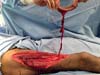
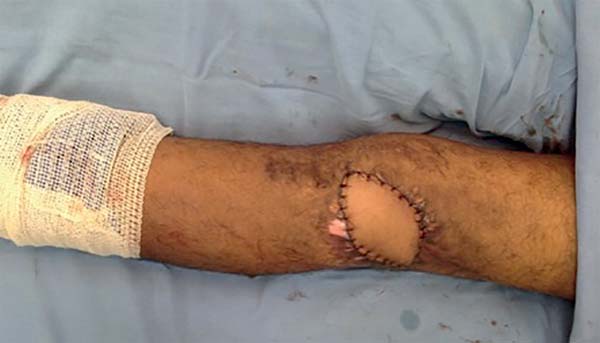
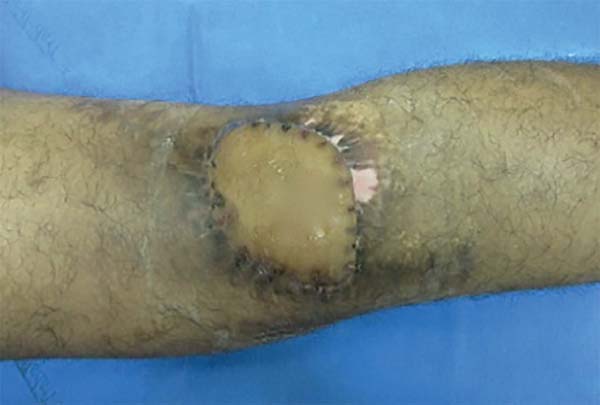
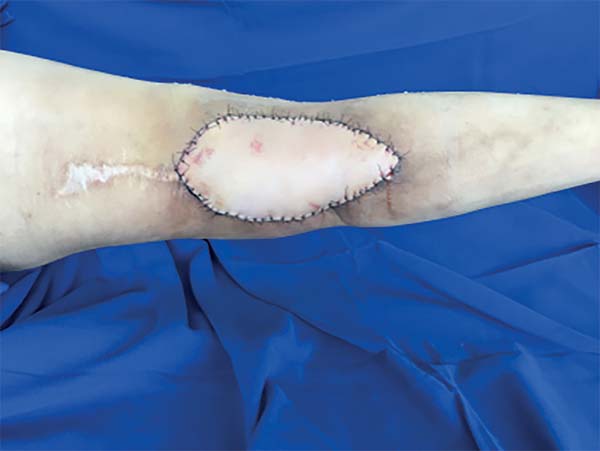
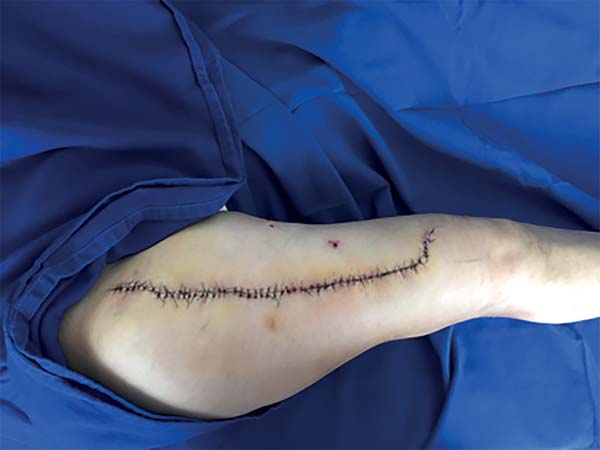
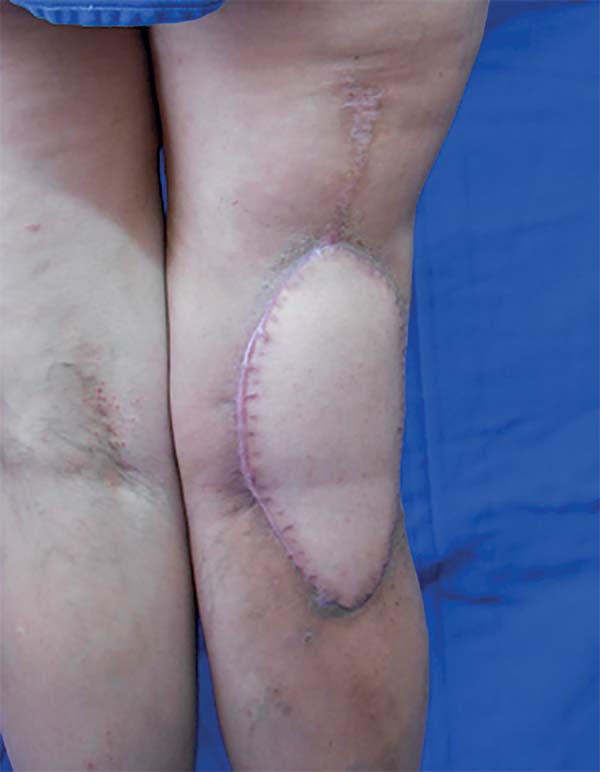
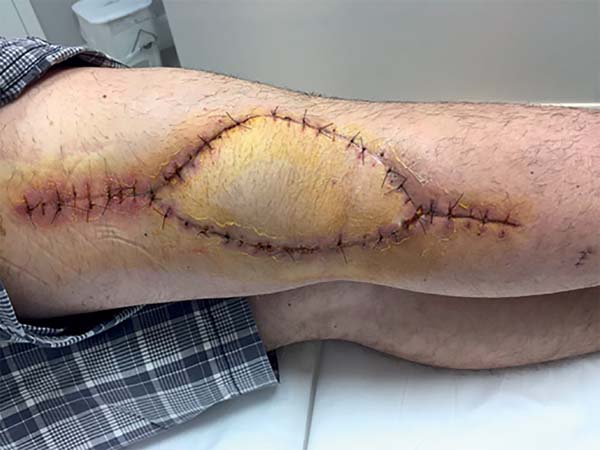
The surgery started with wound excision and debridement of the scar tissue around it. The flap was released in accordance with the technique described in our methodology. The flap was then transposed to the defect in the popliteal fossa, passing through the subcutaneous tunnel created in the medial knee region (Figure 3). The donor area was closed primarily and a cast-splint was placed, keeping the knee in extension to prevent bending of the vascular pedicle. In the immediate and 10-month postoperative periods, the area had a good appearance (Figures 4 and 5).
Case 2
A 30-year-old woman with a history of exposed fracture of the proximal tibia was treated with Ilizarov external fixation, which resulted in a large scar retraction and unstable wound that limited the complete flexion of the left leg.
The physical examination revealed an unstable wound of 2.5 × 2.5 cm in size in the anterolateral proximal leg region (Figure 6). Thus, reconstruction of the region was planned with a reverse ALT flap.
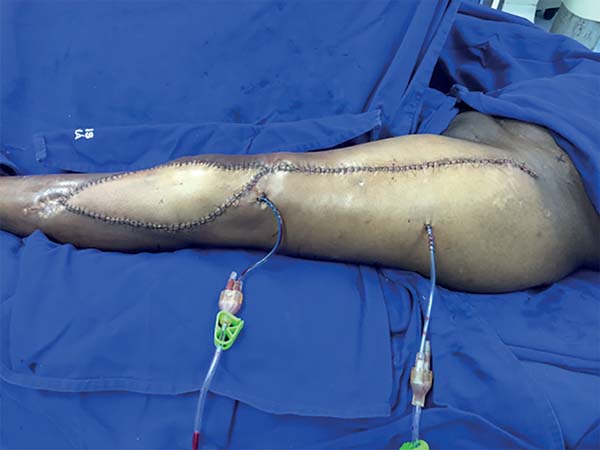
Surgery was started with the dissection and location of the LSGA once the patient had retraction in the anatomical region of the LSGA, which was then followed by wound excision and debridement of the surrounding scar tissue. The next steps were as described in the methodology, with only one difference. In this case, elaboration of tunnel was not necessary for the pedicle, as the incision was in communication with wound resection. At the end of the procedure, a suction drain was placed in the donor and recipient areas. The final appearance was good (Figure 7).
Case 3
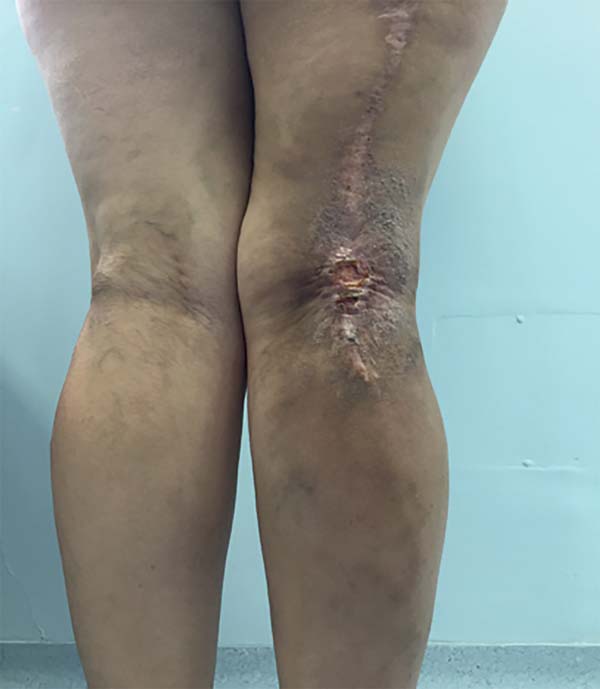
A 40-year-old woman had a history of resection of a liposarcoma in the right popliteal region, complemented by post-resection radiotherapy, which evolved with a large chronic wound and local radiodermatitis for a period of 3 years.
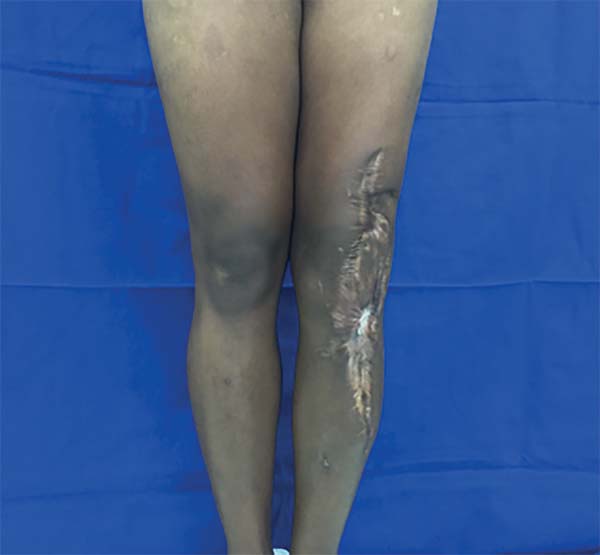
Physical examination revealed an unstable 7 × 4cm wound in the right popliteal fossa (Figure 8). Hence, reconstruction of the region was planned with a reverse anterolateral thigh flap (Figure 9).
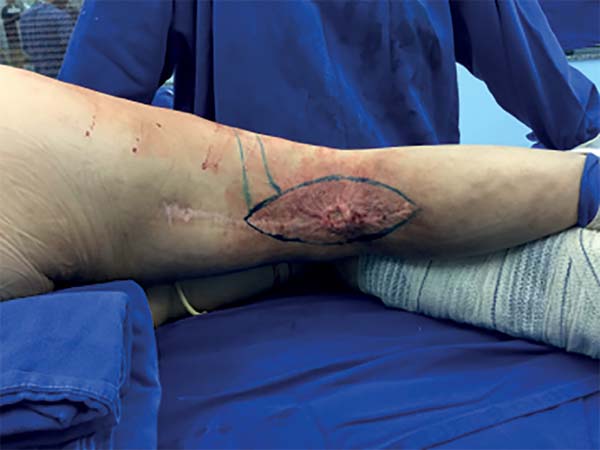
Marking of the donor area and flap release followed the steps described in the methodology. In this case, the anatomical variation made the artery dissection difficult because the LFCA perforator that nourished the flap had a proximal origin. Thus, the level of ligature was almost at the emergence of the deep femoral artery. After confirmation of adequate retrograde flux of the LSGA, the proximal ligation of the LFCA was safely conducted. Next, excision of the chronic wound with the radiodermatitis area (Figure 10) was performed, and the flap transposed to the defect of the popliteal fossa, passing through a subcutaneous tunnel created in the lateral region of the knee (Figures 11 and 12). The wound and donor areas had a pleasing final appearance (Figures 12 and 13) at 3 months after operation (Figure 14).
Case 4
A 35-year-old male patient presented a large fibrosarcoma on the right popliteal fossa, with infiltration of noble structures.
Physical examination revealed a large tumor in the right popliteal fossa of 10 × 10 cm in size, fixed to the depth. Magnetic resonance imaging of the right knee detected an invasion of the common fibular nerve, posterior joint knee capsule, and medial and lateral heads of the gastrocnemius muscle of the right lower limb. No invasion of the popliteal artery or lateral genicular arteries was identified. Therefore, tumor resection with reconstruction of the region with reverse anterolateral thigh flap was planned.
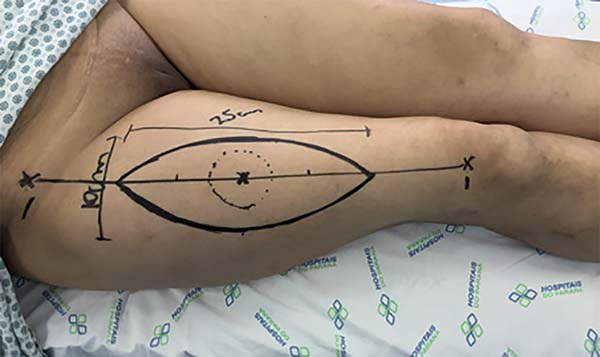
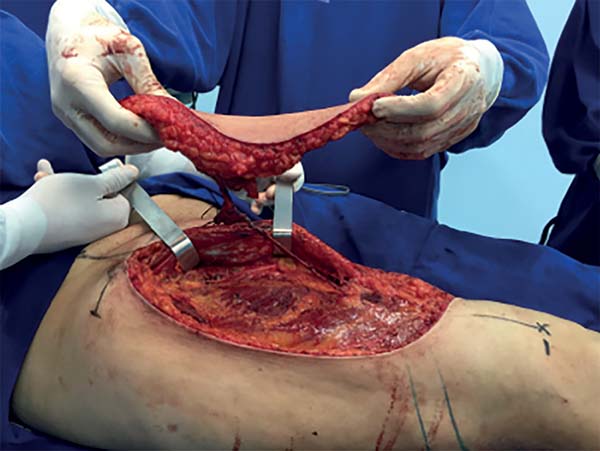
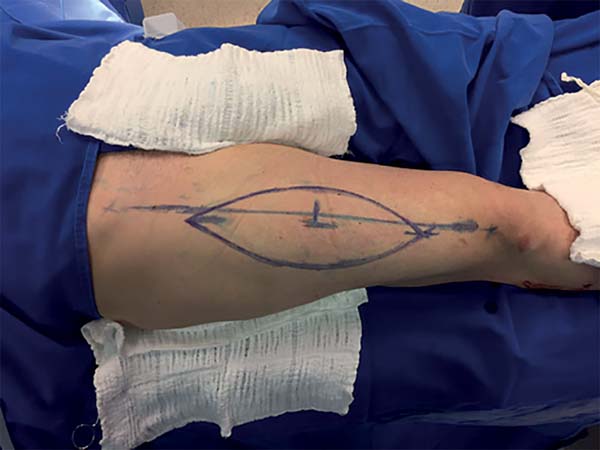
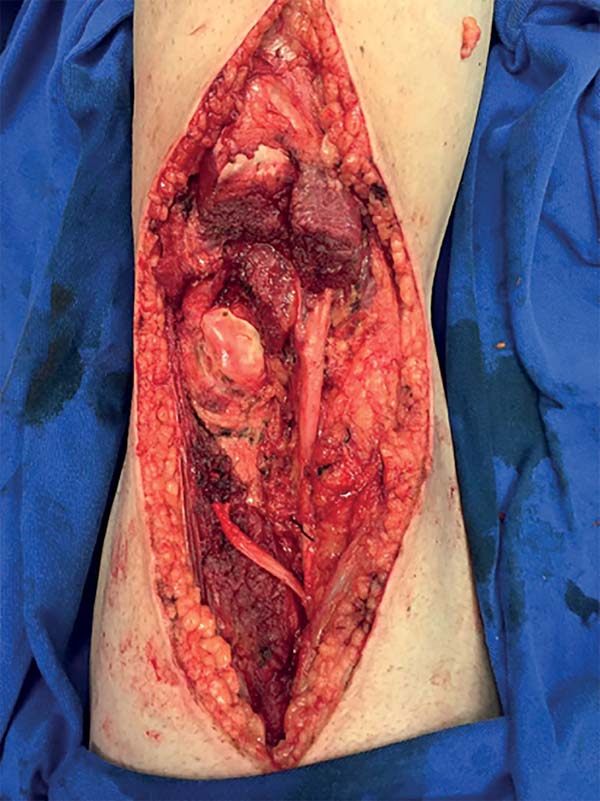
The marking of the donor area was comprised of a spindle-shaped area to be resected (Figure 15). The oncological surgeon began surgery with a wide resection with safety and tumor-free margins. The resection went deep into the posterior joint capsule of the knee, encompassing 15 cm of the common fibular nerve and insertion of the medial and lateral heads of the gastrocnemius muscle (Figure 16).
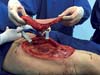
Next, the popliteal fossa reconstruction was started, with dissection of the sural nerve for microsurgical graft and nerve reanastomosis with interposition of the common fibular nerve graft. The nerve suture performed was epineural with the use of fibrin glue. Once the nerve graft was performed, dissection of the reverse ALT flap was started, following the technique described in the methodology (Figure 17).
Patients 1 to 4 were followed up for 18, 11, 4, and 2 months. The only complication occurred in case 2, which had a postoperative hematoma in 15% of the flap area. The debrided flap was subsequently grafted successfully. In case 1, thinning of the flap with liposuction was performed. In cases 3 and 4, no other interventions were needed.
Regarding limb function and resolution of the baseline problem, all the cases showed good results. From the aesthetic point of view, the only case that required reconsideration was case 2, which led to the patient’s complaint of an aesthetic impairment. Finally, the patients were questioned on the overall outcome of their procedures, all of whom were satisfied.
DISCUSSION
The knee and fossa popliteal region have inherent characteristics that can make even a small wound a challenge. Defects of the soft parts of this region may be accompanied by exposed bone or tendon, in addition to limitation in the range of joint knee movement1.
The cutaneous aspect of the anterolateral thigh region has an excellent vascular communication network, which allows the elevation of large ALT flaps with only one good-caliber perforator7. Consequently, the reverse ALT flap is a well-established option for defects in the knee region and has grown in popularity8.
The vascular base of this flap is the anastomosis between the descending branch of the LFCA and LSGA, which is located approximately 3 to 10 cm above the lateral border of the patella. This connection maintains a constant cutaneous perfusion through a retrograde blood flow, which was clearly described by Pan et al.6, which is enough for flap survival (Figure 1).
The reverse ALT flap has many advantages as follows: 1. long pedicle, large caliber, and enough blood supply; 2. large size and range of arc rotation; 3. The thickness of the flap is thinner than that of the muscle cutaneous flap; and 4. small morbidity of the donor area.4,9
Among the inconveniences described in this procedure are the risk of venous congestion due to long retrograde flow and arterial impairment due to compression or kinking of the pedicle4, which occurred in only one case (case 2) due to hematoma under the flap. In all the other cases, no complications occurred.
As it is a fasciocutaneous flap and allows primary closure of the donor area, the reverse ALT flap generates a purely aesthetic sequela. Another flap option to be used in the reconstruction of lesions of this region is the gastrocnemius muscle flap, which ends up generating a functional sequela of the limb.
Free flaps are also another option for reconstruction of this region, but to create these flaps, a highly specialized professional is needed, as well as specific materials such as a surgical microscope, which is often an unfeasible option in economically disadvantaged regions. Although the technique of detachment of the reverse ALT flap is laborious, no special material is needed to make this flap. Hence, it can be created even in regions with few resources, sparing the need for a microsurgery.
CONCLUSION
On the basis of the above-mentioned findings, the reverse ALT flap showed to be a viable reproducible option, presenting good functional and aesthetic results that are suitable for cutaneous and soft tissue reconstructions in the popliteal fossa, knee, and upper leg regions.
COLLABORATIONS
|
GSSJ |
Author’s contribution: analysis and/or data interpretation; conception and design study; data curation; final manuscript approval; methodology; project administration; realization of operations and/or trials; validation; writing - original draft preparation; writing - review & editing. |
|
RSF |
Author’s contribution: analysis and/or data interpretation; conception and design study; data curation; final manuscript approval; methodology; project administration; writing - original draft preparation; writing - review & editing. |
|
JRN |
Author’s contribution: analysis and/or data interpretation; conception and design study; data curation; final manuscript approval; methodology; project administration; writing - original draft preparation; writing - review & editing. |
|
AGM |
Author’s contribution: analysis and/or data interpretation; conception and design study; data curation; final manuscript approval; formal analysis; methodology; project administration; writing - original draft preparation. |
|
DRP |
Author’s contribution: analysis and/or data interpretation; conception and design study; data curation; final manuscript approval; formal analysis; methodology; project administration; writing - original draft preparation. |
|
RFRM |
Author’s contribution: analysis and/or data interpretation; conception and design study; data curation; final manuscript approval; formal analysis; methodology; project administration; writing - original draft preparation. |
|
VRS |
Author’s contribution: analysis and/or data interpretation; conception and design study; data curation; final manuscript approval; formal analysis; methodology; project administration; writing - original draft preparation. |
|
ABP |
Author’s contribution: analysis and/or data interpretation; conception and design study; data curation; final manuscript approval; formal analysis; methodology; project administration; writing - original draft preparation. |
REFERENCES
1. Demirseren ME, Efendioglu K, Demiralp CO, Kilicarslan K, Akkaya H. Clinical experience with a reverse-flow anterolateral thigh perforator flap for the reconstruction of soft-tissue defects of the knee and proximal lower leg. J Plast Reconstr Aesthet Surg. 2011;64(12):1613-20.
2. Sahin I, Guzey S, Aykan A, Nisanci M. The Reverse Fasciocutaneous ALT Flap Harvested From Deeply Wounded and Scarred Area for Reconstruction of the Knee: A Case Report. Int J Low Extrem Wounds. 2016;15(2):136-8.
3. Wang XC, Lu Q, Li XF, Burd A, Zhao BC, Wang YY, et al. Reversed anterolateral thigh adipofascial flap for knee and proximal calf defects. Burns. 2008;34(6):868-72.
4. Sadigh PL, Wu CJ, Shih HS, Jeng SF. Reverse Anterolateral Thigh Flap to Revise a Below-knee Amputation Stump at the Mid-tibial Level. Plast Reconstr Surg Glob Open. 2014;1(9):e88.
5. Zhang G. Reversed anterolateral thigh island flap and myocutaneous flap transplantation. Zhonghua Yi Xue Za Zhi. 1990;70(12):676-8.
6. Pan SC, Yu JC, Shieh SJ, Lee JW, Huang BM, Chiu HY. Distally based anterolateral thigh flap: an anatomic and clinical study. Plast Reconstr Surg. 2004;114(7):1768-75.
7. Saint-Cyr M, Wong C, Schaverien M, Mojallal A, Rohrich RJ. The perforasome theory: vascular anatomy and clinical implications. Plast Reconstr Surg. 2009;124(5):1529-44.
8. Liu TY, Jeng SF, Yang JC, Shih HS, Chen CC, Hsieh CH. Reconstruction of the skin defect of the knee using a reverse anterolateral thigh island flap: cases report. Ann Plast Surg. 2010;64(2):198-201.
9. Zhou G, Zhang QX, Chen GY. The earlier clinic experience of the reverse-flow anterolateral thigh island flap. Br J Plast Surg. 2005;58(2):160-4.
1. Hospital do Trabalhador de Curitiba, Curitiba,
PR, Brazil.
2. Universidade Federal do Paraná, Curitiba, PR,
Brazil.
Corresponding author: Guataçara Schenfelder Salles-Junior, Avenida Republica Argentina, nº 4406 - Novo Mundo, Curitiba, PR, Brazil, Zip Code: 81050-000. E-mail: guatajr@yahoo.com.br
Article received: April 8, 2018.
Article accepted: October 1, 2018.
Conflicts of interest: none.






 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter