

Original Article - Year 2018 - Volume 33 -
Evaluation of the nipple-areola complex after reduction mammoplasty with dermal release versus resected volume of the breast tissue
Avaliação da sensibilidade do complexo areolopapilar após mamoplastia redutora com liberação dérmica versus volume ressecado de tecido mamário
ABSTRACT
Introduction: The nipple-areola complex (NAC) plays an
important role both in breastfeeding and sexual lives of
the patients. Because of this, we must mention possible
complications of reduction mammoplasty, such change or
even loss of sensitivity of the NAC.
Method: This was a
prospective, randomized, controlled, double-blind study
to evaluate the relationship between the sensitivity of the
NAC after reduction mammoplasty with dermal release
and the resected volume of breast tissue. This study was
conducted between August 2013 and August 2015 at the
Hospital das Clínicas of the Federal University of Pernambuco
(HC-UFPE), in Recife City, Brazil.
Results: The study
involved 39 patients. The mean age and body mass index
(BMI) of the patients were 31.7 years and 25.5 kg/m2, respectively.
None of the patients was a smoker. The complication
rate was 41%, including 7 cases of non-aesthetic scars, 6
cases of hematoma (bruises), and 4 cases of dehiscence.
No patient had pain or NAC necrosis, and all the patients
expressed being satisfied with the final surgical result. No
statistically significant differences were found between
the patients of the experimental and control groups, both
in the group with resection of up to 300 g and those with
resection >300 g.
Conclusions: The maneuver of dermic
release did not result in any differences in the sensitivity of
the NAC, regardless of the quantity of resected breast tissue.
Keywords: Mammoplasty. Breast/innervation; Nipple; Dermis; Reconstructive surgical procedures
RESUMO
Introdução: O complexo areolopapilar (CAP) desempenha grande importância tanto na
amamentação quanto na vida sexual das pacientes, consequentemente, devemos
ressaltar que uma complicação potencial da mamoplastia redutora é a
alteração ou até a perda da sensibilidade do CAP.
Método: Estudo prospectivo, randomizado, controlado e duplo-cego para avaliar a
relação entre a sensibilidade do complexo areolopapilar após mamoplastia
redutora com liberação dérmica e o volume ressecado de tecido mamário. O
estudo ocorreu no período de agosto de 2013 a agosto de 2015, no Hospital
das Clínicas da Universidade Federal de Pernambuco (HC-UFPE).
Resultados: O estudo totalizou 39 pacientes. A média de idade da amostra foi de 31,7
anos, índice de massa corporal (IMC) médio de kg/m2 e nenhuma das pacientes
era tabagista. A taxa de comorbidade foi de 5,1% da amostra. O índice de
complicações foi de 41%, composto de 7 casos de cicatriz inestética, 6 de
hematoma e 4 de deiscência. Não houve caso de sofrimento ou necrose do CAP e
todas as pacientes se mostraram satisfeitas com o resultado cirúrgico final.
Não houve diferenças estatisticamente significantes em nenhuma das ocasiões
entre os pacientes do grupo experimento e controle, tanto no grupo de
ressecção de até 300 gramas quanto acima de 300gramas.
Conclusões: A manobra de liberação dérmica não provocou diferença na sensibilidade do
complexo areolopapilar, independentemente da quantidade de tecido mamário
ressecado.
Palavras-chave: Mamoplastia; Mama/inervação; Mama; Derme; Procedimentos cirúrgicos reconstrutivos
INTRODUCTION
The breast has been considered a symbol of femininity since the start of Western civilization, and in this culture, a breast with functional changes, such as changes in size or shape, can also generate a feeling of social inadequacy or low self-esteem in women1. In this field, reduction mammoplasty has been one of the surgical procedures most commonly performed in Brazil and worldwide1-3. The nipple-areola complex (NAC) plays an important role both in breastfeeding and sexual lives of the patients4. Because of this, we must mention possible complications of reduction mammoplasty, such as change or even loss of sensitivity of the NAC. The innervation thereof arises from the sensitive cutaneolateral rami of the 3rd, 4th, 5th, and 6th intercostal nerves, which come out laterally, and the 4th, which has an anterior lateral ramus that comes out after it5.
In this regard, in 1930, Schwartzman6 described a technique for cutaneous decortication, preserving the tissue around the nipple and, therefore, its respective vascular and nervous systems, thus attempting to assure better vascularization and sensitivity of the NAC after breast reduction. There is no consensus in the literature regarding the sensitivity of NAC after reduction mammoplasty. Authors, such as Mofid et al.7 and Agostini et al.8, found no changes in sensitivity after the surgical procedure. In contrast, DelVecchyo et al.9 and Wechselberger et al.10 concluded that sensitivity was improved after surgery. Spear2 reported a decrease in sensitivity, but it gradually improved for 12 months.
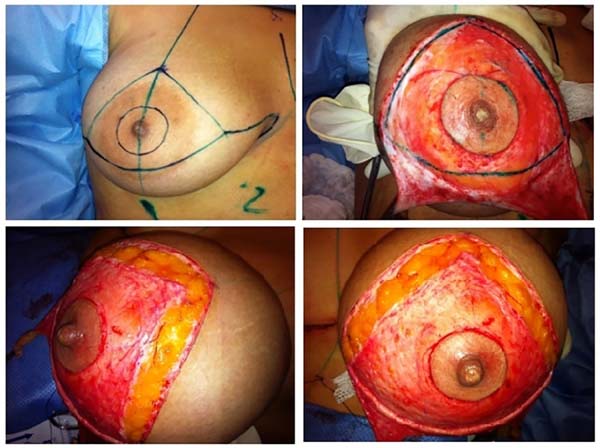
Currently, at the Plastic Surgery Department of Hospital das Clínicas, of the Federal University of Pernambuco (HC-UFPE) in Recife, Brazil, a careful section of the dermis has been performed routinely (Figure 1) after Schwartzman maneuver, seeking to facilitate the migration and the lower distortion of the NAC during the construction of the breast, particularly in cases that require greater involvement of these structures, to provide a more pleasing overall aesthetic result. However, its relationship with mammary sensitivity and the quantity of resected mammary tissue is still unclear.
OBJECTIVE
This study aimed to analyze the relationship between the sensitivity of the NAC after reduction mammoplasty with dermic release and the resected volume of the breast tissue.
METHODS
The research was conducted at HC-UFPE in Recife City, State of Pernambuco, Brazil, with prior authorization granted by the Research Ethics Committee of the Institution and approved with Certificate of Presentation for Ethical Appreciation (CAAE) No. 05351312.3.0000.5208. The study is a randomized, prospective, controlled, and double-blind study, conducted between August 2013 and August 2015.
The inclusion criteria were women who spontaneously sought the outpatient clinic of the Plastic Surgery Department and who were indicated for reduction mammoplasty, and aged between 21 and 50 years. The main exclusion criteria were with previous breast surgery; neurological disease; cardiovascular impediment; diabetes mellitus; self-immune diseases; collagen disorders; nipple-areola complex (BMI) >30; menopausal women, or those with psychiatric problems (as evaluated by the Mini Mental State Examination - MMSE). All patients underwent surgery at HC-UFPE. All surgical procedures were performed by the same surgeon, with the patients under general anesthesia and subjected to reduction mammoplasty, using the Pitanguy technique.
The patients underwent surgery consecutively, with breast reduction surgery being performed on both sides, with each patient grouped into the experimental or control NAC , and they were randomized using the website Random.org. In the case of the experimental NAC, a surgical maneuver of skin section was performed to facilitate the rising of the areola in the construction thereof, whereas in the case of the control NAC, the conventional surgical techniques were performed, without this maneuver.
In this way, sensitivity was assessed in five regions of the NAC (Figure 2), namely, the papillary, upper nipple, lateral nipple, medial and inferior regions, through the Semmes-Weinstein microfilaments, wherein the value for the areolar region was obtained calculating the arithmetic mean of the four points measured.
The periods for checking were pre- and postoperatively, after 3 weeks, 6 weeks, and 1 year. These checks were always conducted by the same member of the research team, blinded to the patient groups. Data regarding the total resected mammary tissue for each patient was also obtained, and the patients were divided into two groups: with total resected weight up to 300 g and >300 g of mammary material.
The data were grouped using a Microsoft Office Excel 2015 spreadsheet and analyzed using SPSS version 2.0. Wald’s test was used to compare the percentages of sensitivity of the evaluated regions of the control and experimental NACs, within the groups considered: resection up to 300 g and >300 g. The conclusions were made considering a level of significance of 5%.
RESULTS
The study involved 39 patients and 78 observations. The mean age and BMI were 31.7 years and 25.5 kg/m2, respectively. None of the patients were smokers. Comorbidities were present in 5.1% of the sample, with hypertension accounting for all the cases. The rate of complications was 41%, which consisted of 7 cases of non-aesthetic scars, 6 cases of bruises, and 4 cases of dehiscence. No patient complained of pain or NAC necrosis, and all patients were satisfied with the surgical result after the 1-year observation period.
Table 1 shows no statistically significant differences with regard to sensitivity of the nipple area between groups for patients with a resected weight of up to 300 g of mammary tissue.
| Time of measurement of nipple sensitivity* | ||||
|---|---|---|---|---|
| Group | 1 | 2 | 3 | 4 |
| Control (n=25) | 96 | 88 | 72 | 92 |
| Experiment (n=21) | 90.5 | 66.7 | 85.7 | 95.2 |
| p-value | 0.188 | 0.085 | 0.343 | 0.718 |
* 1 = before surgery; 2 = 3 weeks postoperatively; 3 = 6 weeks postoperatively; 4 = 1 year postoperatively.
Table 2 shows that no statistically significant difference with regard to sensitivity of the nipple area pre- and postoperatively between groups of patients with resected volume of >300 g of mammary tissue. However, statistical difference was found in the level of sensitivity for the control group at 3 and 6 weeks postoperatively.
| Time of measurement of nipple sensitivity* | ||||
|---|---|---|---|---|
| Group | 1 | 2 | 3 | 4 |
| Control (n=14) | 85.7 | 100 | 100 | 92.9 |
| Experiment (n=18) | 94.4 | 83.3 | 94.4 | 88.9 |
| p-value | 0.123 | < 0.001 | < 0.001 | 0.877 |
* 1 = before surgery; 2 = 3 weeks postoperatively; 3 = 6 weeks postoperatively; 4 = 1 year postoperatively.
Table 3 shows no statistically significant differences with regard to sensitivity of the areola between groups for patients with resected weight of up to 300 g of mammary tissue.
| Time of measurement of areolar sensitivity* | ||||
|---|---|---|---|---|
| Group | 1 | 2 | 3 | 4 |
| Control (n=25) | 100 | 92 | 92 | 96 |
| Experiment (n=21) | 95.2 | 81 | 95.2 | 95.2 |
| p-value | 0.338 | 0.054 | 0.779 | 0.735 |
* 1 = before surgery; 2 = 3 weeks postoperatively; 3 = 6 weeks postoperatively; 4 = 1 year postoperatively.
Table 4 shows no statistically significant differences with regard to areolar sensitivity between groups for patients with resected weight of > 300 g of mammary tissue.
| Time of measurement of areolar sensitivity* | ||||
|---|---|---|---|---|
| Group | 1 | 2 | 3 | 4 |
| Control (n=14) | 100 | 100 | 100 | 100 |
| Experiment (n=18) | 94.4 | 100 | 100 | 100 |
| p-value | 0.07 | 1 | 1 | 1 |
* 1 = before surgery; 2 = 3 weeks postoperatively; 3 = 6 weeks postoperatively; 4 = 1 year postoperatively.
DISCUSSION
The Plastic Surgery Department of the HC-UFPE has the performed dermis resection as a routine activity performed after Schwartzman maneuver in reduction mammoplasties to facilitate migration and reduce distortion of the NAC during breast construction. It is recommended mainly for cases where significant movement of the NAC is needed or when the breast shows a firm parenchyma, with little sliding of overlying skin, meaning that the periareolar dermis sets a limit on the mobilization thereof, and can even cause distortion, thereby having an aesthetic influence upon the final result of the surgical procedure.
The literature showed no studies evaluating the association between NAC sensitivity and dermic resection and the volume of the resected mammary tissue; moreover, the specialized literature shows disagreement regarding NAC sensitivity after reduction mammoplasty. The authors that defend improvement in sensitivity reported that this is a result of the superimposition of dermatomes and the relief of natural chronic traction by the weight of the breasts9,10. Spear2 reported a decline in sensitivity, but this improves for 12 months. However, the various methodologies used make comparison of the results of these papers difficult.
As we can conclude looking at Tables 1 to 4, in the experimental group, for volumes of resected tissue over 300 g, a negative effect was observed on the papillary sensitivity and a positive effect for areolar sensitivity at the end of the monitoring period. In the case of the control group, for resected mammary volume of >300 g, sensitivity was improved both in the papillary and areolar regions.
Despite this, no statistically significant differences were found between the patients of the experimental and control groups, both in the group with resection up to 300 g and those with resection >300 g. However, in the papillary region and considering the control group with resection >300 g, sensitivity improved both 3 and 6 weeks postoperatively. This later becomes equivalent to the result for the experimental group 1 year postoperatively, as proposed in the study by Spear2, on the gradual return of sensitivity.
These findings do not support the findings of Wechselberger et al.10 and Gonzales11, as these studies did not find any association between the quantity of mammary tissue resected and changes to the breast sensitivity postoperatively. However, these articles used different cutoff points from those of the present study: 400 g and 550 g, respectively. However, as we operated on the patients consecutively in this study, we selected a cutoff point of 300 g, this being the most common weight; in the sample; however, we have seen resections of up to 1275 g without any loss of sensitivity.
In the literature, we have also found some criticism on the method of evaluation through microfilaments as proposed by Semmes and Weinstein because they do not bring absolute values and also due to variations between observers; however, the evaluations were made by the same examiner, in the same place, and using the same set of filaments, thus being an easy, reliable and reproducible method for comparisons11. With regard to the observation period, most of the articles published consider 1 year of monitoring as being adequate2,12.
Due to the lack of a statistically significant difference regarding sensitivity between the experimental and control groups, whether for the groups with up to 300 g and >300 g linked to the ease of ascension of NAC and breast construction, it is thus proven that the maneuver, apart from being totally harmless with regard to sensitivity, it may also be safely used in reduction mammoplasty, even in large and bulky breasts.
CONCLUSIONS
In line with the results obtained, considering a significance level of 5%, we conclude that the maneuver for the release of skin did not cause any difference in the sensitivity of the NAC, regardless of the volume of breast tissue resected.
COLLABORATIONS
|
JZS |
Analysis and/or interpretation of data; statistical analysis; final approval of the manuscript; data collection; conceptualization; concept and design of the study; management of resources; project management; investigation; methodology; execution of operations and/ or experiments; writing - preparation of the original; writing - proofreading and editing; software; supervision; validation; visualization. |
|
KK |
Data analysis and/or interpretation; final approval of manuscript; data collection; conceptualization; management of resources; investigation; methodology; execution of operations and/or experiments; writing - preparation of the original, writing - proofreading and editing; software; supervision; validation; visualization. |
|
RHCB |
Statistical analysis; data collection. |
|
ASR |
Statistical analysis; data collection. |
|
ATC |
Data collection; investigation; execution of operations and/or experiments. |
|
ACCRB |
Final approval of the manuscript; writing - preparation of the original. |
REFERENCES
1. Chiari A Jr, Nunes TA, Grotting JC, Cotta FB, Gomes RC. Breast sensitivity before and after the L short-scar mammaplasty. Aesthetic Plast Surg. 2012;36(1):105-14.
2. Spear ME, Nanney LB, Phillips S, Donahue R, Rogers KM, Wendel JJ, et al. The impact of reduction mammaplasty on breast sensation: an analysis of multiple surgical techniques. Ann Plast Surg. 2012;68(2):142-9.
3. Hamdi M, Greuse M, De Mey A, Webster MH. A prospective quantitative comparison of breast sensation after superior and inferior pedicle mammaplasty. Br J Plast Surg. 2001;54(1):39-42.
4. Jaspars JJ, Posma AN, van Immerseel AA, Gittenberger-de Groot AC. The cutaneous innervation of the female breast and nipple-areola complex: implications for surgery. Br J Plast Surg. 1997;50(4):249-59.
5. Fernandes THA, Freitas JOG, Sperli AE. Estudo de alterações de sensibilidade do complexo areolopapilar após mamoplastias com a técnica de retalhos cruzados. Rev Bras Cir Plást. 2012;27(1):73-6.
6. Schartzman E. Die Technik der Mammaplastik. Chirurg. 1930;2:932-43.
7. Mofid MM, Dellon AL, Elias JJ, Nahabedian MY. Quantitation of breast sensibility following reduction mammaplasty: a comparison of inferior and medial pedicle techniques. Plast Reconstr Surg. 2002;109(7):2283-8.
8. Agostini T, De Scisciolo G, Lazzeri D, Almesberger D, Mori A, Cassardo A, et al. Laser- evoked potentials as a novel tool for sensibility assessment following inferior pedicle breast reduction. Eur J Plast Surg. 2013;36(7):423-30.
9. DelVecchyo C, Caloca J Jr, Caloca J, Gómez-Jauregui J. Evaluation of breast sensibility using dermatomal somatosensory evoked potentials. Plast Reconstr Surg. 2004;113(7):1975-83.
10. Wechselberger G, Stoss S, Schoeller T, Oehlbauer M, Piza-Katzer H. An analysis of breast sensation following inferior pedicle mammaplasty and the effect of the volume of resected tissue. Aesthetic Plast Surg. 2001;25(6):443-6.
11. Gonzalez F, Brown FE, Gold ME, Walton RL, Shafer B. Preoperative and postoperative nipple-areola sensibility in patients undergoing reduction mammaplasty. Plast Reconstr Surg. 1993;92(5):809-14.
12. Schlenz I, Rigel S, Schemper M, Kuzbari R. Alteration of nipple and areola sensitivity by reduction mammaplasty: a prospective comparison of five techniques. Plast Reconstr Surg. 2005;115(3):743-51.
1. Hospital das Clínicas, Universidade Federal de
Pernambuco, Cirurgia Plástica, Recife, PE, Brazil.
Corresponding author: Jairo Zacchê de-Sá, Av. República do Libano, nº 251, Bloco A, sala 903 - Pina - Recife, PE, Brazil, Zip Code 51110-160. E-mail: jairozacche@gmail.com
Article received: June 28, 2018.
Article accepted: October 4, 2018.
Conflicts of interest: none.








 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter