

Original Article - Year 2018 - Volume 33 -
Bichectomy and its contribution to facial harmony
Bichectomia e sua contribuição para harmonia facial
ABSTRACT
Introduction: Buccal fat removal was described for the first time by Heister in 1732. In 1802, Bichat identified the adipose nature of this tissue. There is a close association between buccal fat and masticatory muscles, which helps infants suck owing to the sliding motion of the tissues. Its prominence diminishes with age, both through modest reduction in volume and facial growth. Bichectomy or bichatectomy is a surgical procedure that involves extraction of Bichat's fat pad for aesthetic and/or functional purposes. This study aimed to show that bichectomy is a low-risk surgical procedure with good results, provided it is appropriately indicated and is performed following technical standards according to the anatomy of the facial structures.
Methods: This prospective cohort study was conducted between January 2016 and April 2018 and included 59 patients with a mean age of 31 years. The follow-up time was 12-26 months.
Results: Of 59 patients, 46 were female, and 13 were male. All patients underwent same-day surgery. On average, 3.2 mL of fat was removed.
Conclusion: Removal of Bichat's fat according to anatomical principles is safe. This technique can improve facial harmony. Success depends on application of appropriate techniques.
Keywords: Mouth surgery; Reconstructive surgical procedures; Mouth; Fats; Facial asymmetry
RESUMO
Introdução: O tecido gorduroso bucal foi descrito pela primeira vez em 1732, por Heister.
Em 1802, Bichat diagnosticou sua natureza adiposa. Há uma estreita relação
entre a gordura bucal e músculos da mastigação, auxiliando os lactentes na
sucção do leite por atuar com um tecido de deslizamento. Sua projeção
diminui com o aumento da idade, tanto pela redução discreta de seu volume
quanto pelo crescimento facial. A bichectomia ou bichatectomia é o
procedimento cirúrgico que visa remover a "bola gordurosa de Bichat", com
fins estéticos e/ ou funcionais. O objetivo é demonstrar que a bichectomia é
um procedimento de baixo risco cirúrgico e com bons resultados, desde que
seja bem indicada e siga os padrões técnicos, respeitando a anatomia das
estruturas faciais.
Métodos: Estudo prospectivo de coorte, realizado entre janeiro de 2016 e abril de
2018, totalizando 59 pacientes, com média de idade de 31 anos. O tempo de
seguimento foi de 12 a 26 meses.
Resultados: Foram avaliados 59 pacientes,
com média de idade de 31 anos, sendo 46 do sexo feminino e 13 do sexo
masculino. Todos os pacientes receberam alta no mesmo dia. Em média, foram
retirados 3,2ml de volume da gordura de Bichat.
Conclusão: A retirada de porções das gorduras de Bichat é segura, desde que sejam
observados os detalhes anatômicos. Pode oferecer maior harmonia entre os
três terços da face. O sucesso dos resultados depende de uma indicação
precisa para o procedimento.
Palavras-chave: Cirurgia bucal; Procedimentos cirúrgicos reconstrutivos; Boca; Gorduras; Assimetria facial
INTRODUCTION
Buccal fat removal was first described by Heister in 1732; at that time, it was believed that buccal fat was a glandular structure, known as the malar gland. In 1802, Bichat identified the adipose nature of this tissue. There is a close association between buccal fat and masticatory muscles, which helps infants suck owing to the sliding motion of the tissues. Its prominence decreases with age, both due to discrete reduction in volume and facial growth.
Bichat's fat pad is involved in mastication and is also associated with the buccal branch of the facial nerve and parotid duct1. It is 6-mm thick and has a mean weight of 3.9 g in most cases. There is normally a difference in weight (0.51 g on average) between the right and left sides.
Its size is weakly correlated with total body fat, and it has 2 compartments: one yellowish white and another nut-brown. This structure has many clinical applications, such as closure of oronasal fistulas, correction of intraoral defects, repair of palatal defects, covering of maxillary bone grafts, and correction of cleft palate1.
Ever since Egyedi first reported the technique for closure of oroantral communications using Bichat's fat pad, this procedure has become useful in reparatory mouth surgery. Over the last 3 decades, several authors have used Bichat's fat pad to occlude oroantral communications of varied etiologies, whether acute, chronic, or recurring.
The advantages associated with its use include ease of flap availability and a large supply of blood to the receiving bed, which leads to high success rates. Complications are rare when using this technique. In most cases, acceptable aesthetic, phonetic, and masticatory results are obtained².
The adipose tissue in the cheek has 6 extensions scattered around the masseteric, superficial temporal, deep temporal, pterygomandibular, sphenopalatine, and lower orbital regions, and comprises a fat mass lying between the masseter and buccinator muscles³. Despite being histologically similar to other fat deposits in the body, the adipose tissue of the cheeks is not decreased by metabolism, therefore being very similar to orbital fat. In some people, this anatomical structure can give the face a rounded appearance, thereby creating a disharmonic facial contour1.
Bichectomy or bichatectomy is a surgical procedure that removes “Bichat's fat pad” for aesthetic and/or functional purposes. Its main functional indication is for the correction of masticatory problems such as chronic lesions of the jugal mucosa (morsicatio buccarum)1. This is a simple procedure that can be carried out under local anesthesia.
The fat pads are removed through an intraoral incision, thereby allowing a more refined facial appearance; this makes the angles of the mandible more prominent, thereby emphasizing the malar region and diminishing the volume of the lowest third of the face³. The most common complications of this procedure include injuries to Stensen's duct or buccal branch of the facial nerve, which respectively cause a sialocele or salivary fistula and temporary or permanent buccal paralysis, in addition to bruises, facial asymmetry, and rarely postoperative infections. The results of surgery may be observed between 4 and 6 months after soft tissue edema has been reabsorbed3,4.
Clinical evaluation has been the only method available for recommending surgery. In some cases, it is possible to overestimate the volume of Bichat's fat pad through clinical examination alone, but there are few complementary methods that can help surgeons in deciding whether to recommend bichectomy. This means that new methods should be used to avoid possible incorrect recommendations and to clarify patient expectations for the results.
Bichat's fat pad produces linear echogenic images with interspersed conjunctive tissue. For correct evaluation of fat pad volume, it is necessary to apply pressure to this triangular and highly compressible tissue.
Some studies have shown that surgery was not indicated in up to 28.12% of patients, based on the volume of Bichat's fat pad on echography. In these cases, the quantity of Bichat's fat was very small or even absent. Computed tomography can also be used for assessment before surgery; however, this examination entails a significant increase in costs4.
OBJECTIVE
This study aimed to demonstrate that bichectomy is a low-risk procedure with good results, provided technical standards are followed and the anatomy of the facial structures is taken into consideration.
METHODS
This prospective cohort study included 59 patients (46 females and 13 males, mean age of 31 years) who underwent aesthetic bichectomy in an outpatient unit at the Costa Daher Clinic in Brasília, Brazil Federal District, between January 2016 and April 2018. Follow-up time was 12-26 months.
This study included patients who were physically fit non-smokers who wanted to reduce the lateral projection of the inferomedial third of the face. In 1 case, the procedure was not advised because Bichat's fat pad could not be palpated on bidigital examination. No preoperative imaging studies were performed.
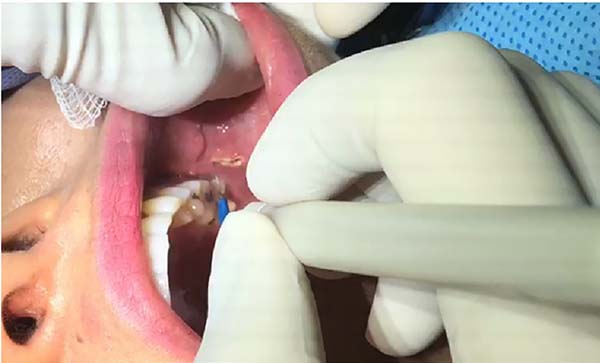
All procedures were performed with attention to anatomical structures, particularly for surgical access, as the location of the parotid duct is the main reference point. The incision in the oral mucosa is made immediately under and slightly behind the duct; the incision is about 1.5 cm long in its greatest length (Figure 1).
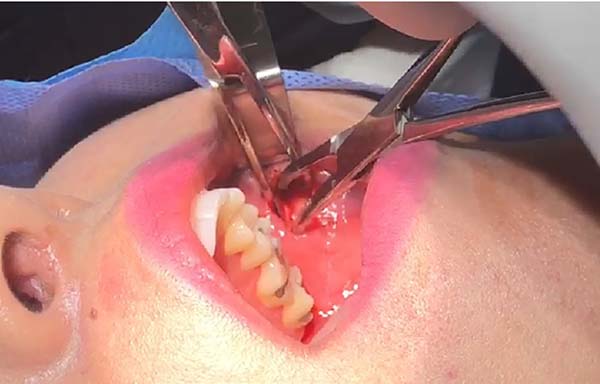
The anatomic planes are carefully dissected, using atraumatic instruments (two Kelly forceps), with attention to essential structures such as branches of the facial artery, the mandible, the parotid duct, and the facial nerve (Figure 2). Soft-tissue forceps are used to manipulate the fat pad and the surrounding fibrous capsule is delicately incised.
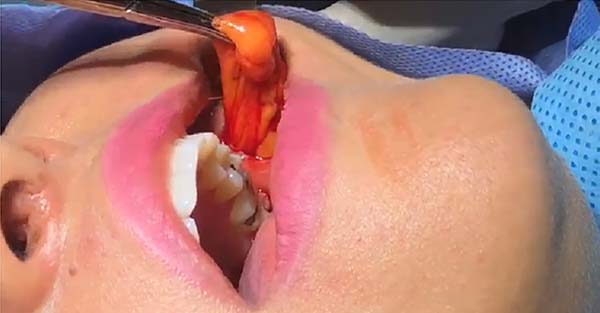
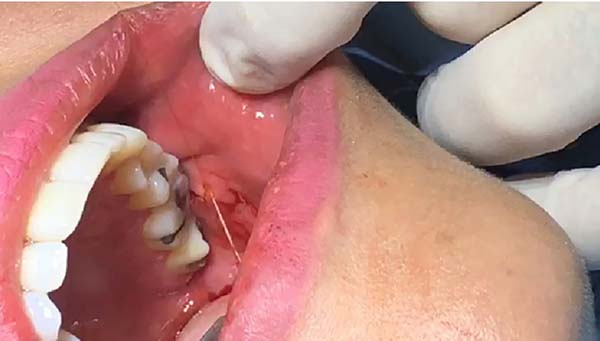
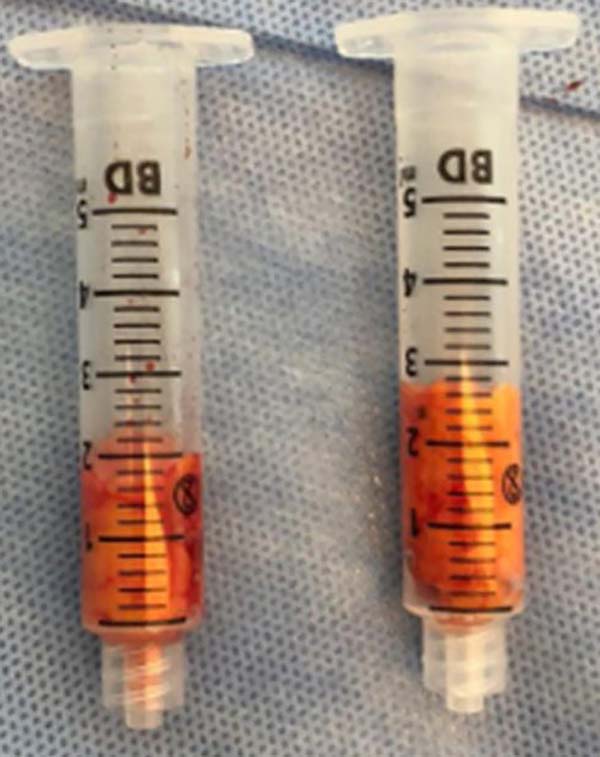
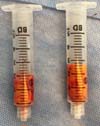
Much of Bichat's fat pad can be excised in a circular pattern, while preserving about one-third of total volume (Figure 3). Tissue is approximated using 5-0 catgut at separate points (Figure 4). The volume removed can be measured with a Luer syringe (Figure 5). Surgical specimens are usually not sent for pathological examination, as this is not formally recommended when no macroscopic changes are observed.
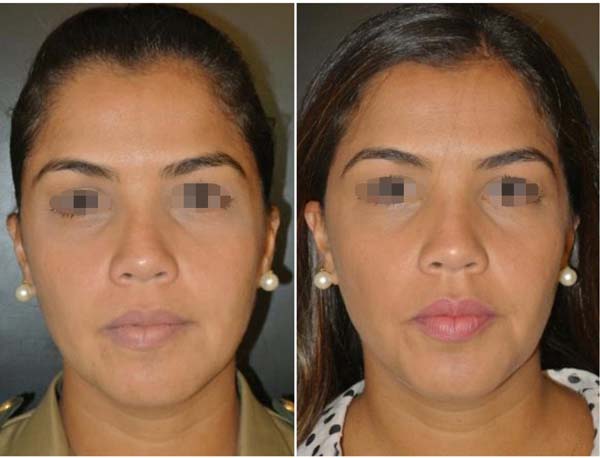
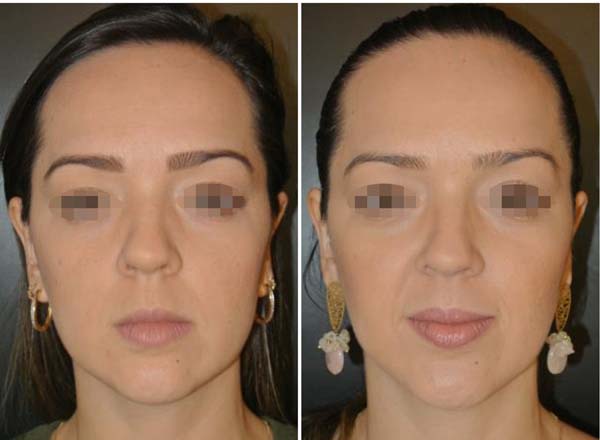
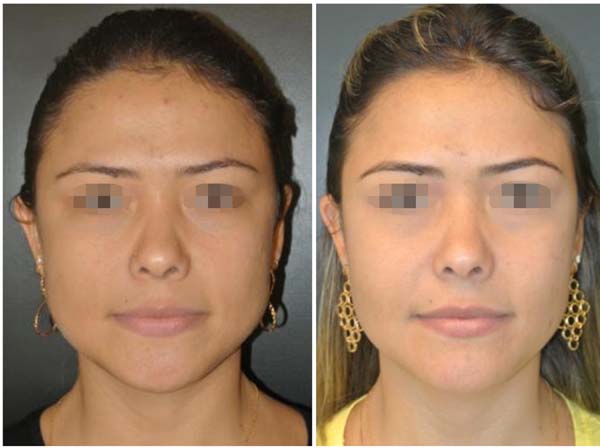
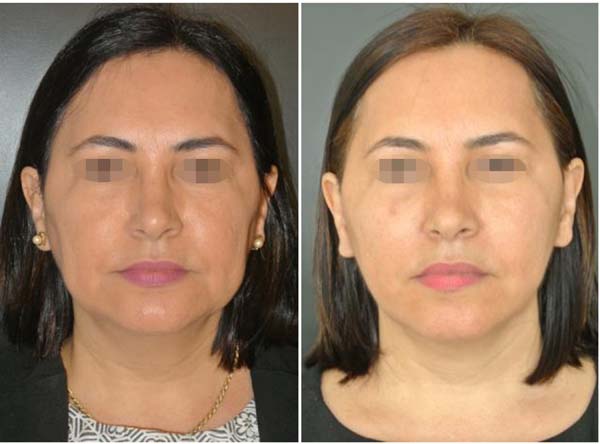
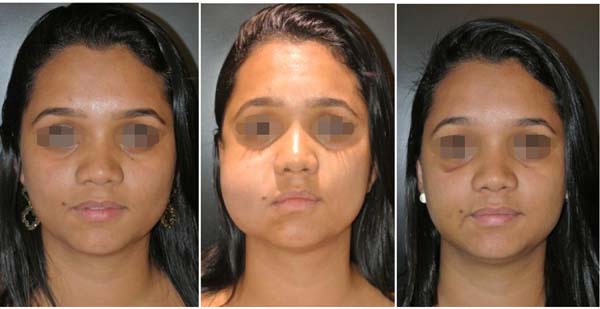
The final results are evaluated by comparing photographs taken before and after the operation (with postoperative photographs taken at 3, 6, and 12 months after surgery). A patient satisfaction survey is performed after at least 12 months.
RESULTS
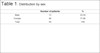
Of 59 patients with a mean age of 31 years (range: 21-53), 46 were female (77.96%), and 13 were male (22.04%). Patient details are shown in Table 1. The procedures were conducted under local anesthesia without sedation, requiring an average of 42 minutes (range: 27-74 minutes). All patients underwent same-day surgery. On average, a volume of 3.2 mL of fat was removed bilaterally (range: 1.2-4.3 mL).
| Number of patients | % | |
|---|---|---|
| Male | 13 | 22.04 |
| Female | 46 | 77.96 |
| Total | 59 | 100 |
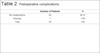
No complications involving branches of the facial nerve (buccal or zygomatic) or Stensen's duct were observed, as shown in Table 2. Photographs (Figures 6 to 10) show a more harmonious cervicofacial contour.
| Number of Patients | % | |
|---|---|---|
| No complications | 58 | 98.31 |
| Bruising | 1 | 1.69 |
| Total | 59 | 100 |
We observed 1 case of bruising (1.69%) (Figure 11) in the period immediately after surgery (2 hours after the procedure); we performed immediate surgical retreatment and found no evidence of active bleeding. This case was managed conservatively and showed spontaneous regression after 7 days. The final aesthetic result was not affected. Four patients expressed dissatisfaction with the result after 6 months, accounting for 6.78% of our total sample. Two of these patients were male and 2 were female, as shown in Table 3.
| Number of patients | % | |
|---|---|---|
| Satisfied | 55 | 93.22 |
| Dissatisfied | 4 | 6.78 |
| Total | 59 | 100 |
DISCUSSION
Facial lipoplasty, also known as bichectomy, is an aesthetic and functional surgical procedure on the face. This facial plastic surgery aims to reduce the size of the cheeks through removal of Bichat's fat pad. This operation is considered fairly simple and can be performed under local anesthesia.
The fat pads are removed through an intraoral incision, giving the face a more slender appearance and emphasizing the angles of the mandible and malar region, while making the lower third of the face less prominent1.
The use of a pediculated Bichat ball for other purposes, including treatment of oroantral communications and bony jaw defects with good results, has been reported. Flaps of mouth fat use a mechanism for lipolysis different from that of subcutaneous adipose tissue; thus, patient age and sex do not affect the outcome with this technique. For this reason, good results have been reported using the mouth fat flap technique, even in elderly patients.
Oroantral communications treated with Bichat's fat range from 2 to 50 mm in diameter. The pedicle flap technique, as proposed by Bichat, also has limitations in cases with major defects, as closure requires traction of a greater volume of tissue, which increases the possibility of complications after surgery, such as aesthetic depression of the cheek. Alkan et al. reported successful closure of bone defects of up to 50 × 30 mm2. Rapidis et al. recommended that the use of this flap be limited to defects smaller than 40 × 40 mm2.
The success of techniques based on flaps of buccal fat has been ascribed to the extensive vascularity of the area close to the receiving bed, the presence of stem cells, consistent volume in most individuals, ease of surgical access, and low rate of complications. Alkan et al. reported that success depended on complete epithelialization of the graft and absence of graft infection, fistula, or defects in the facial contour5.
The aesthetic harm caused by facial asymmetry is obvious and causes social and psychological problems. The introduction of 3-dimensional surgical models using computed tomography has helped to improve the results in patients with facial asymmetry. The autologous transfer of fat is a technique that has been used to correct defects in facial soft tissues, with long-lasting results.
This concept could be used to optimize results after surgery in cases of bichectomy. The autologous fat graft is readily available, biocompatible, malleable, and easily achieved through a minimally invasive procedure. Indeed, the technique for autologous transfer of fat is simple and has minimal complications. Even though overcorrection is performed by many surgeons to compensate for reabsorption, the need and safety have a scientific basis6.
To achieve rejuvenation of the face, it is important to understand the distribution of facial fat and how it changes according to age. Several previous studies have shown that facial fat is highly compartmentalized. The facial fat compartments are independent, thereby forming distinct anatomical units. However, the process of facial aging is not well understood.
It is not clear whether the compartments gain or lose volume, or if they change their shape over time. If we can establish the physiological size and shape of each compartment of facial fat, including changes according to age, we can then redistribute and simulate the distribution of facial fat in younger people7.
Ultrasonography proved to be an effective tool for clinical diagnosis and decision-making, thereby avoiding unnecessary surgery and reducing unrealistic patient expectations, according to Jaeger et al.4. In cases of asymmetry between Bichat's fat pads, there is still doubt as to the recommendation for surgery, since there is a risk of asymmetry in the postoperative period.
Moreover, when the fat pad volume is small, the surgeon should discuss the subtle results that may occur with the patient. Other tools, including computed tomography and nuclear magnetic resonance, may also be used to determine the buccal fat volume. Considering the disadvantages of computed tomography (ionizing radiation and contrast agent exposure) and magnetic resonance imaging (lack of availability, prolonged examination, high cost), we see that ultrasonography is the best choice for evaluation of the volume of Bichat's fat pad4.
In our experience, the bidigital maneuver is sufficient to recommend or advise against the procedure, and imaging examination should only be performed when there are doubts regarding the diagnosis, as these resources can lead to a significant increase in the costs of the procedure.
CONCLUSION
The procedure for removal of portions of Bichat's fat pads (bichectomy or bichatectomy) is safe, provided anatomic features are taken into consideration. This operation can provide greater facial harmony by tapering of the inferomedial third, which makes the appearance of the face more triangular and elegant.
The success of the results depends on appropriate indications for the procedure. For this reason, not all patients are candidates for this surgery, as many have hypertrophy of the masseter muscles and little or no excess of Bichat's fat. As this procedure provides a subtle result, it is essential to establish an appropriate dialogue with the patient to avoid unrealistic expectations.
COLLABORATIONS
|
CADCF |
Analysis and/or interpretation of data; final approval of the manuscript; data collection; conceptualization; conception and design of the study; management of resources; management of the project; investigation; methodology; performance of operations and/ or experiments; writing and preparation of the original; writing, proofreading, and editing; supervision; validation; visualization. |
|
RCSD |
Analysis and/or interpretation of data; data collection; investigation; performance of operations and/or experiments; writing and preparation of the original; writing, proofreading, and editing. |
|
ACC |
Data collection; performance of operations and/or experiments; wording in preparation of the original. |
|
JCD |
Conceptualization. |
|
RSCC |
Data Collection. |
|
LDPB |
Data Collection. |
REFERENCES
1. Ahari UZ, Eslami H, Falsafi P, Bahramian A, Maleki S. The Buccal Fat Pad: Importance And Function. J Dent Med Sci. 2016;15(6):79-81.
2. Alonso-González R, Peñarrocha-Diago M, Peñarrocha-Oltra D, Aloy-Prósper A, Camacho-Alonso F, Peñarrocha-Diago M. Closure of oroantral communications with Bichat´s buccal fat pad. Level of patient satisfaction. J Clin Exp Dent. 2015;7(1):e28-33.
3. Stevao ELL. Bichectomy or Bichatectomy - A Small and Simple Intraoral Surgical Procedure with Great Facial Results. Adv Dent Oral Health. 2015;1(1):1-4.
4. Jaeger F, Castro CHBC, Pinheiro GM, Souza ACRA, Mazzoni Junior GT, Mesquita RA, et al. A novel preoperative ultrasonography protocol for prediction of bichectomy procedure. Arq Bras Odontol. 2016;12(2):7-12.
5. Alkan A, Dolanmaz D, Uzun E, Erdem E. The reconstruction of oral defects with buccal fat pad. Swiss Med Wkly. 2003;133(33-34):465-70.
6. Rapidis AD, Alexandridis CA, Eleftheriadis E, Angelopoulos AP. The use of the buccal fat pad for reconstruction of oral defects: review of the literature and report of 15 cases. J Oral Maxillofac Surg. 2000;58(2):158-63.
7. Peñarrocha-Oltra D, Alonso-González R, Pellicer-Chover H, Aloy-Prósper A, Peñarrocha-Diago M. Closure of oroantral communication with buccal fat pad after removing bilateral failed zygomatic implants: A case report and 6-month follow-up. J Clin Exp Dent. 2015;7(1):e159-62.
8. Wang YC, Wallace CG, Pai BC, Chen HL, Lee YT, Hsiao YC, et al. Orthognathic Surgery with Simultaneous Autologous Fat Transfer for Correction of Facial Asymmetry. Plast Reconstr Surg. 2017;139(3):693-700. DOI: http://dx.doi.org/10.1097/PRS.0000000000003113
9. Gierloff M, Stöhring C, Buder T, Gassling V, Açil Y, Wiltfang J. Aging changes of the midfacial fat compartments: a computed tomographic study. Plast Reconstr Surg. 2012;129(1):263-73. PMID: 21915077 DOI: http://dx.doi.org/10.1097/PRS.0b013e3182362b96
1. Clínica Costa Daher, Cirurgia Plástica,
Brasília, DF, Brazil.
Corresponding author: Cesar Augusto Daher Ceva Faria, SGAS 611, Lt. 74, Bloco 2, Salas 132 a 134 - Asa Sul, Brasília, DF, Brazil, Zip Code 70200-700. E-mail: cesardaher@costadaher.com.be
Article received: August 9, 2018.
Article accepted: November 11, 2018.
Conflicts of interest: none.











 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter