

Reviw Article - Year 2018 - Volume 33 -
Speech therapy and orthognathic surgery: a literature review
Fonoaudiologia e cirurgia ortognática: revisão de literatura
ABSTRACT
Introduction: Dentofacial deformities are associated with
changes in dental occlusion, which may cause changes in the
myofunctional system according to the type of disproportion.
These deformities can cause changes and/or adaptations in
the stomatognathic system. The objective of this study was
to identify the relationship between speech therapy and
orthognathic surgery based on refereed publications.
Method:
A bibliographic survey was conducted without considering a
specific publication period in the databases, PubMed, SciELO
and BVS.
Results: Fifteen articles were critically evaluated
with respect to the type of study, objectives, number and sex
of participants, methodology, results and conclusions. Based
on their aims, the articles were grouped into 1) speech-therapy
group (STG); 2) changes group (CG); 3) techniques group
(GT) and 4) others group (OG).
Conclusion: There is little
information regarding direct speech therapy intervention,
and the majority of the studies were directed to the aesthetic
and functional changes in the hard and soft tissue in patients
who underwent orthognathic surgery. Some studies addressed
methods and/or specific examination procedures to verify
the changes in the soft and hard tissues of the facial profile
of patients who underwent orthognathic surgery, and a study
detailed the profile of individuals who underwent treatment
for dentofacial deformity and apnea-hypopnea syndrome.
Keywords: Speech therapy; Orthognathic surgery; Stomatognathic system; Maxillomandibular abnormalities; Esthetics; Physiology
RESUMO
Introdução: As deformidades dentofaciais estão associadas às alterações de oclusões
dentárias, que podem causar modificações no sistema miofuncional de acordo
com o tipo de desproporção. Essas deformidades, podem provocar alterações
e/ou adaptações no sistema estomatognático. O objetivo desse estudo foi
identificar, com base na literatura arbitrada, a relação entre a
Fonoaudiologia e a Cirurgia Ortognática.
Método: Foi realizado levantamento bibliográfico sem período específico, nas bases de
dados PubMed, SciELO e BVS.
Resultados: Foram avaliados 15 artigos de forma crítica, quanto ao tipo de estudo, seus
objetivos, número e gênero dos participantes, metodologia, resultados e
conclusões. Os artigos foram agrupados com base nos seus objetivos em 1)
Grupo Fonoaudiologia (GF); 2) Grupo Mudanças (GM); 3) Grupo Técnicas (GT) e
4) Grupo Outros (GO).
Conclusão: Pouco se encontrou sobre a intervenção fonoaudiológica direta, sendo a
maioria dos estudos direcionada às mudanças estéticas e funcionais do tecido
duro e mole de pacientes submetidos à cirurgia ortognática. Houve também
estudos que abordaram métodos e/ou exames específicos para verificar as
mudanças nos tecidos moles e duros do perfil facial dos pacientes submetidos
à cirurgia ortognática e estudo que detalhou o perfil dos indivíduos que
realizaram tratamento para deformidade dentofacial e síndrome da Apneia e
Hipopneia do Sono.
Palavras-chave: Fonoaudiologia; Cirurgia ortognática; Sistema estomatognático; Anormalidades maxilomandibulares; Estética; Fisiologia
INTRODUCTION
Dentofacial deformities (DFD) are defined as severe skeletal changes associated with alterations in dental occlusion1,2. These deformities lead to modifications in the myofunctional system depending on the type of disproportion. Such modifications include alterations in the functions of chewing, swallowing, breathing, and speech, temporomandibular disorders (TMD), alteration in the usual posture of the lips and tongue, and muscular asymmetry3. The modifications in the orofacial myofunctional system (OMS) are due to muscular responses, called muscular adaptations, necessary for the functioning of the stomatognathic system (SS)2,3.
Literature indicates that skeletal and occlusal alterations can be caused by alterations in the OMS, and the latter could direct the bone growth of the face4, bringing together speech sciences and plastic surgery.
Orthognathic surgery (OS) is performed to correct maxillomandibular bone disproportions and, consequently, provide a balance between the stomatognathic functions and harmony between the anatomical structures5. Planning of this procedure is performed in conjunction with the surgeon and orthodontist, and the contribution of the speech therapist in this step is crucial, because this professional identifies the orofacial myofunctional alterations present and allows the planning of a possible rehabilitation program in order to provide greater stability in the surgical results2.
The role of the therapist in the team responsible for patients with indication for surgical procedures to reposition the bone bases is important, but it is still a field that is being explored. The speech therapist who operates in the area of OS contributes to a better neuromuscular reorganization after the surgical procedure by correcting the form and reshaping the tissues, and seeking a balance between the anatomic functions and the SS.
For these reasons, speech therapy services within the interdisciplinary team are important to assist in the accomplishment of a proper prognosis and contribute to the harmonious implementation of the SS2,5,6.
The speech therapist, when part of the OS interdisciplinary team, performs important functions such as evaluation of the SS in the pre-operative and post-operative periods. They can offer the patient and the team a comparison between the evaluations at different moments, verifying the characteristics, compensations and adaptations presented2.
Speech therapy before and after surgery is assessed according to the service and in accordance with the specific characteristics of each patient2. The authors suggest that in each moment of the intervention, the therapist plays an important role, beginning with the preoperative phase and continuing to be involved till the postoperative period.
Several studies have explained each phase of speech-language intervention, detailing the aims of the therapy2,5. In the preoperative phase, it is recommended that interventions be carried out in one and three months prior to surgery, aiming to provide guidance and clarification on the perception of the mechanisms and correct muscle patterns during the conduct of the oral functions and rest. This moment of action is critical, because this information will postoperatively contribute to the sensory impulses to be sent to the central nervous system, and constitute a new proprioceptive system5.
In the post-surgical period, the speech therapist can begin assessment immediately after the surgery or within approximately 20 to 60 days after the procedure, depending on the service rendered by the therapist and the time the patient is discharged by the surgeon. The process can be divided in two phases: immediate postoperative period (intermaxillary fixation and restriction) and the therapy itself.
In the initial period, this professional should reiterate their guidance and perform a preventive analysis to identify the structures of the SS that may lead to instability in the postoperative period. After this phase, the therapy can be initiated, during which the characteristics presented by the patient should be evaluated for possible changes and/or adaptations in soft tissues, postural, muscular and functional disorders. From this evaluation, the initiation of muscular exercises, gradual reintroduction of feeding, sensitization work, and others that are listed according to the needs of the patient may be carried out2,5.
For speech-language therapy in OS, the patients must be dedicated and must contribute towards achieving the proposed goals. With adequate performance and automation of SS functions, speech therapy discharge can be determined, with more spaced sessions eventually being required to enable the speech-language pathologist to ensure that recurrence does not occur5.
OBJECTIVE
Given the above, the objective of this study was to identify the relationship between speech therapy and OS in refereed publications.
METHOD
The precepts of the Cochrane Handbook were followed to establish the research method7.
The location and selection of studies was conducted by a search of published texts, without a specific time period, in the following databases: PubMed SciELO, and BVS. In the PubMed database, the articles selected were limited to studies conducted in humans, in English and Portuguese, using the descriptors: “orthognathic surgery and clinical protocols and speech therapy,” “orthognathic surgery and therapy and speech therapy,” and “orthognathic surgery and therapeutics and speech therapy.”
In the SciELO and BVS database the descriptors used were: “Cirurgia ortognática e protocolos clínicos,” “Cirurgia ortognática e terapia,” and “Cirurgia ortognática e terapêutica,” and were limited to studies carried out in humans, in Portuguese or English languages.
The text search in the databases was performed independently by the researchers, aiming to minimize citation losses. The analysis of each of the citations retrieved in the database was also performed independently by the researchers. Initially, the analysis of the titles and abstracts of the citations was performed, to identify the pertinence of their selection and inclusion in the study. Citations in languages other than English and Portuguese were excluded, as were repeated overlapping keywords. Also excluded were studies related to literature reviews, letters to the editor and those that were not directly linked to the topic.
In a second phase, the complete texts selected by researchers which were effectively related to the research proposal were read in full. Publications which could not be recovered in full through the CAPES Journal Portal and/or the official site of the journal were also excluded.
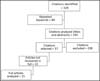
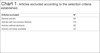
All stages of the study were conducted independently by the researchers and, when any discordance was identified, the final position was determined by consensus. Figure 1 shows the article selection strategy used in this study, while Chart 1 presents a summary of the reasons for study exclusion.
| Articles excluded | Nº |
|---|---|
| Review articles | 08 |
| Articles with non-primary themes | 170 |
| Articles without abstracts | 08 |
| Articles not freely available | 22 |
The 15 articles selected were evaluated critically regarding the type of study, objectives, number, and gender of participants, age, criteria and methods, results and conclusions. In relation to the criteria and methods, we sought to verify and describe the methodology employed in each one of the studied articles, in order to analyze whether there was homogeneity among them. A general description of the results and conclusions section was performed, as presented by the articles.
RESULTS AND DISCUSSION
The overall results of the study are briefly described in Chart 2.
| References | Objectives | Methods | Results/Conclusions |
|---|---|---|---|
| Migliorucci et al., 20178 | To propose a myofunctional therapy program for individuals who underwent OS. | 3 distinct stages: 1) Preparation of an initial program from a literature review about the therapeutic process after surgery; 2) Implementation of the initial program in 21 patients which resulted in a second version of the program; 3) Content analysis by three speech therapists and new modifications were carried out. | The program was developed based on 38 scientific publications. After the suggestions of specialists, the final version was composed of 12 sessions - Evaluation + 10 therapy sessions once a week (myofunctional exercises, sensory stimulation and functional training) + revaluation. It was possible to develop a program of orofacial myofunctional therapy for patients who underwent OS. |
| Lima et al., 20152 | To describe the case of a patient who underwent OS and the speech accompaniment in the preoperative and postoperative periods, as well as to evaluate the impact of the dentofacial deformity on quality of life. | Case study of a patient with Class III malocclusion. The evaluation was performed by means of the MBGR Evaluation Protocol with scores. The speech intervention occurred in the preoperative period (three months) and postoperative beginning on the 20th postoperative day (for three months). The impact of dentofacial deformity in the quality of life of the patient was assessed by means of Oral Health Impact Profile - reduced version. | Improvement in muscular mobility, reduced pain on palpation, tonus balance, more efficient chewing, alternate bilateral, appropriation of the swallowing pattern and adequacy of speech production, and improvement in quality of life. |
| Palomares, 20141 | To evaluate the quality of life related to oral and specific health of ortho- surgical patients taking into consideration the following aspects: - esthetic self-perception of patients; - clinical characteristics of malocclusions; - gender, age, socioeconomic status. | A total of 254 patients were divided into four groups, according to the stage of treatment: Initial (pre-treatment), in orthodontic preparation for OS, in post-surgical orthodontic finalization and containment (after completion of treatment). They were interviewed in three major centers of Rio de Janeiro. Quality of life was assessed by the OHIP-14 and OQLQ questionnaires. The severity of malocclusion and esthetic self-perception were assessed on the basis of the Index of Orthodontic Treatment Need (IOTN) and the Dental Esthetic Index (DAI). | The patients who completed all the steps of orthosurgical treatment showed significant improvement in specific quality of life relating to oral health, compared to the other groups. The esthetic self-perception of the containment groups and the post-surgical procedure was more positive than in other groups. Clinical characteristics that can be correlated with negative impacts on quality of life: crowding, crossbite, open bite. Correlation between the OHIP-14 and OQLQ instruments was moderate, confirming that they assess different aspects of oral health-related quality of life. OQLQ demonstrates greater sensitivity in detecting changes in the quality of life of ortho-surgical patients than OHIP-14. |
| Alves e Silva et al., 20139 | To compare the changes related to self-esteem and satisfaction with the appearance between pre and postoperative phases in patients submitted to OS and evaluate the quality of life of these patients six months after the surgery. | A study was conducted on 15 patients, randomly selected, with dentofacial deformities, who underwent OS in the Oswaldo Cruz University Hospital of the University of Pernambuco. The study had a follow-up period of six months, with two stages: 1) Pre-operative (day of hospitalization): application of a questionnaire to assess patients’ satisfaction with their appearance and social relations; and 2) in the post-operative period (six months after surgery), using application Form I which evaluated the same variables of the pre and the WHOQOL-bref. | The results showed that 13.3% of the patients had improvement of esteem, especially in relation to the satisfaction of appearance. Improvements were also observed in social, professionals and family relations. With regard the assessment of the quality of life, and in accordance with the questionnaire of the World Health Organization, the lowest average improvements corresponded to environmental control. |
| Jakobsone et al., 201310 | To analyze changes in facial profile of the soft tissue after bimaxillary surgery of Class III correction, with the objective of determining if a decrease or increase in the height of the face affects the changes in profile, with an emphasis in the anteroposterior direction. | Sample comprised 84 operated patients with Le Fort I osteotomy + bilateral sagittal osteotomy with rigid fixation. The surgery was performed in Oslo University Hospital, Ullevaal, between 1990 and 2003. The patients were monitored over 3 years - T1: one week before surgery; T2 one week after surgery; T3, T4 and T5: 2, 6 and 12 months after surgery, and T6: 3 years after surgery. Cephalometry of 81 patients (55 men and 26 women were evaluated. The patients were divided into three subgroups according to the change in the anterior facial height during surgery (1 = no change group - less than 2 mm shift in the in the anterior face height; 2 = decrease group - decrease of 2 mm or more in the anterior face height; 3 = increase group - increase of 2 mm or more in the anterior facial height. Calculations of soft and hard tissue ratios were based on long-term soft tissue response to surgical repositioning. | The soft and hard tissues followed the same pattern of changes in male and female patients, with the exception of point B in soft tissues. The horizontal surgical repositioning varied, depending on whether the anterior facial height was increased or decreased. For the prominence of the upper lip, the pattern of long-term change was the same regardless of changes in facial height. In all groups, the thickness of the upper lip decreased in both the short- and long-terms, particularly in patients with surgical increase in facial height. The inferior thickness of the lips increased in the short term, but decreased during the follow-up period. There were significant associations between tissues and the corresponding changes in hard tissues, with the exception of point A of the soft tissue and the upper lip, when the facial height increased. The proportions were higher for mandibular variables than for maxillary variables, particularly at point B and pogonion when the height of the anterior face reduced. The different changes in the patterns of soft tissue should be taken into consideration during the planning of the degree to which maxillary advances and mandibular recesses would be made. |
| Rustemeyer & Martin, 201311 | To evaluate the response of facial tissues in patients with Class II and III facial pattern treated with bimaxillary OS, evaluated cephalometrically and by 2-D photogrammetry; To compare the capacity of the exams to predict postoperative results. | 28 patients who underwent bimaxillary surgery for a correction of Class II, and 33 patients who underwent bimaxillary surgery for the correction of Class III. The lateral cephalogram and a lateral photogram were analyzed in two moments - before the dental treatment and after 9 months of the surgery. | No significant differences were found between men and women, in the results of cephalometry or photogrammetry. Angles of hard tissues changed significantly in the comparison between the pre- and post-operative periods in Class II and Class III surgical procedures. The pre- and post-operative measures of soft tissues did not differ between the methods of evaluation. This study revealed that cephalometry and 2-D photogrammetry provide additional information to improve the accuracy in predicting changes in the tissues in orthosurgical surgery, especially in skeletal Class II patients. |
| Chen et al., 201212 | To assess changes in facial profile after osteotomy in the vertical branch to correct mandibular prognathism. | 30 patients (20 females and 10 males, with an average age of 20.7 years) who needed surgical correction for mandibular prognathism were treated at the Kaohsiung Medical University Hospital from January 1993 to December 1998. The average time of follow-up of these patients was 27.2 months (12 and 102 months). To evaluate the changes in the profile after surgery, two periods of cephalometry registration – pre-operative T1 and T2 were done one year after the surgical procedure, in which markings were performed, and the same were compared. | Significant horizontal changes were observed in relation to T1 and T2. The mean horizontal retreat of the pogonion point (Pog) was 11.7 mm. The ratio of the retreat of the lower labial (Li) / lower incisor (Li), labiomental (Si) / B-point, and soft tissue (PogS) / pogonion points were 0.98, 0.99 and 0.95, respectively. No differences were identified in relation to sex. A satisfactory treatment plan for people with mandibular prognathism not only corrects malocclusion but also considers facial improvement. |
| Bergamo et al., 201113 | To present the treatment of skeletal malocclusion Class III with transversal alteration and facial asymmetry, whose magnitude required orthodontic and surgical treatment. | A male patient with 15:1 years, was brought into the orthodontic clinic of Ribeirão Preto School of Dentistry, USP, with the main complaint of occlusal changes. Facial analysis indicated sharp facial asymmetry, slightly concave facial bones, maxillary hypoplasia, increase of the lower third of the face, Class III, narrow maxilla, posterior open bite, deviation of mean line of maxilla to the right. | At the end of the treatment functional occlusion, overjet, overbite and adequate intercuspation were observed. Mandibular prognathism and facial asymmetry were eliminated. In the case presented, the ortho-surgical treatment was well indicated, promoting adequate masticatory function and adequate facial esthetics. |
| Gornic et al., 201114 | To evaluate and quantify, through cephalometry, changes caused in the airways due to the OS involving mandibular setback. | 17 patients submitted to ortho-surgical treatment for Class III correction were selected. Among the patients evaluated, 14 underwent combined OS of maxillary advancement and mandibular indentation; while in the others, mandibular setback was performed alone. Pre-operative cephalometric profile radiographs were evaluated, up to 7 months before surgery, and immediate post-operative radiographs, up to one week after surgery. | The mean setback of the mandible was 7.32 mm after the surgery. The impact on the airspace was evidenced by an average reduction of 0.97 mm at the level of the oropharynx and 3.41 mm at the level of the hypopharynx as the initial mean diameter of these spaces was 16.88 mm and 13.05 mm, respectively. This reduction was statistically significant only in the region of the hypopharynx (p = 0.025). |
Based on the objectives, the studies were grouped into four categories, namely: 1) speech-therapy group (STG) = studies addressing speech and/or direct therapy intervention2,8; 2) changes group (CG) = studies that reported esthetic and functional changes in hard and soft tissue1,6,9-16; 3) techniques group (TG) = studies that describe specific tests and/or methods to verify changes in hard and soft tissues17,18 and 4) others group (OG) = studies that did not fit the objectives of the previous groups19 (Figure 2).
Regarding types of studies, majority were found to be longitudinal descriptive studies (46.5%)5,8-11,13,16, followed by cross-sectional descriptive studies (26.5%)1,16,18,19 and case reports (20%)2,13,15. Only one study was a theoretical descriptive type (7%)8.
Figures 3 and 4 detail the mean ages in each group, as well as the more prevalent sex in the studies. It should be noted that some studies did not perform such classifications, therefore the data were not presented in the charts.
In general, adult individuals with completed craniofacial growths were considered. The literature recommended that indication for OS should be determined after the completion of craniofacial growth, considering available orthodontic and surgical resources, in order to correct maxillary and/or mandibular deformities. This is because orthodontic treatment alone is unlikely to correct the deformities20.
Women underwent OS significantly more often than men in selected studies. This finding is comparable to those of previous studies that claim that more women OS21, in general because women have greater concerns about their health and esthetics, and seek treatment more frequently22.
Analysis of the articles based on the methodology used and according to the groups stipulated in the study indicates that in the STG, one study2 is a case report, and another article8 is a theoretical descriptive study that describes the elaboration of a speech therapy program for patients undergoing OS and the process of their content validation. In the CG, most articles used longitudinal descriptive studies6,9-12,14, and in the majority of the papers, the study was conducted in the university hospitals in the country and/or abroad or in reference to national hospitals. In this group, two other articles13,15 were case reports.
In the TG, a study that used a longitudinal descriptive approach was carried out in the United Kingdom while another using a cross-sectional study design did not specify the location of study. In the OG, a longitudinal descriptive study that took place in a medical school in the state of São Paulo was identified.
In general, majority of the studies were performed in university hospitals. Literature indicates that these institutions must integrate research, teaching, and care, and this premise is noted in the official definition of a university hospital, which was published on the MEC website, one of the governing bodies and maintainers of university hospitals in Brazil23. This finding may be related to the principles of Brazilian university hospitals, as stated in the literature23, which explains that the main hospitals in the world are recognized not only as centers of education and care, but, above all, as knowledge centers.
With respect to the results and conclusions of the studies, the researchers found improvement in quality of life, in the functions of the stomatognathic system, and mobility and tonus of the muscles in the STG, which may be confirmed by means of standardized clinical protocols2. In one study8, the researchers managed to develop and validate the content of a speech program that contains evaluation, therapy (involving orofacial myofunctional exercises, sensory stimulation and functional training) and reevaluation.
In the CG, the researchers’ findings in general were: 1) increased confidence after completion of OS, mainly in relation to satisfaction of appearance; 2) improvements in social, professional and family relations; 3) significant reduction in facial height due to mandibular repositioning; 4) decrease in the thickness of the upper lip, both in the short- and long-terms, particularly in patients with surgical increase in facial height; 5) an increase in the thickness of the lower lip in the short-term, although it decreased in the follow-up. Furthermore, several studies reported no significant differences in changes between soft or hard tissues between males and females, schooling and family income; changes in the marker points of soft tissue when pre- and post-surgical results were compared, as well as improvements in facial esthetics.
In the GT group, researchers17 showed no statistically significant differences between two methods of superposition, namely, Voxel-based registration and 3-D evaluation. However, surface-based registration displayed high variability in mean distances between the corresponding surfaces compared to the Voxel registration, especially in soft tissues. Within each method, there was a significant difference between the overlays of the hard and soft tissue models. Researchers18 reported that the proposed method significantly aided in diagnosis, prognosis, teaching parameters for facial analysis in orthodontics and OS, and in patient guidance and patient follow-up.
The TG is related to CG for this analysis, since the researchers used several techniques and/or exams to verify the anatomical changes in hard and soft tissues, and esthetic and functional changes in their studies. Such techniques include tomographic imaging, surface electromyography (EMG) examination, pressure measurement system exam, gypsum models, facial analysis, periapical radiography, 2-D photogrammetry and, most commonly, cephalometry.
Thus, both groups deal with examinations and/or objective procedures which sought to evaluate the changes in soft and hard tissues in the pre- and post-operative periods to evaluate masticatory function, and to compare and verify changes, stability and relapse. Based on the literature, we can state that the examinations and procedures used in these two groups are important to enable speech therapists, orthodontists and oral and maxillofacial surgeons use the required parameters to perform a proper diagnosis, pre- and post-surgical evaluations and treatment. These data need to be precisely documented to ensure the best possible outcome for each patient24.
CONCLUSION
The objective of this review was to identify the relationship between speech therapy and OS. During the literature search, little information was found on direct speech therapy intervention, and most of the studies were directed to esthetic and functional changes in the hard and soft tissue of patients who underwent OS. Some studies addressed specific methods and/or exams to verify soft and hard tissue changes in the facial profile of patients who underwent OS and one study detailed the profile of individuals who underwent treatment for dentofacial deformity and apnea-hypopnea syndrome.
COLLABORATIONS
|
MFNS |
Analysis and/or interpretation of data; conception and design of the study; completion of surgeries and/or experiments; writing the manuscript or critical review of its contents. |
|
LDMT |
Analysis and/or interpretation of data; aprovação final do manuscrito; conception and design of the study; completion of surgeries and/or experiments; writing the manuscript or critical review of its contents. |
REFERENCES
1. Palomares NB. Impacto das etapas do tratamento orto-cirúrgico na qualidade de vida de pacientes portadores de deformidades dentofaciais [Dissertação de mestrado]. Rio de Janeiro: Faculdade de Odontologia, Universidade do Estado do Rio de Janeiro; 2014.
2. Lima JAS, Luna HB, Pessoa LSF, Alvez GAS. Ganhos funcionais mensurados pelo MBGR e impacto na qualidade de vida em sujeito submetido à cirurgia ortognática: relato de caso. Rev CEFAC. 2015;17(5):1722-30. DOI: http://dx.doi.org/10.1590/1982-021620151751015
3. Pereira JBA, Bianchini EMG. Caracterização das funções estomatognáticas e disfunções temporomandibulares pré e pós cirurgia ortognática e reabilitação fonoaudiológica da deformidade dentofacial classe II esquelética. Rev CEFAC. 2011;13(6):1086-94. DOI: http://dx.doi.org/10.1590/S1516-18462011000600015
4. Moss ML. The functional matrix hypothesis revisited. 3. The genomic thesis. Am J Orthod Dentofacial Orthop. 1997;112(3):338-42. PMID: 9294365 DOI: http://dx.doi.org/10.1016/S0889-5406(97)70265-8
5. Aléssio CV, Mezozono CL, Körbes D. Intervenção Fonoaudiológica nos casos de pacientes classe III com indicação à Cirurgia Ortognática. Arq Odontol. 2007;43(3):102-10.
6. Almeida RCC. Avaliação tridimensional da alteração estabilidade do tecido mole decorrentes da cirurgia de avanço mandibular [Dissertação de mestrado]. Rio de Janeiro: Universidade do Estado do Rio de Janeiro; 2009.
7. Higgins JPT, Grenn S. Cochrane Handbook for Systematic Reviews of Interventions Version 5.0.2, updated September 2009 [acesso 2017 Maio 8]. Disponível em: http://training.cochrane.org/handbook
8. Migliorucci RR, Passos DCBOF, Berretin-Felix G. Programa de terapia miofuncional orofacial para indivíduos submetidos à cirurgia ortognática. Rev CEFAC. 2017;19(2):277-88. DOI: http://dx.doi.org/10.1590/1982-021620171921317
9. Alves e Silva AC, Carvalho RA, Santos Tde S, Rocha NS, Gomes AC, de Oliveira e Silva ED. Evaluation of life quality of patients submitted to orthognathic surgery. Dental Press J Orthod. 2013;18(5):107-14. DOI: http://dx.doi.org/10.1590/S2176-94512013000500018
10. Jakobsone G, Stenvik A, Espeland L. Soft tissue response after Class II bimaxillary surgery. Angle Orthod. 2013;83(3):533-9. DOI: http://dx.doi.org/10.2319/043012-356.1
11. Rustemeyer J, Martin A. Soft tissue response in orthognathic surgery patients treated by bimaxillary osteotomy: cephalometry compared with 2-D photogrammetry. Oral Maxillofac Surg. 2013;17(1):33-41. DOI: http://dx.doi.org/10.1007/s10006-012-0330-0
12. Chen CM, Lai S, Lee HE, Chen KK, Hsu KJ. Soft-tissue profile changes after orthognathic surgery of mandibular prognathism. Kaohsiung J Med Sci. 2012;28(4):216-9. DOI: http://dx.doi.org/10.1016/j.kjms.2011.10.018
13. Bergamo AZ, Andrucioli MC, Romano FL, Ferreira JT, Matsumoto MA. Orthodontic-surgical treatment of Class III malocclusion with mandibular asymmetry. Braz Dental J. 2011;22(2):151-6. DOI: http://dx.doi.org/10.1590/S0103-64402011000200011
14. Gornic C, Nascimento PP, Melgaço CA, Ruellas ACO, Medeiros PJD, Sant'Anna EF. Análise cefalométrica das vias aéreas superiores de pacientes Classe III submetidos a tratamento ortocirúrgico. Dental Press J Orthod. 2011;16(5):82-8. DOI: http://dx.doi.org/10.1590/S2176-94512011000500013
15. Dalla-Bona DE, Matsumoto E, Tanaka E, Tanne K. Tratamento ortognático de um paciente com assimetria mandibular severa e disfunção dos músculos mastigatórios -Relato de um caso clínico. Rev Fac Odontol. 2005;46(1):80-9.
16. Veronez FS, Tavano LDA. Modificações psicossociais observadas pós-cirurgia ortognática em pacientes com e sem fissuras labiopalatinas. Arq Ciênc Saúde. 2005;12(3):133-7.
17. Almukhtar A, Ju X, Khambay B, McDonald J, Ayoub A. Comparison of the accuracy of voxel based registration and surface based registration for 3D assessment of surgical change following orthognathic surgery. PLoS One. 2014;9(4):e93402. DOI: http://dx.doi.org/10.1371/journal.pone.0093402
18. Maniglia JV, Molina FD, Marques CG. Proposta de análise fotográfica do perfil facial em cirurgia ortognática. Rev Med. 2009;88(3/4):168-74. DOI: http://dx.doi.org/10.11606/issn.1679-9836.v88i3/4p168-174
19. Marques CG, Maniglia JV, Molina FD. Service profile of Orthognathic Surgery of a medical school. Braz J Otorhinolaryngol. 2010;76(5):600-4. DOI: http://dx.doi.org/10.1590/S1808-86942010000500011
20. Mamani MH. Preparo ortodôntico em casos de cirurgia ortognática [Monografia]. Piracicaba: Universidade Estadual de Campinas, Faculdade de Odontologia de Piracicaba; 2013.
21. Faber J, Faber APMH. Percepções das deformidades dentofaciais: do bem-estar psíquico à indicação de cirurgia. Dental Press J Orthod. 2010;15(4):13-4. DOI: http://dx.doi.org/10.1590/S2176-94512010000400002
22. Zaroni FM. Características de 485 cirurgias ortognáticas realizadas em um serviço de cirurgia e traumatologia bucomaxilofacial [Dissertação de mestrado]. Curitiba: Universidade Federal do Paraná; 2015.
23. Araújo KM, Leta J. Os hospitais universitários federais e suas missões institucionais no passado e no presente. Hist Ciênc Saúde. 2014;21(4):1261-81.
24. Yoshida MM, Câmara PRP, Goldenberg DC, Alonso N. Padronização de avaliação em cirurgia ortognática. Rev Soc Bras Cir Craniomaxilofac. 2007;10(4):125-32.
1. Faculdade de Ceilândia, Universidade de
Brasília, Ceilândia, DF, Brazil.
Corresponding author: Laura Davison Mangilli Toni, Faculdade de Ceilândia, Centro Metropolitano, Conjunto A, Lote 1 - Brasília, DF, Brazil. Zip Code 72220-900. E-mail: davisonmangilli@yahoo.com.br
Article received: January 30, 2018.
Article accepted: September 5, 2018.
Conflicts of interest: none.










 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter