

Original Article - Year 2018 - Volume 33 -
Reconstruction of the papilla and immediate tattooing of the nipple-areola complex: the technique, results, and a literature review
Reconstrução da papila e imediata tatuagem do complexo areolopapilar: técnica, resultados e revisão de literatura
ABSTRACT
INTRODUCTION: The reconstruction of the nipple-areola complex (NACRec) is the final stage of breast reconstruction; and tattooing the nipple-areola complex (NAC) is well established as effective, although not widespread among Brazilian plastic surgeons. We have shown a simple method of NACRec using skin flaps for the preparation of the papilla and immediate tattooing of the NAC, shortening the recovery of the patient and avoiding new surgeries.
METHODS: We performed a retrospective study of patients submitted to NACRec in our private clinic, from September 2015 to December 2016. We also searched the Medline database from 2004 to 2016 for reports of diseases associated with tattooing.
RESULTS: Twenty-six patients underwent 28 reconstructions of the nipple-areola complex, with a mean age of 48 years (ranging from 29 to 65 years), with no major complications, except for the irregularity in pigment absorption in eight reconstructions (28.5%).
CONCLUSION: The use of tattooing techniques in the preparation of the nipple-areola complex proved to be effective, with minimal morbidity, and easy to perform, with high patient satisfaction rates, despite the need for a future touch-up to obtain the ideal shade.
Keywords: Tattooing; Breast neoplasms; Mammaplasty; Reconstructive surgical procedures; Cosmetic techniques.
RESUMO
INTRODUÇÃO: A reconstrução do complexo areolopapilar (RecCAP) constitui-se na etapa final da reconstrução mamária, estando a tatuagem do complexo areolopapilar (CAP) bem estabelecida como efetiva, apesar de pouco difundida entre cirurgiões plásticos brasileiros. Nós mostramos um método simples de RecCAP com a utilização de retalhos cutâneos para confecção da papila e imediata tatuagem do CAP encurtando a recuperação do paciente e evitando novos tempos cirúrgicos.
MÉTODOS: Foi realizado um estudo retrospectivo de pacientes submetidas à RecCAP em nossa clínica privada, no período de setembro de 2015 a dezembro de 2016. Também se procedeu uma pesquisa na base de dados Medline no período de 2004 a 2016, incluindo relatos de doenças associadas à tatuagem.
RESULTADOS: Vinte e seis pacientes foram submetidos a 28 reconstruções do complexo areolopapilar, com faixa etária média de 48 anos (variando de 29 a 65 anos), não havendo maiores complicações, com exceção da irregularidade na absorção do pigmento em oito reconstruções (28,5%).
CONCLUSÃO: A utilização de técnicas de tatuagem na confecção do complexo areolopapilar mostrou-se eficaz, com mínima morbidade e de fácil execução, com altos índices de satisfação do paciente, apesar da necessidade de retoques futuros na obtenção da tonalidade ideal.
Palavras-chave: Tatuagem; Neoplasias da mama; Mamoplastia; Procedimentos cirúrgicos reconstrutivos; Técnicas cosméticas.
The reconstruction of the nipple-areola complex (NAC) is the final stage of breast reconstruction, with reports of NAC tattooing in the scientific literature for more than 30 years1 and being usually performed in two stages, with the new papilla being prepared a few weeks before the NAC tattoo.
Although many surgeons still perform total skin grafting as a reconstruction of the areola, there is significant depigmentation of the graft over time, in addition to no initial pigmentation of the new papilla.
Since September 2015, we have reconstructed the NAC in a single step, making the new papilla with skin flaps and immediately proceeding to the tattooing of the new papilla and areola. We emphasize the need for the plastic surgeon to master the micropigmentation technique as an important ally in the correction of defects acquired in the areolae, even after epidermolysis and/or NAC necrosis in cases of reduction mammoplasties or mastopexies of large mammary ptosis.
OBJECTIVE
To stimulate the plastic surgeon to master the micropigmentation techniques, enabling to correct NAC acquired defects in cases of aesthetic and/or restorative surgeries.
METHODS
This technique was performed in 26 patients from September 2015 to December 2016, with a mean age of 48 years (ranging from 29 - 65 years) After breast reconstruction with a large dorsal myocutaneous flap + silicone prosthesis (17 patients) or silicone expander (9 patients) at least six months from the main breast reconstruction mastectomy surgery in patients at a private clinic in Fortaleza, CE.
The procedure was performed in the surgical center, under local anesthesia + anesthetic sedation. The new NAC site was marked with a disposable plastic element (electrode) for electrocardiographic monitoring (Figure 1).
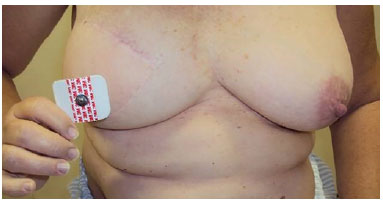
Figure 1. Use of the electrode in choosing the position of the nipple-areola complex.
The skin flap c-v was performed according to techniques already described in the medical literature2. However, we performed an extension of the "v" slightly larger than the ideal (20 mm) allowing the rotation without its constriction when suturing it, with the desired redundancy of the flap created (Figure 2).
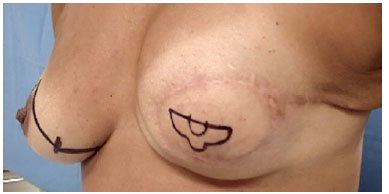
Figure 2. Skin marking of the C-V flap.
The colors of the tattoo and preparation of the areola were selected with a shade slightly darker than the contralateral areola. Immediately after, the new papilla was tattooed with a different and brighter tone.
The choice of darker shades of the tattoo predicts a possible fading of the colors over time (Figures 3 and 4).
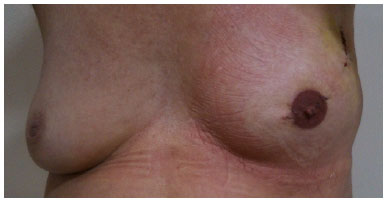
Figure 3. Areola tattoo: darker shade.
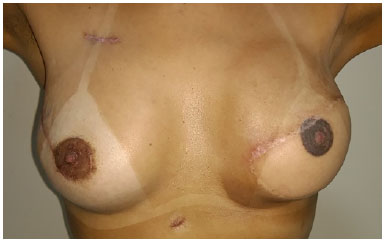
Figure 4. Areola tattoo: darker shade.
Initially, a dermograph-like tattoo machine, used in paramedic micropigmentation during definitive makeup, was used. However, after successive cases of malfunction of this device (and similar reports of other professionals), it was decided to use professional tattoo machines (rotating type or coil), which allow for a greater variety of arrangements, diameters, and quantity of needles, and present greater robustness and safety of work.
The use of professional tattoo machines allowed control of the depth in millimeters of penetration of the needle into the dermis, indispensable in thinner skin flaps (Figure 5).
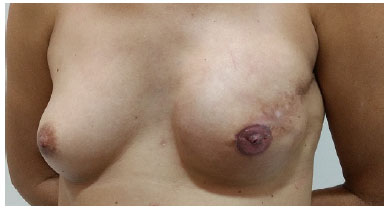
Figure 5. Thin skin flap, but without previous radiotherapy.
RESULTS
There was a partial failure in pigmentation in 28.5% of reconstructions (eight NAC reconstructions in seven patients), and no cases of allergic reaction or local infection and/or inflammation (Figures 6 to 9).
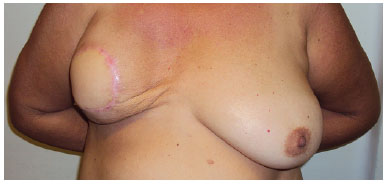
Figure 6. Preoperative mastoplasty with silicone prosthesis in opposite breast + fat grafting in rippling and preparation of nipple-areola complex.
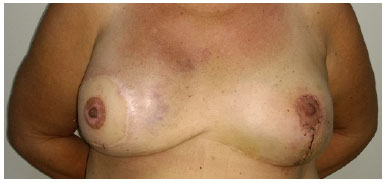
Figure 7. Partial failure of areolar pigmentation.
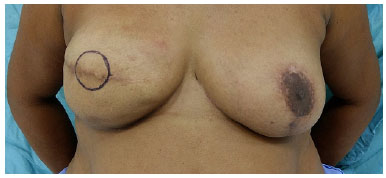
Figure 8. Preoperative preparation of nipple-areola complex.
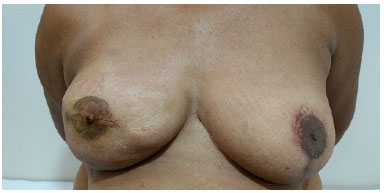
Figure 9. Partial failure (new papilla scar) of areolar pigmentation.
DISCUSSION
The objective of NAC reconstruction is to aim for a suitable position, appropriate projection, approximate pigmentation, size, shape, and symmetry of the contralateral areola.
The tattooing technique is a simple, low-morbidity procedure with a rapid learning curve, providing a high level of satisfaction to for the patient immediately after the procedure3,4.
In the areolar reconstruction, the use of total skin or contralateral areola grafts allows greater morbidity of the donor area with local pain, cellulitis, adhesions, and dyschromia of the donor areola.
There is no papillary pigmentation when we choose local skin flaps for its preparation, in addition to progressive depigmentation of the graft over time (Figures 10 and 11).
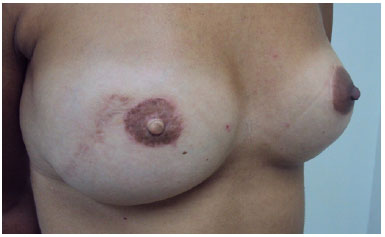
Figure 10. Absence of papilla pigmentation.
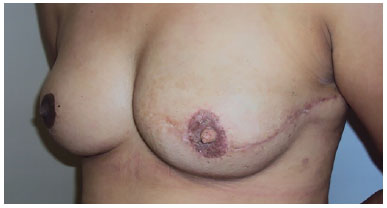
Figure 11. Absence of papilla pigmentation and graft depigmentation.
Although the tattoo also has its colors fading over time, it can be touched up when we master this technique, as opposed to the surgical impossibility of performing a new skin graft5.
The preparation in the new papilla provides an adequate restoration of the papilla with the sensation of touch and projection under the patient's garments and not imitated by three-dimensional tattoo techniques6 (Figure 12).

Figure 12. Different shades between papilla (skin flap) and areola.
In skin flaps previously submitted to radiotherapy, we avoid the preparation of new papilla, either with contralateral papilla graft or local flaps, only performing the NAC tattoo7.
After research on the Medline database in recent years, we have identified some relevant scientific papers listed below.
Hoffman & Mikell3 performed NAC tattooing at about six to eight weeks after making the new papilla, with a slightly darker shade than desired. They emphasized the importance of informing the patient of the need for possible touch-up due to the fading of colors over time. The tattoo was re-evaluated after 3 to 6 months. They recommended discarding the pigment bottle after use, avoiding reuse on another client. They denied the emergence of problems such as infection, allergy or delayed healing in 10 years of experience.
Chen et al.2 described a new skin flap in "medallion" associated with the tattoo in the NAC reconstruction. A total of 11 NAC reconstructions were performed over a two-year period, with an average of eight months postoperatively of the initial breast reconstruction. The areola tattoo was performed after healing of the skin flap in "medallion." There was no skin flap projection loss during postoperative assessment.
Bonomi et al.7 reported the indication of papillary reconstruction with autologous papilla graft in a previously irradiated patient as the first option to making local flaps, which may lead to the necrosis of these flaps and eventual local infection and loss of the silicone implant due to poor vascularization of the irradiated skin flap. They also emphasized the option of not performing any papillary reconstruction techniques when evaluating a minimal thickness in this skin flap, performing only the areola tattoo.
White et al.8 reported the preference to perform NAC tattooing two weeks prior to making the local skin flap (c-v), avoiding the irregular pigment absorption in newly opened surgical wounds and the technical difficulty of pigmenting a new three-dimensional structure (papilla).
Kim et al.9 reported the treatment of 32 mature scars in 28 patients, with an average follow-up period of 14 months. The types of scars were hypopigmented (12), red (7), alopecia (11) and others (2). There was a need for touch-up after 3 weeks in 10 patients (31%) attributed to inadequate pigment penetration, local dyschromia or blood crusts formed. They suggest using pigments that are slightly lighter than the patient's skin color, avoiding unnecessary distress in the healing/inflammation period after the procedure.
LeBlanc et al.10 reported outbreaks of non-tuberculous mycobacterial strains (chelonia, fortuitous and abcessum) detected in New York in January 2012, initially attributed to tap water and/or used to dilute (unduly) tattoo pigment. However, contamination in the industrial production of ink and its components (water, glycerin, pigments) was not ruled out.
The authors emphasized the lack of regulation by the FDA of tattoo ink, considered a cosmetic product, and the importance of alerting clients of the possibility of fungal infection, which presents by peripheral papular lesions or local cutaneous rush, initially confused with allergic processes and hindering the clinical diagnosis and early treatment of the infection.
Pessoa et al.11 described the technique of micropigmentation of the areola in 10 previously submitted patients (6-month interval) to mammary reconstruction immediately after the mastectomy with myocutaneous flaps (9) or silicone expander (1). The tattoo was performed 6-12 weeks after reconstruction of the papilla with a local skin flap. They reported the absence of allergic reactions and a case of local cellulitis treated with a systemic antibiotic.
Loh et al.12 criticized a previously published article that recommended NAC tattooing prior to the preparation of new papilla. They argued that there is no difficulty in absorbing the pigment in the new papilla and/or in newly formed scars, highlighting the service experience, and using new pigments and tattooing techniques. In addition, they reported achieving satisfactory results in the creation of a shading at the base of the new papilla and a luminous highlight at the top, performed three months after making the papilla.
Wenzel et al.13 reported the results of a research with 3,411 tattooed individuals and an incidence of 6% (up to 4 weeks after the procedure), including itch, permanent or temporary edema (being a precursor of granulomas or scars) or cutaneous papules. These were more frequent in women and in colored tattoos. Other studies have examined the probable causes of local skin infections due to inadequate or non-existent local asepsis and/or antisepsis, lack of care and hygiene guidelines after the procedure.
Colored tattoos were related to granulomatous cutaneous reactions, lichens or allergic hypersensitivity, besides the formation of cutaneous tumors, such as seborrheic keratosis, epidermal cysts, milia, histiocytofibroma. They suggest more rigorous legislation prohibiting, for introduction in the skin, the use of chemical substances not used in external makeup.
Liliav et al.14 proposed to tattoo the NAC immediately before the skin flap in c-v was made, promoting the pigmentation of the future papilla even before the flap was elevated. They also recommended a distinct coloring of the region of the new papilla, as well as a darker shade of every tattoo anticipating a gradual discoloration of the tattoo over time.
Simunovic & Shinohara15 recommended a skin biopsy on suspicious lesions to diagnose from systemic inflammatory diseases (scleroderma, sarcoidosis, lichen, eczema) to bacterial or atypical (non-tuberculous mycobacteria) infections. These fungal infections can be acquired by using contaminated water present in the inadequately diluted pigment, manifesting after a month of the tattoo with the presence of pustules, ulcers, nodules in the tattooed region. They are also occasioned by inadequate care in local hygiene after the procedure. They also reported the appearance of delayed hypersensitivity reactions to the pigment or its components.
Levites et al.16 reported the tendency of tattoos losing color over time. They try to create a mathematical model to predict the change of color tone over time, facilitating the use of a color closer to that resulting from wear and tear after a few months. They reported that the pigment introduced into the skin would be extruded over the months by epidermal cells and local macrophages and with basement membrane reestablishment, the pigments reside only in dermal fibroblasts. The authors commented another work that recommended the use of pigments 1/3 darker than the contralateral areola. They concluded that the use of a tattoo that does not need multiple touch-ups over the months would translate into greater patient satisfaction.
Liszewski et al.17 reported an incidence of 21% of Americans with at least one tattoo and no regulation of tattoo care by the FDA, avoiding bacterial or fungal contamination. They emphasized that since tattoo pigments are considered for cosmetic use, there is a differentiated regulation for each state of sanitary surveillance standards regarding the use of sterile gloves, disposable biosafety measures and mandatory reporting of accidents or infections to local health authorities. They also emphasized the need to provide the client with written instructions on wound (tattoo) care regarding the management of infection prevention, trauma caused by the needle and local inflammatory process, until final healing in two to four weeks.
CONCLUSION
The use of tattooing techniques in the preparation of the NAC proved to be effective, with minimal morbidity and easy to perform, with high patient satisfaction rates despite the need for a future touch-up to obtain the ideal shade.
COLLABORATIONS
FJFB Final approval of the manuscript; conception and design of the study; completion of surgeries and/or experiments; writing the manuscript or critical review of its contents.
RMGM Completion of surgeries and/or experiments.
REFERENCES
1. Becker H. The use of intradermal tattoo to enhance the final result of nipple-areola reconstruction. Plast Reconstr Surg. 1986;77(4):673-6. DOI: http://dx.doi.org/10.1097/00006534-198604000-00032
2. Chen SG, Chiu TF, Su WF, Chou TD, Chen TM, Wang HJ. Nippleareola complex reconstruction using badge flap and intradermal tattooing. Br J Surg. 2005;92(4):435-7. DOI: http://dx.doi.org/10.1002/bjs.4885
3. Hoffman S, Mikell A. Nipple-areola tattooing as part of breast reconstruction. Plast Surg Nurs. 2004;24(4):155-7. DOI: http://dx.doi.org/10.1097/00006527-200410000-00006
4. Goh SC, Martin NA, Pandya NA, Cutress RI. Patient satisfaction following nipple-areolar complex reconstruction and tattooing. J Plast Reconstr Aesthet Surg. 2011;64(3):360-3. DOI: http://dx.doi.org/10.1016/j.bjps.2010.05.010
5. Spear SL, Arias J. Long-term experience with nipple-areola tattooing. Ann Plast Surg. 1995;35(3):232-6. PMID: 7503514 DOI: http://dx.doi.org/10.1097/00000637-199509000-00002
6. Halvorson EG, Cormican M, West ME, Myers V. Three-dimensional nipple-areola tattooing: a new technique with superior results. Plast Reconstr Surg. 2014;133(5):1073-5. PMID: 24776543 DOI: http://dx.doi.org/10.1097/PRS.0000000000000144
7. Bonomi S, Settembrini F, Gregorelli C, Rapisarda V. Patient selection and satisfaction following nipple reconstruction with nipple sharing. J Plast Reconstr Aesthet Surg. 2011;64(12):e339-40. PMID: 21930447 DOI: http://dx.doi.org/10.1016/j.bjps.2011.08.031
8. White CP, Gdalevitch P, Strazar R, Murrill W, Guay NA. Surgical tips: areolar tattoo prior to nipple reconstruction. J Plast Reconstr Aesthet Surg. 2011;64(12):1724-6. PMID: 21778128 DOI: http://dx.doi.org/10.1016/j.bjps.2011.06.031
9. Kim EK, Chang TJ, Hong JP, Koh KS. Use of tattooing to camouflage various scars. Aesth Plast Surg. 2011;35(3):392-5. DOI: http://dx.doi.org/10.1007/s00266-011-9698-8
10. LeBlanc PM, Hollinger KA, Klontz, KC. Tattoo ink-related infections - awareness, diagnosis, reporting, and prevention. N Engl J Med. 2012;367(11):985-7. DOI: http://dx.doi.org/10.1056/NEJMp1206063
11. Pessoa SGP, Matos JRF, Dias IS, Pessoa BBGP, Alencar JCG.Simple and safe technique for nipple-areola reconstruction with intradermal tattoo. Rev Bras Cir Plást. 2012;27(3):415-20. DOI: http://dx.doi.org/10.1590/S1983-51752012000300015
12. Loh CY, Lim P, Lam D. Re: Surgical tips: areolar tattoo prior to nipple reconstruction. J Plast Reconstr Aesthet Surg. 2012;65(8):1123-4. PMID: 22537417 DOI: http://dx.doi.org/10.1016/j.bjps.2012.03.011
13. Wenzel SM, Rittmann I, Landthaler M, Bäumler W. Adverse reactions after tattooing: review of the literature and comparison to results of a survey. Dermatology. 2013;226(2):138-47. PMID: 23689478 DOI: http://dx.doi.org/10.1159/000346943
14. Liliav B, Loeb J, Hassid VJ, Antony AK. Single-stage nippleareolar complex reconstruction technique, outcomes, and patient satisfaction. Ann Plast Surg. 2014;73(5):492-7. PMID: 24135688 DOI: http://dx.doi.org/10.1097/SAP.0b013e318276dac0
15. Simunovic C, Shinohara MM. Complications of decorative tattoos: recognition and management. Am J Clin Dermatol. 2014;15(6):525-36. DOI: http://dx.doi.org/10.1007/s40257-014-0100-x
16. Levites HA, Fourman MS, Phillips BT, Fromm IM, Khan SU, Dagum A, et al. Modeling fade patterns of nipple areola complex tattoos following breast reconstruction. Ann Plast Surg. 2014;73 Suppl 2:S153-6. DOI: http://dx.doi.org/10.1097/SAP.0000000000000120
17. Liszewski W, Jagdeo J, Laumann AE. The Need for Greater Regulation, Guidelines, and a Consensus Statement for Tattoo Aftercare. JAMA Dermatol. 2016;152(2):141-2. DOI: http://dx.doi.org/10.1001/jamadermatol.2015.4000
1. Sociedade Brasileira de Cirurgia Plástica, Fortaleza, CE, Brazil
2. Hospital Geral de Fortaleza, Fortaleza, CE, Brazil
Institution: Clínica Privada, Fortaleza, CE, Brazil.
Corresponding author:
Francisco Jose Fontenele Bezerra
Rua Barão de Aracati, 444/900
Fortaleza, CE, Brazil - Zip Code 60115-080
E-mail: fco.fontenele@yahoo.com.br
Article received: January 17, 2017.
Article accepted: October 19, 2017.
Conflicts of interest: none.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter