

Case Report - Year 2017 - Volume 32 -
Case report: tuberous breast
Relato de Caso: mama tuberosa
ABSTRACT
To report a case of tuberous breast with significant breast asymmetry, describe the technique used and evaluate the outcome of the case. Different techniques were used on each breast, although studies in literature recommend the use of similar strategy in both breasts. The patient progressed without complications and had, 6 months after the surgery, extremely satisfactory result without tuberous breast stigmas, and significant improvement of breast asymmetry. The literature establishes that not only one surgical technique is adequate to correct different types of malformations. Tuberous breast constitutes a challenge in breast plastic surgery and it becomes more complex when the asymmetry is more severe. However, surgeons who is trained in a variety of aesthetic and breast reconstructive techniques can achieve a satisfactory result.
Keywords: Mammoplasty; Congenital abnormalities; Breast; Breast diseases; Breast implantation.
RESUMO
Descrever um caso de mama tuberosa com importante assimetria mamária, descrever a técnica e avaliar o resultado de caso. Diferentes técnicas foram usadas em cada mama, apesar de na literatura dizer que é importante empregar uma estratégia semelhante em ambas as mamas. A paciente evoluiu sem complicações e apresenta, com 6 meses de pós-operatório, resultado extremamente satisfatório, sem estigmas de mama tuberosa e com melhora importante da assimetria mamária. Na literatura é estabelecido que não há uma única técnica cirúrgica adequada para a correção dos diferentes tipos de malformações. A mama tuberosa representa um desafio nas cirurgias plásticas da mama e se tornam mais complexas quando a assimetria é mais exacerbada. Porém, o cirurgião que dominar as mais diversas técnicas mamárias estéticas e reconstrutoras poderá alcançar um resultado satisfatório.
Palavras-chave: Mamoplastia; Anormalidades congênitas; Mama; Doenças mamárias; Implante mamário.
The expression "tuberous breast" is used to define a variety of breast deformities that may present peculiar anatomic-morphological characteristics with different severity degrees.
The breast bud is differentiated and formed during intrauterine life until delivery, but full development occurs at puberty, which can range from 7-9 years to 15-16 years1.
The etiology of tuberous deformity is unclear or well defined. Some authors consider an important element the absence of surface layer in the superficial fascia at the level of the areola. Other authors, however, emphasize the importance of objective clinical data on presence of a constricting fibrous ring around the areola that prevent or restrict the growth of the mammary gland. According to Mandrekas et al., this fibrous ring is a thickening and fibrosis of the superficial fascia or hypertrophy of Cooper's ligaments2.
Classification of different types of tuberous breast deformity3:
Type I - herniated breast tissue into an expanded areola and thin skin with unsatisfactory skin adhesion gland. Cranialized inframammary fold with a fibrotic constriction. Breasts laterally positioned in the chest wall with ample space between breasts.
Type II - breasts severely hypoplastic with solid skin, small areola, and strong skin glandular grip. Constricted mammary base. Absent, flat or concave lower pole. Absent inframammary fold. There is a typical glandular protrusion behind the areola with deformity of its lower lip; this deformity is enhanced after introduction of prosthesis.
Type III - normoplastic breasts with tubular aspect presenting a ptosis on "dive" and nipple areola complex turned down. A circular breast contouring with generally high position, although not excessively lateralized in the chest. Reducing of the distance of areolopapilar complex.
Different types of breast deformities may cause a psychological burden to young patients who are highly influenced by social relationships because of the unusual shape and appearance of their breasts4.
Tuberous breast type III in the left side is often associated with tuberous breast type II in the right5.
CASE REPORT AND DISCUSSION
This was 18-years-old white woman who did not have any comorbidities or underwent previous surgery. She was diagnosed with tuberous breast type II on the right side and tuberous breast type III on the left side in the onset of puberty (Figure 1). Her physical examination showed a hypoplastic right breast, constricted and even small, herniated enlarged areola, with undeveloped lower pole and poorly defined, high and short distance of nipple areolar to inframammary fold, without ptosis degree (Figure 2). The hypertrophic left breast, with tubular appearance, with herniation of breast by enlarged areola, ptosis grade II, high breast fold and presenting a slightly lower pole (Figure 3).
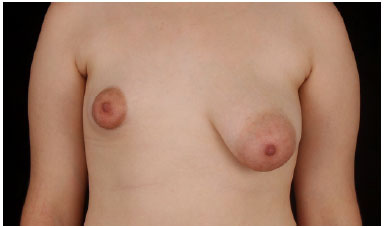
Figure 1. Front view before surgery.
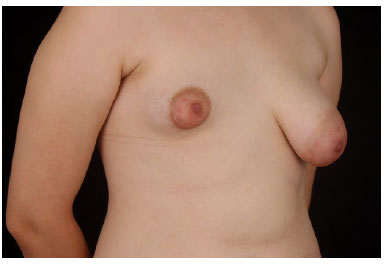
Figure 2. Right oblique before surgery.
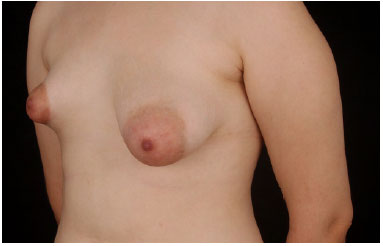
Figure 3. Left oblique before surgery.
The right breast base had 8 cm and left breast 10 cm. Based on these measurements and asymmetry we opted for a polyurethane implants, anatomical profile, extra high projection, all prosthesis had distance from nipple areolar complex to the enlarged fold. According to physical examination of the patient, an asymmetry of at least 200 ml was already possible to detect. Although the possibility of achieve symmetry without breast implants on the left breast, we opted for reduction with implants to achieve similar consistency.
The patient complained about her breast asymmetry that caused difficulty in social relationships and psychological burden.
Surgical technique in the right breast was performed via a periareolar incision, dissection to prepectoral plane, radiated incisions to lysis of the fibrous ring and inclusion of polyurethane implant, anatomical profile, 315 ml, extra high projection and subglandular plan. On the left breast we performed mastopexy using a periareolar approach, dissection to prepectoral plan, clear of excessive skin with inverted T, radiated incisions to lysis the fibrous ring and inclusion of polyurethane implant, anatomical profile, 185 ml, high projection and subglandular plan.
A resection was carried out on excessive level of the retroareolar and lateral tissue, flapping some part of the tissues such as pedicle in the lower pole. To elevate the nipple areolar complex, we used the medial superior pedicle. To resect excessive skin, we used principles of Tailor Tacking with points marked intraoperatively before implant placement.
The right time for surgery is defined when breast development is clearly completed, but, sometimes, the decision of early intervention can be taken due to the impact and emotional stress that this deformity has on the patient.
Literature establishes that not only one surgical technique is adequate to correct different defect types6. After correcting deformity, we can proceed with breast implant. The selection of implant type, the plan and the surgical approach will vary from case to case. It is important to avoid the use of heavy and large implants because they may cause loosing and thinning of the skin, lowering of the prosthesis with pseudoptosis and wrinkling of implant edges.
Type of flaps used in tuberous breast deformity type II:
Glandular flap type II is correlated with tuberous breast deformity type II. This is a glandular flap, glandular pedicled and superficially, subcutaneously rotated. It is used to transfer a certain amount of gland protruding behind the small aerola to the center of the inferior pole under the tense skin. This flap can be defined as a small retroareolar glandular flap.
Glandular flap type III is created from the deep retroareolar surface used to mobilize a certain amount of tissue from the upper side to the inferior side of the areolar both superiorly and inferiorly to it. This flap is used to modify certain type II deformity, where the very small gland is protruding completely behind the small areola.
Glandular flap type IV is a deep flap created using some part of the deep surface of the breast from the upper retroareolar region to the inferior border o the gland and create an "a" flap, which is released and caudally extended by inferior pole. This flap is used to correct tuberous breast deformity type II, when a sufficient thickness of the breast and covering of soft parts of the thoracic wall are present, and also when the base is not too narrow.
According to the literature, it is important to employ a similar strategy in both breasts7, that is, if the case requires the use of an implant size in one side, of the same size should be used on the other side. For this reason, it is recommended whenever possible, reducing the size of the largest breast to be similar to the smaller one in order to place, if the case allows, two equal implants. This objective is achieved through the use of a glandular subcutaneous segmental resection calculated preoperatively.
In our case, however, we opted to carry out, first the correction of the smaller breast with inclusion of the 315 ml implant and use of flap type II to complete the inferior pole. This process was followed by mastopexy and inclusion of smaller prosthesis of 185ml. The use of the same implants size was impossible because of the significant asymmetry presented by the patient (Figures 4 and 5).
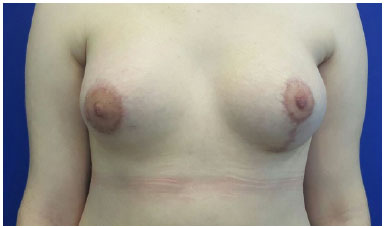
Figure 4. 3 months after surgery.
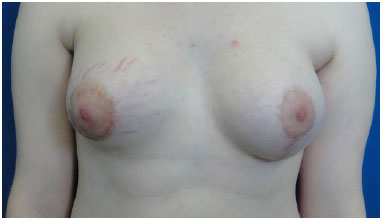
Figure 5. 6 months after surgery.
COLLABORATIONS
TMS Analysis and/or interpretation of data; statistical analyses; final approval of the manuscript; conception and design of the study; completion of surgeries and/or experiments; writing the manuscript or critical review of its contents.
CEJB Analysis and/or interpretation of data.
BMBO Analysis and/or interpretation of data.
BPSFF Analysis and/or interpretation of data.
IDB Analysis and/or interpretation of data.
MADR Analysis and/or interpretation of data.
REFERENCES
1. Neligan PC. Volume 5. Cirurgia Plástica - Mama. 3ª ed. Rio de Janeiro: Elsevier; 2015.
2. Meara JG, Kolker A, Bartlett G, Theile R, Mutimer K, Holmes AD. Tuberous breast deformity: principles and practice. Ann Plast Surg. 2000;45(6):607-11. PMID: 11128758 DOI: http://dx.doi.org/10.1097/00000637-200045060-00006
3. David A. Hidalgo DA, Spector JA. Breast Augmentation. Plast Reconstr Surg. 2014;133(4):567e-83e. DOI: http://dx.doi.org/10.1097/PRS.0000000000000033
4. Mandrekas AD, Zambacos GJ, Anastasopoulos A, Hapsas D, Lambrinaki N, Ioannidou-Mouzaka L. Aesthetic reconstruction of the tuberous breast deformity. Plast Reconstr Surg. 2003;112(4):1099-8. DOI: http://dx.doi.org/10.1097/01.PRS.0000076502.37081.28
5. Scott LS, Jason CG. Aesthetic Reconstruction of the Tuberous Breast Deformity. Discussion. Plast Reconstr Surg 2003;112(4):1109.
6. Kolker AR, Collins MS. Tuberous breast deformity: classification and treatment strategy for improving consistency in aesthetic correction. Plast Reconstr Surg. 2015;135(1):73-86. PMID: 25539297 DOI: http://dx.doi.org/10.1097/PRS.0000000000000823
7. Mandrekas AD, Zambacos GJ. Aesthetic reconstruction of the tuberous breast deformity: a 10-year experience. Aesthet Surg J. 2010;30(5):680-92. DOI: http://dx.doi.org/10.1177/1090820X10383397
1. Hospital Municipal Miguel Couto, Rio de Janeiro, RJ, Brazil
2. Hospital Municipal Barata Ribeiro, Rio de Janeiro, RJ, Brazil
3. Hospital Municipal Souza Aguiar, Rio de Janeiro, RJ, Brazil
Institution: Hospital Municipal Barata Ribeiro, Rio de Janeiro, RJ, Brazil.
Corresponding author:
Tulio Martins Silva
Av. Oswaldo Cruz, 149, apto 1004 - Flamengo
Rio de Janeiro, RJ, Brazil - Zip Code 22250-060
E-mail: tuliomartins2@hotmail.com
Article received: October 19, 2016.
Article accepted: July 9, 2017.
Conflicts of interest: none.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter