

Reviw Article - Year 2015 - Volume 30 -
The role of the plastic surgeon in the treatment of Gorlin syndrome
O papel do cirurgião plástico na Síndrome de Gorlin
ABSTRACT
INTRODUCTION: Gorlin syndrome or nevoid basal cell carcinoma syndrome is a rare multisystemic disease with a potential to cause a broad spectrum of abnormalities and other cancers. It is an autosomal dominant disease with a high penetrance and large variability of expression, manifesting in all ethnic groups but more prevalent in Caucasians, and presenting at a sex ratio of 1:1.
OBJECTIVE: The aim of this study was to discuss Gorlin syndrome, which is little commented on in the literature , and is possibly being underdiagnosed and undertreated by plastic surgeons and other professionals.
METHOD: A literature review was done by selecting articles about Gorlin syndrome from the Medline/PubMed database from 2009 to 2013, and a case-by-case description from the records of the Clinical Hospital of Ribeirão Preto, University of São Paulo is provided.
CONCLUSION: Gorlin syndrome is a multisystemic syndrome with a wide spectrum of manifestations and a great potential for causing problems related mainly to the treatment of its three major changes or features. The plastic surgeon plays an important role in its detection, and can assist in the comprehensive treatment with proper follow-up of patients.
Keywords: Orofacial-digital syndrome; Gorlin syndrome; Plastic surgery.
RESUMO
INTRODUÇÃO: A síndrome de Gorlin ou síndrome do nevo carcinoma basocelular é uma doença multissistêmica infrequente, com um potencial de desenvolvimento de anormalidades de amplo espectro, como também de desenvolvimento de outras neoplasias. A mesma é autossômica dominante, com alta penetrância e grande variabilidade de expressão, manifesta-se em todos os grupos étnicos, sendo mais prevalente em caucasianos, e com relação entre os sexos de 1:1.
OBJETIVO: Discorrer sobre esta afecção pouco comentada em nosso meio e que pode estar sendo subdiagnosticada e subtratada tanto pelo cirurgião plástico como pelos demais profissionais supostamente envolvidos.
MÉTODO: Realizada revisão da literatura selecionando artigos sobre síndrome de Gorlin, no banco de dados da Medline/Pubmed de 2009-2013, e descrição da casuística do serviço do Hospital das Clínicas de Ribeirão Preto - USP.
CONCLUSÃO: A síndrome de Gorlin é uma síndrome multissistêmica, com um amplo espectro de manifestações e grande potencial de mutilação relacionada principalmente ao tratamento de suas três principais alterações/ características. O cirurgião plástico desempenha papel importante na sua detecção e pode colaborar no tratamento abrangente com seguimento adequado aos seus portadores.
Palavras-chave: Síndromes orofaciodigitais; Síndrome de Gorlin. Cirurgia plástica.
Gorlin syndrome or nevoid basal cell carcinoma (BCC) syndrome is a rare multisystemic disease with a potential for causing broad-spectrum abnormalities and other neoplasias1.
It was suggested that the syndrome has existed since the Egyptian dynastic period, as shown by findings dating back to 1000 AD2. The first citation in the literature dates from 1894, when Jarish3 and White4 described a patient with multiple BCCs, associated with scoliosis and learning difficulties. The syndrome was reported in 1960 by Robert James Gorlin and William Goltz5, who established the classic triad that characterize its diagnosis. This diagnostic triad was later modified by Rayner et al.6, who established as a diagnostic criterion the presence of odontogenic cysts associated with calcification of falx cerebri and palm pits. In addition to the classic triad described by Gorlin and Goltz, falx cerebri calcifications, palmar and plantar pits, epidermal cysts, abnormalities in the ribs and spine, macrocephaly, facial milia, frontal bossing, ocular malformations, medulloblastoma, cleft lip or palate, and developmental malformations were also established as characteristics of the syndrome7.
The syndrome is autosomal dominant, with a high penetrance and a large variability of expression8.
The prevalence of the disease is variable. In 1992, Fardon et al.9 estimated that the minimum prevalence was 1 in 57,000 inhabitants. A similar figure was reported by Pratt and Jackson10. A study in the northwest of England showed that the disease affects 1 in 55,600 persons11. In Italy, the incidence of 1 in 256,000 inhabitants is lower than that in Australia, with 1 in 164,000, and that in the United Kingdom12.
The syndrome manifests in all ethnic groups, although several reports reveal a higher occurrence in Caucasians13. The sex ratio is 1:114.
OBJECTIVE
We aimed to discuss Gorlin syndrome, a condition that is little commented on in the literature, and is probably being underdiagnosed and undertreated by plastic surgeons and other professionals.
MATERIALS AND METHODS
We performed a literature review by selecting articles about Gorlin syndrome from the Medline/ PubMed database, from 2009 to 2013. Additionally, this article presents a case-by-case series from the Plastic Surgery Division of the Clinical Hospital of the Medical School of Ribeirão Preto, University of São Paulo.
Case 1
The patient was a 29-year-old married housewife of brown ethnicity. Primary dermatological examination showed lesions on the face and scalp that had been present since birth, with no pathological or family history.
Physical examination revealed ulcerated lesions (5 × 2 cm diameter) with pearl-like edges on the left supraclavicular region, hypertelorism, and poor dental conservation with multiple tooth extractions. The hypothetical diagnosis was Gorlin syndrome. The patient was referred to the plastic surgery service, where she underwent excision of the defect and other lesions that were found on follow-up, with primary suture predominantly, as well as reconstructions with grafts and flaps. All lesions were confirmed as BCCs on pathological tests. She continued her follow-up with the multidisciplinary teams of dentistry, endocrinology, and oculoplastic surgery. She was lost to follow-up after 7 years (Figure 1).
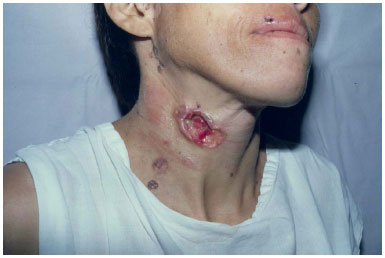
Figure 1. Case 1 patient with multiple basal cell carcinomas, including a cervical ulcerated lesion.
Case 2
The patient was a 22-year-old white male who was a single, unemployed farmer. He sought dermatological care for lenticular lesions in the frontal region, which had been present for 13 years. He stated that 3 years ago, after a trauma, the lesions began to show progressive growth, frequent bleeding, and pigmentation change. In the same period, three lesions appeared in the lower corner of his right eye. He denied any personal medical or family history. He also had a complaint of defective teeth in the upper arch. Physical examination revealed a vegetating lesion, pearlescent, and of 3.2 × 2 cm diameter on the forehead; three papular lesions, also pearlescent, in the inner corner of the right eye; three lesions in the right lower eyelid; and lenticular lesions of erythematous borders in the left pectoral region and left subscapularis. Poor dental conservation and hypertelorism were also observed. A hypothetical diagnosis of Gorlin syndrome was considered.
The patient was referred to the plastic surgery division 2 years later, when he was indicated for excision of a forehead injury.
He was further subjected to multiple excisions of other lesions, with primary suture but also with graft and flap rotation. All BCC lesions were confirmed on pathological tests. He was followed by the dentistry, oculoplastic surgery, and head and neck surgery teams. However, he was lost to follow-up after 6 years (Figure 2A-C).
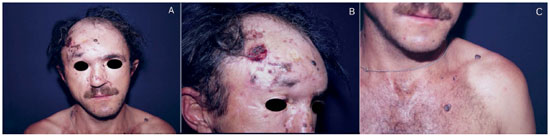
Figure 2. Case 2 patient: (A) multiple basal cell carcinomas (BCCs) of central distribution; (B) details of forehead lesions, including a large ulcerated lesion; and (C) presence of BCCs also in the frontal trunk region.
DISCUSSION
Gorlin syndrome is an autosomal dominant syndrome with a high penetrance and great variability of expression. It is caused by mutations in the tumor suppressor gene PTCH, a homologous gene to the Drosophila gene mapped on chromosome 9q21-238.
A family history of Gorlin syndrome was noted in 70% of the studied cases15, which is explained by an incomplete penetrance and sporadic mutations16. Although a family history is involved in most instances, there was no family history of the syndrome in the cases described herein.
The diagnostic criteria were established by Evans et al.11 and were modified by Kimonis et al. in 1973. According to the authors, the diagnosis of Gorlin syndrome can be established in the presence of two major criteria, or one major criterion and two minor criteria, as described below:
Major criteria: More than two BCCs or one BCC in a patient under 20 years old, odontogenic cysts, two or more palm pits, bilamellar calcification of falx cerebri, forked ribs or fused ribs, and a first-degree relative with nevoid BCC syndrome.
Minor criteria: Macrocephaly adjusted for weight, frontal bossing, cleft lip/palate, hypertelorism, Sprengel deformity, pectus excavatum, syndactyly, sella turcica bridge, hemivertebra, phalangeal radiolucency in candle flame, ovarian fibroma, and medulloblastoma17.
In addition to the above conditions, the syndrome presents a wide range of manifestations in several body systems, such as the central nervous, ophthalmic, otological, urogenital, gastric, cardiovascular, and skeletal systems. A more precise diagnosis can be confirmed by the detection of mutations in the PTCH gene18.
As this syndrome has a wide clinical spectrum, the treatment should be based on a multidisciplinary approach.
Treatment of BCC: Owing to the possibility of multiple diseases, the patient should receive a treatment tailored for his or her medical condition, including curettage and electrodessication, cryosurgery, laser ablation, surgical excision, Mohs surgery, photodynamic therapy, ionizing radiation, and chemical therapies.
Treatment of odontogenic cysts: The treatment of odontogenic keratocyst tumors is also multifactorial. The methods are basically divided into conservative, aggressive, and radical strategies. The conservative method consists of regular enucleation of the tumor in its bone bed. The aggressive technique consists of enucleation, followed by chemical or mechanical curettage of the bone bed. The radical treatment involves the removal of the cyst along with its bony base, with a margin of 5 mm of healthy bone.
Treatment of medulloblastoma: The best results are obtained with a combination of aggressive tumor resection, radiotherapy, and chemiotherapy19.
The patients are usually referred from various specialties to the plastic surgeon, for the evaluation and excision of a suspected nevoid, which is often mutilating when subjected to successive surgical procedures.
In the case of successive resection of BCCs, which are similar to nevoid, in the same patient, plastic surgeons must consider the possible diagnosis of Gorlin syndrome and start proper investigation, in isolation or preferably with a multidisciplinary effort, thus providing a more tailored assistance and adequate patient treatment. Because Gorlin syndrome is an autosomal dominant disease with a high penetrance, it is mandatory to offer genetic counseling to patients20.
CONCLUSION
Gorlin syndrome is a multisystemic syndrome with a wide spectrum of manifestations and a great potential for mutilation related mainly to the treatment of two of its changes: the BCCs, the odontogenic keratocysts and medulloblastoma, which cause physical and psychological harm to patients with this disease.
The plastic surgeon plays an important role in the diagnosis, which can only be done with a knowledge of the characteristics of the syndrome and relating it to the patient, thus contributing to a complete treatment and appropriate follow-up.
REFERENCES
1. Gupta SR, Jaetli V, Mohanty S, Sharma R, Gupta A. Nevoid basal cell carcinoma syndrome in Indian patients: a clinical and radiological study of 6 cases and review of literature. Oral Surg Oral Med Oral Pathol Oral Radiol. 2012;113(1):99-110. PMID: 22669069 DOI: http://dx.doi.org/10.1016/j.tripleo.2011.08.017
2. Casaroto AR, Loures DC, Moreschi E, Veltrini VC, Trento CL, Gottardo VD, et al. Early diagnosis of Gorlin-Goltz syndrome: case report. Head Face Med. 2011;7:2. DOI: http://dx.doi.org/10.1186/1746-160X-7-2
3. Jarisch W. Zur lehre von den hautgeschwulsten. Arch Dermatol Syph. 1894;28:163-5. DOI: http://dx.doi.org/10.1007/BF01843725
4. White JC. Multiple benign cystic ephiteliomas. J Cutan Genitourin Dis. 1884;12:477-84.
5. Gorlin RJ, Goltz RW. Multiple nevoid basal-cell epithelioma jaw cysts and bifid rib. A syndrome. N Engl J Med. 1960;262:908-12. PMID: 13851319 DOI: http://dx.doi.org/10.1056/NEJM196005052621803
6. Rayner CR, Towers JF, Wilson JS. What is Gorlin's syndrome? The diagnosis and management of the basal cell naevus syndrome, based on a study of thirty-seven patients. Br J Plast Surg. 1977;30(1):62-7. DOI: http://dx.doi.org/10.1016/S0007-1226(77)90037-6
7. Pandeshwar P, Jayanthi K, Mahesh D. Gorlin-goltz syndrome. Case Rep Dent. 2012;2012:247239. PMID: 23082255 DOI: http://dx.doi.org/10.1155/2012/247239
8. Ljubenović M, Ljubenović D, Binić I, Jovanović D, Stanojević M. Gorlin-Goltz syndrome. Acta Dermatovenerol Alp Pannonica Adriat. 2007;16(4):166-9.
9. Farndon PA, Del Mastro RG, Evans DG, Kilpatrick MW. Location of gene for Gorlin syndrome. Lancet. 1992;339(8793):581-2. PMID: 1347096 DOI: http://dx.doi.org/10.1016/0140-6736(92)90868-4
10. Pratt MD, Jackson R. Nevoid basal cell carcinoma syndrome. A 15-year follow-up of cases in Ottawa and the Ottawa Valley. J Am Acad Dermatol. 1987;16(5 Pt 1):964-70. DOI: http://dx.doi.org/10.1016/S0190-9622(87)70122-4
11. Evans DG, Ladusans EJ, Rimmer S, Burnell LD, Thakker N, Farndon PA. Complications of the naevoid basal cell carcinoma syndrome: results of a population based study. J Med Genet. 1993;30(6):460-4. DOI: http://dx.doi.org/10.1136/jmg.30.6.460
12. Lo Muzio L, Pastorino L, Levanat S, Musani V, Situm M, Ponti G, et al. Clinical utility gene card for: Gorlin syndrome-update 2013. Eur J Hum Genet. 2013;21(10). DOI: http://dx.doi.org/10.1038/ejhg.2012.299
13. Titinchi F, Nortje CJ, Parker ME, van Rensburg LJ. Nevoid basal cell carcinoma syndrome: a 40-year study in the South African population. J Oral Pathol Med. 2013;42(2):162-5. DOI: http://dx.doi.org/10.1111/j.1600-0714.2012.01188.x
14. Kiran NK, Tilak Raj TN, Mukunda KS, Rajashekar Reddy V. Nevoid basal cell carcinoma syndrome (Gorlin-Goltz syndrome). Contemp Clin Dent. 2012;3(4):514-8. DOI: http://dx.doi.org/10.4103/0976-237X.107459
15. Tom WL, Hurley MY, Oliver DS, Shah MR, Bree AF. Features of basal cell carcinomas in basal cell nevus syndrome. Am J Med Genet A. 2011;155A(9):2098-104. PMID: 21834051 DOI: http://dx.doi.org/10.1002/ajmg.a.34127
16. Shah M, Mavers M, Bree A, Fosko S, Lents NH. Quality of life and depression assessment in nevoid basal cell carcinoma syndrome. Int J Dermatol. 2011;50(3):268-76. DOI: http://dx.doi.org/10.1111/j.1365-4632.2010.04658.x
17. Agrawal A, Murari A, Vutukuri S, Singh A. Gorlin-goltz syndrome: case report of a rare hereditary disorder. Case Rep Dent. 2012;2012:475439. PMID: 23050170 DOI: http://dx.doi.org/10.1155/2012/475439
18. García de Marcos JA, Dean-Ferrer A, Arroyo Rodríguez S, Calderón-Polanco J, Alamillos Granados FJ, Poblet E. Basal cell nevus syndrome: clinical and genetic diagnosis. Oral Maxillofac Surg. 2009;13(4):225-30. DOI: http://dx.doi.org/10.1007/s10006-009-0169-1
19. Kiwilsza M, Sporniak-Tutak K. Gorlin-Goltz syndrome-a medical condition requiring a multidisciplinary approach. Med Sci Monit. 2012;18(9):RA145-53. DOI: http://dx.doi.org/10.12659/MSM.883341
20. Valiati AA, Pavelecini M, Netto R, Pereira Filho G, Fauri MA, Lima LP, et al. Síndrome do Nevo Basocelular: relato de caso. ACM Arq Catarin Med. 2009;38(Suppl 1):160-2.
1. Universidade de São Paulo, Ribeirão Preto, SP, Brazil
2. Sociedade Brasileira de Cirurgia Plástica, São Paulo, SP, Brazil
Institution: Hospital das Clínicas, Faculdade de Medicina de Ribeirão Preto, Universidade de São Paulo. Ribeirão Preto, SP, Brazil.
Corresponding author:
Jayme Adriano Farina Junior
Av. Bandeirantes, 3900, Monte Alegre
Ribeirão Preto, SP, Brazil Zip Code 14048-900
E-mail: jafarinajr@gmail.com
Article received: September 18, 2014.
Article accepted: March 15, 2015.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter