

Original Article - Year 2015 - Volume 30 -
Round versus anatomical breast implants: algorithm for choosing the appropriate form
Implante mamário redondo versus anatômico: algoritmo para escolha da forma adequada
ABSTRACT
INTRODUCTION: Several surgeons have their own formulas or protocols to select the volume and shape of breast implants. To determine the shape, we measured the distances between the upper edge of the breast and the papilla (A), and between the papilla and the inframammary fold (B). Based on these measurements, we propose an algorithm to select round or anatomical implants.
METHODS: Preoperative assessment was performed with the patients in the orthostatic position. The following distances were considered: 1) from the sternal notch to the papilla, to assess the need for supra-areolar skin excision; 2) breast base, to assess the volume of the implant; 3) distances A and B, to evaluate the shape of the implant. This algorithm was applied to 59 patients undergoing augmentation mammoplasty.
RESULTS: We used round implants in 27 patients; nine had a distance A = B, and 18 had B > A. We utilized anatomical implants in 32 patients. The volume of round implants ranged from 195 to 425 cc, whereas that of anatomical implants ranged from 185 and 315 cc. Regarding postoperative measurements of the patients who used round implants, 26 (96.3%) maintained the desired ratio with B > A or A = B. Among the patients with anatomical implants, 25 (78.1 %) showed proportional changes from A > B to A = B or B > A.
CONCLUSIONS: When the distance A is equal to or smaller than the distance B, we recommend round implants. When B < A, we recommend anatomical implants.
Keywords: Mammoplasty; Breast implants; Breast Implants/trends; Algorithms
RESUMO
INTRODUÇÃO: Vários cirurgiões têm suas próprias fórmulas ou protocolos para selecionar os volumes e formato de implantes mamários. Para determinar a escolha do formato, medimos as distâncias entre a borda superior da mama e a papila (A) e entre a papila e sulco submamário (B). Baseados nestas medidas, propomos um algoritmo para selecionar próteses redondas ou anatômicas.
MÉTODOS: As avaliações pré-operatórias foram realizadas com a paciente em posição ortostática considerando-se as medidas: 1) da fúrcula esternal à papila, para avaliar a necessidade de retirada de pele supra-areolar; 2) da base da mama, para avaliar o volume do implante; 3) das distâncias A e B, para avaliar a forma do implante. Este algoritmo foi aplicado a 59 pacientes submetidas à mamoplastia de aumento.
RESULTADOS: Utilizamos implantes redondos em 27 pacientes; nove tinham distância a = b, e 18 B > A. Empregamos implantes anatômicos em 32 pacientes. Os volumes dos implantes redondos variaram entre 195 cc e 425 cc, enquanto os implantes anatômicos ficaram entre 185 cc e 315 cc. Com relação às medidas pós-operatórias das pacientes que utilizaram implantes redondos, 26 (96,3%) mantiveram a proporção desejada com B > A ou A = B. Entre as pacientes com implantes anatômicos, as medidas de 25 delas (78,1%) mostraram alteração das proporções, de A > B para A = B ou B > A.
CONCLUSÕES: Quando a distância A é igual ou menor que a distância B, recomendamos implantes redondos. Quando B < A, recomendamos implantes anatômicos.
Palavras-chave: Mamoplastia; Implantes de mama; Implantes mamários/tendências; Algoritmos.
One of the major difficulties in breast implant surgery is the choice of the appropriate volume for the breast anatomy and biotype, and for meeting patient expectations. Tebbetts1 discussed over 50 patient- and surgeon-related factors that affect the result of augmentation mastoplasty. Many surgeons have their own formulas or protocols regarding the choice of the volume and type of implant, location, fold position, and incision, which have been widely reported in the medical literature and used in clinical practice1-5. The provision of implants with different forms and projections by manufacturers increased the number of options but also introduced additional factors that should be considered when planning an augmentation mastoplasty6.
OBJECTIVES
To present an algorithm that can be used in choosing between round and anatomical implants in the preoperative assessment of augmentation mammoplasties.
METHODS
Based on the morphology of the breast, namely the fact that the areolar-papillary complex is projected in a position pointing upward and outward, we believe the distance from the top of the breast edge to the central point of the papilla (distance A) should be smaller than the distance from the papilla to the inframammary fold (distance B) (Figures 1 and 2).
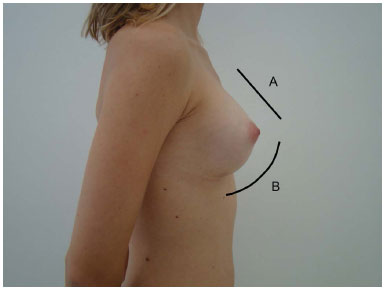
Figure 1. In the ideal proportions, distance A must be shorter than distance B.
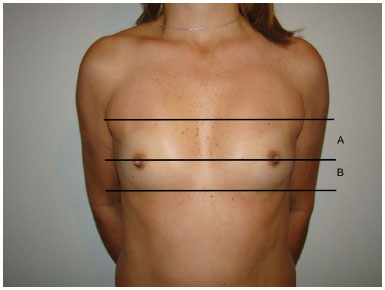
Figure 2. Limit of distances A and B.
The surgeon can determine the upper limit by exerting a light pressure on the breasts. All measurements were made with a measuring tape without skin traction. Round implants caused greater projection in the central portion of the breast while the so-called anatomical implants produced greater projection in the lower breast pole. Based on preoperative assessment of breast shape, we propose an algorithm for choosing between round and lower-projection (anatomical) implants, according to the final desired form.
Preoperative assessment was performed with the patients in the orthostatic position, and the following distances were considered: 1) from the sternal notch to the papilla, to assess the need for supra-areolar skin excision; 2) breast base, to assess the volume of the implant; 3) distances A and B, to evaluate the shape of the implant and the patient's expectation regarding the shape and volume of the implant. Naturally, these data were studied together with the patients in order to meet their expectations.
When distance A is less than or equal to distance B (A < B), we recommend round implants (Figure 3A). By contrast, when distance A is greater than distance B (A > B), we recommend anatomical implants of greater projection in the lower pole in order to reverse this ratio (Figure 3B).
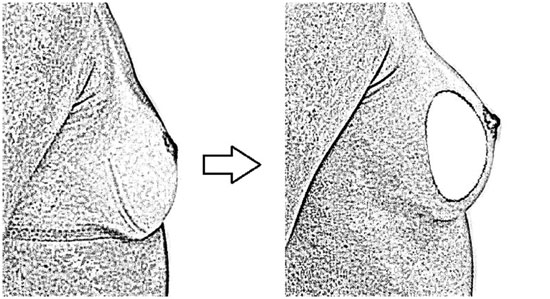
Figure 3A. A round implant producing greater projection in the middle third, behind the areola, while preserving the ratio between distances A and B.
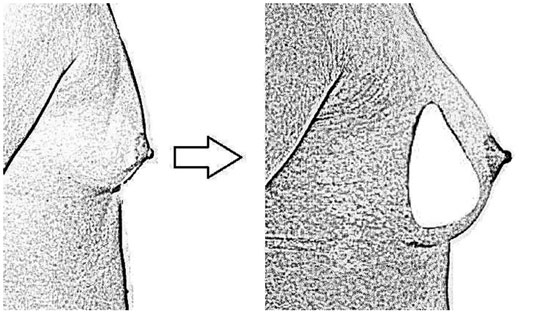
Figure 3B. An anatomical implant producing greater projection in the lower third, reversing the proportions between distances A and B.
We present a prospective study of 59 patients aged between 18 and 48 years who underwent breast implantation on the basis of the results of this algorithm from July 2010 to December 2014. We aimed to establish an indicative criterion for deciding on whether to use a round or an anatomical breast implant. The subjects in this study were patients being treated at the private clinic of the main author. The study was conducted according to the principles of the Declaration of Helsinki, and the study was approved by the responsible ethics committee (12/2009).
Patients who previously underwent implant inclusion (implant exchange) and those in need of skin removal (mastopexy) were excluded from the study. The inclusion plane was always subfascial, and all implants had a polyurethane coating (Silimed®).
RESULTS
We recommended round implants to 27 patients. Of these implants, nine had a distance A = B, and 18 had a distance B > A (Figures 4 and 5). We indicated anatomical implants to 32 patients with a distance A > B (Figures 6 and 7).
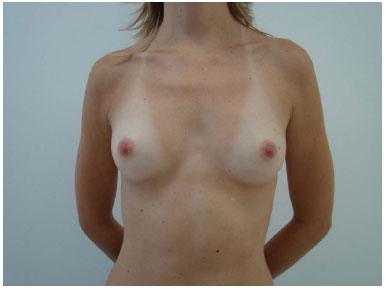
Figure 4A. Preoperative appearance.
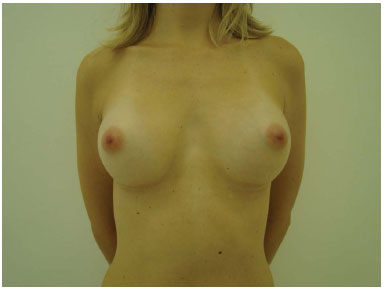
Figure 4B. Postoperative appearance at 8 months' follow-up. A sample case for recommendation of round implants (225 cc).
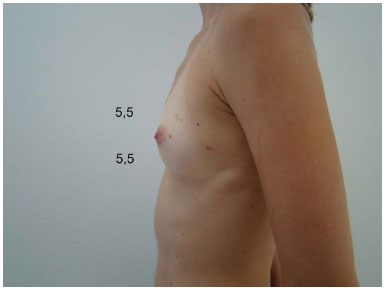
Figure 4C. Preoperative measurements: segment A = B.
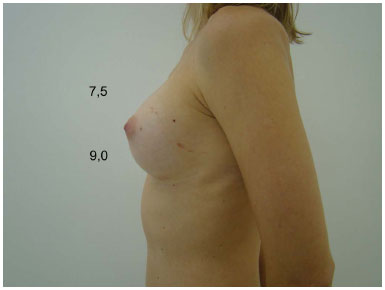
Figure 4D. Postoperative measurements: segment B > A. Appropriate anatomical proportions.
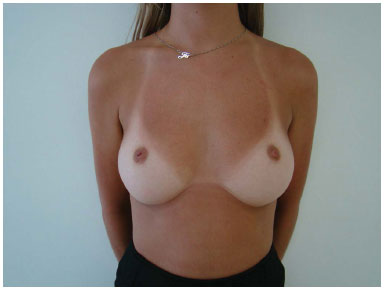
Figure 5A. Preoperative appearance.
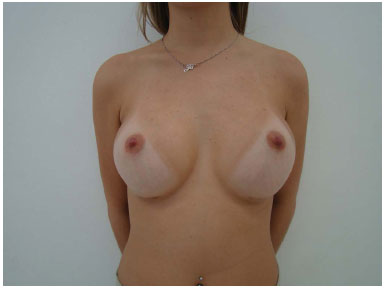
Figure 5B. Postoperative appearance with round implants (255 cc).
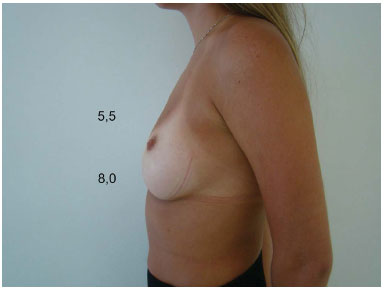
Figure 5C. Preoperative appearance.
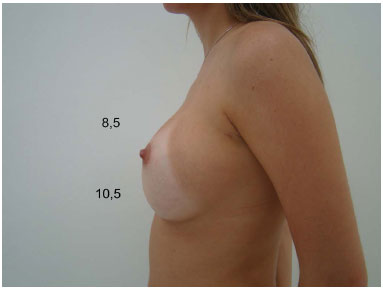
Figure 5D. Postoperative appearance with round implants (255 cc).
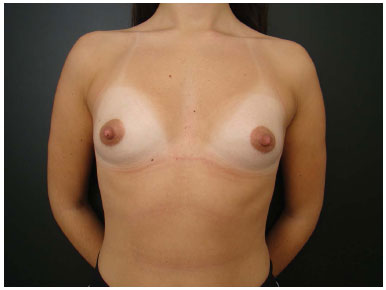
Figure 6A. Preoperative appearance.
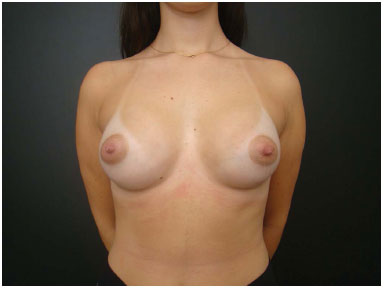
Figure 6B. Postoperative appearance.
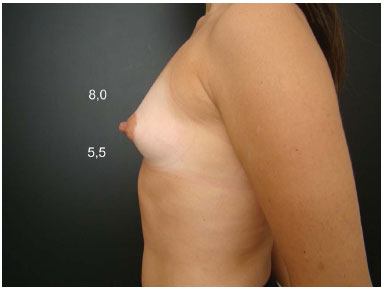
Figure 6C. Preoperative appearance.
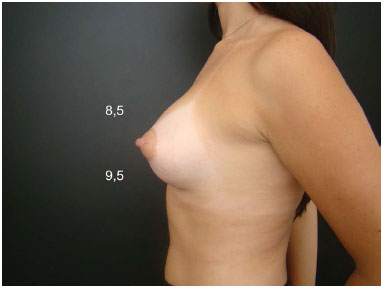
Figure 6D. Postoperative appearance at 9 months' follow-up. Anatomical implant recommendation (245 cc) due to segment A > B. Important atrophy of the lower segment. Postoperative appearance with reversal of the appropriate measurements and anatomical proportions.
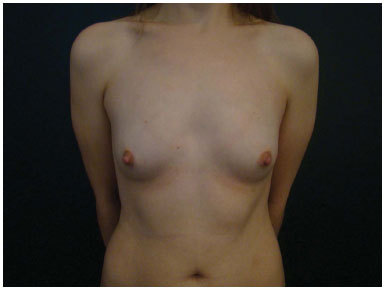
Figure 7A. Preoperative appearance.
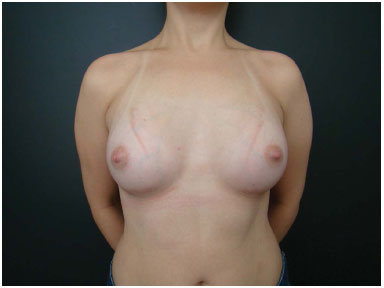
Figure 7B. Postoperative appearance.
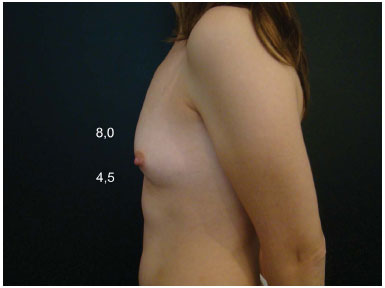
Figure 7C. Preoperative appearance.
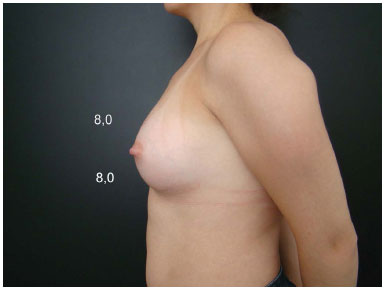
Figure 7D. Postoperative appearance with an anatomical implant (230 cc).
The postoperative evaluation was performed in the orthostatic position after the third month. No complications occurred that could interfere with the measurements in any of the 59 patients evaluated.
The volume of the round breast implants ranged from 195 to 425 cc, whereas that of the lower projection implants ranged from 185 to 315 cc. In five patients who received lower-projection implants, different volumes were used for asymmetry correction.
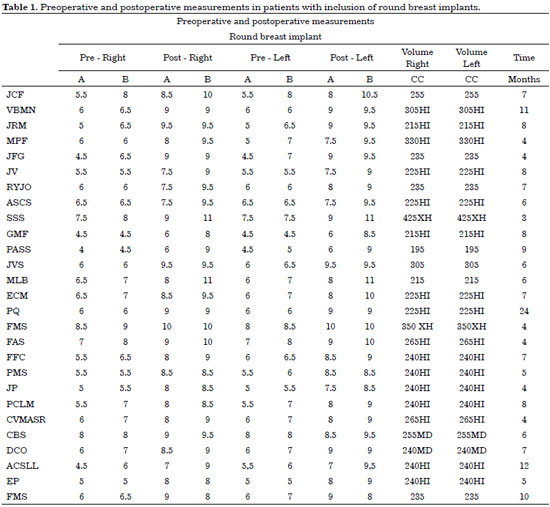
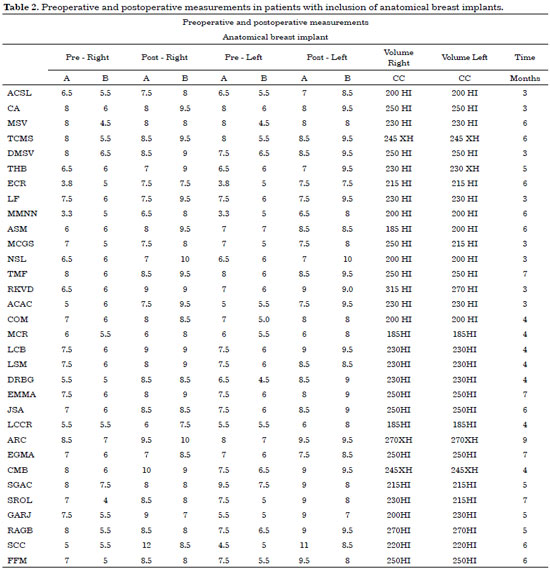
Concerning the size of the breasts for inclusion of a round implant, 26 patients (96.3%) maintained the desired proportion of B > A or A = B. One patient (3.7%) did not present the desired size in the postoperative assessment (Table 1). Among the patients who underwent inclusion with lower-projection implants (anatomical), 25 (78.1%) showed an inversion of measurements from A > B to A = B or B > A. Two patients (6.2%) showed unilateral measurement inversion, and five (15.6%) did not show inversion of measurements (Table 2). Of these patients, two underwent a new surgery for supra-areolar skin excision, achieving the desired measurements.
DISCUSSION
The search for the ideal shape and volume of breast implants stimulates the development of formulas, protocols, and measurements, in order to optimize the choice in each situation. Bozola et al.7 concluded that the ideal shape of breast implants should contain the Phi ratio and that this form of prosthesis is able to correct cases of hypomastia, including reconstructions, providing good aesthetic results. However, application of the formula presented by these authors is complex.
Tebbetts1 described more than patient- and surgeon-related 50 factors that can affect implantation results. The criteria for volume selection, inclusion plane, and incision site are based on pre-established concepts, surgeon experience, and patient expectations. Tebbetts and Adams2 proposed a protocol with only five parameters for evaluating the necessary covering tissue, volume, inclusion plane, access path, and position of the fold, considering implants available in manufacturer catalogs.
Tepper et al.8 analyzed three-dimensional images of patients who received round saline and silicone implants through a periareolar incision, analyzing the changes in breast morphology after augmentation mastoplasty. They evaluated the breast volumetric distribution in the upper and lower poles, and calculated the effect of the volume and shape of the implant relative to these poles. No difference was observed in the volumetric distribution after insertion of round implants, thus preserving the same proportion of tissue in the upper and lower poles before and after surgery. This study showed that when a greater projection in the breast's lower pole is desired, implants with larger volume and projection in its lower portion should be chosen. The authors also observed 20% loss in the anteroposterior projection of the breasts with round implant insertion through a periareolar incision, relative to measurements referred in the implant code. This observation suggests that the periareolar scar may restrict the projection of the implant, whereas incision in the inframammary fold would not have this inconvenience, facilitating the stretch of the papillary fold distance and giving the desired proportions, that is, the lower pole (B) greater than the upper pole (A).
We conclude that the following factors influence the result of augmenting mastoplasties: anatomical aspects, concepts and techniques used by the surgeon, and patient expectations. Some of these factors have been reported in recent9-13 publications.
Camarena and Brambila14 suggest using anatomical implants in different thoracic heights and widths, asymmetries, small breast volumes, and significant deficit in the lower breast pole. In addition, the authors recommend using round implants in cases of poor volume in the upper pole, pseudoptosis, and small asymmetries. Hedén15 uses a mathematical approach to calculate the dimensions of the implant.
In our casuistic, we observed in seven patients that placing lower projection implants did not give the final desired measurements. This can be attributed either to the beginning of our learning curve or to the long distance between the sternal notch and the papilla, not corrected properly by the supra-areolar skin excision. In the case of round breast implants, the appropriate measurements are easier to obtain because the implant only projects the volume in the central part, preserving thereby the breast proportions.
In the case where the desired proportion was not obtained, we attribute this to a higher positioning of the implant. The patient did not complain of the result, however. This is an exclusive observation of the author. In the case of asymmetries in the inferior pole, different implants were used, chosen according to the table provided by the manufacturer.
Stevens et al.6 reported a study with 708 textured implants (Silimed®). They state, "Form-stable silicone gel breast implants retain their shape, especially in the vertical position, and have a lower incidence of wrinkling, and a low rate of capsular contracture, compared to fourth-generation silicone gel implants and saline implants."
The cohesive gel content contributes to the maintenance of the result and minimizes the possibility of leakage. The larger variety of shapes and volumes, in addition to the choice between different projections, widths, and heights, allows refining of the choice but requires greater care during the preoperative assessment.
In cases of significant hypomastia due to the absence of a defined breast shape, we recommend lower-projection implants in order to define or induce a shape with suitable breast proportion. We believe that application of the proposed algorithm is more likely to achieve a natural breast form.
CONCLUSIONS
Breast implant shape was determined through the relationship between the distances of the upper edge of the breast to the nipple (A) and from the papilla to the breast folds (B). When distance A < B, we recommend round projection implants. By contrast, when distance B < A, we recommend lower projection implants. In this way, we are able to attain the desired proportions in augmenting mammoplasties.
REFERENCES
1. Tebbetts JB. A system for breast implant selection based on patient tissue characteristics and implant-soft tissue dynamics. Plast Reconstr Surg. 2002;109(4):1396-409. DOI: http://dx.doi.org/10.1097/00006534-200204010-00030
2. Tebbetts JB, Adams WP. Five critical decisions in breast augmentation using five measurements in 5 minutes: the high five decision support process. Plast Reconstr Surg. 2006;118(7 Suppl):35S-45S. PMID: 17099482 DOI: http://dx.doi.org/10.1097/01.prs.0000191163.19379.63
3. Adams WP Jr. The process of breast augmentation: four sequential steps for optimizing outcomes for patients. Plast Reconstr Surg. 2008;122(6):1892-900. PMID: 19050543 DOI: http://dx.doi.org/10.1097/PRS.0b013e31818d20ec
4. Spear SL, Bulan EJ, Venturi ML. Breast augmentation. Plast Reconstr Surg. 2006;118(7 Suppl):188S-196S. DOI: http://dx.doi.org/10.1097/01.PRS.0000135945.02642.8B
5. Rudolph R, Forcier N. Calculation of silicone breast implant volumes using breast magnetic resonance imaging. Aesthet Surg J. 2009;29(4):310-3. DOI: http://dx.doi.org/10.1016/j.asj.2009.02.009
6. Stevens WG, Hirsch EM, Tenenbaum MJ, Acevedo M. A prospective study of 708 form-stable silicone gel breast implants. Aesthet Surg J. 2010;30(5):693-701. DOI: http://dx.doi.org/10.1177/1090820X10381880
7. Bozola AR, Longato FM, Bozola AP. Análise geométrica da forma da beleza da mama e da forma de prótese baseado na proporção Phi: aplicação prática. Rev Bras Cir Plást. 2011;26(1):94-103. DOI: http://dx.doi.org/10.1590/S1983-51752011000100019
8. Tepper OM, Small KH, Unger JG, Feldman DL, Kumar N, Choi M, et al. 3D analysis of breast augmentation defines operative changes and their relationship to implant dimensions. Ann Plast Surg. 2009;62(5):570-5. DOI: http://dx.doi.org/10.1097/SAP.0b013e31819faff9
9. Martin del Yerro JL, Vegas MR, Sanz I, Moreno E, Fernandez V, Puga S, et al. Breast augmentation with anatomic implants: a method based on the breast implantation base. Aesthetic Plast Surg. 2014;38(2):329-37. DOI: http://dx.doi.org/10.1007/s00266-013-0190-5
10. Adams WP Jr, Mallucci P. Breast augmentation. Plast Reconstr Surg. 2012;130(4):597e-611e.
11. Swanson E. Prospective outcome study of 225 cases of breast augmentation. Plast Reconstr Surg. 2013;131(5):1158-66 DOI: http://dx.doi.org/10.1097/PRS.0b013e318287a0e1
12. del Yerro JL, Vegas MR, Fernandez V, Moreno E, Sanz I, Puga S, et al. Selecting the implant height in breast augmentation with anatomical prosthesis: the "number Y". Plast Reconstr Surg. 2013;131(6):1404-12. DOI: http://dx.doi.org/10.1097/PRS.0b013e31828bd65b
13. Lista F, Tutino R, Khan A, Ahmad J. Subglandular breast augmentation with textured, anatomic, cohesive silicone implants: a review of 440 consecutive patients. Plast Reconstr Surg. 2013;132(2):295-303. DOI: http://dx.doi.org/10.1097/PRS.0b013e3182958a6d
14. Cárdenas-Camarena L, Encinas-Brambila J. Round gel breast implants or anatomic gel breast implants: which is the best choice? Aesthetic Plast Surg. 2009;33(5):743-51. PMID: 19484175
15. Hedén P. Mastopexy augmentation with form stable breast implants. Clin Plast Surg. 2009;36(1):91-104. DOI: http://dx.doi.org/10.1016/j.cps.2008.08.003
Universidade Federal do Rio de Janeiro, Rio de Janeiro, RJ, Brazil
Institution: Hospital Universitário-Universidade Federal do Rio de Janeiro, Rio de Janeiro, RJ, Brazil.
Corresponding author:
João Medeiros Tavares-Filho
Rua Buenos Aires, 255
Petrópolis, Rio de Janeiro, Brazil Zip Code 25610-141
E-mail: clinicajoaomedeiros@gmail.com
Article received April 7, 2015.
Article accepted June 7, 2015.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter