

Original Article - Year 2015 - Volume 30 -
Burn injuries: self-inflicted patients
Queimaduras: pacientes autoinfligidos
ABSTRACT
INTRODUCTION: Self-inflicted burn injuries lead to physical, psychological, and economic consequences not only to the victims but also to their families and the society. The prevalence of this type of accident varies greatly throughout the existing literatures. This study aimed to analyze the epidemiological profile, behavior, and lethality rate in patients with self-inflicted burn injuries who received treatment in a burn unit, as a way to contribute to the effective intervention to minimize the effects of risk factors and behaviors associated with this type of accident.
METHOD: We conducted a retrospective study in which we analyzed medical records of patients hospitalized in the burn unit of Asa Norte's Regional Hospital, DF, Brazil, during the period between January 2008 and December 2012.
RESULTS: The study sample consisted of 88 patients with self-inflicted burn injuries, of whom 54.5% were female, with a mean age of 33 years and mean burned body surface area of 36%. The mean hospitalization time was 23 days. Open flame was the etiological agent in 97.7% of the burn cases, and alcohol was the accelerating agent in 68.2% of these cases. The lethality rate was 32.9%. Sixty patients had comorbidities, with psychiatric disorders and alcoholism being the most common.
CONCLUSION: The patients with self-inflicted burn injuries were generally women, with a mean age of 33 years, who used alcohol as accelerating agent. The mean body surface area affected was 36%. Of the patients, 32.9% had associated psychiatric disorders. The lethality rate was 32.9%. From a social perspective, public measures should be established to detect potential patients in order to administer appropriate therapies.
Keywords: Burn injuries; Self-destructive behavior; Suicide; Burn units.
RESUMO
INTRODUÇÃO: As queimaduras autoinfligidas geram consequências físicas, psicológicas e financeiras não só para a vítima, mas também para familiares e para sociedade. A prevalência desse tipo de acidente tem ampla variedade na literatura. O trabalho tem como objetivo analisar o perfil epidemiológico, a conduta e a taxa de letalidade dos pacientes com queimaduras por autoagressão atendidos em centro de tratamento de queimados, como uma forma de contribuir para intervenção efetiva em fatores e comportamentos de risco para tais acidentes.
MÉTODO: Estudo retrospectivo por meio da análise dos prontuários de pacientes internados na Unidade de Queimados do Hospital Regional da Asa Norte, Brasília - DF, no período de janeiro de 2008 a dezembro de 2012.
RESULTADOS: Foram incluídos no estudo 88 pacientes autoinfligidos, 54,5% do gênero feminino, idade média de 33 anos, média da superfície corporal queimada de 36%. A média de tempo de internação foi de 23 dias. A chama aberta foi o agente etiológico das queimaduras em 97,7% dos casos e o álcool foi o agente acelerador em 68,2%. A taxa de letalidade foi de 32,9%. Sessenta pacientes apresentavam comorbidades, sendo os distúrbios psiquiátricos e o etilismo os principais.
CONCLUSÃO: As vítimas de queimaduras por autoagressão são geralmente mulheres, com idade média de 33 anos, utilizando álcool como agente da queimadura, afetando em média 36% da superfície corporal, com distúrbios psiquiátricos associados em 32,9% e com taxa de letalidade de 32,9%. No âmbito social, deve-se pensar em medidas públicas que detectem os pacientes em potencial para que seja instituída terapêutica adequada.
Palavras-chave: Queimaduras; Comportamento autodestrutivo; Suicídio; Unidades de queimados.
Burn injuries are considered a public health problem in Brazil and the world owing to its high incidence, morbidity, and lethality1,2. A report from the World Health Organization (OMS) showed that burn injuries are the fifth leading cause of violent deaths worldwide, having a death toll of more than 320,000 people every year3. Self-inflicted burn injury, though severe, is an uncommon type of burn injury, which is a frequent cause of hospitalization in burn units4-6.
Self-inflicted burn injuries lead to physical, psychological, and economic consequences not only to the victims but also to their families and the society7. The prevalence of this type of accident varies considerably throughout the world, accounting for 1.95% of the total burn hospitalizations in the United States and up to 40.3% in other regions of the world, such as the Middle East7-13.
This type of injury may be characteristic of a suicide attempt or self-punishment. Awareness that these burn injuries are closely associated with several psychiatric disorders and sociocultural factors is important7,14.
OBJECTIVE
In Brazil, the statistical data and preventive actions on this subject are still scarce, being restricted to a few burn treatment units6,15. This study aimed to analyze the prevalence, characteristics, etiology, and lethality rates in patients with self-inflicted burn injuries who were hospitalized in a regional burn unit in Brazil, as a way to contribute to an effective intervention to minimize the effects of risk factors and behaviors associated with this type of accident.
METHOD
This was a retrospective and descriptive study performed by analyzing the medical records of patients hospitalized in the burn unit of Asa Norte's Regional Hospital, DF, Brazil, during the period between January 2008 and December 2012.
Patients who were hospitalized in the burn unit of the Asa Norte's Regional Hospital because of self-inflicted burn injuries resulting from a suicide attempt and for whom duly completed medical records were available were included in the study. Patients who were hospitalized because of accidental burn injuries, patients treated in the emergency service of the hospital and with ambulatory regimens, and patients with self-afflicted burn injuries without the intention to commit suicide were excluded from the study.
The variables analyzed were age, sex, percentage of burned body surface area, etiology of the burn injury, infectious complications, history of psychiatric disorders, surgical interventions (debridement and skin grafts), hospitalization period, and lethality rate.
This study was approved by the ethics committee of the Health State Secretary of Brazil, DF, Brazil, under No. 643,696.
RESULTS
We analyzed 1326 medical records and selected for this study all patients with self-inflicted burn injuries. The number of samples selected was 88, corresponding to 6.63% of the total number of patients hospitalized in the burn unit during the study period, with an average of 18 cases per year, ranging from 13 to 23 cases.
In the study sample, 48 patients (54.5%) were female and 40 (45.5%) were male. Their ages ranged from 14 to 73 years, with a mean of 33 years. The percentage of burned body surface area ranged from 3% to 94%, with a mean of 36% (Table 1). Of the patients evaluated, 56.8% had third-degree burns, while the remaining patients has second- and/or first-degree burns. The mean hospitalization time in the burn unit was 23 days, ranging from 1 to 104 days. As for the agents used for suicide, we observed that open flame was responsible for 97.7% of the cases and alcohol was the accelerating agent used by 60 patients (68.2%). The parts of the body that were most affected were the torso (90.9%), upper limbs (84%), face (68.2%), lower limbs (59%), and perineum (7.9%).
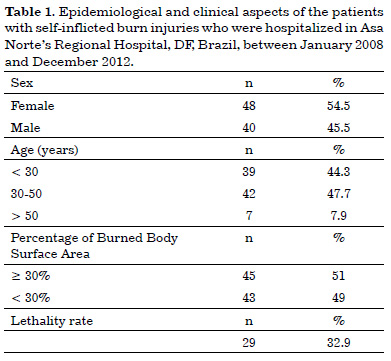
The lethality rate was of 32.9% (Table 1). In these patients, death occurred between the first and the 29th hospitalization day, with a mean survival time of 8.4 days.
In our study sample, 60 patients (68.2%) had one or more comorbidities such as psychiatric disorders (n = 29, 32.9%), history of alcohol abuse (n = 27, 30.7%), smoking history (n = 13, 14.8%), history of drug abuse (n = 8, 9%), epilepsy (n = 4, 4.5%), systemic arterial hypertension (n = 3, 3.4%), diabetes (n = 2, 2.3%), asthma (n = 2, 2.3%), mental retardation (n = 1, 1.1%), and human immunodeficiency virus (n = 1, 1.1%) Of the patients evaluated, only one (1.1%) was homeless. Among the patients with self-inflicted burn injuries, 61 (69.3%) had infectious complications, especially bloodstream and wound infections.
Sixty-nine patients (78.4%) underwent surgical debridement, ranging from 1 to 9 procedures per patient. Of these patients, 42 received skin grafting, with the first grafting procedure performed on the 17th day of hospitalization, on average, ranging between the 10th and 44th day of hospitalization. Fifty-eight patients (65.9%) required blood transfusions during the hospitalization period.
DISCUSSION
Suicide attempt by burning is among the most remarkable forms of suicide. Of all the forms of self-inflicted injuries, it has the longest documented history and a strong cultural meaning and political impact worldwide16,17.
Self-flagellation, the most painful of all the forms of suicide, is not a common form of suicide in Brazil and in the European countries18-20. However, it is highly prevalent in some developing countries, especially in the Asian and African regions. Some studies show high self-flagellation rates in Iran, accounting for 25-70% of all the suicide cases21-23.
The literature on suicides shows that men are more prone to commit suicide than women, whereas women are more prone to attempt suicide20. This study, similarly to another Brazilian study, shows a predominance of females among the patients6. This is also observed in other studies performed in Iran24-27, Egypt, Zimbabwe, and Sri Lanka8,28, but is in disagreement with the data collected from developed countries such as Canada, Australia, England, and Wales29,30. However, some studies showed no sex differences in countries such as Russia and Italy31,32. Socioeconomic factors, political protest, forced marriages, and previous partners are the motives that could explain the sex- and geography-related differences between suicidal individuals25.
Suicide attempts accounted for 6.63% of the total hospitalized patients in the burn unit during the study period, showing a similarity to the data obtained by a previous Brazilian study6. These data are similar to those observed in Italy (4.4%)33, Ireland (4.2%), United Kingdom (4.9%), Switzerland (6.8%)34, and Australia (4.1%)19. However, these are in disagreement with the data referring to other regions of the world where suicide is the leading cause of extensive burn injuries and, consequently, death, such as India13, Iran24, Egypt8, and Sri Lanka28, corresponding to 24.8% of the hospitalizations in an Iranian burn unit23.
In our study, open flame was the most common etiologic agent of burn injuries derived from suicide attempts, and alcohol was the most frequently used catalyst agent, which is in accordance with the finding of a previous study performed by Macedo et al.6. However, this differs from other countries such as Iran and India, where the catalyst agent of this type of burn injury is gasoline35-37.
Self-inflicted burn injuries, differently from accidental burn injuries, seem to cause more severe damages. In this study, the mean burned body surface area was 36%, which is lower than that reported in the previous study performed in this unit (38%)6. The mean hospitalization period was 23 days, ranging from 1 to 104 days. The hospitalization period is compatible with the extent of the burn injuries, complications, and behavior difficulties. The combination of all these factors can result in longer hospitalization periods and slower recovery process than those of patients with accidental burn injuries. In the patients with accidental burn injuries, the mean hospitalization period was 12 days and the mean burned body surface area was 14%38.
The lethality rate of self-inflicted burn injuries during the first 48 h of hospitalization was 75% in Greece39 and 47.9% in Iran39. In this study, we observed a lethality rate of 32.9%. The reasons for the high lethality rate in these patients are the extent of the burn injury, the presence of infectious complications, and resistance to the treatment by the patients33,40. The desire to die and the lack of cooperation tend to hinder prognosis. Psychiatric and psychological support help maintain the cooperation of patients and therefore facilitate the work performed by the medical doctors and nurses. The suicide attempt by burning is a strong predictive factor of mortality34,41.
The presence of psychiatric disorders among the patients with intentional self-inflicted burn injuries seems to be common in the European, North American, and Middle Eastern countries. Depression was the most frequent psychiatric diagnosis, followed by schizophrenia36 and alcoholism19. Interpersonal problems and marital discord seem to be the main motivations of self-inflicted burns in Brazil6, similarly in India13. Political protest is the least frequent motivation36. In Brazil, ignorance of severe, or even fatal, consequences of intentional self-inflicted burn injuries leads to a significant proportion of these injuries, thus resulting in unintended deaths6. In this study, 68.2% of the patients had comorbidities, with psychiatric disorders being the most frequently reported. In Greece, 43% of the patients had a history of psychiatric disorders, with depression being the most frequent disorder observed39.
CONCLUSION
The patients with self-inflicted burn injuries had more severe characteristics, as these patients tend to have a larger burned body surface area, longer hospitalization periods, higher infection rates, and higher lethality rates than the patients with other types of burn injuries. In burn units, psychological and psychiatric support are extremely important to the evolution of the clinical situation. Rehabilitation and reintegration of surviving patients into the community are important, given the severity of their injuries. From a social perspective, public measures that aim to detect potential patients should be established in order to administer appropriate therapies.
REFERENCES
1. Cruz BF, Cordovil PBL, Batista KNM. Perfil epidemiológico de pacientes que sofreram queimaduras no Brasil: revisão de literatura. Rev Bras Queimaduras. 2012;11(4):246-50.
2. Takejima ML, Netto RFB, Toebe BL, Andretta MA, Prestes MA, Takaki JL. Prevenção de queimaduras: avaliação do conhecimento sobre prevenção de queimaduras em usuários das unidades de saúde de Curitiba. Rev Bras Queimaduras. 2011;10(3):85-8.
3. World Health Organization. Facts about injuries: burn [Acesso 26 Fev 2014]. Disponível em: www.who.int/mipfiles/2014/burns1.pdf
4. Cameron DR, Pegg SP, Muller M. Self-inflicted burns. Burns. 1997;23(6):519-21. DOI: http://dx.doi.org/10.1016/S0305-4179(97)00039-9
5. Krummen DM, James K, Klein RL. Suicide by burning: a retrospective review of the Akron Regional Burn Center. Burns. 1998;24(2):147-9. PMID: 9625241 DOI: http://dx.doi.org/10.1016/S0305-4179(97)00092-2
6. Macedo JLS, Rosa SC, Silva MG. Queimaduras autoinfligidas: tentativa de suicídio. Rev Col Bras Cir. 2011;38(6):387-91.
7. Tahir SM, Memon AR, Kumar M, Ali SA. Self inflicted burn; a high tide. J Pak Med Assoc. 2010;60(5):338-41.
8. Mabrouk AR, Mahmod Omar AN, Massoud K, Magdy Sherif M, El Sayed N. Suicide by burns: a tragic end. Burns. 1999;25(4):3379. DOI: http://dx.doi.org/10.1016/S0305-4179(98)00179-X
9. García-Sánchez V, Palao R, Legarre F. Self-inflicted burns. Burns. 1994;20(6):537-8. DOI: http://dx.doi.org/10.1016/0305-4179(94)90016-7
10. Sheth H, Dziewulski P, Settle JA. Self-inflicted burns: a common way of suicide in the Asian population. A 10-year retrospective study. Burns. 1994;20(4):334-5. DOI: http://dx.doi.org/10.1016/0305-4179(94)90062-0
11. Klasen HJ, van der Tempel GL, Hekert J, Sauër EW. Attempted suicide by means of burns. Burns. 1989;15(2):88-92. DOI: http://dx.doi.org/10.1016/0305-4179(89)90136-8
12. Bille-Brahe U, Jessen G. Suicide in Denmark, 1922-1991: the choice of method. Acta Psychiatr Scand. 1994;90(2):91-6. PMID: 7976464 DOI: http://dx.doi.org/10.1111/j.1600-0447.1994.tb01561.x
13. Wagle SA, Wagle AC, Apte JS. Patients with suicidal burns and accidental burns: a comparative study of socio-demographic profile in India. Burns. 1999;25(2):158-61. DOI: http://dx.doi.org/10.1016/S0305-4179(98)00138-7
14. Shahana N, Turin TC, Rumana N, Rahman AF, Hossain S, Nahar S. Mental illness as a contributor to intentional self inflicted suicidal burn injury. Dhaka National Med Coll Hosp. 2012;18(1):49-57. DOI: http://dx.doi.org/10.3329/jdnmch.v18i1.12242
15. Coutinho BBA, Balbuena MB, Anbar RA, Anbar RA, Almeida KG, Almeida PYNG. Perfil epidemiológico de pacientes internados na enfermaria de queimados da Associação Beneficente de Campo Grande Santa Casa/MS. Rev Bras Queimaduras. 2010;9(2):50-3.
16. Crosby K, Rhee JO, Holland J. Suicide by fire: a contemporary method of political protest. Int J Soc Psychiatry. 1977;23(1):60-9. DOI: http://dx.doi.org/10.1177/002076407702300111
17. Thombs BD, Bresnick MG, Magyar-Russell G. Who attempts suicide by burning? An analysis of age patterns of mortality by self-inflicted burning in the United States. Gen Hosp Psychiatry. 2007;29(3):244-50. DOI: http://dx.doi.org/10.1016/j.genhosppsych.2007.01.012
18. Nakhaie M, Tabiei S. Epidemiology of self-immolation in Imam Reza Hospital. Forensic J. 2004;39:49-54.
19. Seoighe DM, Conroy F, Hennessy G, Meagher P, Eadie P. Self-inflicted burns in the Irish National Burns Unit. Burns. 2011;37(7):1229-32. PMID: 21726948 DOI: http://dx.doi.org/10.1016/j.burns.2011.04.011
20. Hahn AP, Jochai D, Caufield-Noll CP, Hunt CA, Allen LE, Rios R, et al. Self-inflicted burns: a systematic review of the literature. J Burn Care Res. 2014;35(1):102-19. DOI: http://dx.doi.org/10.1097/BCR.0b013e31828b0a46
21. Meir PB, Sagi A, Ben Yakar Y, Rosenberg L. Suicide attempts by self-immolation--our experience. Burns. 1990;16(4):257-8.
22. Kooshan M, Nakhaue MS, Zadeh AR, Haider A, Tofighian T, Maskami K. Prevalence of risk factors for suicide. J Sabze¬var Univ Med Sci. 2008;15(2):123-8.
23. Ahmadi A, Mohammadi R, Schwebel DC, Khazaie H, Yeganeh N, Almasi A. Demographic risk factors of self-immolation: a case-control study. Burns. 2009;35(4):580-6. DOI: http://dx.doi.org/10.1016/j.burns.2008.06.012
24. Mehrpour O, Javadinia SA, Malic C, Dastgiri S, Ahmadi A. A survey of characteristics of self-immolation in the east of Iran. Acta Med Iran. 2012;50(5):328-34.
25. Dastgiri S, Kalankesh LR, Pourafkary N. Epidemiology of Self-Immolation in the North-West of Iran. Eur J Gen Med. 2005;2(1):14-9.
26. Ahmadi A. Suicide by self-immolation: comprehensive overview, experiences and suggestions. J Burn Care Res. 2007;28(1):30-41. DOI: http://dx.doi.org/10.1097/BCR.0b013E31802C8878
27. Zarghami M, Khalilian A. Deliberate self-burning in Mazandaran, Iran. Burns. 2002;28(2):115-9. PMID: 11900933 DOI: http://dx.doi.org/10.1016/S0305-4179(01)00092-4
28. Laloë V, Ganesan M. Self-immolation a common suicidal behaviour in eastern Sri Lanka. Burns. 2002;28(5):475-80. PMID: 12163288 DOI: http://dx.doi.org/10.1016/S0305-4179(02)00047-5
29. Shkrum MJ, Johnston KA. Fire and suicide: a three-year study of self-immolation deaths. J Forensic Sci. 1992;37(1):208-21. PMID: 1545201
30. Prosser D. Suicides by burning in England and Wales. Br J Psychiatry. 1996;168(2):175-82. PMID: 8837907 DOI: http://dx.doi.org/10.1192/bjp.168.2.175
31. Anoshchenko IuD, Smirnov SV. The medicosocial status of the victims of burns as a consequence of a suicide attempt (cases of self-immolation). Zh Nevrol Psikhiatr Im S S Korsakova. 1995;95(4):72-4.
32. Castellani G, Beghini D, Barisoni D, Marigo M. Suicide attempted by burning: a 10-year study of self-immolation deaths. Burns. 1995;21(8):607-9. DOI: http://dx.doi.org/10.1016/0305-4179(95)00046-E
33. Taghaddosinejad F, Sheikhazadi A, Behnoush B, Reshadati J, Sabery SH. A survey of suicide by burning in Tehran, Iran. Acta Med Iran. 2010;48(4):266-72.
34. Forster NA, Nuñez DG, Zingg M, Haile SR, Künzi W, Giovanoli P, et al. Attempted suicide by self-immolation is a powerful predictive variable for survival of burn injuries. J Burn Care Res. 2012;33(5):642-8. DOI: http://dx.doi.org/10.1097/BCR.0b013e3182479b28
35. Maghsoudi H, Garadagi A, Jafary GA, Azarmir G, Aali N, Karimian B, et al. Women victims of self-inflicted burns in Tabriz, Iran. Burns. 2004;30(3):217-20. DOI: http://dx.doi.org/10.1016/j.burns.2003.10.010
36. Lalöe V. Patterns of deliberate self-burning in various parts of the world. A review. Burns 2004;30(3):207-15.
37. Cheng AT, Lee CS. Suicide in Asia and the far East. In: Hawton K, van Heeringer, eds. The International Handbook of Suicide and Attempted Suicide. Chichester: John Wiley and Sons; 2000. p.29-48.
38. Carvalho GGF, Freitas FC, Macedo JLS. Estudo prospectivo das vítimas de queimaduras atendidas no serviço de emergência do Hospital Regional da Asa Norte de Brasília. Rev Saúde Dist Fed. 2005;16(1/2):7-15.
39. Castana O, Kourakos P, Moutafidis M, Stampolidis N, Triantafyllou V, Pallantzas A, et al. Outcomes of patients who commit suicide by burning. Ann Burns Fire Disasters. 2013;26(1):36-9.
40. Theodorou P, Phan VT, Weinand C, Maegele M, Maurer CA, Perbix W, et al. Suicide by burning: epidemiological and clinical profiles. Ann Plast Surg. 2011;66(4):339-43. PMID: 21301290 DOI: http://dx.doi.org/10.1097/SAP.0b013e3182071f83
41. Macedo JL, Santos JB. Predictive factors of mortality in burn patients. Rev Inst Med Trop São Paulo. 2007;49(6):365-70. PMID: 18157403 DOI: http://dx.doi.org/10.1590/S0036-46652007000600006
1. Sociedade Brasileira de Cirurgia Plástica, São Paulo, SP, Brazil
2. Hospital Regional da Asa Norte (HRAN), Brasília, DF, Brazil
3. Universidade de Brasília (UnB), Brasília, DF, Brazil
4. Escola Superior de Ciências da Saúde, Brasília, DF, Brazil
Institution: Unidade de Queimados do Hospital Regional da Asa Norte, Brasília, DF, Brazil.
Corresponding author:
Priscilla Bondezan Vieira
Rua Dom Pedro II, 2732, sl 04
Toledo, PR, Brazil Zip Code 85902-010
E-mail: pri_bvieira@hotmail.com
Article received October 30, 2014.
Article accepted July 20, 2015.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter