

Ideas and Innovation - Year 2014 - Volume 29 -
Use of the thoracodorsal flap for the treatment of hidradenitis suppurativa
Uso do retalho toracodorsal para tratamento de hidradenite supurativa
ABSTRACT
INTRODUCTION:Hidradenitis suppurativa is a chronic skin disease that affects the regions harboring the apocrine sweat glands. It has an estimated prevalence of 1% of the population and a preference for the female sex.
METHOD: LMN, a 48-year-old female patient, presented, on examination, palpable, coalescent, painful nodules and a circumjacent area of fibrosis and scar retraction in both axillae, mainly in the left axilla. She was subjected to wide excision of the lesions at the axilla and left thoracic region, with a need for a rotational fasciocutaneous flap, usually used in patients who undergo lateral quadrantectomy.
RESULTS: A satisfactory aesthetic result was attained, together with the preservation of movements.
CONCLUSION: Although there are few reported cases of the use of the lateral thoracodorsal fasciocutaneous flap, this technique is an excellent alternative in axillary reconstruction, owing to the ease of resection, good coverage of the receiving area, and the satisfactory aesthetic result.
Keywords: Hidradenitis suppurativa; Sweat glands; Mastectomy.
RESUMO
INTRODUÇÃO: A hidradenite é uma doença cutânea crônica, que acomete as regiões que abrigam as glândulas apócrinas. Tem uma prevalência estimada de 1% da população, com predileção pelo sexo feminino.
MÉTODO:LMN, 48 anos, sexo feminino. Ao exame, a paciente apresentava nodulações palpáveis, coalescentes, dolorosas e uma área de fibrose e retração cicatricial circunjacente em ambas as axilas, principalmente em axila esquerda. Submetida a exérese ampla das lesões em axila e região torácica esquerda, sendo necessária a realização de um retalho fasciocutâneo de rotação, habitualmente usado em pacientes submetidas à quadrantectomia lateral.
RESULTADOS: Obteve-se um resultado estético satisfatório associado à preservação dos movimentos.
CONCLUSÃO:Apesar de existirem poucos casos relatando o uso do retalho fasciocutâneo toracodorsal lateral, essa técnica mostrou ser excelente alternativa na reconstrução axilar, devido à facilidade de ressecção, boa cobertura da área receptora além de um resultado estético satisfatório.
Palavras-chave: Hidradenite; Glândulas sudoríparas; Mastectomia.
Hidradenitis suppurativa is a chronic skin disease that more commonly affects the regions with apocrine glands. Inflammatory nodules and abscesses, which evolve to ulceration and fistulization, are formed in this condition. The axilla is the most commonly affected site, followed by the anogenital region. It has an estimated prevalence of 1% of the population and primarily affects women (3:1).
The treatment of hidradenitis suppurativa is a challenge. Conservative therapies, drainage of abscesses, and use of intralesional and systemic topical antibiotics are limited and have temporary efficiency1. In addition, the chronic use of medications, due to the high degree of relapse of the lesions, leads to the development of bacterial resistance2. Surgery is indicated for severe and recurrent hidradenitis suppurativa. The lesion should be resected with margins, and healing by second intention is not recommended because of resulting contractures. Primary closure is associated with high relapse rates3. Thus, it is important to be aware of the many flap reconstruction techniques for the region and to seek new reconstruction procedures for the site.
A patient with chronic significant hidradenitis suppurativa in the axillary region was evaluated in our service. In this patient, the complete excision of the lesion created an extensive wound, making primary closure impossible. The surgical team then decided to employ a lateral thoracodorsal fasciocutaneous flap, traditionally used for reconstruction after a mastectomy.
OBJECTIVE
In this study, we aimed to seek a larger variety of complex reconstruction techniques for the axillary region, in order to reduce functional and aesthetic damage.
METHOD
The patient (LMN) is a 48-year-old woman, born in Campo Belo, married, a passive smoker for 26 years, with no other comorbidities, and denied use of medications. At 14 years of age, she already had multiple painful nodular lesions in both axillae, which evolved with the formation of recurrent abscesses, ulcers, and fibrosis. She has a positive family history for hidradenitis suppurativa (her father, brothers, and her two children). She had chronic use of multiple antibiotics during dermatological follow-up, mainly cefalexin; however, remission of the disease did not occur.
In 2011, she was submitted to the drainage of the abscesses in both axillae; however, there was no improvement in the clinical presentation. She was then forwarded to the plastic surgery service of Hospital das Clinicas of the Universidade Federal de Minas Gerais. Upon examination, she presented with palpable, coalescent, painful nodules and an area of fibrosis and scar retraction circumjacent in both axillae, mainly in the left axilla. In November 2011, after complete information on the procedure and signing of an informed consent form, the first surgical approach was completed, which consisted in the excision of nodular lesions of the right axilla, with primary closure.
In May 2012, the second surgical procedure was carried out, involving a wide excision of the left axillary fossa, removal of skin and underlying subcutaneous tissue, including the apocrine glands related to the hidradenitis suppurativa, and drainage of purulent secretion compatible with chronic infection of the region. The wide resection did not allow primary closure. Thus, the use of a lateral thoracodorsal rotational fasciocutaneous flap was decided, which is traditionally used for surgical treatment of patients undergoing lateral quadrantectomy. The decision about using the flap was discussed with the patient, and she agreed to undergo the procedure.
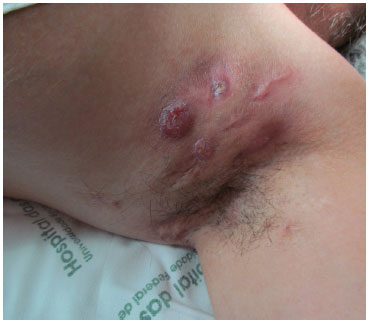
Figure 1. Preoperative.
Skin incision of previously demarcated lines was performed (Figure 2). We took the precaution of demarcating the lateral and lower limits of the breast, in order to preserve its contour after the procedure (Figure 3). The flap was detached from the fascial plane by using a no. 20 scalpel and electrocautery. The viability of the flap was verified by the presence of blood flow in the extremities (Figure 4). After rotation of the flap and rigorous review of hemostasis, the flap was finally sutured, by planes: subcutaneous, subdermal, and cutaneous. A portovac 3.2 drain was positioned in the wound and removed on the second postoperative day (Figure 5).
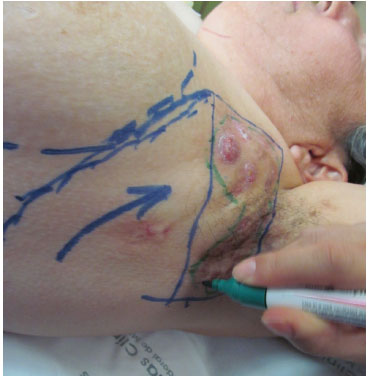
Figure 2. Planning of the flap.
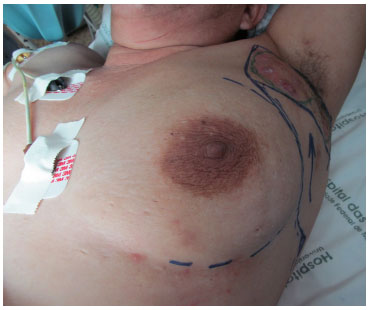
Figure 3. Planning of the flap in relation to the breast.
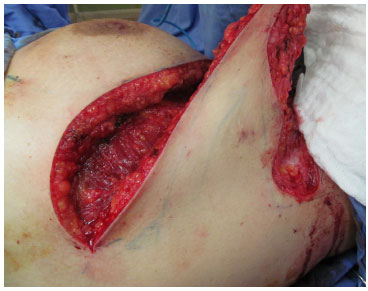
Figure 4. Detached flap with good vascularization.
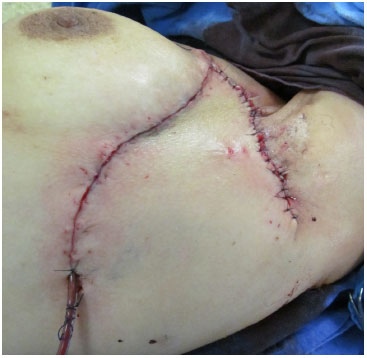
Figure 5. End result.
The type of anesthesia used was general anesthesia. Antibiotic therapy was instituted with oral cephalexin until the seventh postoperative day, and the use of ordinary analgesics was symptomatic. The patient was instructed to keep the limb immobilized next to the body during the first few days after the surgery to prevent dehiscence of the wound, and the skin sutures were removed on the 15th postoperative day.
RESULTS
The excess skin and fatty tissue in the lateral thoracic region presents adequate vascularization from the perforating vessels of the fifth, sixth, and seventh intercostal spaces. This anatomic detail allowed the rotation of the skin and fat to the mammary and lateral axillary region with the firm closure of the resected area.
Thus, a lateral thoracodorsal fasciocutaneous flap was prepared with an inferior to superior rotation axis, toward the axilla, and closing was done with minimal tension. A satisfactory aesthetic result was obtained with no functional losses. The technique allowed the harmonious reconstruction of the axilla. To date, there was no evidence of scar retraction, loss of movement, or relapses in the operated area; however, the inguinal lesions worsened. The patient remains under follow-up 1 year after the operation. She expressed extreme satisfaction with the results of the axillary reconstruction, but is still waiting for the treatment of the inguinal lesions.
DISCUSSION
The diagnosis of hidradenitis suppurativa is, in most cases, delayed, and effective treatment is not carried out, prolonging the suffering of the patient and increasing the possibility of complications. Some of the complications are due to chronic suppuration (anemia, hypoalbuminemia, and amyloidosis), depression, axillary arthropathy, lymphatic obstruction, fistulas, contractures, and even squamous cell carcinoma2,3.
Extensive surgical excision of the tissue enables the best remission of the disease; however, insufficient debridement of the affected area is the main cause of relapse4. After a wide resection, owing to the three-dimensional anatomical architecture of the axillary fossa, adequate reconstruction is required with a flap that enables the movement of tissues of the axillary region, without causing scar retraction during arm movements5.
Different types of flaps are described in the literature: lipocutaneous, fasciocutaneous, myocutaneous, and free flaps6. The frequent use of myocutaneous and fasciocutaneous flaps in plastic surgery has spread the use of these flaps also in the treatment of hidradenitis suppurativa, with satisfactory results. Giovannini and Giannas5 advocate the use of parascapular fasciocutaneous flaps owing to their better rotation capacity, lower thickness, and less morbidity of the donor area. In addition, the technique used for the completion of the fasciocutaneous flap is less complex, thus requiring a shorter surgical time7. Teo et al.8 recently described two cases of a radical approach for axillary hidradenitis suppurativa by using a lateral thoracic flap. The authors highlight the large dimensions possible for the flap (30'15cm) and the importance of the delay for this technique.
The lateral thoracodorsal flap was described by Holmström and Lossin7, in 1986, as a technique for breast reconstruction. This is an example of a fasciocutaneous flap that can be safely used for axillary reconstruction after the excision of extensive hidradenitis suppurativa, as in our case. This flap has rich anastomoses and good vascularization, and careful dissection is important with maintenance of the muscle fascia throughout the flap extension9.
In the study by Woerdeman6, in which the surgical results of the lateral thoracodorsal flap in postmastectomy patients were evaluated, the technique resulted in few complications. This allowed the author to consider that the use of this flap is suitable for other deformities, not only of the breast but also scars and axillary defects. However, there are few studies on the use of this flap for the treatment of extensive chronic hidradenitis.
Many surgical treatments for hidradenitis suppurativa have been described in the literature10. Simple excision with primary suture, commonly preferred by surgeons who are not specialists in plastic surgery, is associated with high rates of disease relapse3. Mandal and Watson11 observed that 69% of patients who underwent primary suture needed at least a new surgical approach. It is also well known that simple excisions with secondary suture need a long period for complete healing. In addition, both primary and secondary closures are associated with a higher appearance of cicatricial contraction and limitation of movements3.
CONCLUSION
Hidradenitis suppurativa is a chronic disease that affects the quality of life of the patient, involving the physical, emotional, and social aspects9.
The thoracodorsal fasciocutaneous flap is an excellent alternative for axillary reconstruction, owing to the ease of resection, good coverage of the receiving area, and the satisfactory aesthetic result.
REFERENCES
1. Menderes A, Sunay O, Vayvada H, Yilmaz M. Surgical management of hidradenitis suppurativa. Int J Med Sci. 2010;7(4):240-7.
2. Buyukarik O, Hasdemir AO, Kahramansoy N, Cavit C, Erkol H. Surgical approach to extensive hidradenitis suppurativa. Dermatol Surg. 2011;37:835-42.
3. Teixeira JCEDO, Filho ADSR, De Castro OC. Thoracodorsal fascicutaneous flap in the treatment of hidradenitis suppurativa: a case report and literature review. Rev Bras Cir Plást. 2012;27(1):170-3.
4. Soldin MG, Tulley K, Kaplan H, Hudson DA, Grobbelaar AO. Chronic axillary hidradenitis: the efficacy of wide excision and flap coverage. Br J Plast Surg. 2000;53(5):434-6.
5. Giovannini UM, Giannasi S. Fasciocutaneous flap to treat Verneuil disease (hidradenitis suppurativa) in the axillary region. Ann Plast Surg. 2003;50(1):108-9.
6. Woerdeman LA. Surgical risk factors of breast reconstruction and their clinical implications. Plast Reconstr Surg. 2004;113:196-203.
7. Holmström H, Lossing C. The lateral thoracodorsal flap in breast reconstruction. Plast Reconstr Surg. 1986;77:933-41.
8. Teo WL, Ong YS, Tan BK. Radical surgical excision and use of lateral thoracic flap for intractable axillary hidradenitis suppurativa. Arch Plast Surg. 2012;39(6):663-6.
9. Bienek A, Matusiaki Y, Okulewicz-Gojlic D, Szepietowski JC. Surgical treatment of hidradenitis suppurativa: experiences and recommendations. Dermatol Surg. 2010;36:1998-2004.
10. Margesson LJ, Dellavalle RP, Ofori AO, Danby W. Pathogenesis, clinical features and diagnosis of hidradenitis suppurativa. Ann R Coll Surg Engl. 1997 Mar;79(2):83-9.
11. Mandal A, Watson J. Experience with different treatment modules in hidradenitis suppurativa: a study of 106 cases. Surgeon. 2005;3:23-6.
1. Resident in Plastic Surgery at the Hospital das Clínicas, Universidade Federal de Minas Gerais (HC-UFMG)
2. PhD in Surgery, Specialist in Plastic Surgery - Plastic Surgeon Preceptor of the HC-UFMG
3. Resident in Plastic Surgery at the HC-UFMG
4. Medical Student at the UFMG - Coordinator of the Academic League of Plastic Surgery of the UFMG
5. Medical Student at the UFMG - Coordinator of the Academic League of Plastic Surgery of the UFMG
6. Resident in Plastic Surgery at the HC-UFMG
7. Resident in Plastic Surgery at the HC-UFMG
8. Resident in Plastic Surgery at the HC-UFMG
Institution: Department of Plastic Surgery, Hospital das Clinicas da UFMG-MG, Armando Chiari Junior.
Corresponding Author:
Thaís Gomes Casali
Rua Professor Alfredo Balena, 110 - Santa Efigênia
Belo Horizonte, Brazil Zip code: 33120-050
E-mail: casalithais@hotmail.com
Article submitted: March 24, 2013.
Article accepted: September 1, 2013.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter