

Case Report - Year 2014 - Volume 29 -
Closure of an oronasal fistula with a myomucosal upper lip flap
Fechamento de fístula oronasal com retalho miomucoso labial superior
ABSTRACT
INTRODUCTION: Palatal fistula is the most common complication after palatoplasty, and its presence entails various implications. Its presentation is diverse and repair can be difficult, which is reflected in the existence of a numerous surgical techniques described for its treatment.
OBJECTIVE: To report the surgical correction of palatal fistula with a myomucosal upper lip flap, along with a brief review of the literature.
CASE REPORT: The patient underwent repair of complete cleft palate. At the immediate postoperative time, an anterior fistula of the hard palate and alveolar process was present and was subjected to a correction with an oronasal myomucosal upper lip flap. The patient progressed satisfactorily, without complications or lesion recurrence after 1 year of follow-up.
CONCLUSION: The technique presented is a simple and efficient method for correction of an anterior palatal fistula.
Keywords: Palatoplasty/complications; Palatal fistula; Myomucosal upper lip flap.
RESUMO
INTRODUÇÃO: A fístula palatina é a complicação mais frequente após palatoplastias e sua presença traz diversas implicações. Sua apresentação é diversificada e seu reparo pode ser difícil, o que se traduz na existência de uma diversidade de técnicas cirúrgicas descritas.
OBJETIVO: Relatar a correção cirúrgica de fístula palatina anterior com retalho miomucoso labial superior, além de fazer uma breve revisão da literatura.
RELATO DE CASO: Paciente submetido à correção de fissura palatina completa, apresentando, no pós-operatório mediato, fístula anterior de palato duro e processo alveolar, submetido à correção da fístula palatina oronasal com retalho miomucoso de lábio superior. O paciente evoluiu satisfatoriamente, sem complicações e sem recidiva da lesão após um ano de seguimento.
CONCLUSÃO: A técnica em questão mostrou-se simples e eficiente, prestando-se à correção da fístula palatal anterior.
Palavras-chave: Palatoplastia/complicações; Fístula palatina; Retalho miomucoso labial superior.
Mild to moderate mammary ptosis and changes in the positioning of the nipple-areola complex are frequent findings in patients who wish to undergo breast augmentation surgery1.2. The augmentation mastoplasty associated with mastopexy, especially in these intermediate cases, remains a controversial issue and of great interest to the plastic surgeon because it accounts for the highest rates of complications and postoperative patient dissatisfaction3.
The choice of an adequate surgical treatment is crucial because the simple placement of the breast implant without skin removal often results in the recurrence of ptosis4. On the other hand, corrections through larger scars, such as vertical incisions, in "L" or inverted "T", are less accepted by patients who have lower degrees of ptosis and asymmetry of the nipple-areola complex5,6. For these cases, we have used conical breast prostheses together with the removal of periareolar (circumareolar) skin, and round-block dermal sutures7.8. This approach offers a central access to the creation of a secure implant pocket, allows an accurate dissection in all directions, allows repositioning of the nipple-areola complex, and results in a less apparent scar that is camouflaged on the perimeter of the areola9,10.
Several authors have reported on their experiences with periareolar mastopexy and breast augmentation with various types, sizes, and locations of prostheses1,2,4,6,8-10. However, no studies were found on the use of conical silicone prostheses, which, in theory, could alleviate the problem of breast flattening.
OBJECTIVE
Our aim in this work is to evaluate a series of patients undergoing breast augmentation with periareolar mastopexy by using a polyurethane-coated conical silicone mammary prosthesis placed in a subglandular position. All patients were operated on by the same surgeon.
METHOD
We evaluated 22 patients who underwent breast augmentation with a conical prosthesis, by using periareolar mastopexy with the round-block technique, between February 2011 and February 2013.
We studied the following parameters: degree of ptosis, presence of changes in the position and size of the nipple-areola complex, postoperative complications, and patient satisfaction with the surgical outcome.
Surgical Technique (Figures 1 and 2)
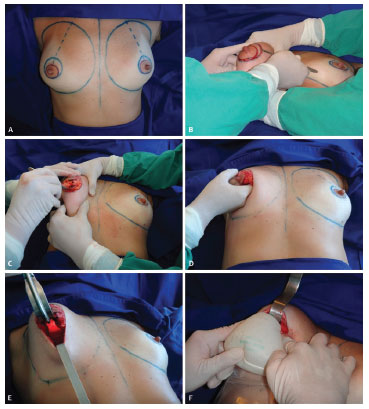
Figure 1. (A) Patient marked as described in text. (B) Resection of the circumareolar epidermis. (C) Semicircular infra-areolar incision up to the pectoral fascia. (D) Digital detachment in the subglandular plane. (E) Ample pocket prepared to receive the implant. (F) Placement of the conical prosthesis.
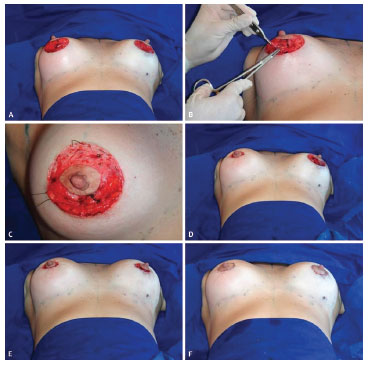
Figure 2. (A) Breasts with implants placed. (B) Approximation of glandular breast tissue with monocryl 3.0. (C) Round-block circular suture with mononylon 2.0 (before approaching the surrounding skin). (D) Right breast already with approximation of the surrounding skin with the round-block suture, up to the diameter of the 4-cm areolotome. (E) Both breasts after the round-block suture. (F) Result after the intradermal suture with monocryl 3.0 in the areolar perimeter.
With the patient in the standing position, the following markings are placed: middle line (from the sternal notch to the xiphoid process), breast meridians (midclavicular line that passes through the nipple), and inframammary fold. Thereafter, four points of reference are marked. Point A (superior) determines the desired height of the areola, being marked at the intersection of the breast meridian with a height corresponding to the middle third of the arm, normally between 18 and 20 cm from the sternal notch. Points B (distal), C (medial), and D (lateral) are determined by means of digital clamping, with a pinch test. The junction of these points forms a circular or slightly oval figure, which determines the extent of circumareolar skin area to be resected.
With the patient under general anesthesia or epidural anesthesia with sedation, in the 30º supine position, the region to be detached (superiorly at the height of the second intercostal space, medially to about 1 cm from the medial line, laterally on the anterior axillary line, and inferiorly in the inframammary fold) is marked. Marking with a 4-cm-diameter areolatome and the removal of the epidermis marked around the areola are performed. A semicircular infra-areolar incision is made through the breast parenchyma up to the pectoral fascia. The detachment is initially performed digitally (blunt), and then with scissors from the subglandular plane up to the previously defined margins. After the revision of hemostasis, the high or extra-high conical polyurethane-coated prosthesis is placed into the pocket, ensuring that the cone apex remains in place where the nipple-areolar complex is repositioned. The same procedure is repeated in the other breast.
Approximation of the breast tissue and subcutaneous tissue is done with a monocryl 3.0 suture. Then, a circular round-block suture in the deep dermis is done with mononylon 2.0, repositioning the surrounding skin up to the diameter of the 4-cm areolotome. Guidance sutures are placed in the four quadrants with mononylon 4.0. Intradermal suture with monocryl 3.0 is performed in the areolar perimeter. Dressing is applied with gauze, micropore, cotton pad, and compression with crepe bands.
Satisfaction Questionnaire
All patients responded to the satisfaction questionnaire below, with eight questions about the following aspects:
1) Aspect of the breast: natural or artificial.
2) Evaluation with scores of 1 to 4 (1-bad, 2-average, 3-good, or 4-excellent):a. Degree of satisfaction with the final result,
b. Form of the breasts,
c. Symmetry of the breasts,
d. Height of the breasts,
e. Quality of the scar,
f. Position of the areola,
g. Size of the areola.
RESULTS
The age of the patients at the time of surgery ranged from 22 to 55 years (mean, 33 years). The postoperative follow-up time ranged from 6 to 26 months (mean, 15 months).
Concerning the degree of ptosis, most patients presented with grade I and II ptosis, according to the classification of Regnault. Only five patients had grade III ptosis (Figure 3).
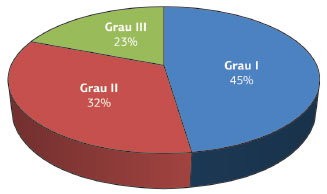
Figure 3. Degree of ptosis (according to the Regnault classification).
Concerning the presurgery position and the size of the nipple-areola complex, 19 patients exhibited asymmetry, 6 showed lateralization, and 4 had large areolas, with some combination in the same patient (Figure 4).
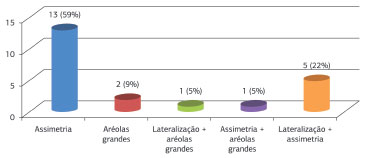
Figure 4. Changes in the position and size of the nipple-areola complex.
The volume of prostheses ranged from 215 to 380 mL, with the most frequently used being 300 mL and 345 mL. All prostheses were conical, 5 pairs with a high profile and 18 pairs with an extra-high profile. In four cases, prostheses of different volumes were used to balance differently sized breasts.
Complications related to the placement of the implant were evaluated, such as hematoma, seroma, infection, capsular contracture, undulations, palpable edge, or mobilization of the implant in the period studied. No complications were found.
There were two cases of enlargement of the scar; however, there were no cases of enlargement the areola, hypertrophic scar, or areolar necrosis. In most cases, wrinkling of the periareolar skin was initially observed; however, a complete improvement was observed between 1 and 2 months after the surgery in all cases.
In the satisfaction questionnaire, 21 of 22 patients were satisfied with the results. They considered the aspect of the breast to be natural in appearance (Figure 5), and gave good grades concerning the form, symmetry, and height of the breasts; quality of the scar; and position and size of areolas (Figure 6).
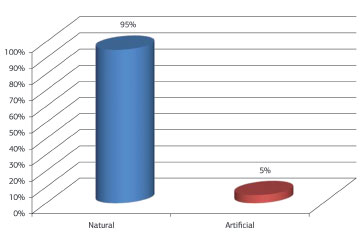
Figure 5. Patients' evaluation of the final aspect of the breasts.
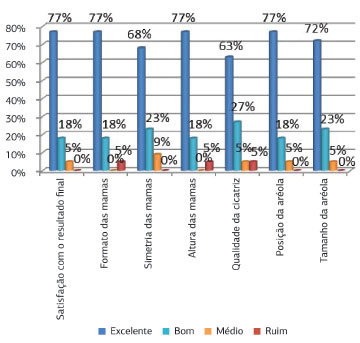
Figure 6. Results from the satisfaction questionnaire.
Photographs of the preoperative and postoperative period in some cases are shown in in Figures 7 to 11.
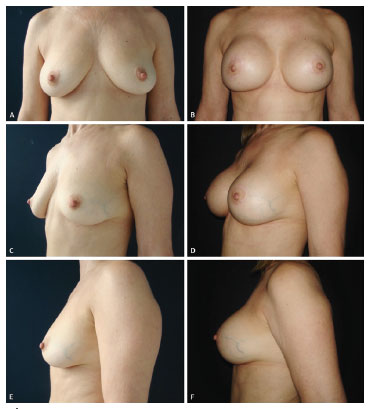
Figure 7. (A, C, E) Preoperative aspect of a 55-year-old patient with grade I ptosis who desired breast augmentation and breast pexy. (B, D, F) Postoperative aspect at 8 months after periareolar mastopexy with a conical prosthesis (300 mL, extra-high profile).
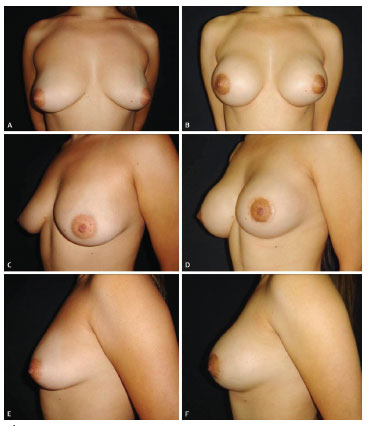
Figure 8. (A, C, E) Preoperative aspect of a 29-year-old patient with grade II ptosis, asymmetry, and sharp lateralization of the nipple-areola complex. (B, D, F) Postoperative aspect at 18 months after periareolar mastopexy with a conical prosthesis (280 mL, high profile).
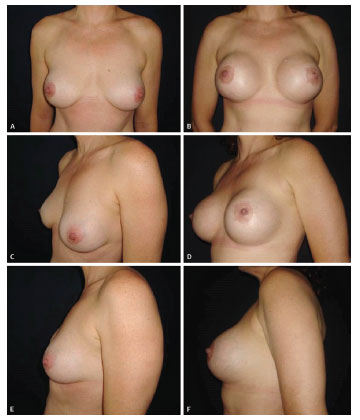
Figure 9. (A, C, E) Preoperative aspect of a 46-year-old patient with asymmetry and grade I ptosis, who already had a 220-mL breast prosthesis placed 10 years ago and wanted breast augmentation and pexy. (B, D, F) Postoperative aspect at 12 months after periareolar mastopexy and replacement with a conical prosthesis (380 mL, extra-high profile).
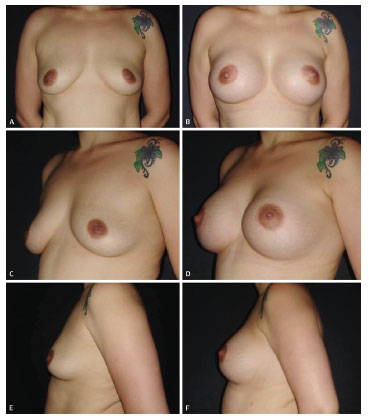
Figure 10. (A, C, E) Preoperative aspect of a 33-year-old patient with hypoplasia and grade I mammary ptosis. (B, D, F) Postoperative aspect at 18 months after periareolar mastopexy with a conical prosthesis (380 mL, extra-high profile).
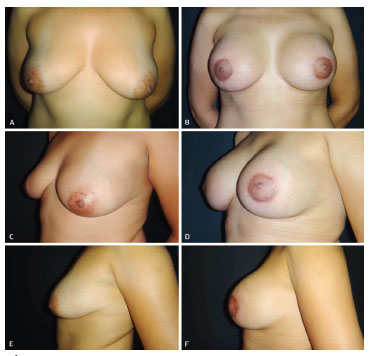
Figure 11. (A, C, E) Preoperative aspect of a 34-year-old patient with grade III ptosis, mammary asymmetry, and large and lateralized areolas. (B, D, F) Postoperative aspect at 6 months after periareolar mastopexy with conical prostheses (extra-high profile, 300 mL in the right breast and 345 mL in the left breast).
DISCUSSION
In the initial work on the use of periareolar mastopexy associated with breast augmentation, a high incidence of unsatisfactory results was reported, mainly owing to the enlargement of the areola, flattening of the breasts, and poor-quality scars, which occurred in up to 40% of cases9,11,12. In our study, however, we managed to obtain natural-looking breasts, with few complications and a good patient satisfaction index. This significant improvement of results has been reported in other recent studies1,2,4,10, and is due to the refinement of the technique and its indications, which will be discussed below.
In relation to the degree of ptosis, most patients (77%) presented with ptosis grades I and II, which, in most of the surgeries, were the main indications for this approach4. The three patients who had grade III ptosis had satisfactory results, and this extension of indication has been reported in more recent studies1,2,10. However, the case with the most advanced grade of ptosis (grade III) was the one that presented scar enlargement and an unsatisfactory result, according to the patient's own evaluation. This indicates that, in cases of more severe ptosis, the association of a vertical scar, in "L" or inverted "T", may give better results.
As shown in Figure 4, a large proportion of patients presented in the preoperative period, in addition to ptosis, other changes of the nipple-areola complex, such as asymmetry, lateralization, or large areolas. These changes occur with great frequency in patients and, when small to moderate, can be corrected or softened during the withdrawal of periareolar skin1,2. The correction of these changes in the nipple-areola complex is an important indication of the technique, especially in patients with mild ptosis, in which the simple placement of the implant, in some cases, would correct the ptosis but would not correct asymmetry, lateralization, or large areolas.
The size and shape of the prostheses used plays an important role in the final outcome. As mentioned above, the average volume used was 330 mL (not exceeding 380 mL). This average is in agreement with the literature that shows better results with moderate augmentation; thus, very large volumes should be avoided1,2,4. More recent studies have used better designed implants, with a high or an extra-high profile, in varying forms, to achieve more natural-looking breasts1,2,4,10. In this study, in addition to the use of high- and extra-high-profile prostheses, we suggest the use of conical implants, which has the advantage of presenting a higher projection of the areola and breast, avoiding breast flattening and therefore attaining the most natural result.
In this study, we did not find any complication related to the placement of the implant, such as hematoma, seroma, infection, capsular contracture, undulations, palpable edge, or implant mobilization. We attribute this result to a systematic and careful surgical technique, with blunt juxtamuscular dissection just above the fascia, creation of an ample pocket, washing with saline solution, and rigorous hemostasis. In addition, coating the implant with polyurethane may have helped because it was found to be related to a lower incidence of capsular contracture13.
Two cases of moderate scar enlargement were observed; however, no cases of hypertrophic scar or change in the form of the areola were observed (the enlargement, flattening, and distortion of the areola are the major complications of the periareolar technique)12,14,15. This result is mainly due to the conservative removal of periareolar skin and the round-block or continuous circumareolar suture technique, in the deep dermis8. This suture technique, which controls the tendency of areolar enlargement, allowed for the expansion of the application of various periareolar techniques7. In our patients, we used nylon 2.0 suture and a curved needle. Some studies have shown good results with the use of Gore-Tex, a heavy permanent suture that slides well in the dermis, with a straight needle14. Other studies propose that the periareolar incision should be made in zigzag form to achieve a more natural-looking final scar16. We believe that all improvements are possible; however, the key to controlling the size of the areola is the round-block technique associated with the conservative removal of periareolar skin.
As seen from the questionnaire answered by the patients (Figures 5 and 6), there is a good level of satisfaction with the surgery. From the review of the literature and the experience gained with these surgeries, we conclude that the ideal indications for breast augmentation with periareolar mastopexy are as follows7:
Large areolas in the preoperative period; Mild to moderate nipple and/or breast ptosis that cannot be corrected only with the implant; Congenital or acquired asymmetry, for which small adjustments are needed; Tuberous breasts; Replacement of implants.
Factors favorable to the technique should also be considered, such as breasts with moderate flaccidity, without streaks or skin dystrophies; small to moderate prosthesis volume, up to 380 mL; and elevation of the nipple areola complex <4 cm, preferably up to 2 cm2.
We attribute the results obtained in this study to a careful selection of patients, a combination of techniques, and the type of prosthesis used.
CONCLUSION
Periareolar (circumareolar) mastopexy with a conical breast prosthesis, by using the round-block suture, allows correcting various common problems, such as mild to moderate ptoses, asymmetries, and changes in the position and size of the nipple areola complex, without major scars or mobilization of breast tissue and resulting in natural-looking breasts with a good degree of patient satisfaction.
REFERENCES
1. Rancati A, Nava M, Tessari L. Simultaneous augmentation and periareolar mastopexy: selecting the correct implant. Aesthetic Plast Surg. 2010;34(1):33-41. http://dx.doi.org/10.1007/s00266-009-9440-y. PMid:20043160
2. Cannon CL 3RD, Lindsey JT. Conservative augmentation with periareolar mastopexy reduces complications and treats a variety of breast types: a 5-year retrospective review of 100 consecutive patients. Ann Plast Surg. 2010;64(5):516-21. PMid:20395815.
Spear SL, Boehmler JH 4th, Clemens MW. Augmentation/mastopexy: a 3-year review of a single surgeon's practice. Plast Reconstr Surg. 2006;118(Suppl 7):136S-47S. http://dx.doi.org/10.1097/01.prs.0000247311.12506.d7. PMid:17099493
4. Moreira M, Silva LC, Fagundes DJ. Mastopexy periareolar with mammary subfascial implantation in the treatment of the association of mammary hypotrophy and ptosis. Rev Bras Cir Plást. 2006;21(3):149-54.
5. de la Fuente A, Martín del Yerro JL. Periareolar mastopexy with mammary implants. Aesthetic Plast Surg. 1992;16(4):337-41. http://dx.doi.org/10.1007/BF01570697. PMid:1414659
6. Fayman MS, Potgieter E, Becker PJ. Outcome study: periareolar mammaplasty patients' perspective. Plast Reconstr Surg. 2003;111(2):676-87. http://dx.doi.org/10.1097/01.PRS.0000041391.44262.E2. PMid:12560688
7. Spear SL, Giese SY, Ducic I. Concentric mastopexy revisited. Plast Reconstr Surg. 2001;107(5):1294-300. http://dx.doi.org/10.1097/00006534-200104150-00032. PMid:11373576
8. Benelli L. A new periareolar mammaplasty: the "round block" technique. Aesthetic Plast Surg. 1990;14(2):93-100. http://dx.doi.org/10.1007/BF01578332. PMid:2185619
9. Rohrich RJ, Gosman AA, Brown SA, Reisch J. Mastopexy preferences: a survey of board-certified plastic surgeons. Plast Reconstr Surg. 2006;118(7):1631-8. http://dx.doi.org/10.1097/01.prs.0000248397.83578.aa. PMid:17102738
10. Stoff-Khalili MA, Scholze R, Morgan WR, Metcalf JD. Subfascial periareolar augmentation mammaplasty. Plast Reconstr Surg. 2004;114(5):1280-91. http://dx.doi.org/10.1097/01.PRS.0000135906.48388.22. PMid:15457050
11. Spear SL, Kassan M, Little JW. Guidelines in concentric mastopexy. Plast Reconstr Surg. 1990;85(6):961-6. http://dx.doi.org/10.1097/00006534-199006000-00023. PMid:2088318
12. Baran CN, Peker F, Ortak T, Sensöz O, Baran NK. Unsatisfactory results of periareolar mastopexy with or without augmentation and reduction mammoplasty: enlarged areola with flattened nipple. Aesthetic Plast Surg. 2001;25(4):286-9. http://dx.doi.org/10.1007/s002660010138. PMid:11568833
13. Miró AL. Polyurethane-coated silicone breast implants: evaluation of 14 years' experience. Rev Bras Cir Plást. 2009;24(3):296-303.
14. Hammond DC, Khuthaila DK, Kim J. The interlocking Gore-Tex suture for control of areolar diameter and shape. Plast Reconstr Surg. 2007;119(3):804-9. http://dx.doi.org/10.1097/01.prs.0000251998.50345.e9. PMid:17312481
15. Hinderer UT. Circumareolar dermo-glandular plication: a new concept for correction of breast ptosis. Aesthetic Plast Surg. 2001;25(6):404-20. http://dx.doi.org/10.1007/s0026601-0015-9. PMid:11731846
16. Gryskiewicz JM, Hatfield AS. "Zigzag" wavy-line periareolar incision. Plast Reconstr Surg. 2002;110(7):1778-84. http://dx.doi.org/10.1097/00006534-200212000-00024. PMid:12447064
1. Full Member, Sociedade Brasileira de Cirurgia Plástica (SBCP), Brasília, DF, Brazil
2. Associate Member, Sociedade Brasileira de Cirurgia Plástica (SBCP), Brasília, DF, Brazil
Institution: Work performed at the Cardoso Clinic, Brasilia, DF, Brazil.
Corresponding author:
Igor Felix Cardoso
SQS 311, Bloco D, Apartamento 504 - Asa Sul
Brasília, DF, Brazil CEP 70364-040
E-mail: igorfelixcardoso@gmail.com
Article received: July 15, 2013.
Article accepted: February 4, 2014.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter