

Original Article - Year 2014 - Volume 29 -
Aesthetic evaluation of two omphaloplasty techniques
Avaliação estética da cicatriz umbilical em duas técnicas de onfaloplastia
ABSTRACT
INTRODUCTION: The treatment of umbilical scarring is important in abdominoplasty, and many omphaloplasty techniques are described in the literature.
OBJETIVE: The objective of this work is to compare the aesthetic result of omphaloplasty with the star technique and the diamond technique.
METHOD: Twenty patients were evaluated through scoring, by using five criteria: shape, location, scar, size, and depth.
RESULT: The patients showed significantly higher scores when evaluating the shape criterion during an omphaloplasty; the star technique scored, on average, 15.8 ± 2.05, whereas the diamond technique scored 12.6 ± 3.65 (p = 0.03). No significant difference was found in all other criteria (location, size, depth, and scar).
CONCLUSION: This study demonstrates that the star technique produces better aesthetic results than the diamond technique.
Keywords: Umbilicus; Plastic Surgery; Omphaloplasty; Star Omphaloplasty; Diamond Omphaloplasty.
RESUMO
INTRODUÇÃO: O tratamento da cicatriz umbilical é um tempo muito importante na plástica abdominal. Existem várias técnicas descritas de onfaloplastia na literatura.
OBJETIVO: Este trabalho tem com objetivo comparar o resultado estético de onfaloplastias com as técnicas em estrela e losango.
MÉTODO: Foram avaliados os resultados de 20 pacientes, por meio de pontuação, utilizando cinco critérios: formato, localização, cicatriz, tamanho e profundidade.
RESULTADO: As pacientes apresentaram somatória significativamente maior de pontos no critério que avaliou o formato da onfaloplastia, sendo utilizada a técnica em estrela 15,8± 2,05, quando comparada com a técnica de onfaloplastia em losango 12,6± 3,65 com p=0,03. Nos demais critérios de localização, tamanho, profundidade e cicatriz não houve diferenças significantes.
CONCLUSÃO: O estudo demonstrou que a técnica em estrela apresentou melhores resultados estéticos no critério de formato do que a técnica em losango.
Palavras-chave: Umbigo; Cirurgia Plástica; Onfaloplastia; Onfaloplastia em Estrela; Onfaloplastia em Losango.
The umbilicus is the first visible scar formed naturally in humans. It is formed owing to the invagination of the umbilical cord stump when the umbilical cord conjunctive tissue undergoes necrosis. The umbilicus, or the navel, is a scar anchored in the pubic midline through the umbilical pedicle. The appearance of the umbilicus may change with age and is influenced by the thickness of abdominal fat, body weight changes, pregnancy, hernias, and abdominal scars. Dick1 studied the anatomy of the navel and found four fibrous cords deeply attached to its surface, pulling it into the body. These fibrous structures correspond to the remains of the obliterated umbilical vein, the urachus, and two umbilical arteries.
The navel is an essential component to the aesthetic appearance of the abdomen, and periumbilical scars resulting from abdominoplasty may negatively influence the final outcome of a well-operated abdomen.
Omphaloplasty was first performed in 1924, when Frist made the first navel transposition. Since then, many geometric shapes have been designed to mimic the original scar2.
Flesch-Thebesiuse Weisheimer, in 1931, kept a skin triangle in the navel.
Others discarded the navel and opted to perform neoomphaloplasty3. In 1949, Pick stressed the importance of conserving the navel in women for aesthetic reasons4.
The concern about keeping the navel began with Vernoni in 1957, in which the navel was transposed by using circular incisions; however, this led to many navel stenoses5.
Brazilian authors have reported various geometric forms, such as Ribeiro, Viterbo, and Saldanha2-5, as well as many shapes such as three-pointed star, diamond, ellipses, crosses, clovers, rectangles, and shield-shaped (with a straight line at the top and a U-shaped bottom)6.
The search for the "ideal navel" is still ongoing; however, three points are well established: (i) a circular scar should be avoided to eliminate the possibility of subsequent stenosis; (ii) the attachment to the aponeurosis is important to hide the scar and achieve a greater depth; and (iii) a visible scar around the navel is the most important aesthetic limitation of abdominoplasty7.
This work aims to evaluate the aesthetic outcomes of two omphaloplasty techniques: star and diamond.
OBJECTIVE
The objective of this work is to compare the aesthetic result of omphaloplasty with the star technique and the diamond technique.
METHOD
Casuistry
This was a prospective study carried out from August 2012 to July 2013, in which 20 patients undergoing lipoabdominoplasty were evaluated. They were divided into two groups of 10 patients each, as follows:
Group 1 (10 patients): star-shaped omphaloplasty;
Group 2 (10 patients): diamond-shaped umbilicoplasty.
The patients' age, underlying disease, smoking habits, body mass index (BMI), menopause, and contraceptive use were considered.
Inclusion criteria
The inclusion criteria were as follows: female, American Society of Anaesthesiologists (ASA) physical status 1 and 2, undergoing lipoabdominoplasty, BMI <30, and age 25-52 years.
All patients underwent cardiac and anesthetic consultation, and were assessed according to the ASA classification preoperatively.
Exclusion criteria
Patients with a history of scar change, underlying disease, and umbilical hernia, as well as postbariatric patients were excluded from the study.
To evaluate the aesthetic results, nine evaluators were divided into three groups: group 1, the patient and a layman; group 2, four third-year plastic surgery residents; and group 3, three plastic surgeons who are members of the Brazilian Society of Plastic Surgery. The omphaloplasty of each patient was evaluated subjectively by using five criteria: shape, location, scar, size, and depth. The FMUSP rating scale was adapted 18:9, with zero score (0) = bad, 1 = fair, and 2 = good, applied individually for each patient and each of the nine evaluators (Table 1).
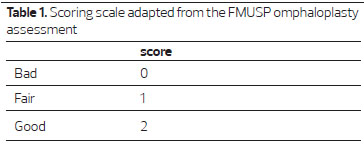
The final score was the sum of all scores in each criterion for each patient. Statistical analysis was performed by using the paired Student's t-test for each of the five criteria.
The results are presented as means and standard deviations (SDs), and the significance level was set as p < 0.05.
SURGICAL TECHNIQUES
Star technique
At the end of lipoabdominoplasty, marking is done with a "cross" on the abdominal wall, ±2cm vertically and 1.5cm horizontally, after centering and measurement of the navel. The incisions of the two lines result in four triangular flaps. The distal portions are resected for better accommodation to the umbilical pedicle.
The umbilical pedicle is previously incised in a diamond shape, degreased, and secured with simple stitches in the aponeurosis of the rectus abdominis muscle, as deep as possible.
The abdominal wall around the navel is not degreased.
The flaps, the abdominal wall to the umbilical pedicle, are sutured with monocryl 4.0 in the subcutis. Separate sutures with mononylon 5-0 are placed for skin coaptation. Healing is induced by applying gauze in the umbilical cavity, and the stitches are removed on the 12th postoperative day.
Diamond technique
After measuring and centering of the umbilicus, the abdominal wall is marked with a diamond shape, ±2cm vertically and 1.5cm horizontally.
The umbilical pedicle is also shaped as a diamond and fixed to the aponeurosis of the rectus abdominis muscle in a deep position. The subdermal sutures and skin coaption are performed similarly to the star technique. The removal of stitches also follows the same procedure.
The authors declare that there is no conflict of interest in this study.
RESULTS
Among the patients who met the inclusion criteria, there was no statistical difference in age between the group operated with the diamond technique and that with the star technique (p = 0.38). BMI ranged from 22 to 30, also with no statistical difference observed between the two groups (p = 0.11) (Table 2).
For the statistical evaluation concerning the omphaloplasty shape, the patients of the star group had a significantly higher mean (15.8 ± 2.05) than the diamond group (12.6 ± 3.65) (p = 0.03) in Student's paired t-test (Figure 1 and Table 3).

Figure 1. Score for the umbilical shape after omphaloplasty for the diamond vs. the star technique. *p = 0.03 (Student's t-test).

Throughout the study, only one patient in the star group presented a keloid scar that was treated with an intralesional injection of triamcinolone, at three sessions every 2 weeks, and with satisfactory results.
Concerning the location, the postomphaloplasty analysis of the scar depth and size showed no significant difference between groups (Figures 2-5 and Table 3).

Figure 2. Score for the postomphaloplasty umbilical location for the diamond technique vs. the star technique. p = 0.84 (Student's t-test).

Figure 3. Score for the postomphaloplasty umbilical scarring for the diamond technique vs. the star technique. p = 0.30 (Student's t-test).

Figure 4. Score for the postomphaloplasty umbilical size for the diamond technique vs. the star technique. p = 0.67 (Student's t-test).

Figure 5. Score for the postomphaloplasty umbilical depth for the diamond technique vs. the star technique. p = 0.19 (Student's t-test).
DISCUSSION
The ideal appearance of the umbilicus in abdominoplasty is still a challenge. Various techniques are recommended.
Circular incisions tend to have a higher possibility of causing stenosis and scar retraction of the navel than those that preserve all the skin of the wall, and are made with patched scars. Besides avoiding complications such as stenosis and scar retraction, the search for a suitable technique for optimal aesthetic results has led to the implementation of other techniques with other geometric shapes, such as three-pointed stars, diamonds, ellipses, and crosses, among others10-13.
In our patients, the use of the diamond or the star technique led to no such complications. Only one patient in the star group had a hypertrophic scar; however, it was not due to the technique but probably to an idiosyncratic reaction. This patient was treated with 20mg/dL triamcinolone for three sessions, with good results.
The aesthetic result of the two omphaloplasty techniques, evaluated by plastic surgeons, residents of plastic surgery, and the patients themselves as well as a layman, had good overall results. The nondegreasing of the abdominal wall around the navel prevents visible umbilical scarring, giving a natural look to the navel.
There was no significant difference in the location of the navel, which depends on the surgeon's technique. However, there was a significant difference in favor of the star technique when the aesthetic appearance of the navel shape was compared. In the other criteria evaluated, no significant differences were observed.
The scores of residents were lower than those of plastic surgeons, and this may be due to a greater demand for good results.
CONCLUSION
The star and the diamond techniques showed similar results in the evaluation of location, scar size, and depth in omphaloplasty. The star technique showed excellent aesthetic results and a significantly higher score than the diamond technique when the shape was evaluated.
REFERENCES
1. Dick ET. Umbilicoplasty as a treatment for persistent umbilical infection. Aust N Z J Surg. 1970;39(4):380-3.
2. López-Tallaj L, Gervais J. Restauração umbilical na abdominoplastia: uma simples técnica retangular. Rev Bras Cir Plast. 2001;16(3):39-46.
3. D'Assumpção EA. Técnica para umbilicoplastia, evitando-se um dos principais estigmas das abdominoplastias. Rev Bras Cir Plast. 2005;20(3):160-6.
4. Mello DF, Yoshino H. Plicatura da base umbilical: proposta técnica para tratar protrusões e evitar estigmas pós-abdominoplastia Rev Bras Cir Plast. 2009;24(4):525-9.
5. Saldanha OR, De Souza Pinto EB, Mattos WN Jr, Pazetti CE, Lopes Bello EM, Rojas Y, et al. Lipoabdominoplasty with selective and safe undermining. Aesthetic Plast Surg. 2003;27(4):322-7.
6. Salles AG, Ferreira MC, do Nascimento Remigio AF, Gemperli R. Evaluation of aesthetic abdominal surgery using a new clinical scale. Aesthetic Plast Surg. 2012;36:49-53.
7. Saldanha OR, et al. Aesthetic Evaluation of lipoabdominoplasty in overweight patients. Plast Reconst Surg. 2013: 132(5):1103-12.
8. Vernon S. Umbilical transplantation upward and abdominal contouring in lipectomy Am J Surg. 1957;94(3):490-2.
9. Baack BR, Anson G, Nachbar JM, White DJ. Umbilicoplasty: the construction of a new umbilicus and correction of umbilical stenosis without external scars. Plast Reconstr Surg. 1996;97(1):227-32
10. Ferreira MC. Evaluation of results in aesthetic plastic surgery: Preliminary. observations on mammaplasty. Plast Reconstr Surg. 2000;106:1630-35; discussion 1636.
11. Rebello CT. Cirurgia estética. Rio de Janeiro: 1977.
12. Salles AG, Ferreira MC, do Nascimento Remigio AF, Gemperli R. Evaluation of aesthetic abdominal surgery using a new clinical scale. Aesthetic Plast Surg. 2012;36:49-53.
13. Sinder R. Cirurgia plástica do abdome. Rio de Janeiro: Ed. Ramil Sinder;1979.
1 - Resident of Plastic Surgery Service "Dr. Ewaldo Bolivar de Souza Pinto" - UNISANTA. Aspirant Member of SBCP
2 - Tutor in the Plastic Surgery Service "Dr. Ewaldo Bolivar de Souza Pinto" - UNISANTA. Member of SBCP
3 - Director of the Plastic Surgery Postgraduate Course in UNISANTA. Member of SBCP
4 - Resident of Plastic Surgery Service "Dr. Ewaldo Bolivar de Souza Pinto" - UNISANTA. Aspirant member of SBCP
5 - Instructor in the Plastic Surgery Service "Dr. Ewaldo Bolivar de Souza Pinto" - UNISANTA. Member of SBCP
Institution: University Santa Cecilia.
Corresponding author:
Debora de Paula Ramos Castro
R. Desembargador Eliseu Guilherme 301 - Paraíso
São Paulo - Brazil
E-mail: dradeboracastro@yahoo.com.br
Article received: January 28, 2014
Article accepted: June 1, 2014



 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter