

Original Article - Year 2014 - Volume 29 - Issue 2
Epidemiology of patients with facial fractures treated by the plastic surgery team in an emergency room in the Federal District of Brazil
Epidemiologia da fratura de face de pacientes atendidos no pronto socorro de cirurgia plástica do Distrito Federal
ABSTRACT
INTRODUCTION: Trauma remains a major cause of morbidity and mortality amongst young adults in the Western world. The prevalence of traumatic lesions on the face is especially high, as the facial area is generally exposed with little protection.
OBJECTIVE: To evaluate the etiology, age, sex, location, symptoms, and the type of treatment given to victims of facial trauma treated at the North Wing Regional Hospital (NWRH), Brasilia, Federal District.
METHOD: This was a retrospective study conducted in the emergency room of the NWRH to evaluate the epidemiological profile of patients with facial trauma who presented during the 2nd half of 2012.
RESULTS: The study included 46 patients, of which 32 patients (69.56%) were male. Physical aggression was the prevailing cause in both sexes with 22 cases (47.82%), followed by falls with 11 (23.91%). Falls were the predominant cause of injuries in children. Physical aggression as a mechanism for facial trauma became more common with age. The main age group affected was the 21 to 30 years group, comprising 43.47% of cases. The nose was the most commonly affected bone in facial fractures, with nasal fractures occurring in 62.96% of cases. The mean hospital stay was two days and the mean time between the first visit and the operation was six days.
CONCLUSION: The predominant epidemiological profile of a patient with facial fracture is that of a young male, victim of physical aggression, presenting with a nasal fracture and a clinical picture of this type of injury, and treated with closed reduction.
Keywords: Plastic Surgery; Facial Injuries; Physical Aggression.
RESUMO
INTRODUÇÃO: O trauma permanece como uma das principais causas de morbidade e mortalidade, no mundo ocidental, entre os adultos jovens. A prevalência de lesões traumáticas na face é alta devido à enorme exposição dessa região e a sua pouca proteção.
OBJETIVO: Avaliar a etiologia, a idade, o gênero, a localização, os sintomas e o tipo de tratamento das vítimas de traumas de face dos atendidos no Hospital Regional da Asa Norte (HRAN), Brasília, Distrito Federal.
MÉTODO: Trata-se de um estudo retrospectivo, realizado no pronto socorro do HRAN-DF, visando avaliar o perfil epidemiológico de vítimas de trauma de face, no período do 2º semestre de 2012.
RESULTADOS: O estudo compreendeu 46 pacientes, destacando-se o gênero masculino, com 32 pacientes (69,56%). Quanto à causa, predominou a agressão física, em ambos os sexos, com 22 casos (47,82%), seguida pelas quedas, com 11(23,91%). As quedas foram as causas predominantes das lesões em crianças, mas se verificou a participação cada vez maior da agressão física como mecanismo de trauma facial com o aumento da idade. A principal faixa etária foi de 21 a 30 anos, compreendendo 43,47% dos casos. O nariz foi o local mais acometido nas fraturas de face, correspondendo a 62,96% dos casos. O tempo médio de internação foi de dois dias e o tempo entre o primeiro atendimento e a operação foi de seis dias.
CONCLUSÃO: O perfil epidemiológico do paciente com fratura de face é de um jovem, do gênero masculino, vítima de agressão física, com fratura de nariz e quadro clínico desse tipo de lesão e submetido a redução fechada.
Palavras-chave: Cirurgia Plástica; Traumatismos Faciais; Agressão Física.
Traumas are among the leading causes of death and morbidity in the world1-8. Among the various types of trauma, facial trauma stands out as one of the most important, since its consequences can include emotional repercussions, functional difficulties, and the possibility of permanent deformities.
Facial traumas make up 7.4%-8.7% of emergency care3.18. A large proportion of serious trauma cases involve facial lesions due to the exposure and scarce protection afforded to this region.
Facial traumas are among the most frequent diagnoses in patients presenting to the emergency room, either alone or associated with multiple trauma. Trauma care should be systematic and multidisciplinary to provide the proper sequence of care in severe cases and avoid missing possible fractures in mild trauma.
Knowledge of the data of facial trauma regarding the prevalence of sex, causative events, association of trauma with alcohol consumption, and treatment methods and its complications, is of vital importance to a better understanding of the problems faced in trauma management, to contribute to the implementation of preventive, educational and technical measures to achieve an excellent standard of care in the management of lesions. Unfortunately, this information is still scarce in Brazil compared to other countries.
OBJECTIVE
This study aims to evaluate the epidemiological profile of facial trauma victims treated at the Plastic Surgery Service of the North Wing Regional Hospital, Brasilia, Federal District, in the second half of 2012. This is to enable the creation of data sources to guide the implementation of preventive measures by the Health Department of the Federal District, and the treatment of this type of trauma.
METHOD
This is a retrospective study in which data were collected through analysis of medical and emergency care documents (GAEs) of patients seen under the plastic surgery department emergency service at the North Wing Regional Hospital (HRAN - Hospital Regional da Asa Norte), Brasilia, Federal District, in the second half of 2012.
All patients with facial trauma seen in the emergency room of HRAN by the plastic surgery team in the second half of 2012 were included. The exclusion criteria were patients who had GAEs that were incomplete or lacking important information for the analysis, and those who had already received treatment in other hospitals.
Data were collected using a data collection sheet that included the following variables: age, sex, cause of accident, face injury signs, symptoms, location, types of treatment given, and length of hospital stay.
The cases were classified according to etiology into seven categories: physical aggression (including interpersonal violence), bites, car and motorcycle accidents (including collision with other vehicles, poles, walls, houses and falling from motorcycle), sport (including various forms of sport, including martial arts), bicycle accident, fall from height, and impact unrelated to falls.
In impact unrelated to the fall, we included direct collision trauma with furniture, fixtures, and structural elements both inside and outside the home.
Data were analyzed and coded by Epi Info software, version 3.2.2. The project was approved by the Committee of Ethics in Research of the Health State Department of the Federal District.
RESULTS
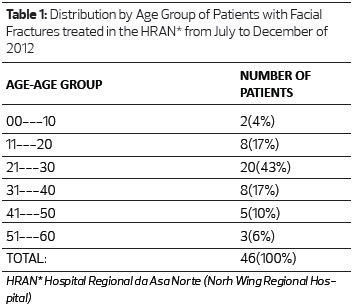
The study included 46 patients, of whom 32 (69.56%) were male. The age group with the highest prevalence of facial trauma was 21 to 30 years, comprising 43.47% of the entire study population. The mean age was 29 years (range 1-60 years) (Table 1).
Regarding the cause of facial trauma (Table 2), the predominant cause was physical aggression, corresponding to 22 (47.82%) cases. Second was falls, accounting for 11(23.91%) cases and, thirdly, car accident, with 5 (10.86%) cases (Figure 1).
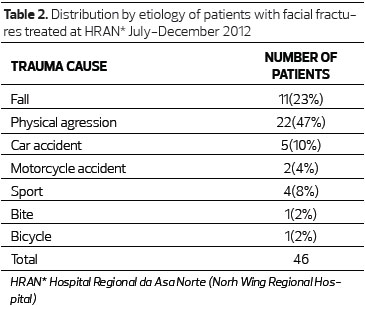
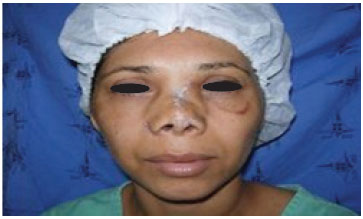
Figure 1. After car accident nasal fracture
By evaluating the nature of facial traumas related to age, we found that 4% of children aged 0 to 10 years suffered a fall from their own height. In the 11-50 years age group, physical aggression was the main cause of facial trauma. However, the main cause of facial trauma in patients older than 50 years was a fall from their own height, corresponding to 6% of cases.
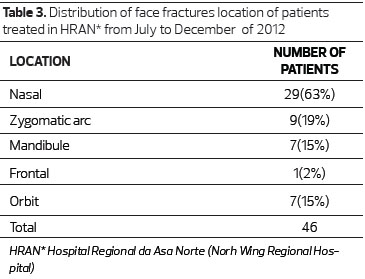
The nose was the most commonly affected area in facial fractures in 62.96% of cases (Table 3). The second most affected region was the zygomatic arch, with 19.56% of cases, and tied for third place were the jaw and the orbit, with 15.21% of cases each. Eight (17.39%) patients had more than one fracture: the zygoma and orbit were fractured in 6 (13%) patients, the nose, orbit and frontal bone in 1patient (2%), and the nose and orbit in 1 patient (2%). (Table 3)
The average time between the trauma and the first visit was 2 days and between trauma and surgery was 6 days.
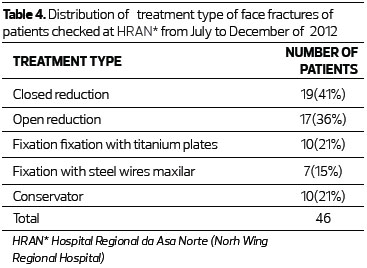
The most common treatment, given in 41% of cases, was the closed reduction of nasal bone fractures with the use of Asch forceps, followed by the isolated use of plates and screws for rigid internal fixation in 21% of cases.
Of those patients with nasal fractures who were treated with open surgery, a costal cartilage graft (Figures 1-3) was used for nasal reconstruction in x patients (y%). For the cases undergoing open reduction and bone fixation except for nose fracture, we used rigid internal fixation, either alone or associated with methods such as osteosynthesis with steel wire and jaw blockage, in 36% of patients. These data confirm rigid internal fixation as the currently preferred method when there is need for osteosynthesis (Table 4).
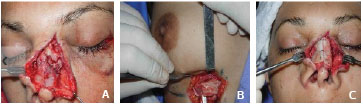
Figure 2. Intraoperative : (A) fracture of the Framework , ( B ) costal cartilage graft and ( C ) fixation of the graft to the back and tip .
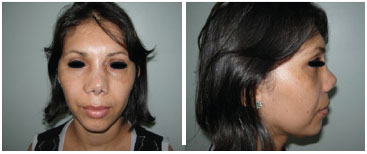
Figure 3. Late post - operative (6 months).
Non-surgical conservative treatment was used in 21.73% of the study patients, mostly those with nasal fractures without sinking, lateral deviation, or nasal obstruction.
The average length of inpatient stay at NWRH was two days.
DISCUSSION
There is a high prevalence of facial fractures among patients at any emergency facility. These need systematic care in order to avoid sequelae, which are often difficult to treat and carry significant additional costs.
Three decades ago, studies indicated that accidents by motor vehicles were the main cause of facial traumas1-7. However, there is an increasing significance of physical aggression as a facial trauma mechanism in Brazil1-10. Similar findings have been described by Borghese et al. , with 31.8% of the cases, and also by Masako et al. with 29% of cases in other countries; this trend was also present in this study, with a prevalence of 47.82% of victims7-18.
In addition, public policies seeking greater control and penalties for speeding on the roads and the lack of seat belt use have contributed to the decrease in the incidence of facial trauma due to motor vehicle accidents.
The introduction of safety devices, including compulsory use of seat belts, "air bags", side protection bars and a ban on drinking and driving, has not only decreased the rates of car accidents as a cause of facial trauma, but has also reduced facial8,9,12 fracture complexity. Covington et al. showed that the adoption of seat belts in the US over a period of 10 years reduced the incidence of multiple facial fractures from 46.3% to 20.1%. This is similar to data found in this study, with 17.39% of cases having multiple facial fractures.
This is also confirmed in the study by Goldenberg et al., in which they operated on 265 patients with facial fractures following traffic accidents, of which 215 were pedestrians who were run over and 92 were in cars. In car accidents, 29 of the patients using seat belts showed mild traumatic brain injury (TBI) and 8 severe TBI, vs. 32 and 13 of those who were unbelted, respectively. The maxilla was the most commonly fractured bone in both groups: with belt there were 23 fractures, and without belt 50 fractures. The belted group showed an average of 2.2 fractured bones per patient vs. 3.4 in the unbelted group (p<0.01). Comminuted fractures occurred in 29.5% of cases with seatbelts and 46.3% of cases without (p<0.01)18.
In Brazil, district laws regulate the increasing number of electronic barriers to reduce the speed of vehicles on the roads, and the mandatory use of seat belts in cars and crash helmets by motorcycle drivers, as well the fact that all vehicles must stop at the track while a pedestrian is crossing. Such measures may have contributed to the reduction of facial trauma resulting from pedestrians being run over and accidents with vehicles and motorcycles.
The capital is surrounded by satellite cities and several other cities in the states of Goiás and Minas Gerais, which make up the geo-economic region of the Federal District around Brasilia. These cities have had a high population growth in recent years. One example is the town of Águas Lindas de Goiás, which is in the vicinity of the Federal District and is considered to have the fastest population growth in Brazil in recent years. However, the opportunities for employment and economic growth in these cities have increased at a much lower rate, contributing to the increase in cases of violence throughout the Federal District.
Most patients seen at HRAN have low purchasing power, among other socioeconomic problems. The increase in urban violence is associated with the socioeconomic and emotional conflicts that individuals, especially young people, are subjected to.
In the recent studies that did not show this etiological change in facial traumas6,12-14, the reason may be the inclusion of trauma victims from the eighties and nineties, during which the use of protective equipment in traffic was not widespread, particularly in Brazil.
In certain regions of the country and the world, the use of the bicycle as a means of recreation and transport is very common. This increases the possibility of accidents with this type of vehicle. In this study, bicycle falls were the cause of facial trauma in a small number of patients.
A fall from their own height proved to be an important mechanism of trauma at the extremes of age, which was also observed in the study of Masako et al., in which this was the cause of trauma in 55% of patients younger than 10 years old and in 85% of those aged over 60 years. Aging gradually decreases the biological functions of people, triggering multiple deficits in sensation, cognition and memory, which when associated with the use of psychotropic drugs and musculoskeletal diseases, increases the risk of falling18.
Falls accounted for the cause of facial injuries in the majority of children. With increasing age, an increase in the prevalence of facial fractures is seen, and aggression becomes the main cause, as also confirmed by other studies15-17. Multiple factors can produce a fall. It is an important mechanism of facial trauma in children since locomotion and balance are under development; furthermore, they have reduced awareness of danger5-18.
The nose is the main site of facial fractures (62.96%), followed by the zygoma (16.66%). This fact was consistent with other studies3,14-17, but contrary to the study of Masako et al., in which the orbit was the most affected region in 48% of cases, followed by nasal fracture, with 33%7. The reason for this lies in the fact that the nose occupies a central position in the face and can be easily fractured as the nasal bones are thin. The main cause of nasal fracture is physical aggression, which was also present in 29% of patients in the same study by Masako et al18-20.
Overall, physical aggression was the main cause of facial trauma in patients seen in the HRAN emergency room by the plastic surgery team. This knowledge is important to enable public services to be targeted towards patients with this type of injury in the Federal District.
CONCLUSION
The predominant epidemiological profile of patients with facial fractures treated at the Plastic Surgery Service of the North Wing Regional Hospital of Brasilia is young, male, a victim of physical aggression, with nose fracture and clinical characteristics of this type of injury (epistaxis, periorbital ecchymosis, nasal deviation, and nasal obstruction) and treated with closed reduction of the fracture.
REFERENCES
1. Wulkan M, Parreira JR, Botter DA. Epidemiologia do trauma facial. Rev Assoc Med Bras. 2005;51(5):290-5.
2. Kelley P, Crawford M, Higuera S, Hollier LH. Two hundred ninety four consecutive facial fractures in an urban trauma center: lessons learned. Plast Reconstr Surg. 2005;116(3):42e-9.
3. Brasileiro BF, Passeri LA. Epidemiological analysis of maxillofacial fractures in Brazil: a 5-year prospective study. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2006;102(1):28-34.
4. Filho EF, Fadul Jr. R, Azevedo RA, et al. Fraturas de mandíbula: análise de 166 casos. Rev Assoc Med Bras. 2000;46(3):272-6.
5. Sastry SM, Sastry CM, Paul BK, Bain L, Champion HR. Leading causes of facial trauma in the major trauma outcome study. Plast Reconstr Surg. 1995;95(1):196-7.
6. B. Borghese, Calderoni DR, Passeri LA. Estudo retrospectivo da abordagem das fraturas nasais no Hospital das Clínicas da UNICAMP. Ver Soc Bras Cir Plást.2011;26(4):608-612.
7. Ugueto WF, As AJ, Fonseca AS, Barreira GC, Antunes RB, Bastos E, Goldenberg DC, et al. Trauma crânio-maxilo-facial e a influência do uso de cinto de segurança e capacete: Nove anos de seguimento. Rev Bras Cir Craniomaxilofacial. 2010;(13):23-23.
8. Passeri LA, Ellis E, Sinn DP. Relationship of substance abuse to complications with mandibular fractures. J Oral Maxillofac Surg. 1993;51(1):22-5.
9. Thaller SR, Kawamoto HK. Care of maxillofacial injuries: survey of plastic surgeons. Plast Reconstr Surg. 1992;90(4):562-7.
10. Covington DS, Wainwright DJ, Teichgraeber JF, Parks DH. Changing patterns in the epidemiology and treatment of zygoma fractures: 10-year review. J Trauma. 1994;37(2):343-8.
11. Lindqvist C, Sorsa S, Hyrkäs T, Santavirta S. Maxillofacial fractures sustained in bicycle accidents. Int J Oral Maxillofac Surg. 1986;15(1):12-8.
12. Karlson TA. The incidence of hospital-treated facial injuries from vehicles. J Trauma. 1982;22(4):303-10.
13. Rhee SC, Kim YK, Cha JH, Kang SR, Park HS. Septal fracture in simple nasal bone fracture. Plast Reconstr Surg. 2004;113(1):45-52.
14. Iida S, Hassfeld S, Reuther T, Schweigert HG, Haag C, Klein J, et al. Maxillofacial fractures resulting from falls. J Craniomaxillofac Surg. 2003;31(5):278-83.
15. Brook IM, Wood N. Aetiology and incidence of facial fractures in adults. Int J Oral Surg. 1983;12(5):293-8.
16. Van Beek GJ, Merkx CA. Changes in the pattern of fractures of the maxillofacial skeleton. Int J Oral Maxillofac Surg. 1999;28(6):424-8.
17. Macedo JLS, Camargo LM, Fragoso PA, Correa SR. Mudança Etiológica do Trauma de Face de Pacientes Atendidos no Pronto Socorro de Cirurgia Plástica do Distrito Federal. Rev Bras Cir Plast 2007;22(4):323-5.
18. Pereira MD, Kreninski T, Santos RA, Masako LF. Trauma Craniofacial: Perfil epidemiológico de 1223 fraturas atendidas entre 1999 e 2005 no Hospital São Paulo - UNIFESP-EPM. Rev Soc Bras Cir Craniomaxilofac. 2008;11(2):47-50.
19. Ugueto WF, Sa AJ, Foscenca AS, Barreira GC, Antunes RB, Bastos E, Goldenberg DC, Utsomia K, Alonso NA. Influência da "lei seca" no padrão das fraturas de face operadas no HCFMUSP Rev Bras Cir Craniomaxilofacial. 2010;(13):97-101.
20. Abreu RA, Martins W, Faria JC. Análise prospectiva das fraturas de face na população idosa do hospital universitárioda PUC-Campinas. Rev. Cir Craniomaxilofacial. 2010;13(2):12.
1 - Specialist in Plastic Surgery and Micro Surgery - Plastic Surgeon at North Wing Regional Hospital of Brasilia
2 - Member of the Society of Plastic Surgery - Plastic Surgeon at the North Wing Regional Hospital of Brasilia (NWRH), Brasilia, DF, MSc and PhD from the University of Brasilia - Plastic Surgeon at the North Wing Regional Hospital of Brasilia (NWRH), Brasilia, DF
3 - Specialist in Plastic Surgery - Plastic Surgeon at the Regional Hospital of Brasilia (NWRH), Brasilia, DF
4- Specialist in Plastic Surgery - Plastic Surgeon at the Regional Hospital of Brasilia (NWRH), Brasilia, DF
5- Specialty Trainee in Plastic Surgery - Resident in Plastic Surgery at the North Wing Regional Hospital -DF
6- Specialty Trainee in Plastic Surgery - Resident in Plastic Surgery at the North Wing Regional Hospital -DF
7- Specialty Trainee in Plastic Surgery - Resident in Plastic Surgery at the North Wing Regional Hospital -DF
8- Specialty Trainee in Plastic Surgery - Resident in Plastic Surgery at the North Wing Regional Hospital -DF
Institution: North Wing Regional Hospital of the Federal District.
Corresponding author:
Altino Vieira de Rezende Filho Neto
Street 3, Setor Oeste, número 906, apto 101, Ed. Johen Carneiro
Goiânia - GO
E-mail: altinofn@hotmail.com
Article received: July 23, 2013
Article accepted: March 4, 2014


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter