

Original Article - Year 2014 - Volume 29 -
Temporary hemostatic traction (THT) in rhytidoplasty
Tração hemostática temporária (THT) em ritidoplastias
ABSTRACT
INTRODUCTION: To slow the aging process, facial contouring surgery was developed as a rejuvenating technique, and is constantly improving, as are the results. However, as with any surgical procedure, complications are possible, the main one being hematoma. Dissatisfied with the prospect of hematoma and the use of drains, and with a goal of lower costs, the authors felt the need to develop a new surgical procedure, temporary hemostatic traction (THT).
METHODS: Sixty-four rhytidoplasties, all performed at the Valle Pereira Clinic (Florianópolis, SC, Brazil) from May 2012 to January 2013, were included in this study. All patients underwent the new THT procedure.
RESULTS: Only two patients developed epidermolysis with optimal evolution following THT, and one developed generalized facial edema. There were no instances of hematoma at any of the postoperative stages.
CONCLUSIONS: This new surgical technique avoids the use of drains and decreases dead space, thereby improving flap adhesion, and decreases hematoma, seroma, and postoperative edema; it also decreases tension on the incision, hence improving the results of rhytidoplasty.
Keywords: Rhytidoplasty; Facial Surgery; Hematoma.
RESUMO
INTRODUÇÃO: Na tentativa de desacelerar o processo de envelhecimento, as cirurgias de contorno facial foram estabelecendo-se como técnicas rejuvenescedoras, sendo constantemente aprimoradas, assim como os resultados. Porém, como qualquer procedimento cirúrgico, há a possibilidade de intercorrências e a principal complicação delas é o hematoma. Descontentes com a presença desta complicação, com o uso de drenos e visando menor custo, os autores viram a necessidade de desenvolver uma nova tática cirúrgica chamada tração hemostática temporária - THT.
MÉTODOS: Foram incluídas neste estudo todas as ritidoplastias realizadas na Clínica Valle Pereira (Florianópolis, SC), no período compreendido entre maio de 2012 e janeiro de 2013, totalizando 64 pacientes. Todos foram submetidos à nova tática cirúrgica chamada tração hemostatica temporária.
RESULTADOS: Apenas 2 pacientes apresentaram epidermólise com ótima evolução sob a THT, e 1 caso de edema facial generalizado. Não houve caso com hematoma, em qualquer período pós-operatório.
CONCLUSÕES: esta nova tática cirúrgica evita o uso de drenos, diminui o espaço morto aumentando a adesão do retalho descolado e, consequentemente, diminui a presença de hematoma, seroma e edema pós-operatório, assim como diminui a tensão cicatricial na incisão da pele, visando aprimorar os resultados das ritidoplastias.
Palavras-chave: Ritidoplastia; Face/Cirurgia; Hematoma.
Chronological aging can be fully appreciated in the face, a body part particularly susceptible to environmental aggression and also prone to displaying genetics-driven signs of tissue decline1.
Attempts to delay aging led to the 20th century development of surgical techniques of facial contouring as an approach to rejuvenation; these techniques are constantly being perfected, with improvement in the results.
As with any other surgical technique, complications must be considered. The main complication in the rhytidoplasty postoperative period is hematoma2-4, which can affect up to 8% of patients4-8. Hematomas can compromise postoperative recovery and limit the final esthetic result. Large hematomas usually occur within the first 48h1, and require immediate treatment to avoid the development of prolonged facial edema, epidermolysis, and skin necrosis3.
Different means of preventing the development of hematomas have been suggested7-12, and one most often chosen is the use of drains9. Their use is not without risks and complications2.
Baroudi and Ferreira12, Pontes13, and Auersvald14 have introduced other important concepts. To reduce dead space and drifting of large detachments, Baroudi has described internal adhesion points. Pontes characterized quilted sutures, singly or in the shape of a necklace, for large detachments in the submental area. Auersvald described a hemostatic net of continuous points crossing all skin layers, and attaining near complete occlusion of the entire operated region.
OBJECTIVE
This work describes a different surgical approach, with the goal of decreasing dead space and increasing adhesion of the detached flap, hence reducing postoperative hematoma, seroma and edema; in addition, the use of drains is avoided and tension at the incision site is decreased, with improved rhytidoplasty results.
METHOD
From May 2012 to January 2013, 64 patients underwent rhytidoplasty at the Valle Pereira Clinic.
All patients were female, requiring a wide intervention at the middle and lower thirds of the face, with or without blepharoplasty, or even a superciliary brow lift.
All patients underwent temporary hemostatic traction (THT).
Patients were evaluated upon discharge, 48h postoperatively, and weekly thereafter; concerns were the development of hematoma, seroma, and edema; the correct definition of the jaw angle; adhesion of the detached flap; status of scar infection; and necrosis. Photographs were taken, according to routine procedures, 48h postoperatively, and 1 week and 1 month later.
A routine informed consent form, standard at the clinical service, was signed by all patients undergoing surgery.
Surgical procedure
The proposed combined anesthesia, both local and assisted, was administered according to routine procedures at the Valle Pereira Clinic. The anesthetist was constantly present in the operating room, and intermittent pneumatic compression was compulsory, with thromboembolism prophylaxis, whenever required, using low molecular weight heparin.
Local anesthesia was performed with 40ml of 1% lidocaine, 310ml of 0.9% physiologic saline, and 1 vial of epinephrine (1:350 000), with an approximate volume of 150ml on each side of the face.
Rhytidoplasty was performed according to protocols previously established by the surgeons in the team, with temporal incisions either in the scalp or on the forehead (depending on the patient), pretragal incisions, and posterior short prehairline incisions. Wide flap detachment was performed with a Metzenbaum scissors in a single subcutaneous plane. Hemostasis was rigorously maintained. Superficial muscular aponeurotic system (SMAS) plication, following the direction of tragus to Darwin's tubercle, and lateral plication of the platysma muscle, were performed with Monocryl 4.0 suture. The procedure continued with THT, resection, and synthesis.
THT
1. Traction and repositioning of the flap is done in the direction of tragus to Darwin's tubercle, in the temporal and pre-auricular regions, with tendency to vertical positioning in the retroauricular region.
2. Maintaining the same traction, the THT line is marked with methylene blue. This line begins in the retroauricular region and follows an arch towards the pretemporal region, running equidistant to the line of probable flap resection and the line that limits the end of the detaching area. (Figure 1)

Figure 1. THT line.
a) Starting with the crossing of the skin layers, the needle is introduced in the direction of skin to subcutaneous cellular tissue, and follows by holding the deep layer. The needle then returns to the skin, ultimately leaving the skin. (Figure 2)

Figure 2. Beginning of the THT procedure.
b) The process is repeated under the marked THT line, with the needle progressing every 2cm. (Figure 3)

Figure 3. End of the THT procedure.
c) It is important to stress that suturing is performed under direct visualization of the needle pathway.
d) The THT line marked in the skin follows an arch with a wider radius than the arch of the deep plane.
e) The ends of the suture are pulled to finish stitching.
f) The suture traction establishes the flap movement, which corresponds to the difference between the radii of the arches (subcutaneous and deep), and dictates the amount of skin to be resected.
3. After marking the line, THT is performed with a continuous suture of mononylon 2-0 crossing the skin layers.
4. The ends of the suture are pulled to allow movement of the detached flap. (Figure 4)
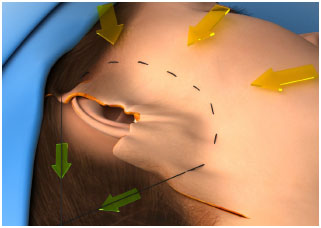
Figure 4. Direction of traction after the end of the THT.
5. Maintaining the correct traction, two-point quilted sutures are created under silicone protection in the retroauricular and temporal regions.
6. The traction is renewed and the skin to be resected is marked.
7. The appropriate skin is resected and tissue synthesis is performed with intradermal stiches using Monocryl 4.0 suture. For wound healing, gauze pads are used and a helmet-like head bandage is applied. Cold pads are applied to the eyelids (when these also undergo intervention) intermittently for the following 24 h.
RESULTS
All 64 patients selected were included in the study. Two of the patients required temporal pre-hairline incisions, and the other 62 underwent intra-hairline incisions.
Blepharoplasties were performed in 61 patients; another five patients required superciliary brow lifts, performed according to McCord2 and Castanhares3.
All patients had uneventful recoveries post-surgery. Only one patient remained in the clinic overnight, with discharge on the morning after surgery.
Postoperative evaluations at 48 h did not reveal hematoma, seroma, infection, or necrosis. Edema was observed in only one patient: it was moderate but extended to the entire face and neck. The remaining 63 patients had only mild edema.
All patients showed excellent adhesion of the entire detached flap and cicatrization of the incisions. In 63 of the 64 cases, there was rapid definition of the jaw angle.
All padding was removed within 48 h postoperatively; two patients presented with mild epidermolysis in these regions.
Concomitantly, the mononylon 2.0 sutures were removed from the THT region by cutting the external ends of the suture first, followed by removing the stitches one by one, thus avoiding excessive traction when pulling. One of the patients had epidermolysis of the skin below the suture.
On postoperative day seven, all patients had good recovery, with no signs of hematoma, seroma, infection, or necrosis. There was excellent adhesion of the detached flap, good appearance of the scars at the incision sites, and defined jaw angles. Epidermolysis was observed under quilted sutures (1 and 2) in two of the patients, and following THT in another patient; all had positive evolution.
All patients had optimal evolution in subsequent evaluations. Postoperative results before and after removal of the THT can be observed in Figures 5, 6, and 7.

Figure 5. Result before removal of the THT (48 h).

Figure 6. Result after removal of the THT (48 h).

Figure 7. Pre- and postoperatively.
DISCUSSION
Hematoma and its implications for rhytidoplasty remain major concerns for plastic surgeons. Therefore, we continually search for new surgical techniques that can prevent the development of hematomas.
Many authors have promoted the routine use of drains in the past. Both sheet and vacuum drains are currently employed for the prevention of hematomas, but their use is not without risks and complications2. In addition, drains have associated costs and require extra care by patients.
Pontes has described the use of quilted sutures in the submental region, singly or in the shape of a necklace. These are highly relevant to the maintenance of adjusted skin, which undergoes considerable movement in the submental region. The quilted sutures increase the adhesion of the detached flap and decrease the dead space. These sutures are then protected to avoid skin trauma and maintained for 5 to 7 days13.
Recently, Auersvald described a hemostatic net of continuous sutures crossing layers of skin to achieve near total occlusion of the operated site; this is very effective in preventing hematomas. It is a technology with low cost, despite being time consuming and laborious.
There are effective alternatives, but these are not currently in use due to high associated cost, limited availability, or poor acceptance by the patient; these alternatives include fibrin glues, platelet-rich plasma, and compression masks8,10,11.
Baroudi described the effective use of internal adhesion sutures, which decrease dead space and, consequently, minimize associated complications12.These sutures, first described for the prevention of seromas, have broadened the spectrum of available technical approaches. However, use in rhytidoplasty is limited by the size of the flap. Recently, fibrin glues and platelet-rich plasma have been used successfully, but with high cost.
THT, with retention and quilted sutures (1 and 2), should be performed under direct visualization.
The main objectives were to decrease dead space and traction over the SMAS platysma muscle; tension at the skin incision is thus alleviated without the need for external suturing of the skin.
We have randomly set the time for complete removal of THT at 48h postoperatively. We consider this interval to be the minimum required for scar formation because it precedes epithelialization of the suture pathway. Hence, there is a low chance of developing undesirable skin dyschromia, and bleeding is only a very remote possibility due to the advanced coagulation process.
This new technique was effective in decreasing dead space and scar tension, with less hematoma (0%) and seroma (0%) formation, and excellent scar appearance, when compared with the data reported in the literature1-7,9,11.
Other equally important benefits were increased adhesion of the detached flap, less postoperative edema, and rapid definition of the jaw angle.
This strategy was executed rapidly (five min per side), and efficiently, is easy to reproduce, and has low associated cost (one vial of physiologic saline and two mononylon 2.0 sutures). With this technique, we believe that the use of drains can be abandoned in the described procedure.
CONCLUSION
THT is a new surgical technique that avoids the use of drains, decreases dead space, and increases the adhesion of the detached flap. Therefore, this limits postoperative hematoma, seroma, and edema development, and diminishes tension at the skin incision site, contributing to improvement of the rhytidoplasty results.
REFERENCES
1. Carreirão S, Cardim V, Goldenberg D, editores. Cirurgia plástica. Sociedade Brasileira de Cirurgia Plástica. São Paulo: Atheneu; 2005. p.621-45.
2. Baker TJ. Complications of rhytidectomy. Plast Reconstr Surg. 1967;40:31-9.
3. Rees TD, Lee YC, Coburn RJ. Expanding hematoma after rhytidectomy: a retrospective study. Plast Reconstr Surg. 1973;51:149-53.
4. Jones, BM. Facelifting: an initial eight year experience. Br J Plast Surg. 1995;48:203-11.
5. Leist FD, Masson JK, Erich JB. A review of 324 rhytidectomies, emphasizing complications and patient dissatisfaction. Plast Reconstr Surg. 1977;59:525-9.
6. Jones BM, Grover R. Reducing complications in cervicofacial rhytidectomy by tumescent infiltration: a comparative trial evaluating 678 consecutive face lifts. Plast Reconstr Surg. 2004;113(1):398-403.
7. Rees TD, Barone CM, Valauri FA, Ginsberg GD, Nolan WB III. Hematomas requiring surgical evacuation following face lift surgery. Plast Reconstr Surg. 1994;93:1185-90.
8. Marchac D, Sandor G. Face lifts and sprayed fibrin glue: an outcome analysis of 200 patients. Br J Plast Surg. 1994;47:306-9.
9. Jones BM, Grover R, Hamilton S. The efficacy of surgical drainage in cervicofacial rhytidectomy: a prospective, randomized, controlled trial. Plast Reconstr Surg. 2007;120(1):263-70.
10. Kamer FM, Nguyen DB. Experience with fibrin glue in rhytidectomy. Plast Reconstr Surg. 2007;120(4):1045-51.
11. Por YC, Shi L, Samuel M, Song C, Yeow VK. Use of tissue sealants in face-lifts: a metaanalysis. Aesthetic Plast Surg. 2009;33(3):336-9.
12. Baroudi R, Ferreira CA. Seroma: how to avoid it and how to treat it. Aesthet Surg J. 1998;18(6):439-41.
13. Pontes R. O universo da ritidoplastia. Rio de Janeiro: Revinter; 2011. p.358.
14. Auersvald. Rede hemostática: uma alternativa para a prevenção de hematoma em ritidoplastia. Rev. Bras. Cir. Plást. 2012;27(1):22-30.
1 - Full member of the Brazilian Society of Plastic Surgery - Member of the Professor Ivo Pitanguy Alumni Association. Member of the Clinical Medical Staff of the Valle Pereira Clinic
2 - Full member of the Brazilian Society of Plastic Surgery - Member of the Professor Ivo Pitanguy Alumni Association. Member of the Clinical Medical Staff of the Valle Pereira Clinic
3 - Specialist Member of the Brazilian Society of Plastic Surgery. Member of the Clinical Medical Staff of the Valle Pereira Clinic
Institution: Valle Pereira Clinic.
Corresponding author:
João Francisco do Valle Pereira
Avenida Osvaldo Rodrigues Cabral, 1570 - Ático, Beiramar Norte
Florianópolis - SC - CEP: 88015-710
Telefone de contato: (48) 32252299
E-mail: xanico@vallepereira.com
Article submitted: February 5, 2013
Article accepted : March 10, 2013


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter