

Case Report - Year 2013 - Volume 28 -
Multiple symmetric lipomatosis: report of two cases
Lipomatose simétrica múltipla: relato de dois casos
ABSTRACT
Multiple symmetric lipomatosis is an unusual disease of unknown etiology. It is characterized by symmerical accumulation of fat tissue deposits in neck, face, trunk and proximal limbs. It is more common in male adult subjects with a history of alcohol intake. Paliative surgery is the main treatment and it can be performed by conventional open excision or liposuction. Recurrence is common. The objetive of this article is to report two cases of multiple symmetric lipomatosis treated by liposuction in Regional Hospital of Asa Norte, in Brasilia - Federal District.
Keywords: Multiple Symmetric Lipomatosis. Madelung Disease. Liposuction.
RESUMO
A lipomatose simétrica múltipla é uma doença incomum, de etiologia desconhecida, caracterizada pelo acúmulo simétrico de depósitos de tecido adiposo em face, pescoço, tronco e região proximal dos membros. É mais frequente em indivíduos adultos do sexo masculino, geralmente com história de etilismo. O tratamento é cirúrgico, com ressecção paliativa por via aberta ou por lipoaspiração. A recidiva é comum. O presente artigo tem por objetivo relatar dois casos de lipomatose simétrica múltipla, tratados por lipoaspiração no Hospital Regional da Asa Norte, em Brasília-DF.
Palavras-chave: Lipomatose Simétrica Múltipla. Doença de Madelung, Lipoas-piração.
Multiple symmetric lipomatosis, also known as benign symmetric lipomatosis, Madelung disease, or Launois-Bensaude syndrome, was first reported by Brodie in 1846. However, the first case series was described in 1888 by Madelung and in 1898 and by Launois and Bensaude1. Multiple symmetric lipomatosis is a rare disease that usually affects adult men with a history of chronic alcohol use1-6. It is characterized by symmetrical appearance of uncapsulated lipomatous masses in the face, neck, trunk, and proximal limbs, characteristically sparing the distal portions4. The disease is of great importance to plastic surgeons, as it directly affects body contour, with liposuction as the ideal treatment.
CASE REPORTS
Case 1
A 61-year-old, married, retired, and alcoholic man who consumed 350 mL of spirits per day since 17 years of age and was a former smoker complained of early fatty deposits, about 17 years prior, in the thorax, abdomen, and arms with progressive growth (Figure 1). His personal history revealed two operations, one for peptic ulcer 17 years ago and the other was cholecystectomy 2 years ago. He underwent liposuction in two sessions. In the first session, the posterior regions of the trunk were lipoaspirated. In the second session, 9 months later, the anterior trunk and arms were lipoaspirated. The first operation was uneventful, but the second procedure was complicated by seroma and secondary infection that developed into skin necrosis in the abdominal wall (Figure 2). Surgical drains were not used in either of the procedures. The complication was successfully treated with drainage of collections, systemic antibiotics, serial debridement, and delayed primary closure after control of the infection and necrosis .
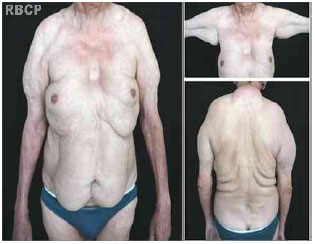
Figure 1 - Preoperative photograph .
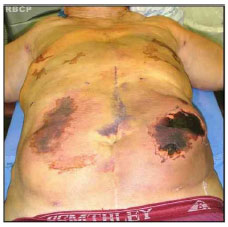
Figure 2 - Case 1: Skin necrosis in the abdominal wall after liposuction .
Case 2
A 35-year-old, married, alcoholic man who was a mason by profession consumed 500 mL of spirits per day and smoked 5 cigarettes per day for 20 years reported early fatty deposits 3 years ago, first in the chest and later in the abdomen and proximal portion of the lower limbs, also with a gradual increase in volume (Figure 3). He underwent liposuction in a single surgical procedure, without complications. Surgical drainage tubes were left in place, under suction, in the lipoaspirated areas.
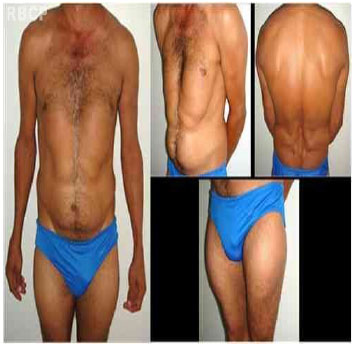
Figure 3 - Preoperative photograph .
DISCUSSION
Multiple symmetric lipomatosis is a rare disease that usually affects the male sex (approximate male-to-female ratio, 15:1) between the third and sixth decades of life, and is associated with chronic alcohol use in up to 90% of cases1,3. Both of the patients presented in this report present an epidemiological profile in agreement with the literature, including long-term heavy alcohol use.
The etiology of multiple symmetric lipomatosis is unknown1-6. However, deficiency in embryonic brown adipose tissue, mitochondrial dysfunction, and defects in the catecholamine-induced lipolytic pathway have been suggested, with alcoholism apparently acting as a cofactor5.
The main clinical manifestation of the disease is the appearance of uncapsulated lipomatous deposits with symmetrical distribution in the face, neck, trunk, and proximal limbs, characteristically sparing the distal portions4. Typical locations include the cervical region ("horse collar"); posterior neck ("buffalo hump"); parotids: submentovertex and retroauricular ("hamster cheek"); and on the chest, deltoids, and supraclavicular and proximal upper limbs ("pseudoathletic form")2. Lipomas in most cases are asymptomatic but may cause difficulty in head movement and affect mediastinal structures such as vessels, nerves, the trachea, bronchi, the pharynx, and the esophagus. Furthermore, they may cause symptoms such as dyspnea, dysphagia, dysphonia, and obstructive sleep apnea1,2,4-6.
Association with metabolic disorders (hyperuricemia, diabetes mellitus, and dyslipidemia), hypertension, liver disease, hypothyroidism, and renal tubular acidosis has also been reported1,2,4-6.
A peculiar aspect of multiple symmetric lipomatosis is a particular form of peripheral neuropathy, which can be motor, sensory, or autonomic, unrelated to alcohol intake1,2,4-6. This form of neuropathy affects up to 90% of patients over the course of the disease and may manifest as paresthesias, cramps, resting tachycardia, postural hypotension, segmental hyperhidrosis, erectile dysfunction, and acrocyanosis, among others4.
The clinical course is traditionally reported as benign. The medical literature reports only one case of malignant degeneration to sarcoma1,4-6. However, multiple symmetric lipomatosis presents specific and significant morbidity and mortality, regardless of the benign nature of the deposits4. In a long-term longitudinal study, 31 patients with a mean follow-up period of 14.5 years had significantly higher mortality than the general population. Cases of sudden death attributed presumably to a cardiovascular manifestation of autonomic neuropathy were responsible for the inflation of the mortality rate. Moreover, a considerable morbidity was observed during the course of the disease due to the high frequency of mediastinal extension and peripheral neuropathy during long-term follow-up4.
In contrast to the literature, we did not observe any of the associated symptoms, the presence of metabolic disorders, or signs of peripheral neuropathy in any of the study patients.
Diagnosis is mainly clinical1,2,4 and based on the presence of multiple fatty deposits in a symmetrical distribution, which spare the distal portion of the limbs4, as observed in both patients. Computed tomography and magnetic nuclear resonance imaging, however, can be useful in determining the extent of lipomas and their relationship with the surrounding structures, especially the mediastinum1,2.
Palliative surgical excision, via the open method or liposuction, is the current treatment of choice1-6. Lipomas are not encapsulated, have an infiltrative nature, have a fibrous component, and are extensively vascularized, usually preventing their complete removal2. Moreover, the basic disorder, which is responsible for fatty deposits, persists, leading to frequent recurrences2. Liposuction presents some advantages in that it is less invasive, prevents extensive scars, requires a shorter recovery period, and can be performed multiple times2,5. However, it may present technical difficulties such as resistance to penetration of the cannula (due to the fibrous component of the lesions) and with profuse bleeding (due to the hypervascular nature of the disease)2. One can choose, as was decided in case 1, to perform more than one session to minimize blood loss3. Removal of redundant skin may be required after completion of the liposuction3. Conventional surgical excision of lipomas provides a greater possibility of complete resection, despite being hampered by the infiltrative nature of lipomas. A cleavage plane with normal tissues is not easily observed5. Hematomas and seromas are common surgical complications1,2,5. Rigorous hemostasis and use of drains are recommended1,2,5.
In the two cases under discussion, we opted for liposuction to improve body contour, and both patients were greatly satisfied with the outcomes. The absence of drains and enhanced liposuction might have contributed to the complications observed in patient 1. After liposuction, the same patient presented with large cutaneous excess in the abdomen, back, and upper limbs but did not desire additional procedures to improve the results. None of the patients had evidence of recurrence until the sixth month of postoperative follow-up (Figures 4 and 5).
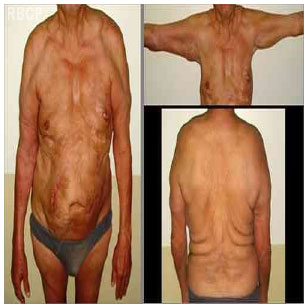
Figure 4 - Case 1: Photograph at 6 postoperative months
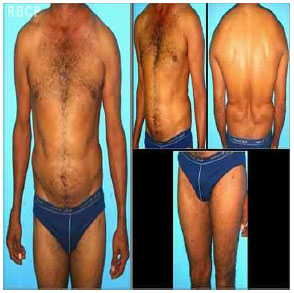
Figure 5 - Case 2: Photograph at 6 postoperative months .
REFERENCES
1. Meningaud JP, Pitak-Arnnop P, Bertrand JC. Multiple symmetric lipomatosis: case report and review of the literature. J Oral Maxillofac Surg. 2007;65(7):1365-9.
2. Sonni VF, Pires CEB, Kay MS, Neiva IF, Bier GE. Síndrome de Madelung - Relato de Caso. Rev Soc Bras Cir Plást. 1999;14(2):65-74.
3. Meyer TN, Meyer GPN. Caso atípico de lipomatose simétrica múltipla. Rev Soc Bras Cir Plást. 2007;22(1):64-6.
4. Enzi G, Busetto L, Ceschin E, Coin A, Digito M, Pigozzo S. Multiple symmetric lipomatosis: clinical aspects and outcome in a long-term longitudinal study. Int J Obes Relat Metab Disord. 2002;26(2):253-61.
5. Ramos S, Pinheiro S, Diogo C, Cabral L, Cruzeiro C. Madelung disease: a not-so-rare disorder. Ann Plast Surg. 2010;64(1):122-4.
6. Brackenbury ET, Morgan WE. Surgical management of Launois-Bensaude syndrome. Thorax. 1997;52(9):834-5.
1. Plastic surgeon of the Asa Norte Regional Hospital and specialist member of the Brazilian Society of Plastic Surgery
2. Head of Medical Residency in Plastic Surgery of the Asa Norte Regional Hospital and full member of the Brazilian Society of Plastic Surgery
3. Resident in plastic surgery of the Asa Norte Regional Hospital and aspiring member of the Brazilian Society of Plastic Surgery
José Luiz de Oliveira Neto
Article recceived:10/01/2011
Article accepted:15/02/2011
Work performed at the Asa Norte Regional Hospital , Brazil.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter