

Case Report - Year 2013 - Volume 28 -
Closure of myelomeningocele defects using a rotation flap that resulted in a trident scar
Retalho de rotação com cicatriz resultante em tridente para fechamento de meningomielocele
ABSTRACT
Myelomeningocele is a defect of the spinal cord, spinal column, and skin covering these areas that results in the defective closure of the posterior portion of the neural tube during the fourth week of gestation. Its etiology is multifactorial and has yet to be clarified. The objective of this study was to demonstrate an additional skin flap alternative for the treatment of this defect. Closure with a flap that creates a trident-shaped scar has been shown to be a viable alternative that is easy to implement, reduces surgical time, minimizes blood loss, and requires no cutaneous grafts to cover the flap donor area.
Keywords: Meningomyelocele. Neural tube defects. Surgical flaps.
RESUMO
A meningomielocele é um defeito da medula espinhal, da coluna vertebral e da pele sobre essa área, resultando em defeito no fechamento da porção posterior do tubo neural durante a quarta semana de gestação. Sua etiologia é multifatorial e ainda não está esclarecida. O objetivo deste trabalho é demonstrar mais uma opção de retalho de pele para tratamento desse defeito. O fechamento com retalho resultando em cicatriz em formato de tridente apresentou-se como alternativa viável, de fácil execução, com tempo cirúrgico reduzido e mínima perda sanguínea, não requerendo enxertos cutâneos para cobertura da área doadora dos retalhos.
Palavras-chave: Meningomielocele. Defeitos do tubo neural. Retalhos cirúrgicos.
Congenital fusion defects of the neural tube and associated tissues are classified as spinal dysraphism. Myelomeningocele, a defect of the spinal cord, spinal column, and skin covering these areas that results in a defective closure of the posterior portion of the neural tube during the fourth week of gestation1-12, is the most common congenital spinal defect.
Its etiology is multifactorial and currently unclear, with factors such as genetics, geographical, low socioeconomic status, and folic acid deficiency being implied in its development. The incidence of myelomeningocele is approximately one in every 800-1,000 live births and has been decreasing because of prenatal screening for neural tube defects as well as pregnancy termination in countries that permit. This screening is conducted by prenatal ultrasound with 80-90% sensitivity depending on the degree of experience of the professional conducting the examination and the equipment used for fetal evaluation. Using this test, the level and extent of the opening in the spinal column can be identified.
Hereditary factors have been observed since there is a higher incidence in families with a history of the disease. In three-fourth of cases, the lumbosacral region is affected and is associated with motor and sensory deficits of the lower limbs, rectum, and bladder.
Early closure of the defect is mandatory to reduce acute infections of the skin related to the central nervous system. In untreated patients, the death rate is 65-75% within the first 6 weeks of life. Several surgical alternatives for large myelomeningocele defects are available, such as skin grafts, local fatty skin flaps, and musculocutaneous flaps. Postoperative complications such as suture dehiscence, partial flap necrosis, fistulas, infections, scoliosis, ventriculitis, and meningitis may occur.
Several surgical flaps can be used for closure of myelomeningocele defects. The objective of the study was to demonstrate an additional skin flap alternative for the treatment of this defect.
CASE REPORT
Our 4-hour-old female infant with a congenital myelomeningocele and motor and sensory impairments in the lower limbs was born via an uneventful cesarean delivery (birth weight, 2,495 g; Apgar score, 9/9). The child's mother had a history of two previous miscarriages of unknown cause and an infection of the genitourinary tract during pregnancy that was treated with nitrofurantoin.
The newborn underwent surgery performed by the neurosurgical team to close the medullary canal. An evaluation by the plastic surgery team was requested for closing the open sacrococcygeal area (Figure 1).
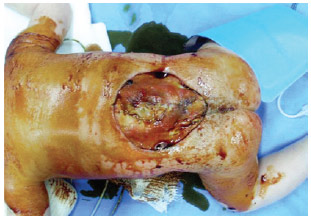
Figure 1 - Preoperative aspect.
On the 3rd day of life, a double fatty-skin flap was prepared in the lumbosacral region by bilateral rotation. On the 12th postoperative day, the interspersed stitches were removed; on the 24th day, the rest of the stitches were removed.
The patient was followed up by the plastic surgery team until the 30th postoperative day, when she was discharged.
Surgical Technique
The patient underwent surgery under general anesthesia in the prone position. The dermal adipose/cutaneous flaps on the skin were marked and sectioned in the mirror format using a standard semicircular mark, randomized irrigation pattern, and rotation and advancement with the resulting scar in the shape of a trident with full lesion coverage (Figures 2 and 3). No drain was needed.
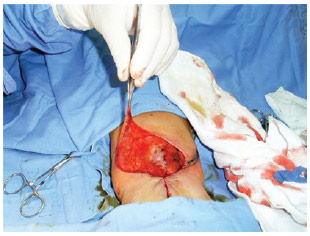
Figure 2 - Flap sectioning.
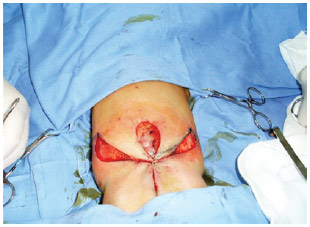
Figure 3 - Flap positioning.
The flap presented good perfusion immediately after the surgery as well as later after immediate re-perfusion after compression, with no change in color (cyanosis or pallor) (Figures 4-6). There was 99% viability, occurring late distal flap vascular compromise on the left side but healing adequately.
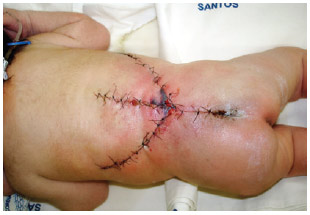
Figure 4 - Appearance on the 2nd postoperative day.
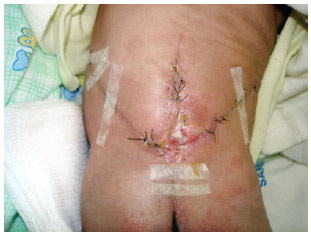
Figure 5 - Appearance on the 17th postoperative day.
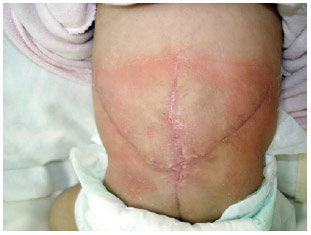
Figure 6 - Appearance on the 30th postoperative day.
DISCUSSION
Myelomeningocele is a congenital defect of unknown etiology that results from non-closure of the posterior portion of the neural tube. The abnormal development of vertebrae at the level of the lamina and spinal apophysis may involve one or more arcs, resulting in hernias containing cerebrospinal fluid (CSF) and spinal cord meninges with possible adhesions in the spinal cord or nerve roots. Various neurological complications may occur in individuals with this defect, such as hydrocephalus, urinary incontinence, voiding bladder dysfunction, changes in bowel habits, sexual impotence, sensory and motor loss in lower limbs, and deformities in the legs.
Early surgical intervention is performed to reduce the increasing number of infections of the central nervous system and to prevent progression of the neurological deficit by protecting the neural tissue. Approximately 25% of the defects cannot be successfully treated with primary closure alone and require more complex procedures for correction. Most cases require primary closure with or without subcutaneous detachments.
The reconstruction procedures can be divided into three groups: skin flaps, skin grafts, and muscle or musculocutaneous flaps. There are reports of various types of flaps that can reduce tension along the suture line: latissimus dorsi, gluteus maximus, V-Y, Limberg, island pedicle, rotation, bipedicled, double, rhomboid, and Z flaps. The grafts are simple and have a low complication rate but may require intervention later due to deformities such as elevation, ulceration, and infection.
Skin grafts are an easy alternative for correcting myelomeningoceles; however, since they do not offer thick coverage, their long-term durability is questionable and their use can cause complications in the donor area.
Musculocutaneous flaps are described as a safe alternative that provide good neural coverage. However, compromising the dorsal muscles can cause a range of problems from decreased bladder emptying efficiency to decreased Valsalva functioning and reduced alternatives for the treatment of pressure ulcers in patients who may require a wheelchair.
Several alternatives to local fatty-skin flaps with varying shapes and transfer modes have been successfully used to close myelomeningocele defects. Transposition, rotation, advanced bilateral v-y, bilobular, and Limberg flaps are alternatives, as they are associated with less blood loss and reduced surgical time, which are important factors when considering patients' conditions; however, some of these may require skin grafts to cover the donor sites1,3,4,7,8.
After myelomeningocele closure, complications such as dehiscence, fistula, and infection may occur. When these patients undergo surgery immediately after birth, the complication rate is much lower (13%) than that after the first 48 hours of life (29%). Dehiscence, one of the most frequent complications, can be prevented using laser therapy, which presents the same good results12.
In our case, we presented a fatty-skin flap alternative for correcting moderate-to-large defects that ensured coverage of neural tissues. There was no postoperative CSF leakage. Necrosis occurred as a complication in a small distal portion of a flap, was treated with simple dressings, and did not need further intervention.
Closure using a trident-shaped flap was found to be a viable alternative that is easy to implement, reduces surgical time, and minimizes blood loss and does not require the use of cutaneous grafts to cover the donor flap area. The existing complication of necrosis at the distal flap portion was easily treated with dressings without the need for further surgical intervention.
REFERENCES
1. Ulusoy MG, Koçer U, Sungur N, Karaaslan O, Kankaya Y, Ozdemir R, et al. Closure of meningomyelocele defects with bilateral modified V-Y advancement flaps. Ann Plast Surg. 2005;54(6):640-4.
2. Muneuchi G, Matsumoto Y, Tamai M, Kogure T, Igawa HH, Nagao S. Rhomboid perforator flap for a large skin defect due to lumbosacral meningocele: a simple and reliable modification. Ann Plast Surg. 2005;54(6):670-2.
3. Atik B, Tan O, Kiymaz N, Yilmaz N, Tekes L. Bilobed fasciocutaneous flap closure of large meningomyeloceles. Ann Plast Surg. 2006;56(5):562-4.
4. Komuro Y, Yanai A, Koga Y, Seno H, Inoue M. Bilateral modified V-Y advancement flaps for closing meningomyelocele defects. Ann Plast Surg. 2006;57(2):195-8.
5. Mutaf M, Bekerecioğlu M, Erkutlu I, Bulut O. A new technique for closure of large meningomyelocele defects. Ann Plast Surg. 2007;59(5):538-43.
6. Gümüş N. A new approach to closure of myelomeningocele defect: z advancement-rotation flap. Ann Plast Surg. 2008;61(6):640-5.
7. Figueiredo JCA, Bonatto Junior A, Nunes R, Reiff ABM, Mélega JM. Retalho intercostal posterior: considerações anatômicas. Rev Soc Bras Cir Plást. 1997;12(3):55-68.
8. Pavanello DP, Cristaldo K, Larsen G, Bervian F, Alvarez G, Oliveira MP, et al. Retalho de Limberg para fechamento de meningomielocele. Arq Catarin Med. 2009;38(Supl 1):163-5.
9. Pinto RDA, Collares MVM, Oliveira ACP, Portinho CP, Viaro MS, Kaiser JM, et al. Tratamento cirúrgico de meningomielocele no período neonatal. Arq Catarin Med. 2007;36(Supl 1):151-3.
10. Sbragia L, Machado IN, Rojas CEB, Zambelli H, Miranda ML, Bianchi MO, et al. Evolução de 58 fetos com meningomielocele e o potencial de reparo intra-útero. Arq Neuro-Psiquiatr. 2004;62(2b):487-91.
11. Hisaba WJ, Moron AF, Cavalheiro S, Santana RM, Passos JP, Cordioli E. Espinha bífida aberta: achados ultra-sonográficos e presença de contrações uterinas na predição da evolução motora neonatal. Rev Bras Ginecol Obstet. 2003;25(6):425-30.
12. Pinto NC, Pinto FCG, Alho EJL, Yoshimura EM, Krebs VLJ, Teixeira MJ, et al. Estudo piloto em neonatos utilizando o laser de baixa intensidade no pós-operatório imediato de mielomeningocele. Einstein. 2010;8(1):5-9.
1. Resident of plastic surgery at the Plastic Surgery Department of the Santa Casa de Misericórdia de Santos, Santos, SP, Brazil
2. Plastic surgeon, specialist member of the Brazilian Society of Plastic Surgery (BSPS), member of the Plastic Surgery Department of Santa Casa de Misericórdia de Santos, Santos, SP, Brazil
3. Student of the School of Medicine of the Universidade Metropolitana de Santos, Santos, SP, Brazil
4. Plastic surgeon, full member of the BSPS, head of the Plastic Surgery Department of Santa Casa de Misericórdia de Santos, Santos, SP, Brazil
Correspondence to:
Fabiana Catherino
Rua Armando Sales de Oliveira, 200 - ap. 24 - Jardim das Nações
Taubaté, SP, Brazil - CEP 12030-080
E-mail: fabianacatherino@hotmail.com
Submitted to SGP (Sistema de Gestão de Publicações/Manager Publications System) of RBCP (Revista Brasileira de Cirurgia Plástica/Brazilian Journal of Plastic Surgery).
Article received: 9/28/2010
Article accepted: 1/10/2011


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter