

Original Article - Year 2013 - Volume 28 -
Assessment of the quality of life ofpatients with diabetes mellitus and foot ulcers
Avaliação da qualidade de vida em pacientes com diabetes mellitus e pé ulcerado
ABSTRACT
BACKGROUND: Diabetic foot is considered as one of the most devastating chronic complications of diabetes mellitus due to the large number of cases that eventually require amputation. In the present study, we aimed to assess the quality of life of patients with diabetes and foot ulcers compared to that of patients with diabetes but without foot ulcers.
METHODS: An analytical, cross-sectional, controlled, and comparative study of patients who visited 2 wound clinics in São Paulo was performed. Fifty patients with diabetes mellitus but without foot ulcers were selected as the control group and 50 patients with diabetes and foot ulcers were selected as the study group. The Short Form-36 Health Survey (SF-36) questionnaire was used to assess the quality of life. Patients were included consecutively in the same order that they visited the clinic.
RESULTS: The mean SF-36 score was 69.38 ± 21.90 in the control group and 30.34 ± 14.45 in the study group (P < 0.001). Mean scores across all SF-36 domains were lower in the study group than in the control group (P < 0.001).
CONCLUSIONS: Patients with diabetes and foot ulcers experience changes in the quality of life in the physical, social, and psychoemotional domains.
Keywords: Quality of life. Diabetes mellitus. Ulcer. Foot ulcer.
RESUMO
INTRODUÇÃO: O pé diabético é uma das mais devastadoras complicações crônicas do diabetes mellitus, em função do grande número de casos que evoluem para amputação. O objetivo deste estudo é avaliar a qualidade de vida de pessoas diabéticas com pé ulcerado comparativamente às pessoas diabéticas sem úlceras.
MÉTODO: Realizado estudo analítico, transversal, controlado e comparativo, com pacientes atendidos em 2 centros de tratamento de feridas de São Paulo. Foram selecionadas 50 pessoas para compor o grupo controle, com diabetes mellitus sem pé ulcerado, e 50 para o grupo estudo, composto de pacientes diabéticos com pé ulcerado. O instrumento usado para avaliar a qualidade de vida foi o questionário Short Form-36 Health Survey (SF-36). A inclusão dos pacientes no estudo obedeceu à ordem de chegada.
RESULTADOS: Na avaliação dos pacientes do grupo controle, o escore médio do SF-36 foi 69,38 ± 21,90 e do grupo estudo, 30,34 ± 14,45 (P < 0,001). A média dos escores em todos os domínios do SF-36 do grupo estudo foi mais baixa em relação ao grupo controle (P < 0,001).
CONCLUSÕES: Os pacientes diabéticos com pé ulcerado apresentam alterações na qualidade de vida, repercutindo nos domínios físico, social e psicoemocional.
Palavras-chave: Qualidade de vida. Diabetes mellitus. Úlcera. Úlcera do pé.
Diabetes mellitus is a syndrome with a multifactorial etiology, and is characterized by the deficiency or diminished effectiveness of insulin1. According to the World Health Organization and the International Diabetes Federation, approximately 160 million individuals worldwide had diabetes mellitus in 2002. Projections estimate that 300 million individuals worldwide will have the disease by 20252.
Foot ulcers develop in approximately 15% of patients with diabetes mellitus. The treatment of these wounds involves a complex process, and deep and infected wounds can result in an increased risk of amputation3. In 1990, the risk of lower limb amputation in patients with diabetes was approximately 40 times higher than that in the general population. A study conducted in Brazil reported that 66.3% of amputations performed in general hospitals occurred in patients with diabetes and foot ulcers3.
Diabetic foot is considered as one of the most devastating chronic complications of diabetes mellitus due to the large number of cases that eventually require amputation4. The term "diabetic foot" is used to characterize injuries that occur on the feet of patients with diabetes mellitus as a result of multiple factors, such as motor-sensitive and chronic peripheral autonomic neuropathies, peripheral vascular disease, biomechanical alterations that lead to abnormal plantar pressure, and infection (which can aggravate the condition)5.
Diabetic foot has immense social and economic consequences, including expenses related to treatment as well as prolonged and recurrent hospitalizations and physical and social problems such as employment and productivity losses. This condition influences individuals' personal lives by affecting their self-image, self-esteem, and role within the family and society; in fact, if physical limitations are present, social isolation and depression may occur6,7.
Diabetes can have a negative impact on the psychosocial functioning and quality of life of the affected individuals, particularly in the physical, social, and psychoemotional domains2,3. The extent of such an impact depends on the manner in which patients and their families perceive the disease and cope with self-care and disease management as well as on family functioning as a whole. Social support from friends is an important resource for patients with diabetes, particularly in adolescents8,9.
Physical functioning impairments include short- and long-term complications such as symptoms, lifestyle changes caused by treatment demands, and medication-related side effects10. The psychoemotional presentation can include worry, frustration, and hopelessness related to the chronic nature of the disease and its complications as well as feelings of management-related overload, exhaustion, and discouragement. Patients may also have low self-esteem as well as feelings of inferiority, anxiety, and depression. Among the social aspects of the condition are its financial cost, patients' perception of the degree of social support they receive, and the quality and level of conflict of interpersonal and family relations11,12.
Evaluations of the quality of life within the framework of research aimed at healthcare providers and clinical practitioners are important in the decision-making and therapeutic benefit assessment processes13,14.
The study of quality-of-life dimensions provides valuable insight that can be used to improve the care of patients with diabetes mellitus and foot ulcers. Thus, in the present study, we aimed to assess the quality of life of patients with diabetes and foot ulcers compared to patients with diabetes but without ulcers.
METHODS
This multicenter, descriptive, analytical, controlled, comparative, and non-randomized clinical study was conducted in the outpatient wound clinics of Hospital Geral Vila Nova Cachoeirinha and Conjunto Hospitalar de Sorocaba. The study group comprised 50 male and female patients aged > 18 years with diabetes mellitus and foot ulcers. The control group comprised 50 male and female patients aged > 18 years with diabetes mellitus but without foot ulcers who exhibited skin integrity in the foot. Participants were treated at the institutions where the data were collected.
Data were collected between August 2008 and January 2009 after receiving approval from the Research Ethics Committee of the Universidade Federal de São Paulo (number 0557/08). Patients were included consecutively in the order in which they visited the center.
The Short Form-36 (SF-36) questionnaire was used to assess the quality of life15. The SF-36 is a multidimensional generic measure that consists of 36 questions covering 8 domains. These domains are as follows: physical functioning, physical role functioning, body pain, general health, vitality, social role functioning, and emotional role functioning.
Physical functioning is measured by 10 items in question 3, which assess how individuals perform tasks such as getting dressed, bathing, walking, and climbing stairs. Physical role functioning is measured by 4 items in question 4, which evaluate how the patient's physical health interferes with their work activities. Body pain is assessed by 2 items in questions 7 and 8, which assess the pain intensity that individuals experienced during the period under evaluation and the limitations that those symptoms imposed on daily life. General health is assessed by 5 items in questions 1 and 11, which evaluate how individuals perceive their health status and what they think it will be like in the future.
Emotional role functioning is assessed by 3 items in question 5, which evaluate how emotional health has interfered with work and other daily activities. Social role functioning is assessed by 2 items in questions 6 and 10, which assess how long the individuals' social activities have been limited due to their physical or emotional state. Vitality is assessed by 4 items in question 9, which evaluate the individuals' state of well-being, energy, and willingness to perform their daily tasks. Mental health is assessed by 5 items in question 9, which measure the extent to which the patients' lives have been affected by feelings of anxiety, depression, happiness, and well-being.
Each SF-36 dimension is evaluated independently and is scored from 0 (worst possible health state) to 100 (best possible health state). The questionnaire focuses on the individuals' perception of their health during the 4 weeks before data collection.
The Mann-Whitney test was applied for the statistical analysis of the sociodemographic variables, whereas Fisher's exact test was used to compare the groups with regard to each of the SF-36 questionnaire domains. The level of significance for all statistical tests was set at P < 0.05.
RESULTS
The sample comprised 50 patients in the control group, of which 26 were followed at the Conjunto Hospitalar de Sorocaba and 24 visited the Hospital Geral Vila Nova Cachoeirinha. In the study group, 30 patients were followed at the outpatient wound clinic of the Conjunto Hospitalar de Sorocaba and 20 patients visited the outpatient wound clinic of the Hospital Geral Vila Nova Cachoeirinha.
Twenty-two (44%) patients in the control group and 15 (30%) patients in the study group were aged between 60 and 69 years. Twenty-eight (56%) patients in the control group and 31 (62%) in the study group were women (Table 1).

Twenty-seven (54%) patients in the control group and 29 (58%) patients in the study group had type 2 diabetes. Thirty-one (62%) patients in the control group and 29 (58%) patients in the study group had hypertension, whereas 33 (66%) patients in the control group and 23 (46%) patients in the study group had heart disease (Table 2). The mean SF-36 score was 69.38 ± 21.90 in the control group and 30.34 ± 14.45 in the study group (P < 0.001) (Table 3).
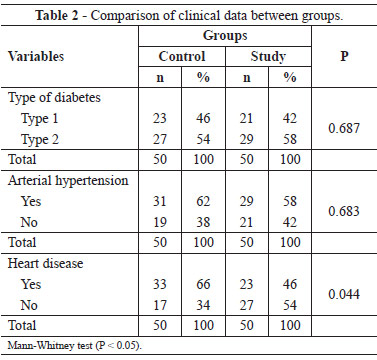
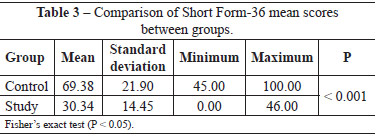
Table 4 shows the mean SF-36 score according to the domain: physical functioning, body pain, physical role functioning, general health, social role functioning, emotional role functioning, vitality, and mental health (P < 0.001).

DISCUSSION
Diabetes mellitus is among the major chronic diseases worldwide due to its high incidence and related complications16.
The foot is a highly specialized structure that is involved in the support and locomotion of the human body; in addition to being important from an aesthetic point of view, it is composed of many structures that work together harmoniously to perform different functions17.
Diabetic foot is a chronic complication of diabetes mellitus that is characterized by infection, ulceration, or destruction of deep tissues and is associated with neurological disorders and various degrees of peripheral vascular disease of the lower limbs. This condition has immense social and economic consequences resulting from amputations, including the inability to work, work absenteeism, and high financial costs associated with management and/or treatment of the disease and its acute and chronic complications18-20.
Patients experience great suffering due to these lesions, thus leading to lifestyle changes as well as decreased self-esteem, physical functioning, and quality of life, which often prevents patients from performing their usual activities21,22.
According to the 2000 census, elderly individuals accounted for 8.6% of the Brazilian population, which represents an increase of 1.02% as compared to the 1991 census findings23. In the present study, the majority of the participants in both groups were aged > 60 years. Thirty -one (62%) patients in the study group and 28 (56%) patients in the control group were women; these proportions are in accordance with those in the literature12,16,17,24.
A high incidence of hypertension and heart disease was observed in the population assessed in the present study. People with diabetes and heart disease have a worse prognosis, lower short-term survival, higher risk of disease recurrence, and worse response to treatment25,26.
In the present study, the quality of life was assessed using the SF-36 questionnaire. The mean SF-36 score was 69.38 ± 21.90 in the control group and 30.34 ± 14.45 in the study group; differences were observed across all domains (P < 0.001), showing that patients in the study group had a lower quality of life than patients in the control group.
Meneses et al.17 showed that patients with diabetes and foot ulcers had a lower quality of life across all domains, as measured by the SF-36, with physical functioning as well as physical, social, and emotional role functioning being the most affected. Shukla et al.27 assessed body pain in 50 patients with chronic wounds and found that it affected their quality of life.
As previously mentioned, foot ulcers cause suffering in patients, including changes in lifestyle, quality of life, and sleep patterns. The condition often prevents individuals from performing their normal social, leisure, and family activities. It can also lead to work absenteeism and loss of employment during a patient's prime age22,28,29. Because patients need help managing their work and leisure activities in social and family environments, their autonomy is limited and they become dependent upon family members and friends for support.
The present study highlights the need to refocus on the health of patients with diabetes and foot ulcers and for healthcare providers to identify the presence of quality of life changes.
Further studies are needed that include larger samples in order to describe the quality of life changes in patients with diabetes mellitus.
CONCLUSIONS
Patients with diabetes mellitus and foot ulcers experience changes in quality of life, particularly in the physical, social, and psychoemotional domains.
REFERENCES
1. Mancini MC, Medeiros MMA. Diabetes mellitus: como diagnosticar e tratar. Rev Bras Med. 2003;60:41-54.
2. Wilds S, Roglic G, Green A, Sicree R, King H. Global prevalence of diabetes: estimates for the year 2000 and projections for 2030. Diabetes Care. 2004;27(5):1047-53.
3. Reiber GE. The epidemiology of diabetes foot problems. Diabet Med. 1996;13(Suppl 1):S6-11.
4. Pecoraro RE, Reiber GE, Burgess EM. Pathways to diabetic limb amputation. Basis for prevention. Diabetes Care. 1990;13(5):513-21.
5. Gamba MA. Amputações por diabetes mellitus: uma prática prevenível? Acta Paul Enferm. 1998;11(3):92-100.
6. Rezende KF, Nunes MAP, Melo NH, Malerbi D, Chacra AR, Ferraz MB. Internações por pé diabético: comparação entre o custo direto estimado e o desembolso do SUS. Arq Bras Endocrinol Metab. 2008;52(3):523-30.
7. Coelho MS, Silva DMGV, Padilha MIS. Representações sociais do pé diabético para pessoas com diabetes mellitus tipo 2. Rev Esc Enferm USP. 2009;43(1):65-71.
8. Salomé GM, Pellegrino DMS, Blanes L, Ferreira LM. Self-esteem in patients with diabetes mellitus and foot ulcers. J Tissue Viability. 2011;20(3):100-6.
9. Guthrie DW, Bartsocas C, Jarosz-Chabot P, Konstantinova M. Psychosocial issues for children and adolescents with diabetes: overview and recommendations. Diabetes Spectr. 2003;16(1):7-12.
10. Marcelino DB, Carvalho MDB. Reflexões sobre o diabetes tipo 1 e sua relação com o emocional. Psicol Reflex Crit. 2005;18(1):72-7.
11. Polonsky WH. Aspectos emocionais e da qualidade de vida do tratamento do diabetes. Curr Diab Rep Lat Am. 2002;1:388-96.
12. Polonsky WH. Understanding and assessing diabetes-specific quality of life. Diabetes Spectr. 2000;13(1):36-41.
13. Roebuck A, Furze G, Thompson DR. Health-related quality of life myocardial infarction: an interview study. J Adv Nurs. 2001;34(6):787-94.
14. Buss PM. Promoção da saúde e qualidade de vida. Ciênc Saúde Colet. 2000;5(1):163-77.
15. Ciconelli RM, Ferraz MB, Santos W, Meinão I, Quaresma MR. Tradução para a língua portuguesa e validação do questionário genérico de avaliação de qualidade de vida SF-36 (Brasil SF-36). Rev Bras Reumatol. 1999;39(3):143-50.
16. Salomé GM, Blanes L, Ferreira LM.Assessment of depressive symptoms in people with diabetes mellitus and foot ulcers. Rev Col Bras Cir. 2011;38(5):327-33.
17. Meneses LC, Blanes L, Veiga DF, Gomes HC, Ferreira LM. Health-related quality of life and self-esteem in patients with diabetic foot ulcers: results of a cross-sectional comparative study. Ostomy Wound Manage. 2011;57(3):36-43.
18. Hokkam EN. Assessment of risk factors in diabetic foot ulceration and their impact on the outcome of the disease. Prim Care Diabetes. 2009;3(4):219-24.
19. Winkley K, Stahl D, Chalder T, Edmonds ME, Ismail K. Quality of life in people with their first diabetic foot ulcer: a prospective cohort study. J Am Podiatr Med Assoc. 2009;99(5):406-14.
20. Zanetti ML, Otero LM, Biaggi MV, Santos MA, Peres DS, Guimarães FPM. Satisfação do paciente diabético em seguimento em um programa de educação em diabetes. Rev Latino-Am Enfermagem. 2007;15(4):583-9.
21. Jaksa PJ, Mahoney JL. Quality of life in patients with diabetic foot ulcers: validation of the Cardiff Wound Impact Schedule in a Canadian population. Int Wound J. 2010;7(6):502-7.
22. Salomé GM, Blanes L, Ferreira LM. Functional capability of patients with diabetes with foot ulceration. Acta Paul Enferm. 2009;22(4):412-6.
23. Fiusa SM, Menezes ALF, Prato SLP Ataíde MBC. Caracterização dos pacientes diabéticos atendidos em um ambulatório de estomaterapia. Rev Estima. 2006;4(3):19-24.
24. Bezerra SMMS, Santos ICRV, Sobral PHAF, Dum GL. Pé diabético: um estudo do custo do tratamento de pacientes internados em hospital público da cidade de Recife. Nursing. 2011;13(154):161-5.
25. Uchimoto S, Tsumura K, Hayashi T, Suematsu C, Endo G, Fujii S, et al. Impact of cigarette smoking on the incidence of type 2 diabetes mellitus in middle-aged Japanese men: the Osaka Health Survey. Diabet Med. 1999;16(11):951-5.
26. Al-Maskari F, El-Sadig M. Prevalence of risk factors for diabetic foot complications. BMC Fam Pract. 2007;10;8:59.
27. Shukla D, Tripathi AK, Agrawal S, Ansari MA, Rastogi A, Shukla VK. Pain in acute and chronic wounds: a descriptive study. Ostomy Wound Manage. 2005;51(11):47-51.
28. Salomé GM, Pellegrino DMS, Vieira TF, Blanes L, Ferreira LM. Sleep quality among patients with venous ulcers: a cross-sectional study in a health care setting in São Paulo, Brazil. Wounds. 2012;24(5):124-31.
29. Salome GM, Blanes L, Ferreira LM. Avaliação de sintomas depressivos em pessoas com úlcera venosa. Rev Bras Cir Plást. 2012;27(1):124-9.
1. Nurse, Audit Specialist, São Paulo, SP, Brazil
2. Medical Student, Universidade do Vale do Sapucaí, Pouso Alegre (UNIVÁS), MG, Brazil
3. Professor of Nursing Graduate Course of the UNIVÁS, Pouso Alegre, MG, Brazil
4. Postdoctoral fellow, professor of the Professional Master's Course in Health Science at UNIVÁS, Pouso Alegre, MG, Brazil
Correspondence to:
Sérgio Aguinaldo de Almeida
Av. Francisco de Paula Quintaninha Ribeiro, 280 - ap.134 - bloco 1
Jabaquara - São Paulo, SP, Brazil -CEP 04330-020
E-mail: estomaterapeuta@outlook.com
Submitted to SGP (Sistema de Gestão de Publicações/Manager Publications System) of RBCP (Revista Brasileira de Cirurgia Plástica/Brazilian Journal of Plastic Surgery).
Article received: October 27, 2012
Article accepted: December 29, 2012
This study was performed at the Outpatient Wound Clinics of Hospital Geral Vila Nova Cachoeirinha, São Paulo, SP, Brazil, and Conjunto Hospitalar de Sorocaba, Sorocaba, SP, Brazil.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter