

Original Article - Year 2012 - Volume 27 -
Impact of adjuvant radiotherapy on the cosmetic outcome of immediate breast reconstruction performed using a transverse rectus abdominis myocutaneous flap
Impacto da radioterapia adjuvante no resultado cosmético da reconstrução mamária imediata com retalho TRAM
ABSTRACT
BACKGROUND: The outcome of adjuvant radiotherapy performed after breast reconstruction using autologous flaps is controversial. In this study, we aimed to assess whether postoperative radiotherapy would induce volumetric and cosmetic changes after immediate breast reconstruction performed using a transverse rectus abdominis myocutaneous (TRAM) flap.
METHODS: We evaluated 25 patients who were previously diagnosed with breast cancer and underwent post-mastectomy autologous reconstruction with a pedicled TRAM flap followed by adjuvant radiotherapy. Late aesthetic results were recorded starting 6 months after the completion of a full course of radiotherapy.
RESULTS: The average patient age was 42.2 years (range, 30-53 years). Two (8%) complete flap losses occurred due to massive fat necrosis. Two (8%) patients exhibited flap contracture and volume loss, whereas skin changes were observed in 52% of patients. Most of the patients (84%), however, had no significant initial flap volume loss, contour distortion, or flap contraction.
CONCLUSIONS: The cosmetic result obtained in the present study by immediate breast reconstruction performed using an irradiated TRAM flap was satisfactory compared to the data described in the literature. These findings suggest that the flap contours may be distorted by contraction and that significant volume losses can be observed in patients who may be candidates for TRAM flap reconstruction and require post-mastectomy adjuvant radiotherapy. Thus, in these circumstances, late complications due to postoperative irradiation should be considered.
Keywords: Mammaplastia. Breast/surgery. Radiotherapy.
RESUMO
INTRODUÇÃO: O efeito da radioterapia adjuvante após a reconstrução mamária com retalhos autólogos é controverso. O objetivo deste estudo é analisar se a radioterapia pós-operatória causa alterações volumétricas e cosméticas após a reconstrução mamária imediata com retalho do músculo reto abdominal (TRAM, do inglês transverse rectus abdominis myocutaneous).
MÉTODO: No total, foram avaliadas 25 pacientes submetidas a reconstrução autóloga com retalho TRAM pediculado pós-mastectomia por câncer de mama e radioterapia adjuvante. Os resultados estéticos tardios foram coletados após o intervalo mínimo de 6 meses posteriormente ao esquema completo da radioterapia.
RESULTADOS: A média de idade das pacientes foi de 42,2 anos, variando de 30 anos a 53 anos. Duas (8%) perdas completas do retalho ocorreram por necrose gordurosa maciça, duas (8%) pacientes evoluíram com contratura do retalho e perda volumétrica, e 52% das pacientes apresentaram alterações cutâneas. Entretanto, a maioria das pacientes (84%) não evoluiu com perda significativa do volume inicial do retalho ou com distorção do contorno e contração do retalho.
CONCLUSÕES: O resultado cosmético após a reconstrução mamária imediata com retalho TRAM irradiado foi aceitável, comparativamente aos dados descritos na literatura. Esses achados indicam que os retalhos podem sofrer distorções de contorno pela contração, além de perda volumétrica significativa em pacientes candidatas à reconstrução com TRAM e necessidade de radioterapia adjuvante pós-mastectomia. Assim, as complicações tardias da irradiação pós-operatória devem ser consideradas nesse contexto.
Palavras-chave: Mamoplastia. Mama/cirurgia. Radioterapia.
The popularity of immediate breast reconstruction has been gradually increasing since mastectomy was initially considered a potential treatment for breast cancer1. These procedures have been shown to improve the quality of life of these patients2,3. However, a subgroup of mastectomized patients requires adjuvant radiotherapy after reconstructive surgery to ensure locoregional control of neoplasms1,3. Although radiation negatively affects breast reconstruction performed with implants, the effect of radiotherapy on the autologous tissue remains uncertain1,3-5.
In this study, we aimed to assess the incidence of atrophy and volume loss of the reconstructed breast after immediate breast reconstruction performed using a transverse rectus abdominis myocutaneous (TRAM) flap in patients undergoing adjuvant radiotherapy for the treatment of breast cancer.
METHODS
A total of 25 patients who underwent immediate breast reconstruction using a TRAM flap followed by adjuvant radiotherapy were prospectively evaluated.
The operations were performed between 2004 and 2011 at the Plastic Surgery Service of Hospital Universitário Walter Cantídio (Fortaleza, CE, Brazil).
Data regarding volume loss, necrosis, and skin changes were collected. After the surgery, photographic records were monitored starting 6 months after the completion of a full course of radiotherapy.
RESULTS
Twenty-five patients who underwent immediate breast reconstruction followed by radiotherapy were evaluated in this study. The average patient age was 42.2 ± 6.8 years (range, 30-53 years).
Two (8%) flaps were completely lost due to massive fat necrosis and skin ulcerations that developed after irradiation of the reconstructed breast and required the implementation of an additional reconstructive surgical procedure in which the latissimus dorsi flap was combined with the implant. Two (8%) patients experienced significant atrophy of the flap that caused extensive asymmetry of the contralateral breast.
Most of the flaps did not display a significant volume reduction, which is commonly responsible for asymmetry. Changes in skin color (hyperpigmentation) or fibrosis, with significant alteration of the skin consistency observed in the irradiated regions, were detected in 13 (52%) patients.
Figures 1 to 10 illustrate some cases in this series.
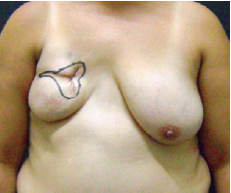
Figure 1 - After breast reconstruction using a contralateral transverse rectus abdominis myocutaneous flap and adjuvant radiotherapy, the patient experienced complete flap loss due to massive fat necrosis. Skin changes including fibrosis and depressions are visible around the scar.
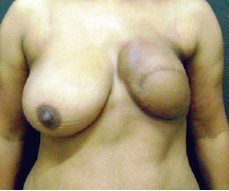
Figure 2 - After breast reconstruction using a contralateral transverse rectus abdominis myocutaneous flap, the patient experienced complete flap loss due to massive fat necrosis. Skin hyperpigmentation and shape distortion of the reconstructed breast are visible in the picture.

Figure 3 - After breast reconstruction using a contralateral transverse rectus abdominis myocutaneous flap, the patient experienced atrophy and volume loss. Breast asymmetry and skin changes are visible in the picture.
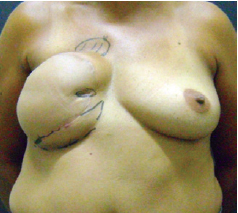
Figure 4 - After breast reconstruction using a contralateral transverse rectus abdominis myocutaneous flap, the patient experienced breast fibrosis and changes in the contour. The volume, however, was preserved.
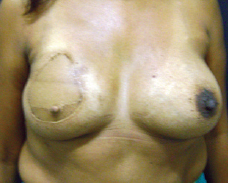
Figure 5 - Patient after breast reconstruction using a transverse rectus abdominis myocutaneous flap. Cutaneous hyperpigmentation was observed after radiotherapy.
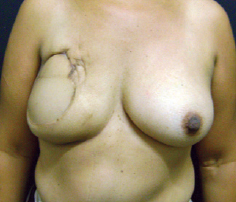
Figure 6 - Patient after breast reconstruction using a transverse rectus abdominis myocutaneous flap followed by adjuvant radiotherapy. Skin changes and fibrosis are visible around the scar.
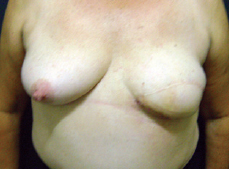
Figure 7 - Patient after breast reconstruction using a transverse rectus abdominis myocutaneous flap followed by adjuvant radiotherapy; no significant changes due to the irradiation were noted.
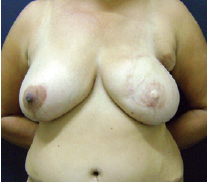
Figure 8 - Patient after irradiation who experienced no significant late changes.

Figure 9 - Patient after irradiation in whom breast volume and symmetry were maintained after the surgery.
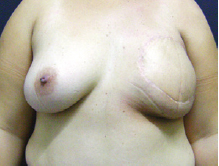
Figure 10 - Patient after breast reconstruction using a transverse rectus abdominis myocutaneous flap in whom breast volume was maintained and skin changes did not occur.
DISCUSSION
To date, no consensus has been reached on the ideal surgical time at which breast reconstruction should be performed, especially considering the multimodal context of oncologic treatment, and particularly when radiation therapy is indicated after mastectomy1.
Some authors recommend late reconstruction after radiotherapy, suggesting that non-breast bed tissues (muscle flaps, skin, and prostheses) would be irradiated unnecessarily, presumably causing further damage to the reconstructed breast1. On the contrary, other scientists support the approach of immediate reconstruction based on the fact that the local tissues and lymphatic drainage would be compromised after radiotherapy - an effect that hampers the flap construction and raises the rates of postoperative complications1,6.
Tran et al.5,6 reported the incidence of aesthetic deformities in patients undergoing immediate breast reconstruction performed using the TRAM flap followed by adjuvant radiotherapy. Although no flap loss was observed, the authors reported that 24% of the patients required an additional reconstructive procedure to correct the flap contracture. In this study, 24% of the patients maintained normal flap volume, although 78% showed loss of symmetry. Williams et al.7 revealed that post-irradiation changes in the TRAM flap occurred in 52.6% of cases and that 31.6% of patients required surgical intervention.
Chatterjee et al.8 conducted a prospective study in which 28 patients underwent immediate breast reconstruction performed using deep inferior epigastric artery perforator (DIEP) flaps. After assessing the pre- and post-irradiation volumes, these authors observed no significant differences among the measurements obtained after radiotherapy. Data from a meta-analysis study assessing the impact of radiotherapy on breast reconstruction confirmed that irradiation has a detrimental effect on surgical outcome regardless of surgical time and technique. These studies also suggest that, when adjuvant radiotherapy is indicated, the immediate autologous approach is the best breast construction procedure3.
Of the patients presented in this study, 16% required surgical repair after radiotherapy. Two patients experienced complete flap loss that hampered the subsequent reconstruction, which is still lower than the percentage of patients with flap loss reported in the literature.
Although immediate breast reconstruction is usually successful, obtaining highly aesthetic and reproducible results is a challenge for plastic surgeons due to possible changes in the volume and contour of the flap caused by the irradiation.
CONCLUSIONS
The cosmetic outcome after immediate breast reconstruction performed using an irradiated TRAM flap was consistent with the data reported in the literature. The high incidence of changes in the appearance of autologously reconstructed breasts after irradiation may lead to flap loss. It is important to consider the unpredictability of the results and the need for corrective procedures after radiotherapy.
REFERENCES
1. Marta GN, Hanna SA, Martella E, Silva JLF. Radioterapia e reconstrução mamária após cirurgia para tratamento do câncer de mama. Rev Assoc Med Bras. 2011;57(2):132-3.
2. Webster RS. Avaliação da satisfação de pacientes submetidas a reconstrução mamária pós-setorectomia e simetrização mamária contralateral imediata. Rev Bras Cir Plást. 2010;25(1):85-91.
3. Barry MJ, Kell MR. Meta-analysis on the impact of post-mastectomy radiotherapy on breast reconstruction outcome. J Clin Oncol. 2010;28:15s.
4. Spear SL, Onyewu C. Staged breast reconstruction with saline-filled implants in the irradiated breast: recent trends and therapeutic implications. Plast Reconstr Surg. 2000;105(3):930-42.
5. Tran NV, Chang DW, Gupta A, Kroll SS, Robb GL. Comparison of immediate and delayed free TRAM flap breast reconstruction in patients receiving postmastectomy radiation therapy. Plast Reconstr Surg. 2001;108(1):78-82.
6. Tran NV, Evans GR, Kroll SS, Baldwin BJ, Miller MJ, Reece GP, et al. Postoperative adjuvant irradiation: effects on transverse rectus abdominis muscle flap breast reconstruction. Plast Reconstr Surg. 2000;106(2):313-7.
7. Williams JK, Carlson GW, Bostwick J 3rd, Bried JT, Mackay G. The effects of radiation treatment after TRAM flap breast reconstruction. Plast Reconstr Surg. 1997;100(5):1153-60.
8. Chatterjee JS, Lee A, Anderson W, Baker L, Stevenson JH, Dewar JA, et al. Effect of postoperative radiotherapy on autologous deep inferior epigastric perforator flap volume after immediate breast reconstruction. Br J Surg. 2009;96(10):1135-40.
1. Member of the Sociedade Brasileira de Cirurgia Plástica/Brazilian Society of Plastic Surgery (SBCP), regent of the Plastic Surgery and Reconstructive Microsurgery Service of the Hospital Universitário Walter Cantídio (HUWC), Fortaleza, CE, Brazil.
2. Resident physician at the Plastic Surgery and Reconstructive Microsurgery Service of the HUWC, Fortaleza, CE, Brazil.
3. Expert member of the SBCP, preceptor of the Plastic Surgery and Reconstructive Microsurgery Service of the HUWC, Fortaleza, CE, Brazil.
4. Graduating medical student of the Universidade Federal do Ceará (UFC), member of the Plastic Surgery League of UFC, Fortaleza, CE, Brazil.
Correspondence to:
Juliana Régia Furtado Matos
Rua Mombaça, 164 - Aldeota
Fortaleza, CE, Brazil - CEP 60160-190
E-mail: julianarfm@gmail.com
Submitted to SGP (Sistema de Gestão de Publicações/Manager Publications System) of RBCP (Revista Brasileira de Cirurgia Plástica/Brazilian Journal of Plastic Surgery).
Article received: July 4, 2012
Article accepted: September 15, 2012
This study was performed at the Plastic Surgery and Reconstructive Microsurgery Service of Walter Cantidio University Hospital (HUWC), Fortaleza, CE, Brazil.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter