

Case Report - Year 2016 - Volume 31 -
Abdominal dermocutaneous flap for reconstruction of a bleeding area in necrotizing fasciitis
Retalho dermocutâneo abdominal para reconstrução de área cruenta pós-fasceíte necrotizante
ABSTRACT
INTRODUCTION: The sequelae caused by Fournier's syndrome are extensive, systemic, debilitating, and deforming. They require both general and local treatments with antibiotics and subsequent debridement to delimit non-necrotic margins, which result from extensive bleeding areas.
METHODS: The area affected and described in this study is the upper third of the right thigh. The goal was to use the dermocutaneous excess, usually removed in abdominoplasties. Abdominoplasty was routinely performed, and the cutaneous excess of the hypogastrium was transferred to cover a bleeding area in the upper third of the thigh throughout its extension. In the bleeding region, adequate occlusion was performed, and a tissue with similar thickness and elasticity was used to minimize the deformities that affected both the donor and receiving areas.
RESULTS: The bleeding area was covered in a single surgery.
CONCLUSION: The use of the cutaneous excess of the hypogastrium to cover the bleeding region of the upper third of the thigh is an alternative technique, which can be conducted in a single surgery in patients presenting excess abdominal skin.
Keywords: Fournier's gangrene; Surgical flaps; Abdominoplasty; Debridement.
RESUMO
INTRODUÇÃO: As sequelas decorrentes da síndrome de Fournier são extensas, de repercussão sistêmica, debilitantes e deformantes, que exigem tratamento geral e local com o uso de antibióticos e sucessivos desbridamentos para delimitar os limites sem necroses resultando áreas cruentas e extensas.
MÉTODOS: O caso presente envolveu o terço superior da coxa direita. A proposta foi a de utilizar o excedente dermocutâneo, que normalmente é eliminado nas abdominoplastias. A abdominoplastia foi realizada dentro da rotina em que este excedente cutâneo do hipogástrio foi transferido para cobrir a área cruenta em toda a sua extensão no terço superior da coxa. A oclusão foi adequada na área cruenta, com um tecido semelhante em espessura e elasticidade, minimizando a deformidade tanto na área doadora quanto na receptora.
RESULTADOS: Foi obtida total cobertura da área cruenta num único tempo operatório.
CONCLUSÃO: A utilização dos excessos cutâneos do hipogástrio para recobrir a área cruenta no terço superior da coxa segue como mais uma opção técnica num único tempo operatório em pacientes com excesso cutâneo abdominal.
Palavras-chave: Gangrena de Fournier; Retalhos cirúrgicos; Abdominoplastia; Desbridamento.
Necrotizing fasciitis is a severe condition characterized by an acute infection affecting the soft tissues, particularly the perineal and abdominal regions. In addition to fungi, the cause is usually gram-negative bacteria, such as Escherichia coli, Proteus mirabilis, Klebsiella sp., and Pseudomonas, and gram-positive bacteria such as Staphylococcus, Streptococcus, and Clostridium spp. It may be very extended, also presenting with systemic repercussion that can lead to death.
Jean Alfred Fournier studied and described this disease for the first time in 18831. He observed that this disease is prevalent in cases of poor hygiene in the perineal region and is associated with predisposing factors such as diabetes mellitus, alcoholism, local trauma, morbid obesity, use of immunosuppressants, and debilitating diseases.
The disease has a higher incidence in individuals aged 20 to 60 years and affects male sex in particular. The sequelae caused by this disease are usually widespread, systemic, and debilitating, and require general and local treatments with antibiotics and subsequent debridement to remove areas of necrosis, thus resulting in extensive bleeding areas2-9.
CASE REPORT
A 38-year-old female patient presented to our clinic with a history of a small inflammatory process in the right groin region, which was rapidly infected. The patient was treated at another hospital, where she had undergone subsequent debridement and received special care. Once the patient presented a satisfactory general condition, being eupneic, hydrated, and afebrile, and having normal skin color, pulmonary auscultation, and abdominal palpitations, she was then referred to our clinic.
She manifested large bleeding areas in the perineal region and medially, in the root of the right thigh, with evolving granulation tissue with little fibrin, without other signs of infections.
The patient underwent low transversal pubic abdominoplasty. The bleeding area was completely occluded by mobilization, rotation, and advancement of an abdominal skin flap of the hypogastrium, with a 3:1 proportion between its base and length (Figures 1 and 3).

Figure 1. Local appearance of the right inguino-crural region after surgical cleaning and under occlusion. Abdominal skin region marked as donor area and used to occlude the bleeding region, followed by low-transversal pubic abdominoplasty, extending up to the anterior superior iliac spine, and dissection until near the sternum.

Figure 2. Completion of the surgery with lesion occlusion, skin suture, and suction drains.
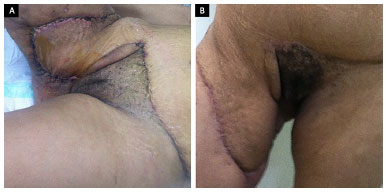
Figure 3. A and B: Twenty days and 4 months after surgery, respectively.
DISCUSSION
After surgery, the patient remained hospitalized for 3 days and her condition progressed normally, without complications. The outpatient follow-up was conducted weekly for 30 days and monthly for 6 months. We believe that this abdominal skin flap provides a satisfactory coverage while reducing hospital stay, conferring a similar thickness to the surface of the affected area and faster return to daily activities. The suggestion of possible future retouches was discarded by the patient.
CONCLUSIONS
The technique using excess abdominal skin to occlude a bleeding area in the upper third of the thigh requires a specific indication and should be performed in combination with abdominoplasty in cases with cutaneous excess of the hypogastrium that is sufficient to occlude the bleeding area.
COLLABORATIONS
RNF Formulated the hypothesis and designed the study; performed the surgeries and/or experiments; analyzed and/or interpreted the data; and wrote the manuscript and critically reviewed its content.
RB Critical review of its contents; final approval of the manuscript.
REFERENCES
1. Fournier AJ. Etude clinique de le gangrène foudroyante de la verge. Semaine Med. 1884;4:69.
2. Masquelet AC, Gilbert A. An atlas of flaps in limb reconstruction. London: Martin Dunitz; 1995. p.111-21.
3. Bloch RJ, Gasques JAL, Bozola AR, Cymrot M. Retalho Fasciocutâneo Súpero-Medial da Coxa. In: Bloch RJ, ed. Retalhos fasciais e fasciocutâneos e osteomiofasciocutâneos. Rio de Janeiro: Revinter; 2002. p. 169-80.
4. Bloch RJ, ed. Retalhos fasciais, fasciocutâneos e osteomiofasciocutâneos. Rio de Janeiro: Revinder; 2002. p. 1-23.
5. Teixeira Neto N, Giachetto E, Kamamoto F, Ferreira MC. Infecções graves de partes moles: relato de caso de fasciíte necrotizante em face utilizando curativo a vácuo e revisão de literatura. Rev Bras Cir Plást. 2011;26(2):356-9.
6. Ferreira PC, Reis JC, Amarante JM, Silva AC, Pinho CJ, Oliveira IC, et al. Fournier's gangrene: a review of 43 reconstructive cases. Plast Reconstr Surg. 2007;119(1):175-84.
7. Zampieri FMC, Ferreira MC, Batista BPSN, Milcheski DA, Nakamoto HA, Tuma P Jr. Tratamento cirúrgico da ferida complexa traumática perineal: experiência da Cirurgia Plástica do Hospital das Clínicas da FMUSP. Rev Bras Cir Plást. 2012;27(3 Supl 1):78.
8. Thorne HMC, Siebert JW, Grotting CJ, Vasconez LO, Shaw WW, Sauer PF. Reconstructive surgery of the lower extremity. In: McCarthy JG, ed. Plastic Surgery. Vol. 6. Philadelphia: W.B. Saunders; 1990. p. 4029-90.
9. Maguina P, Paulius KL, Kale S, Kalimuthu R. Medial thigh fasciocutaneous flaps for reconstruction of the scrotum following Fournier gangrene. Plast Reconstr Surg. 2010;125(1):28e-30e.
1. Hospital Regional da Asa Norte, Brasília, DF, Brazil
2. Sociedade Brasileira de Cirurgia Plástica, São Paulo, SP, Brazil
Institution: Hospital Regional da Asa Norte, Brasília, DF, Brazil.
Corresponding author:
Roger Nayef Fakhouri
Centro Clínico Via Brasil
Asa Sul, SEP/SUL 710/910 - Lotes C e D - Salas 234/236
Brasília, DF, Brazil Zip Code 70390-108
E-mail: rogerplastica@gmail.com
Article received: October 15, 2016.
Article accepted: November 28, 2016.
Conflicts of interest: none.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter