

Original Article - Year 2016 - Volume 31 -
Brachial-dorsal mammoplasty: body contour surgery of the upper region of the trunk after major weight loss
Braquio-dorso-mamoplastia: cirurgia do contorno corporal da região superior do tronco após grandes perdas ponderais
ABSTRACT
INTRODUCTION: In Brazil, 88000 bariatric surgeries were performed in 2014. After weight loss, deflation occurs around the trunk, with sagging and folding of excess skin of the breasts in the posterior dorsal region . We, therefore, propose a surgical procedure to treat upper region of the entire trunk, including breasts, side and rear back, and arms.
OBJECTIVE: To present a personal experience in brachial-dorsal mammoplasty surgeries.
METHOD: We operated 13 patients from 2007 to 2014, 11 women and two men.
RESULTS: The average age was 41.9 years. The brachial-dorsal mammoplasty was performed in all patients. In three cases, L-brachial-dorsal mammoplasty was performed, due to lower latero-posterior deformity. The average surgery duration was 4 hours and 30 minutes. The average Body Mass Index (BMI), before bariatric surgery, was 53.5 kg/m2. Weight loss ranged from 47 to 114 kg. The pre-surgery BMI ranged from 23 to 39 kg/m2. There were no cases of infection, large dehiscence or seroma. Two patients developed hematoma, requiring a new intervention for drainage.
CONCLUSION: Deformities of the thoracic region in patients with large weight loss are variable, requiring several surgical treatments that should address the entire chest as a single anatomical area. It is important to understand the deformity that each patient presents and adapt the surgical approach accordingly. The main indication for a brachial-dorsal mammoplasty is lateral drop of the inframammary fold.
Keywords: Torso; Bariatric surgery; Weight loss; Mammoplasty.
RESUMO
INTRODUÇÃO: No Brasil foram realizadas 88 mil cirurgias bariátricas em 2014. Após o emagrecimento, ocorre desinsuflação de todo o tronco, com flacidez e dobra de excesso cutâneo das mamas à região dorsal posterior. Por isso, propomos procedimento cirúrgico que trate a região superior toda do tronco, incluindo mamas, dorso lateral e posterior e braços.
OBJETIVO: Mostrar a experiência pessoal em cirurgias de braquio-dorso-mamoplastia.
MÉTODO: Foram operados 13 pacientes no período de 2007 a 2014, sendo 11 mulheres e dois homens.
RESULTADOS: A média de idade foi de 41,9 anos. A braquio-dorso-mamoplastia foi realizada em todos os pacientes. Em três casos, foi realizada braquio-dorso-mamoplastia em L, devido à menor deformidade latero-posterior. A duração média das cirurgias foi de 4 horas e 30 minutos. O Índice de Massa Corporal (IMC) médio, antes da cirurgia bariátrica, foi de 53,5 kg/m2. As perdas ponderais variaram de 47 a 114 kg. O IMC pré-operatório variou de 23 a 39 kg/m2. Não houve casos de infecção, grandes deiscências ou seroma. Duas pacientes evoluíram com hematoma, necessitando de nova intervenção para drenagem.
CONCLUSÃO: As deformidades da região torácica no paciente com perda ponderal maciça são variáveis, sendo necessários diversos tratamentos cirúrgicos que deverão abordar o tórax inteiro como área anatômica única. É importante compreender a deformidade que cada paciente apresenta e adequar a abordagem cirúrgica em conformidade. A indicação principal para uma braquio-dorso-mamoplastia é a queda lateral do sulco inframamário.
Palavras-chave: Tronco; Cirurgia bariátrica; Perda de peso; Mamoplastia.
Obesity is, without doubt, a worldwide epidemic. According to the Brazilian Society of Endocrinology and Metabolism, Brazil has around 70 million overweight individuals, which has doubled in the last three decades ago. Of these, 18 million are considered obese. In 2014, approximately 88000 bariatric surgeries were performed in Brazil, according to the Brazilian Society of Metabolic and Bariatric Surgery1.
Obesity surgery (bariatric surgery) is a type of surgical technique designed to promote weight reduction and treatment of diseases that are associated and/or aggravated by obesity.
Usually, the subcutaneous tissue and skin of the chest cling firmly to the muscle-aponeurotic plane in the anterior medial regions (pre-sternal) and back (thoracic spine). Weight increase causes vertical and horizontal circumferential expansion of the chest, remaining adhered to these medial regions described above, called adhesion zones2.
After weight loss, the chest deflates, resulting in excessive skin in these two dimensions, causing the appearance of flaccid skin and creating a larger thoracic skin fold in the lateral region. This causes a lateral descent of the inframammary fold, which continues with the dorsal fold, characterizing the main anatomical aspect of these patients with great weight loss2.
To perform an appropriate treatment of these patients, the plastic surgeon should examine the chest as a whole. Therefore, we believe in the treatment of the upper region of the trunk as a single anatomical area2.
Upper body lift surgery or brachial-dorsal mammoplasty is a combination of brachioplasty, resection of excess skin of upper region of the posterior and lateral trunk and treatment of the breast, or anterior thorax in men. This is necessary in cases where thoracic deformities are related to large weight loss. L-brachial-dorsal mammoplasty can be considered in patients with excess skin in the lateral region of the chest, without major excesses in the posterior region.
The criteria used for the selection of patients who are candidates for reconstructive surgery of thoracic deformity are similar to those of other regions of the body. The patient must have a stabilized weight loss for at least 6 months to 1 year3. One must perform a thorough preoperative evaluation, which includes determination of serum iron and plasma proteins to minimize complications. Note that after bariatric surgeries patients present some degree of malnutrition.
OBJECTIVE
The objective of this study is to present our experience in brachial-dorsal mammoplasty surgeries and report the systematization of the procedure.
METHODS
This review of our experience describes statistical data of all brachial-dorsal mammoplasty surgeries performed by a single surgeon, from 2007 to 2014, in private hospitals and the Clinical Hospital of the Federal University of Paraná, in Curitiba, PR.
The characteristics of patients such as age, gender, body mass index (BMI) pre-weight loss and BMI after weight stabilization, duration of surgery and post-operative complications were assessed.
Operative technique
Demarcation
Marking of brachial-dorsal mammoplasty was initiated with the patient standing. A posterior midline of the chest was demarcated. Then, we marked a superior incision line of the dorsoplasty. With a digital clamping maneuver of the excess skin, we demarcated the inferior line up to the middle axillary line, seeking to maintain the resulting scar within the bra region (Figure 1).
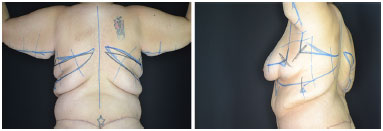
Figure 1. Demarcation of brachial-dorsal mammoplasty - rear and oblique view.
Next, we began the demarcation for brachioplasty, marking the brachial sulcus. Then, 1 cm below this line, the anterior incision from the axilla to the distal segment of the excess skin was demarcated. A digital clamping maneuver was performed to mark the posterior incision, finishing the distal marking with a slight angle toward the antecubital fossa, to hide the scar. In the axillary region, two triangles, with anterior apex, were demarcated, one in each line of the brachioplasty marking, with the aim of breaking the scar and preventing skin retractions in this region (Figure 1).
Then, we performed the markings of the lateral vertical dorsoplasty, connecting the posterior line of the brachioplasty to the superior line of the dorsoplasty, at a right angle. With digital clamping, we marked the anterior dorsolateral line, taking care to avoid lateralization of the breast.
Marking of the mammoplasty in an inverted T was carried out. Usually, we used Peixoto technique in "S", and then joined the dorsolateral markings (Figure 2). In male patients, the demarcation of the anterior region of the chest accompanied the bottom edge of the pectoral muscle, with design of the lower pedicle flap to the areola-papillary complex (Figure 3).
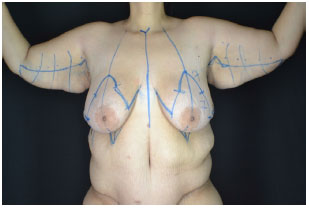
Figure 2. Demarcation of brachial-dorsal mammoplasty - front view.
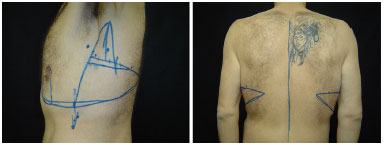
Figure 3. Demarcation of brachial-dorsal mammoplasty in a male patient.
L-Brachial-dorsal mammoplasty
In these cases, the demarcation of brachioplasty and lateral dorsoplasty was carried out, joining the lines of the two laterally to the marking of the lateral extremity of the inframammary fold, in the posterior axillary line. The line was drawn in a curve, calculating the tissue to be resected by digital clamping.
Surgical procedure
Brachial-dorsal mammoplasty
During surgery, we initiated the surgery at the dorsal region, with the patient in ventral decubitus. We infiltrated the markings and incised up to the muscle fascia. Tissue resection was followed by thorough hemostasis. Closure was performed by planes with PDS® 3.0 with fixing of tissues to deep fascia to decrease dead space and, consequently, seroma (Figure 4).
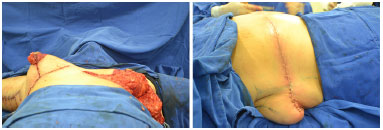
Figure 4. Transoperative aspect - Left, right breast already mounted, using high profile 350 ml textured round breast implant. Left breast after resection of tissue. Right, patient in ventral decubitus - posterior dorsoplasty completed showing excess skin in lateral region of the breast.
The patient was placed in dorsal decubitus, and we performed the brachioplasty incising up to the superficial fascia. Skin and subcutaneous tissue were resected in the block above the superficial fascia, which should be superficial in the axillary region, performing only skin resection to protect the lymphatic drainage. The closure was done by planes with Monocryl® 3.0 and 4.0 (Figure 5).
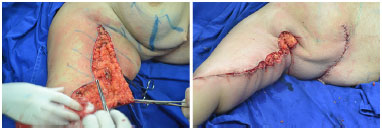
Figure 5. Braquioplastia - Transoperative aspect.
We performed mammoplasty with de-epidermization of the previously marked area and constructing a lower chest flap with lateral extension to obtain a larger breast volume, securing it with nylon 2-0 sutures to the pectoral muscle at the height of the second rib.
In patients with lower tissue volume, we performed breast implants, via the subfascial upper third of the surgical pocket, and constructed a small flap of the chest wall, elevating together with the anterior fascia of the chest to protect the implant. We sutured the superficial fascia at the lower edge of the incision lateral to the periosteum of the rib, in continuity with the dorsoplasty, to fix the inframammary fold to the new position (Figure 6).
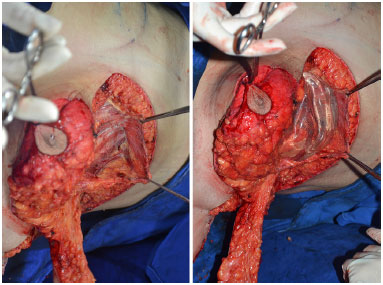
Figure 6. Patient in dorsal decubitus. Detail of mammoplasty with dissection of the subfascial plane, keeping tissue above for protection of the implant, minimizing the risk of extrusion.
In male patients, the incision was performed in the inframammary fold according to the demarcation, with the construction of the inferior pedicled flap to the areola. Resection of excess skin and fixation of flaps was done as shown in Figures 7 to 9.
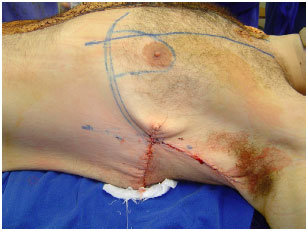
Figure 7. Patient in dorsal decubitus, after posterior dorsoplasty. Detail for ascent of the inframammary fold and demarcation of the pedicled flap for the areola.
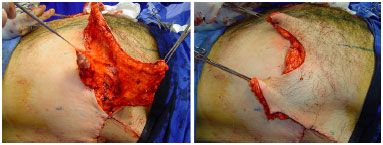
Figure 8. Transoperative aspect of brachial-dorsal mammoplasty in a male patient. Patient in dorsal decubitus, with detail for resection of excess skin on the right.
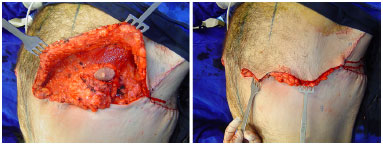
Figure 9. Transoperative aspect of brachial-dorsal mammoplasty in a male patient. Patient in dorsal decubitus, with detail for resection of lower pedicle to the upper areola and resection of lower pedicle to areola lifted on the left. Traction of the upper flap, being fixed, on the left. To the right, picture shows excess upper flap of the anterior chest, after resection of excess tissue.
Finally, there was the resection of the lateral vertical dorsoplasty, with closure in the fascial and cutaneous planes.
An aspiration drain was maintained until the first postoperative day. Deep venous thrombosis prophylaxis was held in all patients with physical methods and drug therapy. The majority of the patients were discharged on the first postoperative day.
L-Brachial-dorsal mammoplasty
The patient was positioned in dorsal decubitus. Brachioplasty and mammoplasty were performed according to the previous description. Finally, lateral dorsoplasty was performed, according to demarcation, with closure of the fascial plane and skin. Care must be taken in the compensation of the suture in both planes.
RESULTS
A total of 13 patients were analyzed, 11 females (84%) and two males (16%) (Figures 10 to 15). The average age at the time of surgery was 41.9 years (ranging from 21 to 62 years). In three patients, breast implants were used. Brachial-dorsal mammoplasty was performed in all patients. In three cases, L-brachial-dorsal mammoplasty was performed, due to lower lateral-posterior deformity.
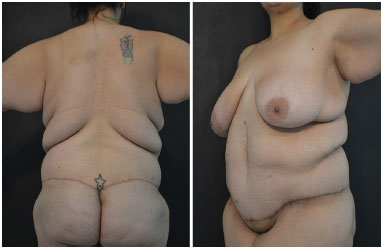
Figure 10. A 21-year-old female patient, after gastroplasty, with weight loss of 56 kg, pre-surgery - posterior and oblique view.
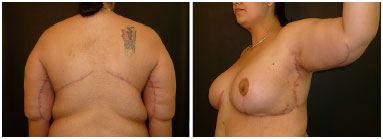
Figure 11. A 21-year-old female patient, after gastroplasty, with weight loss of 56 kg, 2 months after surgery - posterior and oblique view.
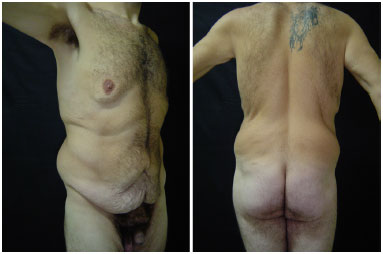
Figure 12. Male patient, 30 years old, after gastroplasty, with weight loss of 114 kg, pre-operative - oblique and posterior view.
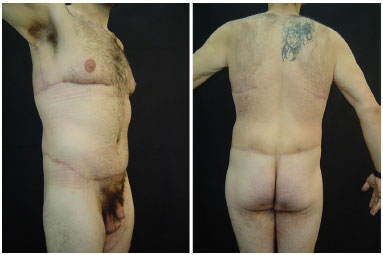
Figure 13. Male patient, 30 years old, after gastroplasty, with weight loss of 114 kg, 3 months postoperative - oblique and posterior view.
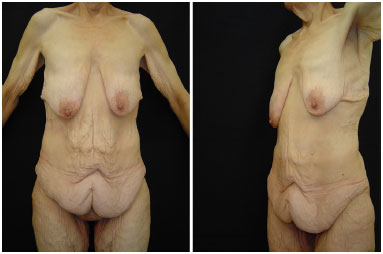
Figure 14. Female patient, 57 years old, after gastroplasty, with weight loss of 109 kg, pre-operative - front and oblique view.
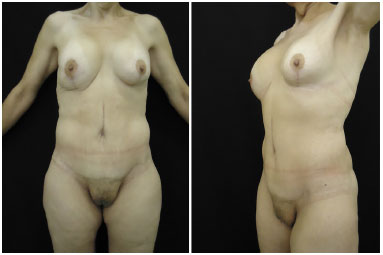
Figure 15. Female patient, 57 years old, after gastroplasty, with weight loss of 109 kg, 1 year postoperative - front and oblique view.
The average duration of surgeries was 272 minutes (4 hours and 30 minutes), ranging from 180 to 360 minutes.
The BMI before bariatric surgery ranged from 41 to 66 kg/m2, with an average of 53.5 kg/m2. Weight loss presented by patients ranged from 47 to 114 kg, with an average of 58.2 kg lost after bariatric surgery. The BMI at the time of reconstructive surgery ranged from 23 to 39 kg/m2. Of the total number of patients, eight had comorbidities (61% of the patients); of these, four with single comorbidity and three with more than one comorbidity.
There were no cases of infection, large dehiscence or seroma. Two patients (15%) developed hematoma, one case of hematoma in the breast and one case of hematoma in the arm that needed a new intervention for drainage, these being the only two complications with the need for reoperation. One patient (7%) evolved with slight breast asymmetry. One patient (7%) evolved with slight dyschromia of the areola. One patient presented higher weight loss after the first reconstructive surgery and needed surgical revision. Small corrections of scars were needed in some cases.
All patients underwent at least one body contour surgery, including brachial-dorsal mammoplasty. Five patients (50%) were submitted to two contour body surgeries. Three patients (30%) had three surgeries, and two (20%) underwent four post-bariatric reconstructive surgeries. Abdominoplasty was performed in seven patients (60%), six (40%) were submitted to circumferential abdominoplasty and five (50%) to dermolipectomy of thighs.
DISCUSSION
Excessive loss of weight after gastroplasty results in large body deformity, including the entire torso, breasts, and arms. This leads to great discomfort, such as difficulty in movement, intertrigo, and psychological sequelae4,5. We emphasize that, even after weight loss, these skin excesses retain the aspect of obesity in the patient, noticeable even with clothes.
The restoration of body contour after excessive weight loss is of great importance for these patients, restoring self-esteem and rehabilitating the patient for physical activities4,5. The upper region of the trunk includes the breasts, arms and back; however the breasts are a cause of greater impact and complaints in female patients4. For women, the breasts are the key factor for restoring body contour.
Excessive loss of body weight causes several undesirable situations, such as mammary ptosis, skin folds on the back, ptosis of the posterior axillary line and excess tissue in the arms4,6. The breasts vary from atrophy to significant hypertrophy4. Due to the catabolism of fat and connective tissue, there is a reduction in mammary projection, flattening, and flaccidity. Furthermore, descent of the nipple and the inframammary fold occurs. The excess skin in these patients ends up worsening the appearance of the breasts, and the skin of the thoracic region droops on itself in cascades, like a curtain6.
Normally, the skin-fat envelope adheres firmly to the musculoskeletal region of the chest, and the inframammary fold has a semi-circular form. Obesity causes a circumferential and vertical growth of the chest. A pronounced weight loss produces flaccidity of the skin and excess skin in these two directions. There are adhesion spots in the chest in the anterior and posterior median, pre-sternal and thoracic spine regions and, in these places, fat is not deposited. After weight loss, the regions lateral to these adhesions tend to dip. The deformity of each patient depends on the quality of the skin, age, BMI and actual weight lost after bariatric surgery.
Most of our patients have an average weight loss of 58.2 kg after bariatric surgery, which results in large flaccidity and various deformities. The deformities caused by the loss of excess weight include inverted "V" deformity, sagging inframammary fold, and excess back skin, breast abnormalities such as hypertrophy, atrophy, and ptosis in women. Men also present large posterior, lateral, and even anterior skin flaccidity, such as breast volume7.
The most appropriate patients to undergo the surgery are those who present weight stabilization for 6 to 12 months, and those that have classical deformities in the upper part of the body; however, those with more adhered tissue do not benefit as much from this surgery7. The patient should be assessed globally, verifying nutritional and metabolic deficiencies, control of associated diseases, and evaluation of psychological conditions5.
The concept of associated surgeries entails some disadvantages such as increased surgical time, increased risk of postoperative complications, especially with the wound, as this is more extensive. However, the biggest advantage is that to achieve the objective of the proposed surgery, fewer operative times are required4. The most important factor in performing resection of tissues in the same surgical time is obtaining a better body contour.
The average surgical time was 4 hours and 30 min, deemed appropriate, according to the resolutions of safe surgery suggested by the Brazilian Society of Plastic Surgery. To attain this, one must have a well-defined routine, systematic procedure and surgical steps, integration, and training of teamwork.
Several techniques have been introduced for the treatment of upper body contour, including brachioplasty to rejuvenate the region of the arms and armpits, procedures for the dorsal region and several techniques to correct the breasts5. The objective of brachial-dorsal mammoplasty is to improve contour of the arms, and entire circumference of the chest, raise the inframammary fold, eliminate excess breast laterally and improve breast contour.
Some reports classify breast deformities to establish the surgical plan, justified in asserting that the type of breast deformity determines the best result. Type 1 is characterized by hypertrophy and excess breast volume. In Type 2, there is ptosis with adequate breast volume. Type 3 patients are those with ptosis with inappropriate breast volume. Surgical options depend on the anatomic characteristics and desire of the patient. Among them are breast implants, dermofat flaps of the lower portion of the breast, and lateral region of the chest4.
Breast deformities have the greatest number of options for treatment, as cited, and can be treated with traditional reduction, autologous breast augmentation or with implants, associated or not with mastopexy4,6. Some innovative techniques are also suggested such as spindle flap, total remodeling of the breast, and use of flap pedicled in perforating vessels4.
These techniques do not always produce satisfactory results due to the lack of breast projection and persistence of the inframammary fold in a lower position. The lack of treatment of the thoracic region and axilla results in aesthetic disharmony6. In our study, the majority of patients were submitted to breast reconstruction with classical techniques, such as mastopexy with breast implants (two patients), mastopexy without breast implants and reduction mammoplasty in "T".
The surgery to correct excess skin of the arms should be assessed individually8.
There are different ways described to perform brachioplasty, such as L-brachioplasty, described by Hurwitz, with demarcation of the medial face of the arm, resection of skin and liposuction. In the technique described by Aly, the demarcation is in the posterior position, resection of skin and fat until the superficial fascia, and Z-plasty in the axilla is performed. This technique allows a more aesthetic scar in the axillary region and with less probability of contracture, being more simple and faster.
Some reports mention that the scars on the axilla in "Z" or "T" are not as aesthetic as the "L" form. The majority of reports that used the "Z" technique suggest that this scar results in a lower chance of contracture9. In the present study, we performed a combinationof the two techniques, with minor modifications. Therefore we believe direct resection without liposuction to be more effective, and drawing of the triangles in the axillary region provides the breakdown of scar preventing contractures, without the unpleasant aesthetic outcome of the visiblehalf of Z-scar in the rear view.
The correction of excess skin in the lateral region of the chest is a deformity that, in the past, was not treated properly. For complete resection of excess lateral and dorsal skin, it must be associated a vertical incision in the midaxillary line, uniting the brachioplasty with breast surgery, resulting in a surgery called brachial-dorsal mammoplasty (upper body lift) in 'L". It must be performed after an adequate assessment of the patient, especially if there is excess posterior skin and descent of the inframammary fold, since in most serious cases a brachial-dorsal mammoplasty should be the best option. It can be a good therapeutic option in other cases as well.
Our sample is based on the achievement of brachioplasty, lateral dorsoplasty or postero-lateral dorsoplasty. An inferior flap of the back was lifted up to the superior incision, allowing to eliminate vertical excess skin, a lateral elevation of the inframammary fold and eliminate lateral excess skin of the breast and back, agreeing with the technique described by Aly2 and the demarcation of the axilla according to Hurwitz6. The results of correction of excess back and lateral skin in patients were satisfactory.
After bariatric surgery, patients undergo some nutritional changes, dependent on the type of surgery performed. The nutritional deficiencies most commonly found are of vitamins, protein, minerals (mainly of zinc and calcium) and iron5. These situations, together with the fact that most have some comorbidity, increase the risk of postoperative complications.
Most of our patients had some comorbidity such as hypertension, hypothyroidism, depression and arthrosis. The main complications found in studies after surgery in patients with excessive weight loss are bleeding, infection, inesthetic scar, improper positioning of the scars and dehiscence, due to extension of the surgical wound and tension vectors in opposite directions7. Bleeding ends up being up to two-fold more frequent in these patients due to the larger caliber of vessels (up to three-fold)9.
The presence of seroma, lack of definition of the inframammary fold, asymmetry, and inappropriate body contouring has also been reported in the literature3. Some patients, when submitted to brachioplasty, might present lymphedema and lymphocele10. In breast surgeries, hematoma, dehiscence, necrosis of the areola and flaps and later recurrence of ptosis might occur.
Despite the complexity of these patients and higher risk of complications, there were no cases of infection or dehiscence in our study. Only two patients developed hematoma requiring surgical drainage. We also had one patient with mild asymmetry and another with discrete dyschromia of the areola, and one case of seroma, with resolution with aspiration with a syringe and compressive dressings.
CONCLUSION
Deformities of the thoracic region in patients with massive weight loss are variable, requiring several surgical treatments that should address the entire chest as a single anatomical area. It is important to understand the deformity that each patient presents and adapt the surgical approach accordingly. The main indication for a brachial-dorsal mammoplasty is lateral drop of the inframammary fold.
COLLABORATIONS
AECM Formulation of the hypotheses and study design; performance of the surgeries and/or experiments; manuscript preparation and critical review of the content.
PB Analysis and interpretation of the data; performance of the surgeries and experiments.
PGC Analysis and interpretation of the data; performance of the surgeries and experiments.
ASKA Analysis and interpretation of the data; performance of the surgeries and experiments.
RSF Final approval of the manuscript.
REFERENCES
1. Sociedade Brasileira de Cirurgia Bariátrica e Metabólica - SBCBM. Volume Cirurgias Bariátricas [citado 2016 Set 12]. Disponível em: http://www.sbcbm.org.br/wordpress/imprensa-2/releases/evolucao-das-cirurgias-bariatricas-no-brasil/
2. Aly AS. Upper body lift. In: Aly AS, ed. Body contouring after massive weight loss. Saint Louis: Quality Medical Publishing; 2006. p. 335-60.
3. Aly A, Soliman S, Cram A. Brachioplasty in the massive weight loss patient. Clin Plast Surg. 2008;35(1):141-7.
4. Huemer GM. Upper body reshaping for the woman with massive weight loss: an algorithmic approach. Aesthetic Plast Surg. 2010;34(5):561-9.
5. Marema RT, Buffington CK, Perez MA. Surgical treatment of morbid obesity. In: Aly AS, ed. Body contouring after massive weight loss. Saint Louis: Quality Medical Publishing; 2006. p.19-47.
6. Hurwitz DJ, Agha-Mohammadi S. Postbariatric surgery breast reshaping: the spiral flap. Ann Plast Surg. 2006;56(5):481-6.
7. Soliman S, Rotemberg SC, Pace D, Bark A, Mansur A, Cram A, et al. Upper body lift. Clin Plast Surg. 2008;35(1):107-14.
8. Aly A, Soliman S, Cram A. Braquioplastia no Paciente com Grandes Perdas Ponderais. In: Aly A, ed. Cirurgia do Contorno Corporal Após Grandes Perdas Ponderais - Cirurgia Plástica. Rio de Janeiro: DiLivros; 2008 p. 163-71.
9. Resende JHC. Tratamento cirúrgico complementar na obesidade mórbida. In: Mélega JM, ed. Cirurgia plástica fundamentos e arte: cirurgia estética. Rio de Janeiro: Medsi; 2003. p. 687-94.
10. Rubin JP, Khachi G. Mastopexy after massive weight loss: dermal suspension and selective auto-augmentation. Clin Plast Surg. 2008;35(1):123-9.
1. Sociedade Brasileira de Cirurgia Plástica, São Paulo, SP, Brazil
2. Universidade Federal do Paraná, Curitiba, PR, Brazil
Institution: Hospital de Clínicas, Universidade Federal do Paraná, Curitiba, Paraná, Brazil.
Corresponding author:
Alexandre Elias Contin Mansur
Avenida Sete de Setembro, sala 1507, 4698 - Batel
Curitiba, PR, Brazil Zip Code 80240-000
E-mail: acmansur@uol.com.br
Article received: July 29, 2015.
Article accepted: September 29, 2015.
Conflicts of interest: none.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter